Self-harm is one of the strongest predictors of subsequent suicide and its prevention is a global public health priority, featuring prominently in suicide prevention strategies.Reference Carroll, Metcalfe and Gunnell1,2 It is defined as any act in which an individual initiates behaviour such as self-cutting or ingesting a toxic substance with an intention to cause harm to themselves.Reference Hawton, Rodham, Evans and Weatherall3 In young people aged 10–18 years, the risk of suicide 12 months after an episode of self-harm is estimated to be over 30 times higher than the expected rate in the general population of the same age.Reference Hawton, Bale, Brand, Townsend, Ness and Waters4 Although incidence rates of self-harm in young people presenting to hospital, primary care services and in the community appear to be increasing, particularly for girls, there is evidence that mortality following presentation for self-harm is comparatively low (1%) in relation to other age groups, and self-harm does not lead to suicide in most young people.Reference Geulayov, Casey, McDonald, Foster, Pritchard and Wells5–Reference Morgan, Webb, Carr, Kontopantelis, Green and Chew-Graham8 Of those who die, however, half of deaths are by suicide.Reference Geulayov, Casey, McDonald, Foster, Pritchard and Wells5,Reference Hawton, Saunders and O'Connor9
The recently updated suicide prevention strategy for England identifies children and young people for ‘consideration for tailored and targeted support at a national level’, including mental health support, support in educational settings and bespoke support to respond to the experiences and circumstances of some young people, such as bereavement and young people in care.2 The strategy calls for further research to understand the experiences of young people in relation to suicide.2 Although young people have low rates of suicide overall, rates have increased in recent years, particularly in females under 25 years.10,11 The strategy highlights the importance of focused efforts on self-harm prevention, the rates of which have also increased in young people.2 The National Institute for Health and Care Excellence (NICE) guidance on the assessment, management and prevention of recurrence of self-harm has been recently updated.12 This guidance recommends a psychosocial assessment by a mental health professional with experience in assessing children and young people is carried out at the earliest opportunity following an episode of self-harm.12 According to the guidelines, an exploration of social, peer group, education and home situations, any caring responsibilities, and any child protection or safeguarding issues should be part of such an assessment.12 This is in contrast to current practice. Only about half of those presenting to emergency departments after an episode of self-harm are assessed by a mental health professional.12
A lack of consensus around factors related to self-harm in young people who subsequently die by suicide can make it difficult for services to respond to their needs. An escalation in risk of suicide following self-harm is well established for older adults, but the relationship is less explored in young people who die by suicide.Reference Clements, Farooq, Hawton, Geulayov, Casey and Waters13–Reference Mars, Heron, Klonsky, Moran, O'Connor and Tilling16 Most studies focus on non-fatal suicidal behaviours (i.e. suicide attempts), which occur more commonly in young people.Reference Geulayov, Casey, McDonald, Foster, Pritchard and Wells5 Alcohol and drug misuse, sleep disturbance, personality traits and exposure to self-harm in others have been identified as potential risk factors for future suicide attempt in young people who self-harm.Reference Chan, Bhatti, Meader, Stockton, Evans and O'Connor17 The aim of this study was to describe self-harm in young people aged 10–19 years who died by suicide in the UK, over a 3-year (2014–2016) period. Specifically, our objectives were to examine the sociodemographic, clinical and service contact characteristics of young people who self-harmed before suicide, and to identify differences in subgroups (i.e. recent self-harm compared with lifetime or no history of self-harm) of young people who self-harm. Our rationale for this hypothesis was that the self-harm group who were in contact with services most recently before death would be the most amenable to intervention.
Method
Study population and setting
We conducted a UK-wide, exploratory, consecutive case series of all young people aged 10–19 years who died by suicide (including probable suicide) between 1 January 2014 and 31 December 2016. National mortality data were obtained from the Office for National Statistics (ONS; for deaths registered in England and Wales), National Records of Scotland and the Northern Ireland Statistics and Research Agency. Deaths receiving a coroner (or country equivalent) conclusion of suicide (ICD-10 codes X60–X84) or undetermined intent (ICD-10 codes Y10–Y34, excluding Y33.9, Y87.0 and Y87.2), including narrative conclusions, were included as suicides in this study.
Of the 595 suicide deaths notified in the 3-year period, information on the antecedents of suicide were obtained for 544 (91%) individuals from the sources detailed below (mainly coroner inquests).
Data sources
Coroner inquest hearings or police sudden death reports
For all deaths in England and Wales, audio recordings of coronial inquest proceedings were requested from the senior coroner of the jurisdiction where the death occurred. If unavailable, statements or depositions submitted during the inquest were requested. In Scotland, redacted police death reports were obtained from the Crown Office and Procurator Fiscal Service (COPFS). We also obtained witness statements and post-mortem reports from the Northern Ireland Courts and Tribunal Service. In total, we obtained coroner inquest hearings or COPFS reports for 526 (88%) deaths. For 40 deaths, the coroner was either unable to or did not wish to provide data, and in 29 data were not returned.
Child death investigations
In England, it is mandatory for Safeguarding Children Partnerships (SCPs) to review all deaths up to the age of 18 years, via Child Death Review processes. Every agency that knew the deceased child and their family during their life and after their death must provide information via statutory Child Death Review forms. The information is then reviewed and compiled into an analysis proforma (Form C) by an independent multiagency Child Death Overview Panel (CDOP). We accessed anonymous Form Cs from all SCPs where a CDOP had completed a review into a child's death by suicide or self-inflicted harm. We obtained Form Cs on 118 (50%) people aged under 18 years.
Case reviews
Case reviews (child safeguarding practice review in England, child practice review in Wales, case management review in Northern Ireland and significant case review in Scotland; collectively referred to here as ‘case reviews’) are conducted for all deaths or serious harm under the age of 18 years, where abuse or neglect is known or suspected. We obtained 20 reviews during the study period after searching each SCP website and the National Society for the Prevention of Cruelty to Children national case review repository.
Criminal justice reports
Fatal investigation reports for suspected suicide deaths in detention were obtained from the Prisons and Probation Ombudsman (PPO) website. The PPO notified the study of the publication of any fatal investigation reports of apparent suicide deaths in custody in people aged under 20 years, that occurred between 1 January 2014 and 28 February 2015 and were available to download from their website. After 1 March 2015, the name of the deceased remains in the fatal investigation report, so additional notifications were not required to search for reports. The Prisoner Ombudsman for Northern Ireland investigates deaths in prison service custody in the province and the report of these investigations are published on their website. We obtained seven criminal justice reports from these sources.
National Confidential Inquiry into Suicide and Safety in Mental Health data
The National Confidential Inquiry into Suicide and Safety in Mental Health (NCISH) collects UK-wide data on all current or former patients who die by suicide within 12 months of contact with mental health services. Data is collected in three steps: (a) information on general population suicide deaths are obtained from national data providers; (b) from these data, patients in contact with mental health services are identified by mental health providers; and (c) a senior professional responsible for the patient's care completes a questionnaire about the patient, including clinical information. Details of the NCISH methodology are published elsewhere.18 We obtained NCISH data for 115 (19%) of the 595 young people who died by suicide in the study period.
National Health Service serious incident reports
If death by suicide of a patient was identified from NCISH data, serious incident reports (or serious adverse incident report or critical incident review) describing an internal investigation of the patient's death were obtained from the medical director of the treating National Health Service (NHS) Trust or Health Board. We were able to access 97 such reports.
Procedures
A structured pro forma was used to extract information on the antecedents of suicide in children and young people from the data sources described above. Detailed information on study design, including the extraction of data items and definitions, have been previously published.Reference Rodway, Tham, Ibrahim, Turnbull, Kapur and Appleby19,Reference Rodway, Tham, Richards, Turnbull, Kapur and Appleby20 For this study, information about demographic and social characteristics, and specific information relevant to self-harm was extracted. The selection of information to be extracted was determined a priori from the research literature on self-harm,Reference Chan, Bhatti, Meader, Stockton, Evans and O'Connor17 and included excessive alcohol use; illicit drug use; mental health history; any history of sexual, emotional and/or physical abuse; any recent life adversity within the 3-month period before death (including relationship breakup, being a victim of a violent crime, bereavement, accommodation, health or finance-related problems) and service contact. Blood levels of antidepressant and antipsychotic medications recorded in toxicological analysis, usually conducted as part of the coroner's investigation for the inquest, were used to determine if a young person was taking psychotropic medication at the time of death. These data items were recorded if they were referred to as being present at any time in the young person's life and specifically in the 3 months before their death (referred to as ‘recent’). Reference to self-harm from any data source was recorded and coded into the following variables: (a) no history of self-harm, (b) recent self-harm (in the 3 months before death) and (c) lifetime self-harm (more than 3 months before death).
Statistical analysis
Stata 16 software was used for analysis. We suppressed cell counts under three including zero, in line with ONS guidance on disclosure control to protect confidentiality. Results for all UK nations were combined. The denominator in all estimates was the total number of individuals on which at least one report was obtained (N = 544), unless otherwise specified. If an antecedent (e.g. mental health diagnosis) was not mentioned in any data source, we assumed that it was unlikely to have been present and recorded it as absent or not relevant to the individual death. Country-specific deprivation quintiles were generated from postcode data for England, Wales and Scotland, obtained for each young person who died by suicide, using the English Indices of Multiple Deprivation, Welsh Index of Multiple Deprivation, Scotland Index of Multiple Deprivation and Northern Ireland Multiple Deprivation Measure.21–24 Each young person's neighbourhood of residence was allocated into deprivation quintiles, having ranked the raw scores within their own nations, with quintile 1 being the most deprived to 5 being the least deprived. Pearson's χ 2-test was used to test for associations between the following subgroups of young people who died by suicide: those who self-harmed within the 3 months before death (referred to as recent self-harm hereafter), those who did not self-harm and those who self-harmed more than 3 months before death (referred to as lifetime self-harm).
Separate χ 2-tests were conducted to compare lifetime self-harm and recent self-harm versus no self-harm as a common reference category, generating two P-values independent of one another. Log binomial regression models adjusted for gender, age and deprivation quintile (to adjust for the confounding effects of the known risk factors for self-harm) were used to examine the association between self-harm and various risk factors in the three self-harm subgroups.Reference Hawton, Saunders and O'Connor9 Odds ratios with 95% confidence intervals were estimated. The lifetime self-harm and no self-harm groups were used as the baseline group and compared with the recent self-harm group in the models. A P-value of <0.05 (two-sided) was considered statistically significant in all results.
Ethics statement
The authors assert that all procedures contributing to this work comply with the ethical standards of the relevant national and institutional committees on human experimentation and with the Helsinki Declaration of 1975, as revised in 2013. All procedures involving human patients were approved by the National Research Ethics Service Committee North-West (Greater Manchester South, UK; approval number 15/NW/0184). Exemption under Section 251 of the NHS Act 2006, enabling access to confidential and identifiable information without informed consent in the interest of improving care, was obtained from the Health Research Authority Confidentiality Advisory Group (identifier 15/CAG/0120) and the Public Benefit and Privacy Panel for Health and Social Care (identifier 1617–0107).
Results
During the 3-year study period (2014–2016), 595 young people aged 10–19 years died by suicide in the UK. Information on the antecedents of suicide was received from one or more data sources for 544 (91%) individuals. A history of self-harm was recorded for 49% (n = 267) of these 544 deaths, equating to approximately 89 deaths by suicide per year. Of the 267 young people with a history of self-harm, recent self-harm was recorded in 139 (52%; 26% of the whole sample), equating to 46 deaths per year, and a lifetime history in 128 (48%; 24% of the whole sample), equating to 43 deaths per year. There was no recorded history of self-harm (recent or lifetime) in 277 (51%) of the 544 young people who died by suicide.
Sociodemographic and clinical characteristics of young people who self-harm before suicide
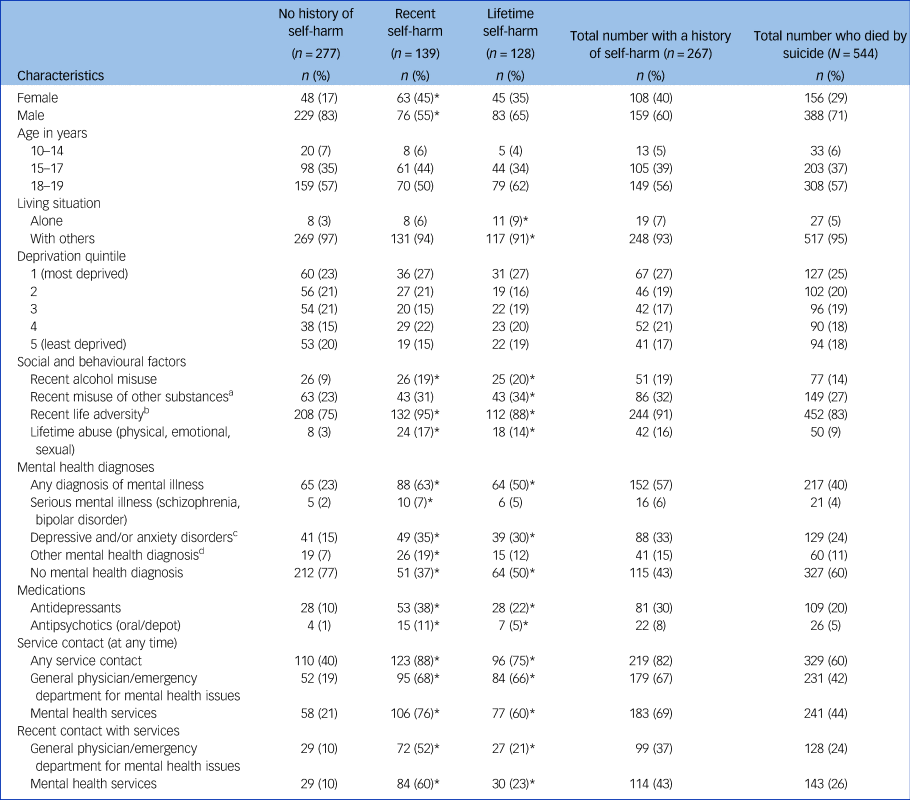
Of the 267 young people with a history of self-harm, 159 (60%) were male and 108 (40%) were female (Table 1). Girls were more likely than boys to have a history of self-harm before suicide (69 v. 41%; P < 0.001), including recent self-harm (40 v. 20%; P < 0.001). Over half (57%) were aged 18–19 years. There were no significant differences in the proportion of young people with a history of self-harm according to age (Table 1). Living alone was rare (n = 19, 7%); 27% of young people who self-harmed lived in the most deprived areas of England, Wales, Scotland and Northern Ireland, and 17% lived in the least deprived areas.
Characteristics of children and young people with a history of self-harm who died by suicide, 2014–2016

a. Includes heroin and other opiates, stimulants (e.g. amphetamines, LSD, cocaine, ecstasy), benzodiazepines (other than as prescribed), cannabis and new psychoactive substances.
b. Includes relationship break-up, problems/arguments with partner/family/peers, being a victim or perpetrator of violent crime or sexual abuse, bereavement, and accommodation, workplace or financial problems.
c. Includes depressive illness, anxiety disorder, obsessive–compulsive disorder, post-traumatic stress disorder, phobia and panic disorder.
d. Includes eating disorder, alcohol dependence/misuse, drug dependence/misuse, personality disorder, adjustment disorder, intellectual disability, pervasive development disorder, attention-deficit hyperactivity disorder, conduct disorder and where a mental disorder was present but diagnosis unknown.
* P < 0.05: lifetime self-harm and recent self-harm groups were compared with the no self-harm group (reference category).
Recent illicit drug use (particularly cannabis use; n = 86, 32%) was more common than alcohol misuse in young people with a history of self-harm (Table 1). For 91%, there was evidence of recent life adversity in the form of relationship problems with family and/or friends, physical ill health, accommodation and financial problems. A total of 16% had experienced abuse.
Of the entire sample, 152 (57%) young people with a history of self-harm had a diagnosis of mental illness, most often depression and/or anxiety disorders (n = 88, 33%; Table 1). Few had diagnoses of autism spectrum disorder (n = 10, 4%) or attention-deficit hyperactivity disorder (n = 10, 4%). Overall, 33% of young people were being prescribed psychotropic medications (either antidepressants or antipsychotics); 14% (n = 47) were being prescribed medication without a recorded mental illness diagnosis. We did not have access to information on whether any young people were receiving psychological intervention for self-harm before death.
Service contact
For 219 (82%) young people who self-harmed, there had been contact with specialist services or agencies at some time; most often with mental health services (n = 183, 69%). Recent contact with services (in the 3 months before death) was recorded for 156 (58%) young people, most often with mental health services (n = 114, 43%), but also included contact with the youth justice system (n = 64, 24%). Overall, 99 (37%) young people had seen their general practitioner or were seen in a hospital emergency department for issues related to their mental health in the 3 months before death.
Young people with recent self-harm
Table 1 presents the antecedents of suicide in young people with a history of recent self-harm, with no history of self-harm and a lifetime history of self-harm as comparators. Several antecedents of suicide varied in frequency depending on the recency of self-harm before suicide. Recent life adversity was reported more frequently in young people who had recently self-harmed (95%) compared with those with lifetime self-harm (88%) and no known self-harm history (75%). Alcohol misuse and a history of abuse were also more likely to be reported in the recent self-harm group when compared with both no known self-harm and lifetime self-harm groups (Table 1). Illicit drug misuse was comparable across recent self-harm and no self-harm groups, but was significantly higher in the lifetime self-harm group when compared with the no self-harm group.
Young people who recently self-harmed were more likely to have a diagnosis of mental illness compared with both the no known self-harm and lifetime self-harm groups. The likelihood of being prescribed antidepressant medication was also higher among young people with a history of recent self-harm compared with no reported or lifetime self-harm. Evidence of being prescribed antipsychotic medication was uncommon (n = 22 in the overall self-harm sample), but more likely in the recent self-harm group (11%) than the no reported (1%) or lifetime self-harm (5%) groups.
For 123 (88%) of young people with a recent history of self-harm who died by suicide, there had been contact with specialist services or agencies at some time; most often with mental health services (n = 106, 76%). Young people who had recently self-harmed were more likely than those with no reported history of self-harm to have had contact with mental health services (60 v. 10%), an emergency department contact or a consultation with a general physician for a mental health condition (52 v. 10%) in the 3 months before death (Table 1).
Recent history of self-harm versus no history of self-harm
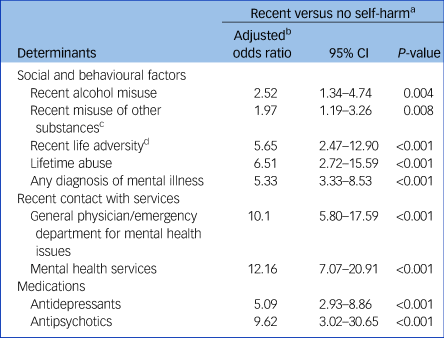
After adjustment for age, gender and small area deprivation quintile, young people with a recent history of self-harm were more likely than young people with no history of self-harm to report recent life adversity, abuse, a diagnosis of mental illness, a history of alcohol and/or drug misuse, recent contact with mental health services or a general practitioner or an emergency department for mental health issues, and having received medication in the form of antidepressants or antipsychotics. However, the confidence interval was wide for antipsychotic medication (odds ratio 13.93, 95% CI 3.02–30.65) because of the small number of young people with a history of self-harm (n = 22) being prescribed these drugs (Table 2).
Adjusted odds ratios for potential social, behavioural and clinical determinants among children and young people who died by suicide with no history of self-harm versus recent self-harm

a. Using ‘no history of self-harm’ as the baseline.
b. Log binomial regression model adjusted for age, gender and deprivation quintile.
c. Includes heroin and other opiates, stimulants (e.g. amphetamines, LSD, cocaine, ecstasy), benzodiazepines (other than as prescribed), cannabis and new psychoactive substances.
d. Includes relationship break-up, problems/arguments with partner/family/peers, being a victim or perpetrator of violent crime or sexual abuse, bereavement, and accommodation, workplace or financial problems.
Recent history of self-harm versus lifetime history of self-harm
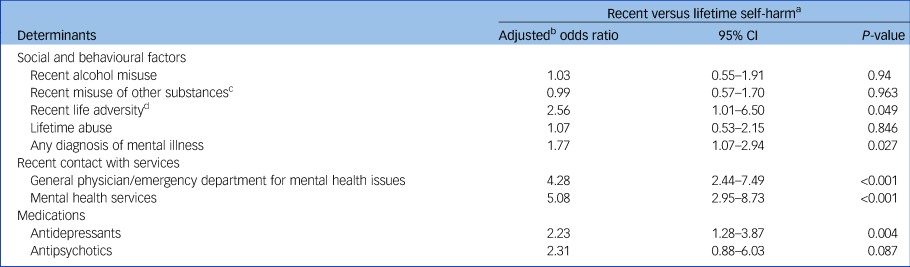
Recent life adversity, a diagnosis of mental illness, receiving antidepressants and recent service contact were also more likely to be reported by young people with a recent history of self-harm compared with those with a lifetime history, after adjustment for age, gender and deprivation quintile (Table 3).
Adjusted odds ratios for potential social, behavioural and clinical determinants among children and young people who died by suicide with recent self-harm versus lifetime self-harm

a. Using ‘lifetime history of self-harm’ as the baseline.
b. Log binomial regression model adjusted for age, gender and deprivation quintile.
c. Includes heroin and other opiates, stimulants (e.g. amphetamines, LSD, cocaine, ecstasy), benzodiazepines (other than as prescribed), cannabis and new psychoactive substances.
d. Includes relationship break-up, problems/arguments with partner/family/peers, being a victim or perpetrator of violent crime or sexual abuse, bereavement, and accommodation, workplace or financial problems.
Discussion
Our findings show that self-harm is common in young people who go on to die by suicide. Almost half of young people who died by suicide in a 3-year period (2014–2016) had harmed themselves at some point in their lives. A quarter had harmed themselves recently (in the 3 months preceding their death). Young people who reported recent self-harm had a clustering of other risk factors. They were more likely to have experienced sexual, emotional or physical abuse, to have a diagnosed mental health condition and to have experienced recent life adversity compared with young people with no known history of self-harm. Furthermore, our findings indicate that most young people with recent self-harm who died by suicide had presented to services for help. This represents an important opportunity to intervene.
We found over a third of young people with a history of recent self-harm had a diagnosis of depressive or anxiety disorder; a quarter had other mental health diagnoses, including schizophrenia, bipolar disorder, personality disorder and eating disorder. The prevalence of psychiatric disorders that we observed in our recent self-harm group, however, is less than that seen in young people (up to the age of 25 years) presenting to general hospitals following an episode of self-harm (63 v. 81%).Reference Hawton, Saunders, Topiwala and Haw25 Our use of medical evidence heard during a coroner inquest (i.e. clinical diagnoses) as opposed to research diagnostic tools (such as the Structured Clinical Interview for DSM Disorders) could be one of the reasons for the observed differences, as could the younger age range (19 v. 24 years). Another possibility is the underreporting of mental health diagnoses in our study, including of neurodivergent or developmental conditions such as attention-deficit hyperactivity disorder, which were rarely reported.
We also found evidence for considerable service contact in young people with self-harm who died by suicide (82%), especially in the recent self-harm group (88%). Service presentations, an important indicator of help-seeking in adolescents before suicide, were higher in our study when compared with other studies. For example, in a Norwegian study using national registry data, only 23% of 10- to 19-year-olds who died by suicide between 2008 and 2018 had contact with mental health services in the year before their death, as opposed to 26% (60% from recent self-harm group) in our sample within 3 months of their death.Reference Astrup, Myhre, Kildahl and Walby26 Recent contact with specialist services or agencies, especially with mental health services, was much more apparent in the recent self-harm group compared with those with no or a lifetime (more than 3 month) history of self-harm. An association between suicide in young people in recent contact with mental health services has previously been reported, especially in young female patients aged under 25 years.27
Our findings suggest an elevated risk of suicide in young people who self-harm and presented to a range of other specialist services and agencies, including primary care, emergency departments, criminal justice agencies and social care. Any such presentation to health, social care or other support services following self-harm by a young person is an opportunity to intervene.Reference Geulayov, Casey, McDonald, Foster, Pritchard and Wells5 However, there is a need to improve support for young people who have self-harmed both in high-income and low- and middle-income countries, where there is limited evidence for the availability of services and interventions for self-harm.2,Reference Cooper, Steeg, Bennewith, Lowe, Gunnell and House28,Reference Aggarwal, Patton, Berk and Patel29
Identifying the short-term risk of suicide in young people who present with self-harm is vital for prevention. This would require adequate training opportunities for the staff working within mental health services, where suicide risk may be being underestimated at assessment, but also for staff in non-healthcare settings, who may benefit from training in risk recognition and management of self-harm in accordance with national guidelines.12,Reference Saunders, Hawton, Fortune and Farrell30 Effective training in self-harm and suicide awareness has been shown to have a positive effect on staff attitudes toward self-harm in young people who may otherwise feel patronised, not listened to or even stigmatised by front-line staff.Reference Saunders, Hawton, Fortune and Farrell30–Reference Aggarwal, Borschmann and Patton32
Many of the young people in our sample, especially in the recent self-harm group, had a clustering of risks (e.g. alcohol misuse, childhood abuse and mental ill health); this comorbidity likely added to suicide risk, but may also have been a reason for non-acceptance by services typically designed for single conditions.Reference Saini, Kullu, Mullin, Boland and Taylor33 Prevention could be aided through age-appropriate expert care and support for young people with co-existing conditions, such as mental illness and substance misuse, with self-harm services being crucial for both groups. Our findings also underscore the importance of following existing NICE guidelines for self-harm management. These guidelines recommend a comprehensive psychosocial assessment at the earliest opportunity after presenting to health services with self-harm, by a mental health professional experienced in assessing young people.12 An individualised assessment of risks and needs of young people presenting to services following self-harm is crucial in reducing future suicide risk.Reference Hawton, Zahl and Weatherall14 Such an assessment should carefully explore any psychosocial and interpersonal stressors, and life events, such as problems with a relationship, housing, loss of employment or bereavement, in addition to evaluating mental health problems and substance misuse. This could help in guiding the service response through appropriate referrals to drug and alcohol services or social care.
Although we do not know from our study how many young people with a recent history of self-harm who died by suicide were receiving support in the form of psychological interventions, we do know that half had taken psychotropic medications at the time of death, as evidenced from a toxicological analysis. The place of pharmacological interventions in the treatment of young people with psychiatric disorders is controversial. NICE guidelines recommend medications should not be used as a treatment for self-harm and should not be a first-line treatment for mild common mental disorders in young people, although they do allow for drug treatment in moderate to severe depression with concurrent psychological therapy.12,34 Shared decision-making to discuss and review all current and any new medicines is also recommended after an episode of self-harm. Many of the young people in our sample were prescribed antidepressants and antipsychotics, but our study was not designed to investigate the appropriateness of such prescribing.
NICE guidelines recommend using safety plans to help people who have self-harmed, to identify and use their strengths and sources of support to overcome crisis moments and prevent repeat self-harm.12 Given the clustering of risks evident in our sample, there is evidence that flexible psychological treatments aligned to the needs of and taking into account the life situations of young people are likely to be more effective than standard treatments.12,Reference Aggarwal, Patton, Berk and Patel29,Reference Witt, Hetrick, Rajaram, Hazell, Taylor Salisbury and Townsend35 The integration of psychological treatments into managing and preventing the recurrence of self-harm in young people is in line with NICE and other global recommendations for self-harm and suicide prevention.12,Reference Witt, Hetrick, Rajaram, Hazell, Taylor Salisbury and Townsend35,Reference World Health Organization36
According to a recent Cochrane review, individual cognitive–behavioural therapy-based psychotherapy and dialectical behaviour therapy adapted for young people are the most promising interventions for self-harm in children and adolescents.Reference Witt, Hetrick, Rajaram, Hazell, Taylor Salisbury and Townsend35 The review recommends more trials to dismantle effect sizes between one or more components of the available interventions. In clinical settings, standalone skills learning groups (e.g. emotion regulation skills groups) for young people at high risk of self-harm and suicidal behaviours can be used when resources are scarce.Reference Durpoix, Lachaux, Weiner and Weibel37
About half (51%) of the young people in our study who died by suicide had no recorded history of self-harm. This group also had lower rates of other risk factors for suicide, such as alcohol and drug misuse, recent life adversity, and service contact. Rodway et al have previously reported that there are a substantial minority of young people who had shown no direct signs of distress such as expressing suicidal ideas or self-harm before death by suicide, and that a different approach to prevention may be needed for this group.Reference Rodway, Tham, Turnbull, Kapur and Appleby38 Our findings reiterate the importance of teaching young people about emotional awareness through school and university-based peer support programmes, public health awareness campaigns and the media, and sensitising professionals, schools and families to recognise lesser degrees of risk among young people. Low-intensity public health programmes (i.e. minimum intensity designed to change) with broader reach and universal coverage, such as the Youth Aware of Mental Health Programme used in Saving and Empowering Young Lives in Europe study (SEYLE) across European schools, can reduce suicidal behaviours in young people by improving their coping skills in the face of life adversities.Reference Wasserman, Hoven, Wasserman, Wall, Eisenberg and Hadlaczky39 Equally important is crisis services being widely available and accessible when the risk escalates.12
Strengths and limitations
Information for the study came mainly from coroners who independently take evidence from families, friends and professionals in contact with the young person before their death, as well as other sources. However, we acknowledge several limitations of our use of these sources. First, because the data we used were not designed for research purposes, we were unable to obtain complete and consistent data on, for example, the type and quality of psychological treatments or supports received by young people preceding or following self-harm. Given that dialectical behaviour therapy adapted for young people is recommended for some young people who self-harm, further research on the psychological interventions received by young people who died by suicide may be warranted.12 Second, blood levels of medications found during toxicological analysis for the coroner investigation were used to determine whether a young person was taking psychotropic medication at the time of death. It is likely that some young people may not have taken medication as prescribed. Third, we assumed that any data items that were not reported in our data sources (e.g. abuse) were unlikely to have been present in the young person's life, and were thus considered as absent or not relevant to the individual death. Some factors, particularly in sensitive areas (e.g. abuse), may therefore be underreported. Fourth, this was an observational case series study with no control group. Since our study was a retrospective examination of self-harm in young people who had died by suicide, it would be difficult to find a comparable control group with equivalent sources of data. This is because there is no easy source of equivalent data on non-suicide controls. It would necessitate a general population control group on who equivalent data are available. The fact of suicide itself and the impact of suicide on disclosure can distort any comparison.Reference Hawton, Appleby, Platt, Foster, Cooper and Malmberg40 A controlled study would also be difficult given the ethical implications in contacting families. Fifth, the information used in this study was derived from secondary data sources (mainly coroner inquests) and we did not conduct new investigations. Although this was not a psychological autopsy study, it was doing something very similar by using the same sources (i.e. families) but relying on interviews conducted by others (i.e. the coroner). Psychological autopsy studies are best suited to small area research where there are fewer challenges with recruiting informants for a representative sample. We do acknowledge, however, that some families have benefited from the experience of being interviewed about the suicide of a loved one.Reference Dyregrov, Dieserud, Hjelmeland, Straiton, Rasmussen and Knizek41 Sixth, our findings cannot be linked causally to suicide. However, the adversities that we have described were taken from personal narrative, which were discussed at inquest, implying the informant or coroner felt they were relevant to the young person's death. Seventh, our study was not designed to explore the potential protective factors in suicide such as positive peer/familial relationships, life satisfaction, a sense of belonging, positive parenting and emotional regulation. The information would have been difficult to collect using the data sources that we used. More research in the area can help us generate definitive evidence for the protective effects of these factors, which in turn, can guide the future suicide prevention efforts in young people.
To summarise, suicide and self-harm rates in young people in the UK have risen over the past decade.10,11 Improving support for children and young people and people who have self-harmed are priorities for suicide prevention in England in the next 5 years.2 We have shown that recent self-harm is common in young people who subsequently die by suicide. Also evident was a clustering of other common risk factors for suicide, including contact with services. Each encounter should be seen as an opportunity to intervene. The findings underscore the importance of assessing and managing self-harm in young people in accordance with NICE guidelines. Addressing the multiple risks that cluster in young people who self-harm, such as mental ill health, alcohol misuse and the traumatic effects of childhood abuse, including through comprehensive and individualised psychosocial assessment and a range of interventions to address the different kinds of comorbidities and life problems we found, are also needed to help prevent suicide in this age group. Addressing the key social determinants of suicide in young people, such as poverty and deprivation, alcohol and drug use, interpersonal violence and childhood abuse, as well as insecurity in jobs and housing, lack of or fears about opportunity, and demand for healthcare that services are struggling to meet, are also integral to suicide prevention.
Data availability
All authors had full access to all the data in the study and take responsibility for the integrity of the data and the accuracy of data analysis. Data from this study cannot be shared because of information governance restrictions in place to protect confidentiality. Access to data can be requested via application to the Healthcare Quality Improvement Partnership (www.hqip.org.uk/national-programmes/accessing-ncapop-data/).
Acknowledgements
We thank coroners and their staff, the Crown Office and Procurator Fiscal Service, Child Death Overview Panels and their respective Local Safeguarding Children's Boards, Medical Directors and administrative staff at NHS Trusts/health boards, and the Prisons and Probation Ombudsman for the provision of data; and members of the NCISH research team: Isabelle Hunt, Alison Baird, Jane Graney, Lana Bojanić, Rebecca Lowe, James Burns, Philip Stones and India Garry. We are grateful to Jessica Raphael, prior Senior Research Associate for Greater Manchester Mental Health NHS Foundation Trust, for her help with data acquisition. We are also grateful to our reference group members for offering advice on data items.
Author contributions
S.A., C.R., S.-G.T., S.I., L.A. and N.K. were responsible for study conception and design. C.R. and S.-G.T. were responsible for data acquisition. S.A., S.-G.T., S.I., C.R. and R.T.W. were responsible for data analysis and interpretation. S.A. wrote the first draft of the manuscript and S.A., C.R., S.-G.T., R.T.W., S.I. and N.K. were involved in writing subsequent drafts and finalising the manuscript. C.R., L.A., P.T. and R.T.W. provided guidance to the study. All authors read and approved the final manuscript and were jointly responsible for the decision to submit for publication. L.A. is the guarantor for the study.
Funding
The study was commissioned by the Healthcare Quality Improvement Partnership on behalf of NHS England, the Welsh Government, the Scottish Government Health and Social Care Directorate, the Northern Ireland Department of Health, and the States of Jersey and Guernsey, and was carried out as part of the National Confidential Inquiry into Suicide and Safety in Mental Health. The funders of the study had no role in study design; in the collection, analysis and interpretation of data; in the writing of the manuscript; or in the decision to submit the paper for publication. R.T.W. is funded by the National Institute for Health and Social Care (NIHR) Manchester Biomedical Research Centre (grant number NIHR203308). R.T.W. and N.K. are funded by the NIHR Greater Manchester Patient Safety Research Collaboration (grant number NIHR204295). N.K., L.A. and P.T. report grants from the Healthcare Quality Improvement Partnership and NHS England. N.K., L.A., P.T. and C.R. report grants from the Department for Education and the MPS Foundation. P.T. reports a grant from the Gambling Research Exchange Ontario. The views expressed are those of the author(s) and not necessarily those of the funding agencies.
Declaration of interest
L.A. is Chair of the National Suicide Prevention Strategy Advisory (NSPSA) Group at the Department of Health and Social Care in England; N.K. is a member of the Group, works with NHS England on national quality improvement initiatives for suicide and self-harm, chaired the guideline development group for the 2012 UK National Institute for Health and Clinical Excellence (NICE) guidelines on the longer term management of self-harm and the guideline development group for the 2022 NICE guideline on depression in adults, and was a topic advisor for the 2022 NICE guideline on self-harm: assessment, management and preventing recurrence. Views expressed in the paper are those of the authors and not those of the NICE or the Department of Health and Social Care. N.K. is a member of the British Journal of Psychiatry Editorial Board, but did not take part in the review or decision-making process of this paper. All other authors declare no other relationships or activities that could appear to have influenced the submitted work.




eLetters
No eLetters have been published for this article.