Introduction
Severe fatigue and insomnia are common symptoms in many long-term medical conditions (Budhiraja et al., Reference Budhiraja, Roth, Hudgel, Budhiraja and Drake2011; Menting et al., Reference Menting, Tack, Bleijenberg, Donders, Droogleever Fortuyn, Fransen, Goedendorp, Kalkman, Strik-Albers, van Alfen, van der Werf, Voermans, van Engelen and Knoop2018; Sarsour et al., Reference Sarsour, Morin, Foley, Kalsekar and Walsh2010). Fatigue is the central feature of myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS), which is characterised by severe and persistent medically unexplained fatigue leading to functional impairment (Fukuda et al., Reference Fukuda, Straus, Hickie, Sharpe, Dobbins and Komaroff1994; Reeves et al., Reference Reeves, Lloyd, Vernon, Klimas, Jason, Bleijenberg, Evengard, White, Nisenbaum and Unger2003). Insomnia is central to insomnia disorder (ID), which is defined as persistent complaining of dissatisfaction with sleep quantity or quality, with significant related daytime consequences (American Academy of Sleep Medicine, 2014). Both conditions have an adverse impact on health and societal costs (Daley et al., Reference Daley, Morin, LeBlanc, Gregoire and Savard2009; Katz and McHorney, Reference Katz and McHorney2002; Morroy et al., Reference Morroy, Keijmel, Delsing, Bleijenberg, Langendam, Timen and Bleeker-Rovers2016; Sarsour et al., Reference Sarsour, Kalsekar, Swindle, Foley and Walsh2011). Severe fatigue and insomnia often co-occur; 89% of ME/CFS patients report insomnia symptoms (Fossey et al., Reference Fossey, Libman, Bailes, Baltzan, Schondorf, Amsel and Fichten2004) and 74% of ID patients report severe fatigue (Van Houdenhove et al., Reference Van Houdenhove, Buyse, Gabriels and Van den Bergh2011).
Both fatigue and insomnia are symptoms with multi-factorial origins. Cognitive behavioural models of fatigue and insomnia do not make assumptions about the aetiology of symptoms, but rather postulate cognitive behavioural factors that can maintain the symptom (Harvey, Reference Harvey2002; Spielman et al., Reference Spielman, Nunes and Glovinsky1996; Vercoulen et al., Reference Vercoulen, Swanink, Galama, Fennis, Jongen, Hommes, van der Meer and Bleijenberg1998). There is considerable overlap in these models.
For example, a disrupted sleep–wake rhythm with napping during the day is assumed to maintain fatigue, but is also thought to perpetuate insomnia (Harvey, Reference Harvey2002; Spielman et al., Reference Spielman, Nunes and Glovinsky1996; Vercoulen et al., Reference Vercoulen, Swanink, Galama, Fennis, Jongen, Hommes, van der Meer and Bleijenberg1998). As a result, CBT for fatigue (CBT-F) and insomnia (CBT-I) have certain elements in common (Knoop and Bleijenberg, Reference Knoop and Bleijenberg2010; Verbeek and van de Laar, Reference Verbeek and van de Laar2015): they overlap with regard to sleep interventions aimed at restoring the circadian rhythm and improving sleep hygiene. Other than these, CBT-I does not include further elements of CBT-F or vice versa. For a comprehensive description of the elements of both therapies, see Appendix A.
Both CBT-F and CBT-I are effective interventions leading to a reduction of their target symptom following treatment (Adamson et al., Reference Adamson, Ali, Santhouse, Wessely and Chalder2020; Castell et al., Reference Castell, Kazantzis and Moss-Morris2011; Malouff et al., Reference Malouff, Thorsteinsson, Rooke, Bhullar and Schutte2008; van Straten et al., Reference van Straten, van der Zweerde, Kleiboer, Cuijpers, Morin and Lancee2018; Wiborg et al., Reference Wiborg, van Bussel, van Dijk, Bleijenberg and Knoop2015). Yet do these therapies retain their effectiveness when severe fatigue and insomnia co-occur? There are indications that CBT-I remains effective for patients with severe fatigue (Ramfjord et al., Reference Ramfjord, Faaland, Scott, Saksvik, Lydersen, Vedaa, Kahn, Langsrud, Stiles, Ritterband, Harvey, Sivertsen and Kallestad2023). Whether CBT-F remains effective in treating fatigue in the presence of co-morbid insomnia has not been investigated before. Co-morbid insomnia might negatively influence the treatment outcome of CBT-F as this has been shown to be the case with mental disorders (Seow et al., Reference Seow, Verma, Mok, Kumar, Chang, Satghare, Hombali, Vaingankar, Chong and Subramaniam2018).
Evidence exists that, apart from treating their target symptom, CBT-F and CBT-I can also have a positive effect on co-occurring symptoms. CBT-F can lead to improvements in subjective sleep quality in patients with ME/CFS (Russell et al., Reference Russell, Kyle and Wearden2017) and CBT-I to moderate improvements in fatigue (Benz et al., Reference Benz, Knoop, Ballesio, Bacaro, Johann, Rucker, Feige, Riemann and Baglioni2020). However, in these previous studies no information was available as to whether the co-occurring symptom (respectively insomnia and fatigue) was present at a clinically relevant level post-treatment. This would be important to know, as additional interventions may still be required.
The first aim of this study was to determine whether the co-occurrence of severe fatigue and insomnia influences treatment outcomes of CBT-F and of CBT-I on their target symptom. The second aim was to determine whether changes in fatigue and in insomnia are correlated in CBT-F and in CBT-I. The third aim was to investigate how many patients still report clinically relevant levels of the co-occurring symptom post-treatment when the target symptom is no longer present at a clinically relevant level. We investigated the effects of CBT-F on patients with ME/CFS and the effects of CBT-I on patients with ID.
Method
Study design
This was an observational study conducted in routine clinical care, with a pre- and post-treatment study design. We used data from two cohorts of patients: (1) a cohort with fatigue as primary complaint: patients with a primary diagnosis of ME/CFS treated with CBT-F; and (2) a cohort with insomnia as primary complaint: patients with a primary diagnosis of ID treated with CBT-I. In each cohort we compared subgroups of patients experiencing only the primary symptom with those reporting co-occurrence of severe fatigue and insomnia at baseline.
Participants
Group with fatigue as primary complaint
Data from 241 ME/CFS patients were used, collected as part of routine clinical care at a tertiary chronic fatigue treatment centre at the Amsterdam University Medical Centre, The Netherlands. Consecutively referred patients aged ≥ 18 years, who (1) met the Centers for Disease Control and Prevention (CDC) case definition for ME/CFS, revised in 2003 (Reeves et al., Reference Reeves, Lloyd, Vernon, Klimas, Jason, Bleijenberg, Evengard, White, Nisenbaum and Unger2003), (2) scored ≥ 35 on the subscale fatigue of the Checklist Individual Strength (CIS-fat) and scored > 700 on the Sickness Impact Profile-8 (SIP-8), (3) started CBT-F between July 2019 and December 2022 and (4) followed at least two sessions of CBT-F, were included. According to the CDC case definition of ME/CFS, a somatic explanation for fatigue was ruled out. The presence of clinical insomnia was not an inclusion criterion.
Of the 241 included patients, 175 (73%) also met the recently formulated case definition Systemic Exertion Intolerance Disease (SEID) criteria (Clayton, Reference Clayton2015) proposed by the Institute of Medicine (IOM) as an alternative for the CDC case definition. See Appendix B for descriptions of the two different case definitions. Of the 241 included patients, 233 (97%) completed the CIS-fat post-treatment and 221 (92%) the Insomnia Severity Index (ISI). There was no statistically significant difference between the patients who did and did not fill out the questionnaires post-treatment on any of the demographic or clinical variables at baseline or on number of treatment sessions.
Group with insomnia as primary complaint
Data from 162 ID patients were used, collected as part of routine clinical care at the Department of Medical Psychology of the Multidisciplinary Sleep-Wake Centre of Hospital Gelderse Vallei, Ede, The Netherlands. Consecutively referred patients aged ≥18 years who (1) met the criteria for ID according to the International Classification of Sleep Disorders-3 (ICSD-3) (American Academy of Sleep Medicine, 2014), (2) scored ≥ 10 on the ISI (Morin et al., Reference Morin, Belleville, Belanger and Ivers2011), (3) started CBT-I between October 2018 and December 2021, and (4) followed at least two session of CBT-I, were included. The presence of severe fatigue was not an inclusion criterion.
Of the 162 included patients, 142 (88%) completed the CIS-fat post-treatment and 141 (87%) completed the ISI. Those who filled out the questionnaires post-treatment had significantly more CBT-I sessions than those who did not (M = 5.5, SD = 1.5 vs M = 6.7, SD = 0.6 sessions, p < 0.001). They did not differ at baseline on any of the demographic or clinical variables.
Interventions
CBT-F was provided according to the protocol of CBT for ME/CFS (Knoop and Bleijenberg, Reference Knoop and Bleijenberg2010), which included modules on goal setting, sleep–wake pattern, helpful thinking with respect to fatigue and the ability to become more active, graded activity and realising goals. Optional modules on social support and pain coping were also available. CBT-I was provided according to the Dutch CBT-I protocol (Verbeek and van de Laar, Reference Verbeek and van de Laar2015), which included goal setting, psycho-education on sleep and sleep hygiene, behavioural techniques, and helpful thinking with respect to sleep and relaxation. For a detailed description of the content of CBT-F and CBT-I, see Appendix A.
Both CBT-F and CBT-I were delivered by psychologists. CBT-F was delivered individually and started with a face-to-face intake. Treatment was provided blended, i.e. a combination of face-to-face consultations, video consultations and email contact. Treatment duration according to protocol is 6–9 months, usually 14 sessions, the first sessions weekly.
CBT-I was delivered in a group format with 3–10 participants. There were six weekly sessions of CBT-I of 75–120 minutes, depending on the group size. A final, seventh session of the CBT-I was scheduled 4–6 weeks later as a booster. During the COVID-19 regulations, CBT-F and CBT-I were delivered via video consultations. Previous studies have shown that video consultation and online therapy interventions are effective therapy formats for CBT-F and CBT-I (Boinon et al., Reference Boinon, Charles, Fasse, Journiac, Pallubicki, Lamore, Ninot, Guerdoux-Ninot, Gouy, Albiges, Delaloge, Malka, Planchard, Savard and Dauchy2021; Janse et al., Reference Janse, Worm-Smeitink, Bleijenberg, Donders and Knoop2018).
Measures
Fatigue and insomnia severity were assessed before the start of the treatment and post-treatment. All measures were self-reported, either by paper and pencil, or online.
Demographics
We obtained data on sociodemographic variables (age, gender, medical co-morbidity) and use of sleep medication from medical records.
Fatigue severity
Fatigue was assessed with the CIS-fat (Worm-Smeitink et al., Reference Worm-Smeitink, Gielissen, Bloot, van Laarhoven, van Engelen, van Riel, Bleijenberg, Nikolaus and Knoop2017). The subscale consists of eight items scored on a 7-point Likert-scale (total score range from 8 to 56). Patients rate fatigue severity experienced in the previous 2 weeks. A total score of ≥ 35 indicates the presence of severe fatigue (Worm-Smeitink et al., Reference Worm-Smeitink, Gielissen, Bloot, van Laarhoven, van Engelen, van Riel, Bleijenberg, Nikolaus and Knoop2017).
Insomnia severity
Insomnia severity was measured with the ISI (Morin et al., Reference Morin, Belleville, Belanger and Ivers2011), a 7-item questionnaire scored on a 5-point Likert scale reflecting the self-reported severity of both night-time and daytime aspects of insomnia disorder in the previous 2 weeks. Total scores range from 0 (no insomnia) to 28 (severe insomnia). A total score of ≥ 10 is used to define clinical insomnia (Buysse et al., Reference Buysse, Ancoli-Israel, Edinger, Lichstein and Morin2006).
Sample size
We powered the study on the first research question. In order to detect a medium difference (Cohen’s d = 0.5) in post-treatment fatigue/insomnia severity between the co-occurrence subgroup and the no co-occurrence subgroup at baseline with 80% power and a 2-sided alpha of 0.05, we would need a total sample size of 64 patients per subgroup in each of the two patient groups (Johnson et al., Reference Johnson, Rash, Campbell, Savard, Gehrman, Perlis, Carlson and Garland2016).
Statistical analysis
Statistical analyses were performed using SPSS 28.0 (SPSS Inc. Chicago, IL, USA). Each patient group was divided in two subgroups: a subgroup with only the target symptom at a clinically relevant level and a subgroup with clinical levels of co-occurring fatigue (CIS-fat ≥ 35) or insomnia (ISI ≥ 10) at baseline. Demographics, clinical characteristics and outcomes are presented in means (standard deviations) and numbers (percentages) depending on their distribution. We used chi-square tests and t-tests to compare the subgroups in each patient group. In the case of significant differences in any of the demographic variables we controlled for that variable in the subsequent analysis.
To investigate whether treatment outcomes differed between subgroups, we used analysis of covariance (ANCOVA) with the subgroup as the independent variable and baseline scores as covariates. We calculated mean between group differences with 95% confidence intervals (CI). Mean between-group differences in fatigue and insomnia severity were expressed in Cohen’s d effect size by dividing the mean difference by the pooled standard deviation post-treatment, with values of 0.2, 0.5 and 0.8 indicating a small, moderate and large effect, respectively (Cohen, Reference Cohen1992). We checked whether violations of assumptions of normality, linearity and homoscedasticity were present. To investigate whether treatment outcomes between subgroups differed in terms of the presence of the target symptom (yes/no) post-treatment, we used logistic regression analysis with the subgroup as independent variable.
To investigate whether a change in the co-occurring symptom (when severe at baseline) was related to a change in the target symptom, we correlated the change scores from insomnia and fatigue by calculating the Pearson correlation coefficient (r).
In the group of patients no longer experiencing the target symptom post-treatment, we calculated the prevalence of patients still reporting clinically relevant levels of the co-occurring symptom post-treatment.
Multiple imputation was used to account for participants who had missing values post-treatment. The imputation model included gender, age, number of treatment sessions, medical co-morbidity, medication use (for the ID patients), presence of the co-occurring symptom at a clinically severe level and the outcome variables pre- and post-treatment and their change scores. A total of five datasets were imputed and were pooled according to Rubin’s rules (Rubin, Reference Rubin1987).
We analysed data separately for ME/CFS patients meeting SEID criteria (Clayton, Reference Clayton2015). Outcomes for patients meeting the SEID criteria that were significantly different from the outcomes of all included ME/CFS patients were reported. p-values of < 0.05 (2-tailed) were considered to be statistically significant.
Results
Participants
Table 1 presents the demographic and clinical characteristics and treatment duration of the ME/CFS group and the ID group, both divided into two subgroups with and without co-occurring symptoms. Appendix C presents the prevalence of medical conditions according to the 11th revision of the International Classification of Diseases (ICD-11) (World Health Organization, 2022).
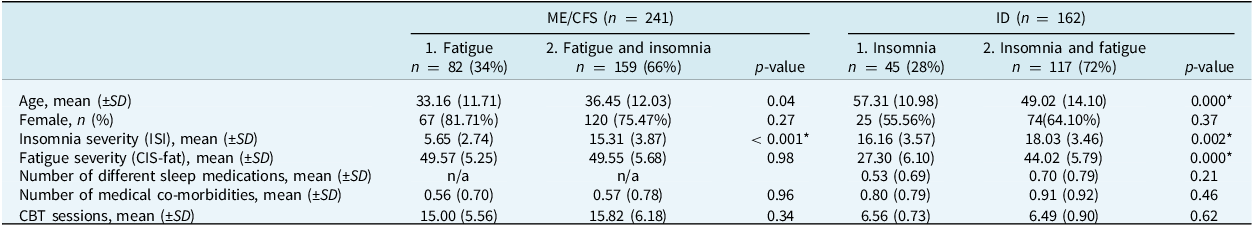
Demographic and clinical characteristics at baseline and treatment duration of the ME/CFS and the ID group, divided in subgroups of co-occurring severe fatigue and insomnia versus no co-occurring symptoms

*p < 0.05. CIS-fat, Checklist Individual Strenght-20, subscales fatigue severity; ISI, Insomnia severity Index. Severe fatigue: CIS-fat ≥ 35; severe insomnia: ISI ≥ 10.
Group with fatigue as primary complaint: ME/CFS
Of the 241 patients, 159 (66%) reported co-occurring clinical insomnia (ISI ≥ 10) at baseline and 82 (34%) did not. The mean (SD) insomnia severity in the subgroup with co-occurring insomnia was 15.31 (SD = 3.87) on the ISI, indicative of moderate insomnia (ISI > 14) (Morin et al., Reference Morin, Belleville, Belanger and Ivers2011). As part of clinical care all ME/CFS patients were asked to stop any sleep medication, so sleep medication use was absent in this group. They reported 0–3 medical co-morbidities, including co-morbid sleep-related breathing disorders (n = 6; 2%) and restless legs syndrome (n = 2; 1%); see Appendix C. The patients reporting co-occurring clinical insomnia at baseline were older (p = 0.04) than the patients without clinical insomnia at baseline, but there were no differences in other patient characteristics or in number of treatment sessions (range 4–38). We controlled for age in the subsequent analyses.
Group with insomnia as primary complaint: ID
Of the 162 patients, 117 (72%) reported co-occurring severe fatigue (CIS-fat ≥ 35) at baseline and 45 (28%) did not. The mean (SD) fatigue severity in the subgroup with co-occurring severe fatigue was 44.02 (SD = 5.79) on the CIS-fat. Patients used between 0 and 4 different types of sleep medication (including benzodiazepine, melatonin, sedating anti-depressant and quetiapine). They reported 0–2 medical co-morbidities, including co-morbid sleep-related breathing disorders (n = 16; 10%) and circadian rhythm sleep–wake disorders (n = 7; 4%). Patients reporting both severe insomnia and fatigue at baseline were significantly younger (p < 0.001) than the participants who experienced only insomnia. They also experienced more severe insomnia symptoms (p = 0.002). The two subgroups (with and without co-occurring symptoms of insomnia and fatigue) did not differ in other baseline characteristics or in treatment duration. We controlled for age in the subsequent analyses.
Treatment outcome of CBT on the target symptom in the case of co-occurring symptoms
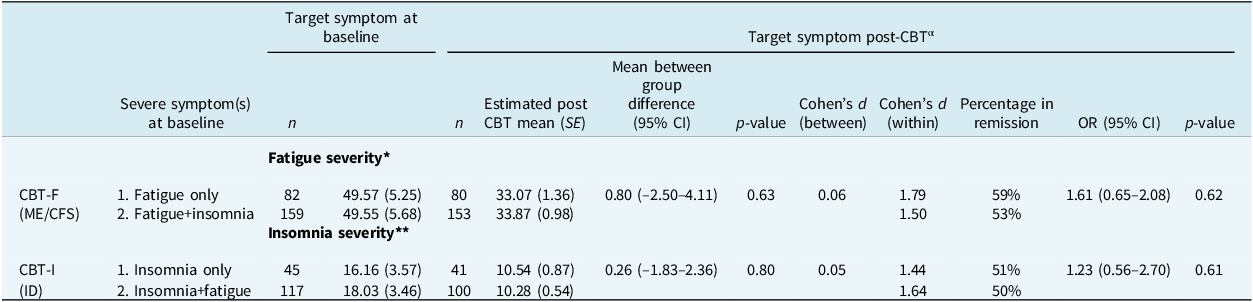
Table 2 presents the outcomes on the target symptom of CBT-F and CBT-I for subgroups with and without co-occurring severe fatigue and insomnia at baseline. For ME/CFS patients treated with CBT-F, no statistically significant difference was found between patients with and without co-occurring insomnia with respect to the mean CIS-fatigue-score post-treatment (p = 0.63, d = 0.06). For ID patients treated with CBT-I, the mean ISI-score post-treatment did not differ between patients being severely fatigued at baseline and patients without severe fatigue at baseline (p = 0.80, d = 0.05). All subgroups demonstrated large within-effect sizes (respectively d = 1.8 and 1.5 for CBT-F and 1.4 and 1.6 for CBT-I). Furthermore, for both ME/CFS and ID patients, no statistically significant difference was found between patients with and without co-occurring severe fatigue or insomnia regarding the percentage of patients for whom the target symptom was in remission post CBT (respectively 59 vs 53%, p = 0.62 for CBT-F and 51 vs 50%, p = 0.61 for CBT-I).
Pre- and post-treatment means and percentages in remission of the target symptom

αControlled for age and severity of target symptom at baseline. *Checklist Individual Strength-20, subscales fatigue severity (CIS-fat); in remission: CIS-fat ≤ 35. **Insomnia severity Index (ISI); in remission: ISI ≤ 10.
Association between change in insomnia and fatigue severity after CBT
For the ME/CFS and the ID patients who experienced co-occurring symptoms at baseline, a change in insomnia severity after CBT was associated with a change in the same direction in fatigue severity (r = 0.30, p < 0.001, n = 221 in CBT-F and r = 0.50, p < 0.001, n = 100 in CBT-I). See Fig. 1 for the scatterplot of the ISI change score and the CIS-fat change score in both therapies. In CBT-F the explained variance was 9% and in CBT-I 25%.
Scatterplot of the fatigue severity (CIS-fat) change score and insomnia severity (ISI) change score (both pre–post treatment scores) at CBT-F and CBT-I. A more positive change score represents a higher reduction of severity.

Prevalence of clinical severity of the co-occurring symptom after treating the target symptom
Of the ME/CFS patients experiencing both severe fatigue and insomnia at baseline but who were no longer severely fatigued post-CBT-F (n = 81), 25 (31%) still reported severe insomnia post-treatment. Of the ID patients experiencing both severe fatigue and insomnia at baseline but who no longer reported clinical insomnia post CBT-I (n = 50), 12 (24%) still reported severe fatigue post-treatment.
Repeating the analysis with the imputed dataset showed the same pattern of results (data not shown).
Discussion
This study investigated the implications of the co-occurrence of severe fatigue and insomnia on the treatment outcomes of two symptom-focused treatments, i.e. CBT-F and CBT-I. In our study, the prevalence of co-occurrence was high, as it was in previous studies (Fossey et al., Reference Fossey, Libman, Bailes, Baltzan, Schondorf, Amsel and Fichten2004; Van Houdenhove et al., Reference Van Houdenhove, Buyse, Gabriels and Van den Bergh2011). Two-thirds of the ME/CFS patients also reported clinical insomnia and two-thirds of the ID patients also reported severe fatigue.
In both therapies, the target symptom improved after therapy, independent of the presence of the co-occurring symptom, meaning that the co-occurring symptom did not influence the effectiveness. In CBT-F, more than half of the ME/CFS patients recovered from severe fatigue, independent of the presence of co-occurring clinical insomnia at baseline. Previous studies have found that fatigue can be treated with CBT-F across different conditions with different co-morbid symptoms or symptom profiles (Castell et al., Reference Castell, Kazantzis and Moss-Morris2011; Malouff et al., Reference Malouff, Thorsteinsson, Rooke, Bhullar and Schutte2008; Menting et al., Reference Menting, Tack, van Bon, Jansen, van den Bergh, Mol, Goedendorp, Donders and Knoop2017; Okkersen et al., Reference Okkersen, Jimenez-Moreno, Wenninger, Daidj, Glennon, Cumming, Littleford, Monckton, Lochmuller, Catt, Faber, Hapca, Donnan, Gorman, Bassez, Schoser, Knoop, Treweek, van Engelen and OPTOMISTIC2018). In the case of co-occurring insomnia, this seems to apply as well. In CBT-I, about half of the patients with insomnia disorder recovered from insomnia after CBT-I, independent of the presence of co-occurring severe fatigue at baseline. Previous studies have found that insomnia can be treated with CBT-I in patients with different co-morbid disorders (Hertenstein et al., Reference Hertenstein, Trinca, Wunderlin, Schneider, Zust, Feher, Su, Straten, Berger, Baglioni, Johann, Spiegelhalder, Riemann, Feige and Nissen2022) and with web-based CBT-I in patients with co-occurring severe fatigue (Ramfjord et al., Reference Ramfjord, Faaland, Scott, Saksvik, Lydersen, Vedaa, Kahn, Langsrud, Stiles, Ritterband, Harvey, Sivertsen and Kallestad2023). Our results confirm that insomnia with co-occurring severe fatigue can be treated with CBT-I.
We also found that in both therapies a change of fatigue severity was associated with a change in insomnia severity in the same direction. One possible explanation is that both CBT-F and CBT-I also target the co-occurring symptom. During CBT-F patients learn to regulate their sleep–wake rhythm which is known to influence insomnia (Manber et al., Reference Manber, Bootzin, Acebo and Carskadon1996). Also, some elements of CBT-I, such as relaxation during the day, might have an effect on fatigue (Kesik et al., Reference Kesik, Ozdemir and Mungan Ozturk2022; Kilic and Parlar Kilic, Reference Kilic and Parlar Kilic2021; Komurkara and Cengiz, Reference Komurkara and Cengiz2022; Yoo et al., Reference Yoo, Kim, Kim and Kim2022). Another possible explanation is that improving sleep quality reduces fatigue and vice versa. However, only 10 (for CBT-F) to 25% (for CBT-I) of the variance of the change in the co-occurring symptom could be explained by the association with the change in the target symptom. This implies that the change in the co-occurring symptom during therapy is mainly due to other factors, most particularly in CBT-F.
A third of the ME/CFS patients still reported clinical insomnia post CBT-F, despite not experiencing severe fatigue any more. This may indicate that although CBT-F includes some, it does not include enough elements of CBT-I for a subgroup of patients. In particular, sleep restriction is a highly effective element in treating insomnia and its effect on insomnia is superior to regulating the sleep–wake rhythm (Maurer et al., Reference Maurer, Espie, Omlin, Reid, Sharman, Gavriloff, Emsley and Kyle2020). Also the combination of all elements of CBT-I (Harvey et al., Reference Harvey, Belanger, Talbot, Eidelman, Beaulieu-Bonneau, Fortier-Brochu, Ivers, Lamy, Hein, Soehner, Merette and Morin2014) is known to result in a higher effectiveness than offering separate elements.
Vice versa, a quarter of the ID patients still reported severe fatigue after CBT-I, although they no longer experienced clinical insomnia. These fatigue symptoms could be a temporary consequence of the sleep restriction during therapy (Kyle et al., Reference Kyle, Morgan, Spiegelhalder and Espie2011) and might disappear over time. The persistence of the co-occurring symptom at clinically relevant levels for a significant number of patients after both CBTs might indicate that fatigue and insomnia do not merely have a bi-directional relationship but are driven by their own symptom-focused factors. Specifically depression and subjective sleep characteristics (e.g. an inverse relationship with sleep duration) are known to predict fatigue severity in insomnia patients (Kim et al., Reference Kim, Kim, Jeon, Leary, Barwick and Mignot2019). Furthermore, many ID participants suffered from a medical co-morbidity. We cannot exclude the possibility that a currently active underlying medical condition may explain the fatigue, although research suggests that severe and chronic fatigue seems more determined by individual patient characteristics and behaviours than by somatic markers of the disease (Menting et al., Reference Menting, Tack, Bleijenberg, Donders, Droogleever Fortuyn, Fransen, Goedendorp, Kalkman, Strik-Albers, van Alfen, van der Werf, Voermans, van Engelen and Knoop2018). The relation between these somatic parameters and fatigue severity is generally weak and tends to diminish over time (Goertz et al., Reference Goertz, Braamse, Spruit, Janssen, Ebadi, Van Herck, Burtin, Peters, Sprangers, Lamers, Twisk, Thong, Vercoulen, Geerlings, Vaes, Beijers, van Beers, Schols, Rosmalen and Knoop2021). Persistent fatigue in chronic disease seems to be a transdiagnostic phenomenon which can be treated with CBT aimed at fatigue perpetuating factors (de Gier et al., Reference de Gier, Picariello, Slot, Janse, Keijmel, Menting, Worm-Smeitink, Beckerman, de Groot, Moss-Morris and Knoop2023).
Given our findings, in the case of co-occurring severe fatigue and insomnia one might consider starting with CBT-I, as CBT-I has a relatively short treatment duration compared with CBT-F (on average 7 vs 15 sessions). CBT-I might result in faster symptom reduction for the patient and requires less therapist time to deliver than CBT-F. If severe fatigue remains present after CBT-I, one could then consider proceeding with CBT-F. Adding CBT-I to treatment of other symptoms results in better, long-lasting effects for both insomnia and the condition (Hertenstein et al., Reference Hertenstein, Trinca, Wunderlin, Schneider, Zust, Feher, Su, Straten, Berger, Baglioni, Johann, Spiegelhalder, Riemann, Feige and Nissen2022). Thus, adding CBT-I might also positively influence outcomes on fatigue of CBT-F. Future studies should use randomisation to investigate this treatment sequence when severe fatigue and insomnia co-occur, comparing CBT-I followed by CBT-F (if needed) with CBT-F alone.
Our study has its limitations. Firstly, the study was under-powered to detect a medium sized difference in outcome between ID patients with and without co-occurring fatigue. However, given the magnitude of the effect size found, the conclusions seem quite robust. A second limitation is that this study focuses on immediate post-intervention outcomes. We do not know if the findings show further change during extended follow-up. Thirdly, CBT-I was delivered in a group format, which seems to be as effective as individual treatment (Furukawa et al., Reference Furukawa, Sakata, Yamamoto, Nakajima, Kikuchi, Inoue, Ito, Noma, Takashina, Funada, Ostinelli, Furukawa, Efthimiou and Perlis2024), although there is also research suggesting that group CBT-I is less effective (Yamadera et al., Reference Yamadera, Sato, Harada, Iwashita, Aoki, Obuchi, Ozone, Itoh and Nakayama2013). Therefore, it might be that the effects would have been better using individual CBT-I. Finally, this study is an observational study based on data used for clinical practice. Therefore a number of other factors which could have influenced the treatment outcomes (for instance depressive symptoms and subjective sleep characteristics as measured with a sleep diary), were not accounted for.
In conclusion, co-occurring severe fatigue and insomnia does not influence treatment-outcome of CBT-F and CBT-I. However, the severe co-occurring symptom can persist after CBT.
Data availability statement
The de-identified patient dataset can be made available after publication. Any request to share the data used in this study will be considered by the authors and will need to be approved by the ethics committee of the Amsterdam UMC, Location University of Amsterdam.
Acknowledgements
None.
Author contributions
Nynke Rauwerda: Conceptualization (equal), Data curation (equal), Formal analysis (lead), Investigation (equal), Methodology (supporting), Project administration (equal), Visualization (lead), Writing - original draft (lead), Writing - review & editing (equal); Tanja Kuut: Conceptualization (equal), Data curation (equal), Formal analysis (supporting), Investigation (equal), Project administration (equal), Visualization (supporting), Writing - original draft (supporting), Writing - review & editing (equal); Annemarie Braamse: Supervision (supporting), Writing - review & editing (equal); Pythia Nieuwkerk: Formal analysis (supporting), Methodology (equal), Writing - review & editing (equal); Myrthe Boss: Writing - review & editing (equal); Hans Knoop: Conceptualization (equal), Methodology (equal), Resources (lead), Supervision (equal), Writing - original draft (supporting), Writing - review & editing (equal); Annemieke van Straten: Conceptualization (equal), Supervision (equal), Writing - original draft (supporting), Writing - review & editing (equal).
Financial support
This research received no specific grant from any funding agency, commercial or not-for-profit sectors.
Competing interests
H.K. receives royalties for a published manual of CBT for ME/CFS. N.L.R., T.A.K., A.M.J.B., P.N., H.M.B. and A.S. declare no competing interests.
Ethical standards
The Dutch law on Medical Research Involving Human Subjects Act (WMO) did not apply because data were collected as part of routine clinical care without additional assessments. This was checked by the Medical Ethical Review Board of the Amsterdam University Medical Centre (W23_068 # 23.091). The study was carried out in accordance with the Declaration of Helsinki.
Appendix
Overview of intervention parts of cognitive behavioural therapy for fatigue (CBT-F) and insomnia (CBT-I)

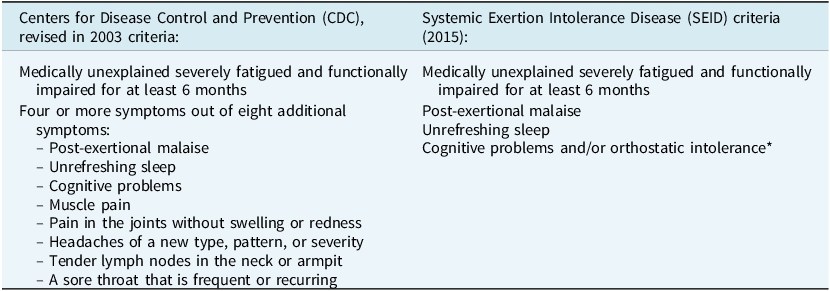
Definition of myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS) according to commonly used case definitions

*Orthostatic intolerance was not assessed.
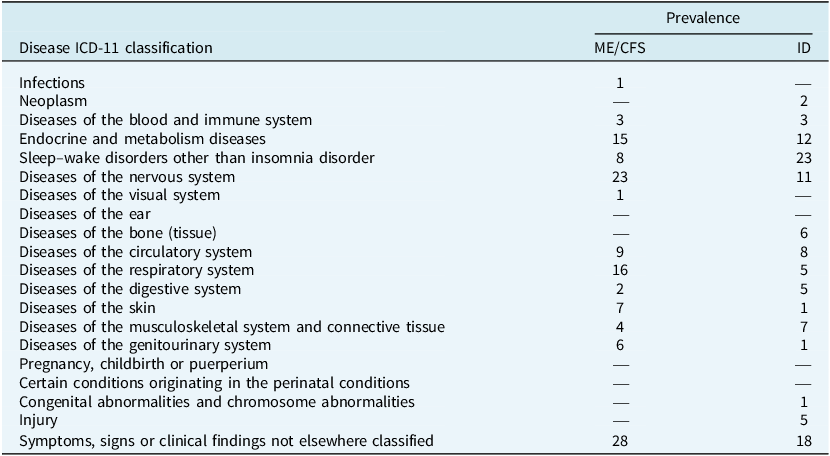
Prevalence (in numbers) of medical conditions (organized in ICD-11 classification) in the ME/CFS and ID participants





Comments
No Comments have been published for this article.