Introduction
Treatments for delusions need to be significantly improved. One approach is to use recent advances in understanding their causes to develop more precisely targeted interventions (e.g. Freeman, Reference Freeman2011; Foster, Startup, Potts and Freeman, Reference Foster, Startup, Potts and Freeman2010; Moritz et al., Reference Moritz, Kerstan, Veckenstedt, Randjbar, Vitzthum and Schmidt2011; Waller, Freeman, Jolley, Dunn and Garety, Reference Waller, Freeman, Jolley, Dunn and Garety2011; Myers, Startup and Freeman, Reference Freeman2011; Lincoln, Hohenhaus and Hartmann, Reference Lincoln, Hohenhaus and Hartmann2012). There is also increasing recognition of the need to improve the social recovery of individuals with psychotic experiences (e.g. Fowler et al., Reference Fowler, Hodgekins, Painter, Reilly, Crane and Macmillan2009). In the current report we describe preliminary work that attempts to link theoretical advances, social recovery, and intervention development.
A substantial epidemiological literature has established that rates of psychosis are higher in urban areas (e.g. McGrath et al., Reference McGrath, Saha, Welham, El Saadi, MacCauley and Chant2004; Sundquist, Frank and Sundquist, Reference Sundquist, Frank and Sundquist2004; Krabbendam and van Os, Reference Krabbendam and van Os2005; Kelly et al., Reference Kelly, O'Callaghan, Waddington, Feeney, Browne and Scully2010). This association with urbanicity also applies to milder non-clinical psychotic-like experiences (e.g. van Os, Hanssen, Bijl and Vollebergh, Reference Van Os, Hanssen, Bijl and Vollebergh2001; Scott, Chant and McGrath, Reference Scott, Chant, Andrews and McGrath2006), including paranoid thinking (e.g. Johns et al., Reference Johns, Cannon, Singleton, Murray, Farrell and Brugha2004; Freeman et al., Reference Freeman, McManus, Brugha, Meltzer, Jenkins and Bebbington2011). One hypothesis proposed to explain the link is that a high level of competition enhances the likelihood of social defeat, which then acts as a stressor (Selten and Cantor-Graae, Reference Selten and Cantor-Graae2005). At a clinical level, patients with persecutory delusions frequently find entering social environments difficult because of their fears of harm. They then avoid going out into busy places in order to minimize threat and the anxious feelings they experience (Freeman et al., Reference Freeman, Garety, Kuipers, Fowler, Bebbington and Dunn2007). In an experimental study, patients with persecutory delusions who went into a busy urban environment showed increases in anxiety and paranoia compared with staying inside (Ellett, Freeman and Garety, Reference Ellett, Freeman and Garety2008). Anxiety is hypothesized to have a central role in the development of paranoid fears: it causes anticipation of threat, worry, and greater use of safety behaviours (Freeman, Reference Freeman2007). Overall, it is plausible that in outside urban environments it is the presence of many people, the heightened stimulus environment, and the stress and anxiety generated that exacerbates paranoia, thereby limiting the social contact of people with psychosis.
On the basis of this epidemiological, theoretical and experimental literature we set out to design a brief intervention specifically focused on helping patients with persecutory delusions feel less distressed when entering busy social urban environments. The aim was to target the anxiety-related cognitive processes that activate the persecutory threat belief. We wished to normalize the stress of urban environments, identify the specific aspects of the environment responsible, highlight how this leads to anxiety and its multiple effects on our minds, bodies and behaviour, and derive strategies to reduce the distress of being outside. We report the first feasibility tests of this intervention, examining the effects of going outside into a busy local street before and after the intervention. We predicted that the intervention would lessen the distress of being outside. A participant group was selected that reported repeated difficulties going outside locally in order to lessen any potential simple habituation effects. However, this initial evaluation of the new intervention did not use a control comparison, meaning that if any clinical change did occur it may not be due to the content of the module.
Method
Participants
Eighteen participants were recruited from Oxleas NHS Foundation Trust, the South London and Maudsley NHS Foundation Trust, Camden and Islington NHS Foundation Trust, and Barnet, Enfield and Haringey Mental Health Trust. The inclusion criteria were: a current persecutory delusion meeting the criteria of Freeman and Garety (Reference Freeman and Garety2000); 50% or greater conviction in the persecutory belief; reports of anxiety in going outside; aged 18 to 65; and a case note diagnosis of schizophrenia, schizo-affective disorder or delusional disorder. Three suitable participants withdrew before the start of the study (providing no data): one patient developed a physical health condition, one patient began working and couldn't attend appointments, and one patient did not attend the appointments offered.
Design
Ethical approval was received from the NHS Research Ethics Service. A simple pre and post design was used to test feasibility and acceptability. There was no control group or control condition. In the first session, lasting approximately 90 minutes, the participants were assessed by the clinician, and completed ratings of symptoms before and after going outside into a local busy street on an approximately 10-minutes return trip. The street chosen was dependent upon where the person lived. All patients then received the intervention on a second occasion. This lasted 2–3 hours, but could be split into two meetings. On the immediate completion of the intervention the patients then repeated the walk into the local street, with symptom measures again being taken before and after the exposure.
The intervention
The intervention (called, “Getting Out and About”) (see Figure 1) was presented individually on a computer, with a clinical psychologist present. Patients were encouraged to go through the programme themselves, stopping for frequent discussion with the therapist. The message of the opening slides was that cities can be stressful and anxiety provoking. A slide with stressful aspects of walking down a street was presented, highlighting, for example, the noise, speeding vehicles, dirt and litter, CCTV cameras, and people walking about. Each aspect could be clicked on the screen to show a picture or video of this aspect of urban environments. The aspects patients found difficult were identified and discussed. The next set of slides highlighted the effects of feeling anxious. This included physiological (e.g. increased heart rate, shortness of breath, feelings of unreality), cognitive (e.g. anticipating threat, worry, focus on threat), and behavioural effects (e.g. a range of safety behaviours including avoidance, escape, keeping vigilant for danger). The specific anxiety effects for the individual patients were discussed. Importantly, the therapist then highlighted how, in this anxious state, fears about the intentions of other people would be likely to occur i.e. paranoid thoughts. A simple formulation was then put together. Key boxes linked by arrows were: Going outside, Triggers, Anxiety, Effects of anxiety, Worries about others, Increased anxiety. The summary leading on to the new strategies was:
The trouble is that being outside on the street can make us anxious. The anxiety makes us anticipate danger, focus on threat, worry, and feel in danger. This will lead us to overestimate how much danger we are actually in. We could be safer than we think.
Examples of slides from the intervention module “Getting Out and About”

Six strategies were then presented on a menu. The therapist provided brief explanations of each, in order to see which the patient would be most interested in trying. Two or three strategies were then looked through in detail on the computer by clicking on the icon. The six strategies were: 1) Taking our minds off fears (changing focus of attention); 2) Letting go of suspicious thoughts (adopting a mindful approach to fearful thoughts); 3) Changing distressing images (imagery work); 4) Coping with worries about difficult situations (decatastrophizing fears); 5) Changing our behaviours (dropping safety behaviours); and 6) Thinking positively (positive self-talk). After a collaborative discussion about how to employ the strategies, patients were then encouraged to try one or two strategies next time they went outside on to the street. A coping card was written as a reminder of the strategy.
Measures
The assessments were first completed inside, and then repeated outside at the end of the walk in the street. Nine visual analogues scales (0–100) were used to assess how anxious the person was currently feeling, how much they were feeling under threat, the level of paranoid thinking (a mean score from five items: I am being deliberately harmed or upset; I am being followed; There is a conspiracy against me; I am being persecuted; I am being laughed at behind my back), the degree of conviction in the persecutory delusion, and the degree of distress associated with the delusion. The State Social Paranoia Scale (SSPS; Freeman et al., Reference Freeman, Pugh, Green, Valmaggia, Dunn and Garety2007) was also completed before and after going outside. To assess acceptability, three further visual analogue scales were completed at the end of the study assessing on 0 to 10 scales the degree to which participants found the intervention useful, interesting, and enjoyable.
Statistical analysis
Analyses were carried out using SPSS Version 20.0.0 (IBM, 2011). For the main analysis, change scores from pre to post were calculated for each occasion of going outside (i.e. to determine the effects on one occasion of going into the street), and these were then compared for the two occasions (pre and post intervention) using paired sample t-tests. Significance test results for all the analyses are quoted as two-tailed probabilities. We did not alter significance levels for multiple testing, agreeing with the view that “simply describing what tests of significance have been performed, and why, is generally the best method of dealing with multiple comparisons” (Perneger, Reference Perneger1998).
Results
The patient group
The mean age of the participants was 41.4 (SD = 9.1) years old. Nine were male, and six female. The ethnicities of the participants were: White British (n = 9), Black British (n = 3), and other (n = 3). They had diagnoses of schizophrenia (n = 13) and schizo-affective disorder (n = 2). The mean length of illness was 9.6 (SD = 11.2) years.
Comparison of responses when outside
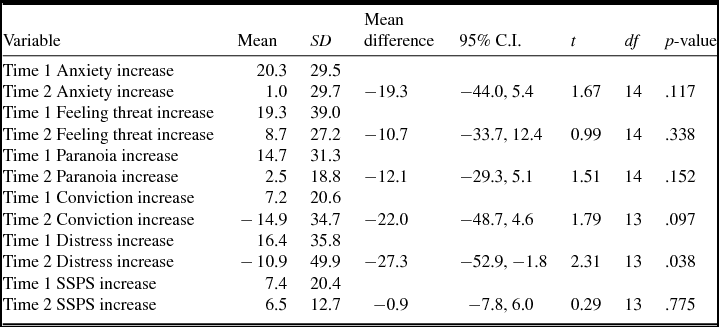
It can be seen from Table 1 that on the first occasion of going outside there were increases in symptoms. There was then a uniform and sizeable attenuation of the increase in symptoms at the second time of entering the street scene. For levels of delusional conviction and distress there was a decrease in scores upon going outside on the second occasion. However, the change in symptoms was only statistically significant in relation to the distress associated with the delusion (p < .05; effect size = 0.76). In other words, the mean increase in distress associated with going outside on the first occasion was reduced significantly on the second occasion.
Differences between symptom ratings before and after going outside on each occasion
Acceptability of the intervention
The mean patient rating of the usefulness of the intervention was 8.7 on the 10-point scale (SD = 1.5. minimum = 6, maximum = 10), with seven patients endorsing the top of the scale. The mean patient rating for how interesting the intervention was found was 8.5 (SD = 1.4, minimum = 6, maximum = 10), with six patients endorsing the top of the scale. The mean rating for the enjoyability of the intervention was also favourable, at 7.9 (SD = 1.9, minimum = 5, maximum = 10), with five patients endorsing the top of the scale.
Discussion
There is a clinical need to develop interventions that help patients with persecutory delusions feel better able to cope when outside with strangers present. This intervention drew on the theoretical links between urbanicity, stress and anxiety, and paranoia. Being outside in busy urban environments causes stress and anxiety, which are factors linked to the occurrence of paranoid thoughts. The study was an initial feasibility evaluation of the intervention for patients reporting consistent difficulties going outside. Going outside after delivery of the brief intervention was clearly associated with less anxious and paranoid responses. Indeed, after the intervention levels of distress decreased from the rating obtained before going out to the rating obtained after spending time outside (indicating the effects of anticipatory anxiety). However, as there was no control group, the effects cannot be causally attributed to the intervention, and one plausible explanation is that reductions were simply due to the repeat exposure. On the other hand, the patients were entering environments they had been in many times previously with persistent difficulty, and habituation is less likely to occur when safety behaviours remain in place (Salkovskis, Reference Salkovskis1991; McManus, Scadura and Clark, Reference McManus, Scadura and Clark2008). Standard CBT for psychosis therefore relies upon behavioural tests of beliefs rather than simple exposure techniques (e.g. Key, Craske and Reno, Reference Key, Craske and Reno2003). The patients themselves viewed the intervention as useful.
The general approach therefore shows promise, and merits a controlled test. However, we also carried out the study in order to learn about the intervention and the methodology of testing it. The patients seemed able to use visual analogue scales both inside and outside in the street, and the scales appeared sensitive to change. However, there was notable variability in symptomatic responses to going outside, even although the group was selected for self-reporting difficulties in such situations. For instance, on the first occasion of going out four patients did not endorse any of the five paranoia items. This might be due to a discrepancy between anticipation and the actual experience (although these four patients also did not endorse the paranoid beliefs before going out). Equally, the patients might have felt safer because of the research context. This clearly weakened the power of the study to find significant effects, but also makes evaluating the outcome of the intervention in this way more difficult. For a larger scale evaluation it may be important to include measures taken outside the research context, for example, examining going out in the flow of daily life using experience sampling methodology (Myin-Germeys et al., Reference Myin-Germeys, Oorschot, Collip, Lataster, Delespaul and van Os2009) or diary records of the number of times the person has gone out. Multiple different measures can raise the risk of Type 1 error, although the ideal is to see convergence in change across outcome assessments. It would also be an innovation to use mobile technologies to deliver elements of the intervention whilst the person is actually outside (Ben-Zeev, Davis, Kaiser, Krzos and Drake, Reference Ben-Zeev, Davis, Kaiser, Krzos and Drake2012). We found great interest expressed by the patients in the intervention and its aims, and consider that the length of time spent should be lengthened. It would be valuable to have at least four sessions, which would allow for the trying out of a number of techniques, practice, and consolidation. The patients in the study had typically experienced for many years difficulties going outside and the effectiveness of the intervention in an early episode group would clearly be of interest. In our experience across a number of recent studies (e.g. Foster et al., Reference Foster, Startup, Potts and Freeman2010; Myers et al., Reference Myers, Startup and Freeman2011), interventions focused on a single outcome and of an acceptable duration can prove both popular and effective with patients with delusions.
Acknowledgements
The research was funded by a Wellcome Trust grant (No. 085396). DF is supported by a UK Medical Research Council (MRC) Senior Clinical Fellowship. PG and EK receive support from the Biomedical Research Centre, South London and Maudsley NHS Foundation Trust. There are no conflicts of interest.




Comments
No Comments have been published for this article.