Introduction
Otitis media with effusion (OME) is often diagnosed in children evaluated for obstructive sleep apnoea syndrome (OSAS) due to adenotonsillar hypertrophy. However, it is unclear whether such effusion is caused by the hypertrophied adenoid pad, and whether adenoidectomy is sufficient for its remission. Adenoidectomy has been shown to increase the likelihood of restoration of normal middle-ear functionReference Black, Sanderson, Freeland and Vessey1, Reference Gates, Avery, Prihoda and Cooper2 and to reduce the need for further tympanostomy tube insertions.Reference Coyte, Croxford, McIsaac, Feldman and Friedberg3, Reference Kadhim, Spilsbury, Semmens, Coates and Lannigan4 However, it has not been proven to improve hearing.Reference Black, Sanderson, Freeland and Vessey1, Reference Lous, Burton, Felding, Ovesen, Rovers and Williamson5 Other studies have failed to show a significant effect of adenoidectomy on the occurrence of otitis media (recurrent or chronic).Reference Hammaren-Malmi, Saxen, Tarkkanen and Mattila6–Reference Casselbrant, Mandel, Rockette, Kurs-Lasky, Fall and Bluestone8 Moreover, children with adenoid hypertrophy were either excluded or inadequately reported in these studies, even though adenoid hypertrophy often coexists with OME.
Tympanostomy tube insertion, on the other hand, is the most commonly used surgical treatment for OME and the second most common operation worldwide (second only to circumcision).Reference Lous9 Although tympanostomy tube insertion improves the quality of life of children with OME,Reference Rosenfeld, Bhaya, Bower, Brookhouser, Casselbrant and Chan10 some researchersReference Lous9 have suggested that a restriction of operative criteria is necessary due to the procedure's possible adverse effects.
In the current study, we sought to evaluate the benefits of adenoidectomy plus tympanostomy tube insertion versus adenoidectomy plus simple myringotomy, in the treatment of OME in children with OSAS and adenoid hypertrophy. A randomised trial was conducted for this purpose.
Materials and methods
Participants
The study was approved by the Scientific and Ethics Committee of the Aghia Sophia Children's Hospital of Athens.
Children were eligible for inclusion in the study if they were scheduled for an adenoidectomy due to sleep-disordered breathing, were older than three years of age and had otitis media with effusion (OME) in both ears.
The diagnosis of OME was based on otoscopy, tympanography and pure tone audiometry. Specifically, the presence of an opaque or thickened tympanic membrane, air–fluid level, or bubbles, or the inability to visualise the incudostapedial joint, were considered signs of OME, in children with a type B tympanogram (compliance <0.2 ml) and an audiogram with an air–bone gap of 20 dB or a hearing loss of 30 dB but no more than 55 dB in at least one frequency in both ears. Absence of the light reflex was not regarded as a specific sign of OME.
Children with no signs of effusion (purulent or otherwise) at the time of myringotomy were excluded from the study. We also excluded children with chronic otitis media, structural changes (e.g. tympanic membrane retraction pockets, ossicular chain erosion or cholesteatoma), previous ear surgery, language delays, behavioural problems and syndromes.
Diagnoses of OME were made and surgical procedures were performed by the same surgeon. Patients were recruited by four experienced pediatric ENT specialists.
Diagnosis of adenoid hypertrophy was based on clinical and radiological (i.e. lateral neck X-ray) examination, and was confirmed at operation.
Intervention
The children were allocated into two groups, to receive either adenoidectomy plus tympanostomy tube insertion (group one) or adenoidectomy plus myringotomy (group two). Adenoidectomy was performed with the use of mirrors. Curetting and suction cautery were used for haemostasis when necessary. Tympanostomy tubes were of the Shepard type. Both groups of children also received ‘cold steel’ tonsillectomy.
Objectives and outcome measures
The primary outcome was each patient's total score for the OM-6. This is a validated, disease-specific questionnaire assessing the effects of OME on quality of life. Scores range from one to seven, with higher values indicating a poorer quality of life. Questionnaires were administered one day pre-operatively and six and 12 months post-operatively. A small percentage of patients (<15 per cent) who were unavailable for direct clinical examination post-operatively completed their questionnaires via telephone interview.
Pure tone audiometry was performed one day pre-operatively and six and 12 months post-operatively. Mean hearing losses at five frequencies (250, 500, 1000, 2000 and 4000 Hz) were recorded for each ear. Follow-up audiograms were performed in about 60 per cent of patients, as demonstrated in Table I. Missed audiological examinations were due to occasional unavailability of resources within the audiology department. However, these patients were not excluded from the study as audiological results constituted a secondary outcome.
Patients' mean hearing loss 6 and 12 mths post-operatively

*AT group mean HL − AM group mean HL. Mths = months; HL = hearing loss; AT group = adenoidectomy plus tympanostomy tubes; AM group = adenoidectomy plus myringotomy; pts = patients; SD = standard deviation
At the time of myringotomy, otoscopy was used to classify middle-ear effusions as serous (i.e. thin and watery) or mucoid (i.e. thick and viscous). The presence and status of the tympanic membrane and the patency of the tympanostomy tube were evaluated six and 12 months post-operatively.
The obstructive sleep disorders-6 (OSD-6), a validated, disease-specific questionnaire designed to assess patients' obstructive disordered breathing, was administered one day pre-operatively and six months post-operatively.
Each patient's age and gender and the season of their operation were also recorded.
Randomisation
Patients were allocated to the two treatment groups using a computer-generated sequence. Random allocation was stratified by season.
Statistical methods
We used t-tests and paired t-tests for comparison of continuous variables, as required. Possible predictors of OME remission one year after the initial operation were incorporated as independent variables, in a multivariable analysis, by use of logistical regression models. Odds ratios for each factor were adjusted for possible confounding by all other factors in the model.
Results and analysis
Patient recruitment took place between May 2007 and May 2008. Patient follow up terminated in June 2009. A total of 52 patients participated in the study (group one, n = 25; group two, n = 27). Five children from group one and six children from group two were lost during follow up.
The baseline characteristics of each group are listed in Table II. No statistically significant difference in baseline characteristics could be identified between the two groups.
Patients' baseline characteristics
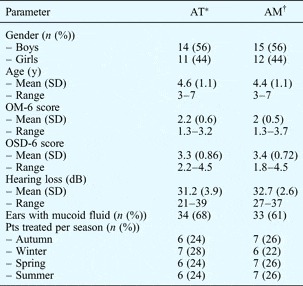
*n=25; †n = 27. AT = group receiving adenoidectomy plus tympanostomy tubes; AM = group receiving adenoidectomy plus myringotomy; y = years; SD = standard deviation; OM-6 = otitis media-6; OSD-6 = obstructive sleep disorders-6; pts = patients
Outcomes
Six months after surgery, the mean OM-6 score for group one had changed significantly (p < 0.05), compared with the pre-operative value.
For each of the two groups, the mean six month post-operative ?? score significantly differed from the pre-operative score (p < 0.05), as would be expected following adenoidectomy in children suffering from obstructed, sleep-disordered breathing.
Six months post-operatively, a statistically significant difference was seen in patients' OM-6 scores (the primary outcome), compared with pre-operative scores (mean score difference −0.38, confidence interval −0.65 to −0.10). However, 12 months post-operatively (i.e. at the end of the trial period), the mean OM-6 score difference was no longer statistically significant (mean score difference −0.23, confidence interval −0.76 to 0.11) (Table III). Differences in audiological outcomes did not reach statistical significance, as seen in Table I.
Patients' OM-6 scores 6 and 12 mths post-operatively

*AT mean score − AM mean score. OM-6 = otitis media-6; mths = months; AT = group receiving adenoidectomy plus tympanostomy tubes; AM = group receiving adenoidectomy plus myringotomy; CI = confidence interval; SD = standard deviation
Adverse events
Four children (20 per cent) in group two underwent tympanostomy tube insertion due to persistent effusion. These children were not excluded from the study, since total quality of life was the primary outcome measure. Tympanostomy tube insertion was not associated with a specific season. None of the children in group one suffered tube-related complications (e.g. otorrhoea or chronic tympanic membrane perforation) during the follow-up period.
Ancillary analyses
Logit regression showed that, when adjusted for age, gender, ear fluid viscosity and operation type, children who underwent surgery during the summer months had a better prognosis than those undergoing surgery during autumn (p = 0.029), in terms of recurrence or persistence of otitis media with effusion one year post-operatively (Table IV).
Predictors of OME recurrence or remission one year post-operatively

Odds ratio (OR) and 95% confidence interval (CI) for each variable obtained from logit regression models adjusted for all variables in the table. *Ear fluid viscosity.
Discussion
To date, several trials have been conducted to study the effect of tympanostomy tube insertion versus simple myringotomy or no treatment, in children receiving concurrent adenoidectomy.Reference Black, Sanderson, Freeland and Vessey1, Reference Dempster, Browning and Gatehouse11–Reference To, Pahor and Robin16 Although comparisons are difficult due to differences in inclusion criteria, study periods and assessed outcomes, a recent Cochrane meta-analysis concluded that simple myringotomy appeared to offer no benefit, compared with no treatment.Reference Lous, Burton, Felding, Ovesen, Rovers and Williamson5 Moreover, studies of the combined effect of adenoidectomy and tympanostomy tube insertion found an additional benefit of only 3–4 dB (95 per cent confidence interval 2–5 dB) at six months, compared with the ear without tympanostomy tube.Reference Lous, Burton, Felding, Ovesen, Rovers and Williamson5 Twelve months after surgery, these same patients had only a 1–2 dB hearing improvement (95 per cent confidence interval 0.1–2.8 dB), compared with the ear without a tympanostomy tube.Reference Lous, Burton, Felding, Ovesen, Rovers and Williamson5 Two years after adenoidectomy in both ears plus tympanostomy tube insertion in one ear, no significant difference was observed between the two ears.Reference Lous, Burton, Felding, Ovesen, Rovers and Williamson5
In the present, randomised study, we confirmed the long term results found by previous studies regarding audiological outcomes in children receiving adenoidectomy plus tympanostomy tube insertion versus adenoidectomy plus myringotomy. Our study findings also provided information on pre- and post-operative health-related quality of life. Most importantly, we compared the effects of the aforementioned procedures in children with OSAS and otitis media with effusion (OME), a subgroup not adequately studied in previous studies.
In children with OSAS and demonstrably large adenoids, the effect of adenoidectomy upon OME may be greater than that in the general population of children with OME but no upper airway obstruction. The underlying pathophysiological mechanism may be eustachian tube dysfunction or a bacterial focus. Our patients' otitis media recurrence rates did not differ significantly from those reported in a recently published study of children without diagnosed OSAS.Reference Popova, Varbanova and Popov17
Limitations of the study
The most important limitation of the current study was probably the small number of patients included. An equivalence study would require a far greater number of patients in order to successfully address several possible confounding factors, such as parental smoking, number of older siblings, preterm delivery, birth weight, breast-feeding, socioeconomic class, blood group and history of allergy. We also emphasise the importance of multi-centre, randomised trials in allowing subgroup analysis. Nevertheless, a recent epidemiological study conducted in a nearby region found that the aforementioned factors did not affect the persistence or recurrence of middle-ear fluid.Reference Xenellis, Paschalidis, Georgalas, Davilis, Tzagaroulakis and Ferekidis18
In the current study, the duration of middle-ear effusion was not known in the majority of cases, since the primary reason for surgery was obstructed breathing and the average waiting period from diagnosis to operation was one month. It would have been impractical to request a minimum three-month ‘watchful waiting’ period, as recommended by most OME treatment guidelines. Instead, we recorded the season of operation as an indirect indication of the effusion duration. Several epidemiological studies have found that persistence of middle-ear fluid is significantly associated with the season of diagnosis.Reference Xenellis, Paschalidis, Georgalas, Davilis, Tzagaroulakis and Ferekidis18, Reference van Balen and de Melker19 This was also shown in our study.
The appropriateness of the health-related quality of life questionnaire used in this study is also of concern. Although the OM-6 is a validated and convenient research tool, it is rather short in length, with only six items. Thus, the statistically insignificant difference in OM-6 total scores, comparing pre-operative versus one year post-operative values, may require verification with a more extended validated questionnaire.
• Adenoid hypertrophy and otitis media with effusion (OME) often coexist in children
• Several trials have shown that adenoidectomy plus tympanostomy tube insertion confers only short term benefit, compared with each procedure alone, as regards OME remission
• This prospective study randomly allocated 52 children with obstructive sleep apnoea syndrome (OSAS) to receive either adenoidectomy plus tympanostomy tubes or adenoidectomy plus myringotomy
• The former treatment conferred only short term benefit over the latter treatment
Finally, blinding constitutes another important issue. Inclusion in the trial itself may have biased the outcomes by increasing the anxiety of parents whose children had not received tympanostomy tubes during the initial operation. However, such request (not to let the parents know whether their children were offered or not a tympanostomy tube) might have been regarded as unethical or impractical. A randomisation based on right versus left ear rather than on the ears of different children would probably have provided some sort of solution to this problem; however, middle-ear status can differ within the same individual, and the two ears are too independent to use the contralateral ear as a control.Reference van Heerbeek, Akkerman, Ingels, Engel and Zielhuis20 On the other hand, this kind of randomisation would have impeded participation in the trial, due to cultural inhibitors in the referred population. Similar reasons, together with hesitation on the part of the surgeons, inhibited the inclusion of a third ‘watchful waiting’ control group.
Conclusion
Children with adenoid hypertrophy and otitis media with effusion (OME) are commonly encountered in paediatric otolaryngology departments. However, they are usually excluded from clinical trials of the effect of adenoidectomy upon OME.Reference Ruben21 This study, despite its limitations, showed a short term benefit for tympanostomy tube insertion in children with OSAS and OME. Nevertheless, tympanostomy tube insertion may be a sensible option for two paediatric patient groups: children receiving operative treatment during the autumn (since they are at greater risk of OME recurrence), and very young children, as shown by previous studies.Reference Casselbrant, Mandel, Rockette, Kurs-Lasky, Fall and Bluestone8, Reference Valtonen, Tuomilehto, Qvarnberg and Nuutinen22 Further study is required to identify which children with OSAS will derive more prolonged benefit from tympanostomy tube insertion. Moreover, more subtle but perhaps still clinically significant differences may emerge from a network meta-analysis of relative randomised trials. At the time of writing, an individual patient data meta-analysis of the effectiveness of adenoidectomy was being undertaken by the University of Utrecht (C. Boonacker, personal communication), aiming to improve the low power of subgroup analyses.
Acknowledgements
We thank Professor Rosenfeld RM and Dr Liamme de Serres for their kind provision of the OM-6 and OSD-6, respectively. We also thank Chantal Boonacker for her valuable comments.





