Mental, neurological and substance use (MNS) disorders contribute significantly to disability worldwide, yet the treatment gap remains especially wide in low- and middle-income countries (LMICs). In conflict-affected regions such as Iraq, Egypt and Jordan, access to specialist services is constrained by displacement, poverty and fragile health systems. Reference Patel, Minas, Cohen and Prince1–3 Communities are often left to rely on overstretched primary care or informal psychosocial networks. Addressing this gap requires innovative task-sharing models that extend mental healthcare beyond psychiatrists to non-specialists.
Building on previous collaborations
The World Health Organization’s Mental Health Gap Action Programme Intervention Guide (mhGAP-IG) was designed for precisely this purpose, equipping non-specialists with the skills to recognise and manage common MNS disorders. 4 In 2022, the Royal College of Psychiatrists partnered with the Iraqi Red Crescent Society to deliver mhGAP-IG training to primary care doctors. That programme demonstrated measurable improvements in knowledge and confidence among trainees. Reference Al-Uzri, Al-Taiar, Abdulghani, Abbas and Suleman5 Building on this momentum, a subsequent initiative sought to extend training beyond physicians to psychosocial support workers – trusted community members often providing front-line assistance.
Cascade training in practice
In September 2023, a four-day mhGAP-IG cascade training was held in Baghdad for 20 psychosocial support workers drawn from Red Crescent Societies in Iraq, Egypt and Jordan. Participants came from varied professional backgrounds, including psychology, nursing, teaching, social work and paramedicine, with one participant from engineering. This multidisciplinary mix reflected the diversity of front-line roles. Training was delivered by four primary care physicians who had received mhGAP-IG training in 2022, supported by a supervising psychiatrist from the Royal College of Psychiatrists. The cascade model enabled trained doctors to consolidate their own knowledge while extending expertise to new groups in a sustainable manner. Reference Gureje, Oladeji, Ayinde, Kola, Abdulmalik and Abass6
Sessions were interactive, featuring case-based discussions, group exercises and clinical scenarios tailored to local contexts. The training aimed to bridge the gap between informal psychosocial support and formal mental health services by strengthening assessment, management and referral skills. Ethical approval was not required as no patients were directly involved; however, the project was formally approved by the Iraqi Red Crescent Society. Informed consent was obtained from all participants.
Impact of the training
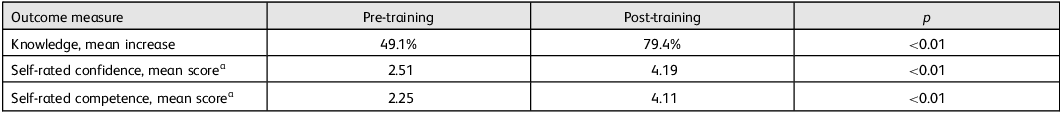
Assessments conducted before and after training demonstrated marked improvement in knowledge, self-rated confidence and self-rated competence (Table 1). Figure 1 illustrates these pre- and post-training changes across the outcome measures. These results reflected the effectiveness of the training in enhancing participants’ ability to recognise and address MNS conditions.
Summary of results of mhGAP-IG cascade training programme

a. Rated on a 5-point Likert scale.
Knowledge, confidence and competence ratings pre- and post-training. Confidence and competence were self-rated on a 5-point Likert scale.

Qualitative feedback from focus groups further illustrated the impact. Participants reported feeling better equipped to identify early signs of mental distress, use clinical terminology appropriately and manage sensitive discussions about stigmatised conditions such as depression and substance misuse. The interprofessional setting fostered cross-disciplinary learning, with participants appreciating the insights of colleagues from different backgrounds.
Barriers and challenges
Despite positive outcomes, systemic challenges persisted. Participants highlighted stigma at both community and institutional levels, inadequate infrastructure such as private consultation spaces, limited availability of psychotropic medications and underdeveloped referral pathways. Reference Hughes, Hijazi and Saeed2,3 These barriers are well documented in other LMIC contexts. Participants also emphasised the importance of sustainability, calling for ongoing supervision, refresher training and digital learning resources. Evidence from similar programmes indicates that without structured follow-up, training has limited long-term impact. Reference Gureje, Oladeji, Ayinde, Kola, Abdulmalik and Abass6
Lessons learned and global implications
This initiative marked the first occasion on which the Royal College of Psychiatrists supported mhGAP-IG cascade training across three countries simultaneously, aligning with its broader international strategy. 7 It represented the third phase of a multi-stage collaboration: initial physician training in 2022, ongoing supervision and finally the cascade training of psychosocial workers in 2023. The success of this model underscores the importance of phased, capacity-building approaches led by local providers rather than external experts. It also reinforces global evidence that mhGAP-IG is an effective framework for strengthening non-specialist mental healthcare provision. Reference Patel, Minas, Cohen and Prince1,4
Although we observed clear improvements in knowledge and self-rated confidence and competence immediately after the course, these measures do not necessarily translate into sustained changes in clinical practice or improved outcomes for patients. In practice, confidence can increase before participants have had enough supervised experience to apply new skills consistently. Ongoing supervision and supported case discussion are therefore likely to be important in helping participants translate training into day-to-day decision-making. Future evaluations should include follow-up after deployment, alongside practice-based measures such as documented detection, referral patterns and supervision-supported case reviews.
The programme demonstrated that psychosocial workers, who are often trusted community figures, can play a pivotal role in bridging the gap between informal support and formal care. Equipping them with mhGAP-IG skills may improve detection, support and referral, while fostering collaboration with primary care. Embedding mhGAP-IG into national curricula, supported by supervision and access to digital resources, offers a sustainable pathway to scaling up this approach. Reference Chaulagain, Pacione, Abdulmalik, Hughes, Oksana and Chumak8
The way forward
The mhGAP-IG cascade training delivered in Iraq, Egypt and Jordan significantly enhanced psychosocial workers’ confidence and competence in mental healthcare. It provides encouraging evidence that cascade models can strengthen capacity in resource-limited, conflict-affected settings, although ongoing support is likely to be needed to translate these gains into consistent practice. Although systemic challenges remain, the programme offers a replicable framework for LMICs seeking to expand access to mental health services. Ensuring sustainability will require institutional support, ongoing supervision and integration into national training systems. Nevertheless, this collaboration demonstrates the potential of task-sharing approaches to advance mental health equity in some of the world’s most challenging contexts.
Data availability
The data that support the findings of this study are available from the corresponding author on reasonable request.
Acknowledgements
We thank our colleagues at the Iraqi Red Crescent Society and Ministry of Health, Iraq, for their support and engagement in the training.
Author contributions
H.A.-H. led the manuscript writing and contributed to data interpretation. M.A.-U. conceived the study idea, provided oversight and supervised the project. H.A.-T. was responsible for data collection and assisted in delivering the training. Y.A.A. contributed to the manuscript writing and oversaw the programme on behalf of the Iraqi Red Crescent. All authors reviewed and approved the final manuscript.
Funding
This research received no specific grant from any funding agency, commercial or not-for-profit sectors.
Declaration of interest
None.




eLetters
No eLetters have been published for this article.