Introduction
Osteoarthritis (OA) is the most common chronic musculoskeletal condition worldwide and a leading cause of chronic disability (Arthritis Care, OA Nations Survey, 2003; Murray and Lopez, 1997b), currently accounting for more than a third of chronic moderate-to-severe pain in the United Kingdom (Breivik et al., Reference Breivik, Collett, Ventafridda, Cohen and Gallacher2006). Of the UK adult population, 10–15% is estimated to have OA, with the prevalence rising considerably in the older population. At least half of those over the age of 60 years have knee, hip and/or hand OA, whereas three of every four people over the age of 75 years have OA in at least one joint (Arden and Nevitt, Reference Arden and Nevitt2006). Over the past 20 years the incidence of OA has increased two- to fourfold and, with the continual ageing of the UK population and the growing problem of obesity, it is expected to continue to rise in the years to come (Murray and Lopez, Reference Murray and Lopez1997a).
Aside from the considerable suffering to individuals in terms of poorly controlled pain, loss of function and markedly reduced quality of life, OA places an enormous burden on healthcare services (Arthritis Care, OA Nations Survey, 2003). OA is a chronic condition that may require periodic review over many years, with primary care acting as the major provider of both initial and continuing care for OA. It has been estimated that at least 20% of adults consult their general practitioner (GP) with a musculoskeletal problem over the course of a year, with the majority of these consultations attributed to OA (Jordan et al., Reference Jordan, Clarke, Symmons, Fleming, Porcheret, Kadam and Croft2007). On average, one in every seven GP consultations is related to a musculoskeletal problem (Jordan et al., Reference Jordan, Clarke, Symmons, Fleming, Porcheret, Kadam and Croft2007).
Efficient primary care management of OA is crucial to reduce or delay the use of limited and expensive specialised care resources, particularly in light of the growing prevalence of OA and the potential increasing burden on the healthcare service. To appropriately manage OA in both primary and secondary care, several evidence-based guidelines have been produced nationally (Conaghan et al., Reference Conaghan, Dickson and Grant2008) and internationally (Jordan et al., Reference Jordan, Arden, Doherty, Bannwarth, Bijlsma, Dieppe, Gunther, Hauselmann, Herrero-Beaumont, Kaklamanis, Lohmander, Leeb, Lequesne, Mazieres, Martin-Mola, Pavelka, Pendleton, Punzi, Serni, Swoboda, Verbruggen, Zimmerman-Gorska and Dougados2003; Zhang et al., Reference Zhang, Doherty, Arden, Bannwarth, Bijlsma, Gunther, Hauselmann, Herrero-Beaumont, Jordan, Kaklamanis, Leeb, Lequesne, Lohmander, Mazieres, Martin-Mola, Pavelka, Pendleton, Punzi, Swoboda, Varatojo, Verbruggen, Zimmermann-Gorska and Dougados2005; Reference Zhang, Doherty, Leeb, Alekseeva, Arden, Bijlsma, Dincer, Dziedzic, Hauselmann, Herrero-Beaumont, Kaklamanis, Lohmander, Maheu, Martin-Mola, Pavelka, Punzi, Reiter, Sautner, Smolen, Verbruggen and Zimmermann-Gorska2007; Reference Zhang, Nuki, Moskowitz, Abramson, Altman, Arden, Bierma-Zeinstra, Brandt, Croft, Doherty, Dougados, Hochberg, Hunter, Kwoh, Lohmander and Tugwell2010), with some related to specific anatomical sites of OA. However, relatively little is known about current management of OA, use of available guidelines and barriers to optimal management of OA at the primary care level.
Therefore, the aims of this study were to survey randomly selected primary care practitioners to obtain data on current management strategies for OA and perceived barriers to providing optimal care.
Methods
Questionnaire development
After discussion with researchers experienced in primary care surveys, we decided on an electronic survey rather than a mail-out, largely because of the immediacy of response. A 21-question survey was constructed to obtain relevant information from GPs on the following questions: how they assess and treat OA; the influences on their management; the burden on their practice; and their need for improving care. The questions were developed in an iterative manner by consultation between the authors and the electronic survey development team and piloted with a GP colleague. Questions offered a variety of relevant set responses, which were developed through a consultation process and with the option to provide additional/other information where appropriate (see Supplementary Appendix).
Sample
GPs across the United Kingdom were randomly selected from the GP database held by Opinion Health and invited to take part in the online questionnaire. Only participants who selected either a GP or a GP with a special interest in musculoskeletal conditions (GPwSI) as their speciality were able to complete the survey. All respondents remained anonymous unless they chose to include contact details to receive a summary of results.
Ethical review
According to the National Research Ethics Service definitions of research, this project is classified as a service evaluation and is therefore exempt from the need for ethical review.
Data analysis
Descriptive statistics were used to present the data according to the questionnaire categories. In some categories, respondents had the opportunity to include more than one response; therefore, data could exceed 100%.
Results
Profile of respondents
A total of 1006 GPs were invited to participate, of whom 232 completed the survey (23%). There were slightly more number of male GPs than there were female GPs; the majority were aged between 35 and 54 years, and a small number were GPwSI (Table 1). Geographically, respondents were evenly spread across the Strategic Health Authorities with the majority working in urban locations and in medium-sized group practices (Table 1).
Characteristics of GPs completing the survey

GPwSI = GP with a special interest.
Patient assessment
OA represented the fourth most demanding condition in terms of practice time (ranked first by 23 respondents (10%)), with depression (n = 81, 35%), diabetes (n = 72, 31%) and hypertension (n = 39, 17%) being the most demanding conditions. Over 60% (n = 139) of GPs reported that they were very confident at differentiating OA from rheumatoid arthritis when assessing a patient presenting with joint pain. In terms of OA management, the majority of respondents rated National Institute for Health and Clinical Excellence (NICE) and professional experience as their biggest influences, followed by Primary Care Trust guidelines, Arthritis Research UK and own practice guidelines (Table 2).
Sources of information used to guide OA management in primary care
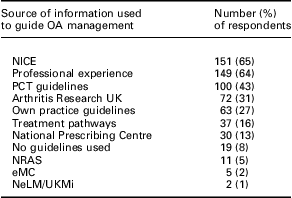
OA = osteoarthritis; NICE = National Institute for Health and Clinical Excellence; PCT = Primary Care Trust; NRAS = National Rheumatoid Arthritis Society; eMC = Electronic Medicines Compendium; NeLM/UKMi = National Electronic Library for Medicines/UK Medicines Information.
When treating patients, pain and mobility were reported to be the most frequently assessed constructs, with quality of life, independent living and sleep quality addressed by over half of them (Table 3). Depression, the effect of OA on relationships with friends and family and the effects on sexual relationships were the least likely constructs to be assessed by GPs. The majority (n = 191, 82%) of GPs reported that they did not use any tools to evaluate pain in OA patients; the few that did use tools (n = 41, 18%) most commonly used a numerical rating scale (n = 24, 58%) or general questioning about pain (n = 17, 42%). Approximately half of the GPs (n = 111, 48%) used educational materials with OA patients; however, only a third rated their current educational material as good or very good. The most commonly cited reasons for not providing adequate information or using educational material with patients were lack of time (n = 128, 55%), availability of material (n = 126, 54%) and quality of material (n = 67, 28%).
Problems assessed by GP when patient presents with OA
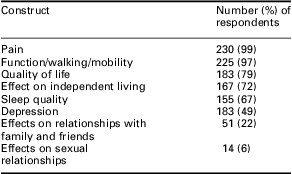
OA = osteoarthritis.
OA management
In accordance with NICE guidelines, recommendation of exercise and/or prescription of paracetamol and topical Nonsteroidal Anti-inflammatory Drugs (NSAIDs) were the most commonly reported management strategies (Table 4), with diet, prescription of oral NSAIDs or COX-2s, referral to a physiotherapist and opioid prescription also commonly used. Referral to a specialist or for joint replacement surgery and recommendation of walking aids or braces were less common (Table 4). GI risk (n = 70, 30%), pain control (n = 51, 22%), severity of condition (n = 46, 20%) and CV risk (n = 46, 20%) were the main reported influences for prescribing NSAIDs. Pain and side effects were also the main focus for NSAID (n = 218 (94%) and n = 223 (96%), respectively) and opioid (both n = 223 (96%)) prescription review, reported to be carried out by 74% (n = 172) of GPs every two to six months. On average, GPs reported prescribing gastroprotection, most commonly omeprazole, to 57% of patients treated with an NSAID.
Treatments recommended by GP to patients with OA
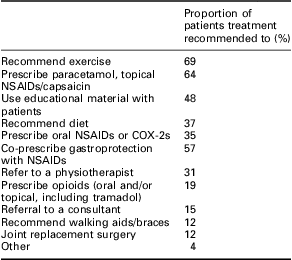
OA = osteoarthritis; NSAIDs = nonsteroidal anti-inflammatory drugs.
Barriers to OA management
Achieving adequate pain control was the most frequently cited challenge to OA management, followed by lack of time and getting patients to make lifestyle changes (Table 5). When asked what would enable GPs to manage OA patients more effectively, more time to see patients, collaboration with a specialist team, a need for improved tools to aid patient communications around risk, accredited training courses for GPs and more staff and resources were commonly suggested solutions (Table 6). Only a small proportion of GPs felt that they were currently managing their OA patients effectively (Table 6).
Most challenging aspects of OA management

OA = osteoarthritis.
Strategies to improve OA management
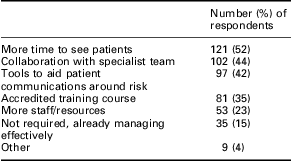
OA = osteoarthritis.
Discussion
Management of OA places considerable burden on primary care practitioners, with only depression, diabetes and hypertension found to be more demanding in terms of practice time. This is the first study to examine the influences on GP treatment of OA and their perceived barriers to optimal patient management. National guidelines were reportedly an important influence for GP treatment of OA, and our data suggest that most GPs employ at least some of the recommendations in their practice. This survey has highlighted a perception about the adequacy of the educational material available for OA and a need to improve both access to and quality of material used by GPs on patients. In particular, OA management within primary care would benefit from increased time for GPs to spend with OA patients, as well as improved interaction with specialist colleagues.
The fact that the majority of responding GPs reported being influenced by the NICE recommendations in their practice is an important finding of this study and underlines the value of this guidance in patient management. This view is also reflected in the data on the therapies used, with most GPs prescribing paracetamol, topical NSAIDs and exercise for their OA patients, which are recommended early treatments in the NICE OA guidance (Conaghan et al., Reference Conaghan, Dickson and Grant2008). Use of gastroprotection was modest (57%), although it appeared to be increased compared with recent reports (van Soest et al., Reference van Soest, Valkhoff, Mazzaglia, Schade, Molokhia, Goldstein, Hernandez-Diaz, Trifiro, Dieleman, Kuipers and Sturkenboom2011) and may reflect the impact of NICE guidance. Importantly, there was a high rate of medication review, with 74% of GPs reporting medication reviews every two to six months, in line with NICE recommendations for periodic review.
Educational material was used by less than half of the GPs who responded. NICE has recommended provision of information as part of the core treatment of OA. It is possible that some of these GPs provided verbal information, but there is a concern about access to written information and its quality. Of note, and an area requiring further investigation, is the opinion of many GPs currently using educational material that it is not adequate. Nearly half of the GPs felt that improved tools to aid patient communication around risk would help with OA patient management. It is encouraging that there are a number of ongoing studies to develop new educational material for GPs to be used with people with OA, with a recent feasibility study of a hip and knee OA management booklet showing small improvements in illness, exercise and fear-avoidance beliefs and increased levels of physical activity in patients provided with the booklet compared with a control group not provided with the booklet (Williams et al., Reference Williams, Amoakwa, Belcher, Edwards, Hassani, Hendry, Burton, Lewis, Hood, Jones, Bennett, Linck, Neal and Wilkinson2011). However, the findings in our study suggest that mechanisms to encourage GPs to use such material and further studies to develop, improve and validate educational material should be explored.
The NICE guidelines recommend a holistic approach to OA assessment and management, considering the global needs of an individual and taking into account social and psychological factors that have an effect on their quality of life and the ability to carry out activities of daily living, employment-related activities, family commitments, relationships and hobbies (Conaghan et al., Reference Conaghan, Dickson and Grant2008). In line with these recommendations, nearly all GPs reported the assessment of pain and function for patients presenting with OA, and the majority also reported to assess quality of life and effect on independent living. However, less than half assessed depression, and only 22% of GPs reported to assess the effect on relationships with family and friends. Anxiety and depression are very common in OA patients and are associated with increased pain and disability (Axford et al., Reference Axford, Butt, Heron, Hammond, Morgan, Alavi, Bolton and Bland2010; Kim et al., Reference Kim, Han, Cho, Chang, Park, Lee, Lee, Seong and Kim2011) and increased risk of functional decline (Dunlop et al., Reference Dunlop, Semanik, Song, Manheim, Shih and Chang2005; Mallen et al., Reference Mallen, Peat, Thomas, Lacey and Croft2007). People with depression are also three times more likely to be noncompliant with medical treatment recommendations (DiMatteo et al., Reference DiMatteo, Lepper and Croghan2000). The strong interrelationship between mental health, pain and disability underlines the importance of a multidisciplinary approach to the treatment of OA and suggests that assessment of anxiety and depression should form a core part of primary care management of OA.
Compared with data reported in 2004 from a GP survey on the use of conventional and complementary treatments for OA (Jordan et al., Reference Jordan, Sawyer, Coakley, Smith, Cooper and Arden2004), the incidence of physiotherapy referral and paracetamol prescription in our survey is increased, whereas the incidence of NSAID prescription is reduced, as might be expected with changes in prescription following growing awareness of NSAID complications in the mid-2000s (Sun et al., Reference Sun, Lee, Bertram and Goldstein2007). In contrast, a 2007 survey of adults aged 50 years or over suffering from knee pain found similar rates of patient-reported paracetamol prescription, recommendation for dieting and referral to a physiotherapist (Porcheret et al., Reference Porcheret, Jordan, Jinks and Croft2007). However, in our survey, recommendation for exercise was much higher, probably reflecting government initiatives to encourage increased physical activity (Health Scotland, 2008; Department of Health, 2009; Foster et al., Reference Foster, Thompson and Harkin2009), whereas NSAID and opioid prescription and recommendation of walking aids were reduced.
It is particularly noteworthy that GPs indicated lack of time to spend with patients to be one of the main challenges to OA management and the factor that, if addressed, would make the biggest difference in terms of their ability to optimally care for people with OA. The issue of time also reportedly hampered the provision of information to patients. Lack of time is an issue that has frequently been highlighted by GPs in other UK and European-based studies as a reason for not practising evidence-based medicine (McColl et al., Reference McColl, Smith, White and Field1998; Al-Ansary and Khoja, Reference Al-Ansary and Khoja2002) or health promotion (McKinlay et al., Reference McKinlay, Plumridge, McBain, McLeod, Pullon and Brown2005), as well as for not researching or implementing research findings (Robinson and Gould, Reference Robinson and Gould2000; Lionis et al., Reference Lionis, Stoffers, Hummers-Pradier, Griffiths, Rotar-Pavlic and Rethans2004). The Royal College of General Practitioners ‘Manifesto for Patient Care 2010’ has also highlighted this point, calling for an increase in the length of GP consultations to cope with the rising demand of the ageing population with their long-term and increasingly complex conditions (Manifesto for Patient Care, 2010). In addition, better collaboration with a specialist team was highlighted as a key need to improve primary care OA management.
Strengths and limitations of the study
This study had certain limitations. Only 23% of those invited completed the online survey and this may have introduced bias. GP response to survey requests is acknowledged to vary widely and is often low. It is also known to be influenced by questionnaire length, insufficient background information, volume of requests and financial information (McAvoy and Kaner, Reference McAvoy and Kaner1996). However, the GP population in this study is broadly reflective of the UK GP population as a whole, with similar gender and age distribution and geographic spread (Health Policy and Economic Research Unit. 2009 UK Medical Workforce, 2010) and only a small proportion reporting a special interest in musculoskeletal conditions. Although the option of recording additional answers not covered by the set text was offered for most questions in the survey, the set answers offered may have influenced GP responses and thus the results of this survey. For example, the use of topical NSAIDs and capsaicin, which are recommended as therapeutic options in the NICE guidelines, were not offered as answers to the question regarding treatment options offered to patients, and therefore the relative use of these treatment modalities cannot be assessed.
This study used clinician self-report as a proxy for clinician behaviour. Although direct measurement of clinical practice may be considered the ‘gold-standard’ measure of performance, these measures are often intrusive, time-consuming and expensive and may introduce bias through positive promotion of desired behaviour in observed individuals. The use of proxy measures is therefore considered a useful means of determining behaviour in an effective and less expensive manner. Studies on clinical behaviour have used a number of proxy measures including clinician self-report (Salmon et al., Reference Salmon, Peters, Rogers, Gask, Clifford, Iredale, Dowrick and Morriss2007), patient self-report (Steel et al., Reference Steel, Bachmann, Maisey, Shekelle, Breeze, Marmot and Melzer2008) and medical record review (Broadbent et al., Reference Broadbent, Maisey, Holland and Steel2008); however, the evidence base for these measures is still limited (Hrisos et al., Reference Hrisos, Eccles, Francis, Dickinson, Kaner, Beyer and Johnston2009). Further work to refine the findings of this study may therefore examine the potential for using a combination of proxy measures to obtain an all round picture of clinical behaviour.
Implications for future research or clinical practice
With the continual ageing of the UK population, the existing massive social and economic burden of OA is set to grow considerably over the coming decades. Developing and delivering strategies to optimise management of OA at the primary care level is therefore essential. Although the use of national guidelines to guide OA management by the majority of responding GPs in this survey is promising, it is evident that further provision is needed to enable GPs to satisfactorily manage their OA patients and aid patients in managing their own condition. Recent trials of self-help material are encouraging, and further studies to develop and validate such material will benefit both GPs and patients. Adequate management of pain is still a concern for GPs. This may well reflect issues with existing analgesic therapies; most clinical trials report group-level or mean pain responses, whereas the response in individuals is quite variable (Moore et al., Reference Moore, Moore, Derry, Peloso, Gammaitoni and Wang2010). The results of this survey also emphasise a need to revisit the duration of GP consultations or to develop novel methods of front-line clinician involvement in OA management, perhaps in line with management of other chronic conditions such as diabetes and cardiovascular disease, in which nurse-led management has proved effective (Woodward et al., Reference Woodward, Wallymahmed, Wilding and Gill2010; Berra et al., Reference Berra, Miller and Jennings2011; Clark et al., Reference Clark, Smith, Taylor and Campbell2011; Wallymahmed et al., Reference Wallymahmed, Morgan, Gill and Macfarlane2011). It may be that such changes to practice might centre on patient self-management with intermittent multidisciplinary intervention, with a focus on the global needs and psychological well-being of individuals. Improved links between primary care and specialist colleagues constitute a much needed focus for future health service research (Ham et al., Reference Ham, Imison, Goodwin, Dixon and South2011).
Additional information
S.R.K. and P.G.C. are funded in part by Arthritis Research UK and the NIHR Leeds Musculoskeletal Biomedical Research Unit.
Competing interests: S.R.K.: no disclosures. P.G.C.: research funding from Centocor and Pfizer; speaker or advisory boards for AstraZeneca, Bioiberica, BMS, Merck, Novartis, Pfizer, Roche.
Acknowledgements
This article is based upon a survey carried out by AstraZeneca. The article has been written independently, and full editorial control remains with the authors. We are grateful to AstraZeneca for financial support for the survey, to Munro and Forster for help in development of the questionnaire and to Opinion Health who conducted the online survey.







