Introduction
The experience of losing a loved one through death is something almost everyone will encounter in their lifetime and is frequently one of life’s most profoundly challenging stressors (Szuhany et al., Reference Szuhany, Malgaroli, Miron and Simon2021). Bereaved individuals in the weeks and months after a loss will often experience intense yearning, longing and prominent thoughts and memories of the deceased, accompanied by intense emotional pain, feelings of disbelief and difficulty accepting the death, avoidance of situations that trigger increases in longing or sadness, and a loss of interest and meaning in the future without the deceased. This can be accompanied by physical pain, sleep disturbances and changes in eating, and difficulties in adapting to changes in role and identity. Typically, individuals alternate between confronting emotional pain and setting it aside, as they engage in loss-oriented and restoration-oriented processing (Stroebe and Schut, Reference Stroebe and Schut1999). Most individuals move over time from acute grief to integrated grief, so that the grief is more in the background, they feel adjusted to the loss, and they can meaningfully re-engage with life without the deceased, including reconnecting to pleasurable activities and reattaching to significant others (Shear et al., Reference Shear, Ghesquiere and Glickman2013).
Although acute grief can be highly distressing and disabling, this reaction should not routinely be pathologized and does not warrant clinical intervention in most cases (Shear et al., Reference Shear, Muldberg and Periyakoil2017a). Instead, a continuum of support is needed that varies depending on the severity and pervasiveness of the grief reaction. Many individuals benefit from an informal supportive response from family, friends, employers, educational establishments and the broader communities around them, providing the opportunity to talk about the loss, reducing feelings of isolation, and receiving assistance with the practical tasks around bereavement (including planning a funeral and managing finances). Some individuals may also benefit greatly from access to formal bereavement counselling approaches, providing a supportive space to talk through the loss in a structured and safe environment (Waller et al., Reference Waller, Turon, Mansfield, Clark, Hobden and Sanson-Fisher2016).
However, for some, acute grief will become stuck and develop into a prolonged, disabling grief reaction. At this point individuals may benefit from access to additional psychological therapies designed specifically for the most severe and entrenched grief reactions. Building on the earlier term of ‘complicated grief’, the ‘prolonged grief disorder’ (PGD) construct has recently been introduced to describe a persistent and stuck grief reaction. While some critics have argued that PGD unhelpfully pathologizes loss (Cacciatore and Frances, Reference Cacciatore and Frances2022), it nevertheless provides a way to identify individuals most afflicted by grief that is not naturally resolving and who may benefit from further support (Prigerson et al., Reference Prigerson, Kakarala, Gang and Maciejewski2021). According to the International Classification of Diseases (ICD-11) diagnostic framework (World Health Organization, 2020), PGD is characterised by a persistent and pervasive longing for, and pre-occupation with, the deceased, combined with at least one symptom of intense emotional pain, that lasts for at least 6 months after the bereavement. The indicators of intense emotional pain include intense sadness, guilt, anger, denial and blame; difficulty accepting the death; feeling one has lost a part of oneself; an inability to experience positive mood; emotional numbness, and difficulty in engaging with social or other activities. PGD sits in the same category as post-traumatic stress disorder (PTSD) in the ICD-11 classification system, as it is labelled as a ‘disorder specifically associated with stress’. It is conceptualised in broadly similar terms in the Diagnostic and Statistical Manual of Mental Disorders (DSM-V-TR) classification system (Prigerson et al., Reference Prigerson, Kakarala, Gang and Maciejewski2021; World Health Organization, 2020).
It is estimated that approximately 10% of all bereaved people will experience PGD (Lundorff et al., Reference Lundorff, Holmgren, Zachariae, Faver-Vestergaard and O’Connor2017), with point-prevalence estimates of around 1.5% of the general population (Rosner et al., Reference Rosner, Comtesse, Vogel and Doering2021). PGD is more likely to occur following violent, traumatic, and/or untimely death (including homicide or suicide); loss of a child or a spouse (or other exceptionally close, positive relationships); where there was not a chance to say goodbye or death rituals like funerals were disrupted; in individuals with a previous history of loss, mental health problems and with insecure attachment styles; and where there is a lack of social support before and after the death (Lobb et al., Reference Lobb, Kristjanson, Aoun, Monterosso, Halkett and Davies2010).
PGD is associated with significant negative outcomes, including chronically high levels of distress and functional impairment, poor physical health, elevated suicide rates, and higher risk of all-cause mortality (Prigerson et al., Reference Prigerson, Shear and Reynolds2022). PGD frequently is co-morbid with other mental health disorder presentations secondary to the loss, including depression, anxiety and PTSD (Shear, Reference Shear2015a; Jordan and Litz, Reference Jordan and Litz2014). PGD therefore constitutes a strong indication for treatment (Shear et al., Reference Shear, Reynolds, Simon, Zisook and Wang2016).
A range of effective, evidence-based psychological treatments for PGD are emerging. One such approach is prolonged grief disorder therapy (PGDT; Shear et al., Reference Shear, Frank, Houck and Reynolds2005; Shear et al., Reference Shear, Muldberg and Periyakoil2017b), which was developed in tandem with the validation of the PGD diagnosis (Kobak et al., Reference Kobak, Shear, Skritskaya, Bloom and Bottex2023). This is a 16-session structured and evidence-based psychotherapy most often delivered in individual, face-to-face format. PGDT is informed by the dual process model of loss (Stroebe and Schut, Reference Stroebe and Schut1999), attachment theory, and self-determination theory (Ryan and Deci, Reference Ryan and Deci2000). The treatment aims to help individuals accept the loss, foster continuing bonds with the deceased through living memories, and to reconnect with rewarding activities, intrinsic interests and core values in a world changed by the loss. This is achieved by combining elements of cognitive behavioural therapy (CBT), interpersonal therapy (IPT), motivational interviewing, positive psychology and psychodynamic psychotherapy.
A series of studies have demonstrated PGDT is effective. An early single arm pilot study (n=21) showed that PGDT led to large effect size pre- to post-treatment reductions in complicated grief, anxiety and depression symptoms (Shear et al., Reference Shear, Frank, Foa, Cherry, Reynolds, Vander Bilt and Masters2001). A subsequent randomised controlled trial (RCT) compared PGDT (n=49) to interpersonal psychotherapy (IPT; n=46) in adults meeting criteria for complicated grief (Shear et al., Reference Shear, Frank, Houck and Reynolds2005). Treatment response (defined as a 20-point or greater improvement on the self-report Inventory of Complicated Grief or a clinician rating of global improvement) was significantly greater for PGDT than IPT (51% versus 28%). A second RCT compared PGDT (n=74) with IPT (n=77) for complicated grief specifically in elderly people (Shear et al., Reference Shear, Wang, Skritskaya, Duan, Mauro and Ghesquiere2014). Response rates were again significantly greater for PGDT than IPT (71% versus 32%). There were also greater gains over time in continuous measures of grief severity, grief-related avoidance, depression, and functioning in PGDT relative to IPT. A third, 4-site trial examined the efficacy of citalopram versus placebo when administered with or without PGDT (Shear et al., Reference Shear, Reynolds, Simon, Zisook and Wang2016); 395 bereaved adults were randomised to placebo, citalopram administered by a pharmacotherapist who also provided a simple grief support intervention, PGDT with placebo, or PGDT with citalopram, with response rates on a grief-related clinical global impression improvement scale as the primary outcome. PGDT with placebo (83% response rate), but not citalopram alone (69% response rate), was superior to placebo (55% response rate). The addition of citalopram to PGDT did not significantly enhance grief outcomes (response rate of 84%) but did lead to a significantly greater reduction in depression symptoms than PGDT alone. PGDT represents one of several emerging interventions to support prolonged grief generally and treat PGD specifically (see reviews by Johannsen et al., Reference Johannsen, Damholdt, Zachariae, Lundorff, Farver-Vestergaard and O’Conner2019; Komischke-Konnerup et al., Reference Komischke-Konnerup, Zachariae, Boelen, Marello and O’Connor2024). PGDT was the first and most extensively tested of these approaches, including the only treatment shown to be superior to other active medication or psychotherapy alternatives across a series of trials.
Despite clear evidence of the need and treatment efficacy, PGDT and related therapies are not routinely available to individuals suffering with PGD. In a United Kingdom (UK) context, one potential service setting to provide treatments like PGDT is in NHS Talking Therapy services (NHS-TT), previously known as Improving Access to Psychological Therapies (IAPT) services (for an overview, see Clark, Reference Clark2018). NHS-TT services provide access to evidence-based psychological therapies for common mental health problems like anxiety, depression and PTSD in a primary care setting. A stepped-care model is followed to maximise the number of clients who can be supported. Clients are assessed by a low-intensity (Step 2) therapist, a psychological wellbeing practitioner (PWP). Less complex presentations are offered low-intensity treatment by PWPs. If individuals have more complex presentations or have not responded to low-intensity treatment, they are stepped-up to high-intensity (Step 3) interventions with a high-intensity (HI) therapist. NHS-TT services also have the potential to deliver PGDT for clients with prolonged grief alongside depression, anxiety and PTSD presentations as part of their high-intensity offering at a scalable, national level via top-up training of their existing CBT workforce.
One way to preliminarily explore the feasibility and utility of PGDT in an NHS-TT context is to implement it in real world NHS-TT services and to carefully evaluate engagement and clinical efficacy while doing so (‘practice-based evidence’; Castonguay et al., Reference Castonguay, Barkham, Youn, Page, Barkham, Lutz and Castonguay2021). The present study reports the outcomes of a pilot implementation of a high-intensity PGDT pathway in a single NHS-TT service in Devon. This pathway was developed in reaction to the service identifying that a significant subgroup of clients was presenting with prolonged grief presentations alongside symptoms of depression, anxiety and/or PTSD (and the anticipation that this kind of presentation might increase in prevalence in the aftermath of the COVID-19 pandemic). While clients with less severe and entrenched grief presentations were perceived as benefiting from signposting to local charitable sector bereavement counselling services, there was insufficient capacity in these services to meet the presenting need and this was not always appropriate for those with more severe and entrenched grief symptoms alongside co-morbid depression, anxiety and/or PTSD. These more severe cases were being treated using existing high-intensity care pathways within the service (predominantly National Institute for Health and Care Excellence (NICE) approved treatments for depression, anxiety and PTSD). However, it was felt that these interventions (with the possible exception of some limited availability of IPT) were not tailored to the specific needs of this population and were not optimally effective. In particular, when clients were presenting with traumatic loss, they were typically treated via the service PTSD pathway, which was perceived as effective at reducing avoidance, hyper-arousal and re-experiencing symptoms, but was felt not to help the underlying grief.
Therefore, in partnership with a mood disorders specialist centre at the University of Exeter, UK and a prolonged grief specialist centre at Columbia University, USA, a cadre of experienced high-intensity therapists working in the NHS-TT service were trained to deliver PGDT via the establishment of a bespoke training, supervision and service pathway. The current study assesses the feasibility and effectiveness of this pathway since its inception.
Routinely collected depression, anxiety and functioning measures in NHS Talking Therapies services were supplemented with the Brief Grief Questionnaire (BGQ; Shear et al., Reference Shear, Jackson, Essock, Donahue and Felton2006). The clinical outcomes were benchmarked with previous PGDT evaluation trials, as well as against national NHS-TT targets and local service performance of other high-intensity treatment pathways.
Method
Setting and design
A high-intensity therapy prolonged grief pathway in NHS-TT service in Devon, UK opened for referral in April 2022. Outcomes for all clients who had completed treatment in the pathway by April 2024 and who met core eligibility criteria were included in this pilot evaluation.
Pathway eligibility criteria and assessment procedure
The formal primary eligibility criteria for the prolonged grief pathway were having suffered a bereavement at least 6 months previously and to be experiencing a sustained prolonged grief response to it, either based on clinical assessment and/or scoring ≥4 on the BGQ (the cut-off for prolonged grief disorder). In addition, clients needed to identify grief as the primary problem they wished to work on, score in clinical ranges for depression and/or anxiety on the standard NHS-TT minimum data set, and meet other standard NHS-TT service eligibility criteria (aged 18 years or over; any concerns about suicide or self-harm can be safely managed in a primary care setting; any substance use issues are not the primary presenting problem and will not interfere with engagement with therapy; not presenting with a severe and enduring mental illness like bipolar disorder, psychosis, or personality disorder; not receiving other concurrent psychotherapy). There were no exclusions for use of psychotropic medication.
Assessments for eligibility for the grief pathway were completed by low-intensity therapists (PWPs), who were trained in how to assess for an unresolved grief reaction. A 1-day service-wide training for all PWPs about how to identify, assess, and support grief had been provided before the pathway was launched. PWPs were also trained in the administration and scoring of the BGQ to screen for unresolved grief. Where there was a query about possible co-morbid PTSD, this was assessed using the PTSD checklist for DSM-5 (PCL-5; Blevins et al., Reference Blevins, Weathers, Davis, Witte and Domino2015).
If there was doubt about fit with the grief pathway, the PWPs discussed the case with PGDT trained high-intensity therapy colleagues to determine appropriateness. Where clients also presented with potential PTSD alongside the loss, clinicians explored with them their goals for treatment (i.e. were they grief related or more suited to a trauma-focused intervention) and this was used to help make a collaborative informed choice about whether to enter the service grief or PTSD pathway. PWPs were allowed to use judgement to allow participants into the pathway who did not meet all criteria where this was clinically warranted. This included allowing some clients to receive input where the loss had occurred less than 6 months ago if this been particularly difficult or traumatic, and was leading to marked difficulties. Moreover, some clients were allowed into the pathway who did meet NHS-TT clinical criteria for depression and/or anxiety, but who were struggling with loss and exhibited PGD. A specific PGDT pathway was established on the service electronic record system (IAPTus), meaning that it was possible to establish a separate waiting list for PGDT. Clients were placed on this waiting list for therapy and picked up by the first available PGDT trained high-intensity therapist.
Intervention
Clients received PGDT, consisting of approximately 16 weekly (1-hour long) individual sessions delivered face-to-face or via video conferencing (for an overview, see Kobak et al., Reference Kobak, Shear, Skritskaya, Bloom and Bottex2023; Shear et al., Reference Shear, Skritskaya, Bloom, Schnyder and Cloitre2022). PGDT is an integrated and focused psychotherapy targeting adaptation to loss, based on research-informed principles and evidence-based methods. It integrates elements from CBT, IPT, motivational interviewing, positive psychology, and psychodynamic psychotherapy. Attachment theory is used to understand bereavement and grief and to help adapt to the loss. Following the dual-process model (Stroebe and Schut, Reference Stroebe and Schut1999), this adaptation is seen as involving both processing the loss and reconnecting with life after the loss to restore wellbeing. While loss and grief are seen as a universal experience, for some the process of moving from resolved to integrated grief can become ‘derailed’ if naturally occurring patterns of thinking, feeling and responding that occur early in grief become persistent and habitual for a sustained period of time. Examples of factors that interfere with adaptation include trying to control or judge the grief; survivor guilt or excessive ruminative self-blame or anger; counterfactual (‘if only’) thinking characterised by attempts to rewrite history in ways that the death did not happen; pronounced avoidance of reminders of the loss; and a disconnection from social support. Clients are supported to resolve ‘derailers’ as they learn to accept the loss and restore the capacity for wellbeing. To do so they move through seven healing milestones. Doing so results in the evolution of grief from a pervasive, intense presence to a quieter, integrated place in the person’s life. Therapists use active listening and personalised interventions, working through a planned series of sessions and clearly specified psychological exercises across the healing milestones during therapy: understanding and accepting grief; managing grief-related emotional pain; imagining a promising future; strengthening relationships with others; telling the story of the death; living with reminders of loss; and connecting with memories of the deceased. The first two themes help clients and understand and accept grief; the next two themes help restore the capacity for wellbeing; and the last three themes help clients accept the reality of the loss and establish a sense of ongoing connection with the person who died. Techniques used include grief monitoring, psychoeducation, goal setting, meeting with a visitor, imaginal revisiting, situational revisiting, and an imaginal conversation.
Therapy was delivered by 17 experienced high-intensity therapists (all of whom were accredited CBT therapists by the British Association of Behavioural and Cognitive Psychotherapies; see Table S1 in the Supplementary material for therapist characteristics). These therapists all had prior training and experience treating depression, anxiety and PTSD, and a minority had prior experience of working specifically with traumatic loss. Therapists all underwent additional training in PGDT, completing (and having sustained access to) a modular web-based training in PGDT (Kobak et al., Reference Kobak, Shear, Skritskaya, Bloom and Bottex2023).Footnote 1 This consisted of didactic information, web-based exercises, simulated patient scenarios, animated graphics, ongoing web-based self-tests, video role-play examples, and access to assessment tools and outcome measures. The training consists of 11 modules (covering the nature of grief, an overview of PGD and PGDT, pre-treatment assessment, a module of each of the seven themes of therapy, and final module exploring treatment progress and managing therapeutic endings). Each module takes around 20–40 minutes to complete. Pilot evaluation of this modular web-based training shows it is acceptable to clinicians and results in improvements in clinical practice (Kobak et al., Reference Kobak, Shear, Skritskaya, Bloom and Bottex2023). All therapists were also given access to a copy of the therapy treatment manual (Shear, Reference Shear2015b), which provided a detailed session-by-session guide to follow.
Therapists treating cases had access to ongoing monthly 60-minute group specialist peer supervision to support their grief work, facilitated by therapists with greater experience in the model. This was in addition to ongoing clinical and case supervision for their routine therapy work in the service. Consistent with standard delivery of NHS-TT treatments, therapists were encouraged to show ‘flexibility within fidelity’ (cf. Kendall, Reference Kendall2021) when delivering (PGDT). The model was followed as per the manual, but if a patient did not wish to engage with a specific intervention component (for example, session with a visitor or imaginal conversation with the deceased) delivery of the treatment was tailored to not include this element. Therapists all had prior experience of delivering CBT (all in high-intensity format and some were also trained in low-intensity approaches) and these skills were useful when delivering treatment components of PGDT (for example, exposure elements of the treatment). Due to resource constraints, it was not possible to assess therapist competence or adherence to the PGDT protocol in this evaluation.
Data collected
Reflecting standard NHS-TT practice, at each treatment session attended, anxiety symptoms were assessed with the 7-item self-report Generalized Anxiety Disorder Scale (GAD-7; Spitzer et al., Reference Spitzer, Kroenke, Williams and Lowe2006), depression symptoms were assessed with the 9-item self-report Patient Health Questionnaire (PHQ-9; Kroenke et al., Reference Kroenke, Spitzer and Williams2001), and functional impairment was assessed with the 5-item self-report Work and Social Adjustment Scale (WSAS; Mundt et al., Reference Mundt, Marks, Shear and Griest2002). External criteria for reliable change on the PHQ-9 and GAD-7 are 6- and 4-points, respectively. There is no agreed threshold for reliable change on the WSAS. Therefore, using internal reliability and intake standard deviation from a similar NHS-TT sample reported in Zahra and colleagues (Reference Zahra, Qureshi, Henley, Taylor, Quinn, Pooler and Byng2014), reliable change was estimated as a change of 11 or more points. (see Section 1 in the Supplementary material for details of these measures). Recovery criteria are scoring <10 points on the PHQ-9, <8 points on the GAD-7, and <10 points on the WSAS. NHS-TT services additionally report on rates of reliable improvement (showing reliable improvement on the PHQ-9 and/or reliable improvement on the GAD-7), recovery (at final session scoring <10 on the PHQ-9 and <8 on the GAD-7), and reliable recovery (meeting both reliable improvement and recovery criteria).
The NHS-TT minimum dataset was optionally supplemented with the BGQ (Shear et al., Reference Shear, Jackson, Essock, Donahue and Felton2006) to assess prolonged grief symptoms at assessment and final treatment session. This asked five questions about grief reactions to bereavement (e.g., ‘How much does your grief still interfere with your life?’), each rated on a scale from 0 (not at all), 1 (somewhat) to 2 (a lot). No time period over which to rate the item is specified. Scores are summed, with higher scores indicating a more marked grief reaction. The scale has adequate internal reliability in a primary care setting (α=.82; Patel et al., Reference Patel, Cole, Little, Skritskaya, Lever, Dixon and Shear2019). Patel et al. (Reference Patel, Cole, Little, Skritskaya, Lever, Dixon and Shear2019) demonstrated that scores of 4 or greater on the BGQ correspond with a score of 30 or more on the longer Inventory of Complicated Grief (Prigerson et al., Reference Prigerson, Maciejewski, Reynolds III, Bierhals, Newsom, Fasiczka, Frank, Doman and Miller1995), which in turn is highly predictive of meeting ICD-11 diagnostic criteria for PGD (Mauro, unpublished data provided to DSM-5 committee). Therefore, in the present study we use a BGQ score of ≥4 to assess pathway eligibility (and a score of <4 was used to indicate clinical remission post-treatment). There is no agreed threshold for reliable change on the BGQ, so we estimated this based on the reliability reported in Patel and colleagues (Reference Patel, Cole, Little, Skritskaya, Lever, Dixon and Shear2019) and the intake standard deviation of the present sample who had been through the NHS-TT grief pathway. This resulted in a change of >4 points being set as the threshold.
In NHS-TT services it will be important in the future to determine who should be allocated to low-intensity versus high-intensity grief care pathways, with presenting severity being one factor influencing this decision. As the criteria for PGD have evolved recently, there are currently no agreed severity thresholds on the BGQ. Here we divide PGD into lower severity (BGQ 4–7) and higher severity (BGQ ≥8) categories. The BGQ was an optional, not mandated, measure due to operational challenges adding it to the electronic outcome measure capture system used in service, meaning clinicians had to manually administer and enter scores (see Section 1 of the Supplementary material for further details on the BGQ). Data about client demographic characteristics, number of sessions attended, first and last treatment session outcome measures, and discharge type were extracted from routine electronic clinical notes for the purposes of this evaluation.
Analysis
Analyses were conducted in the IBM Statistical Package for Social Sciences (SPSS; version 29.0.1.0) on complete case data. We only included in the audit analysis participants who fully met pathway eligibility criteria (i.e. we set aside those allowed into the pathway without fully meeting prolonged grief and anxiety and/or depression caseness criteria).
For continuous variables, mean (SD) values were reported and for categorical variables number (%) values were reported. PGDT pathway feasibility was assessed in terms of rates of therapist retention (number [%] of therapists trained still delivering PGDT), client recruitment, client data completeness (number [%] of clients with a paired pre–post data on each outcome measure), safety (number [%] of clients showing reliable deterioration on each outcome measure; number [%] of treatment related adverse events reported by therapists), and client engagement (mean [SD] number of sessions attended, client discharge code, and number [%] completing a minimum adequate dose of therapy). There is no consensus in the literature as to what constitutes an adequate minimum dose of PGDT, so we report both a liberal estimate of completing four or more sessions sometimes used in NHS-TT services (cf. Robinson et al., Reference Robinson, Delgadillo and Kellett2020) and a conservative estimate of 50% of acute treatment dose often sometimes used in trials in NHS-TT services (e.g. Dunn et al., Reference Dunn, Widnall, Warbrick, Warner, Reed, Price and Kuyken2023), in this case attending at least eight out of a maximum of 16 PGDT sessions.
Clinical outcomes were assessed in terms of change from intake to final treatment session on the PHQ-9, GAD-7, WSAS, and BGQ. Key binary outcomes on each individual outcome measures were reliable improvement, reliable deterioration, recovery (scoring below clinical cut-offs at last session), and response (≥50% reduction in symptoms from first to last session). In addition, three standard NHS-TT pooled outcomes across anxiety and depression were computed: rates of reliable improvement (on either PHQ-9 or GAD-7), recovery (on both PHQ-9 and GAD-7), and reliable recovery (meeting both reliable improvement and recovery criteria). For statistical analyses, alpha was set at .05 and the result of two-tailed tests are reported. The primary statistical analyses used were paired sample-tests, reporting Cohen’s d as the measure of pre–post treatment effect size (<0.2 negligible; 0.2–0.5 small; 0.5–0.8 medium; >0.8 large; Cohen Reference Cohen1988). The primary analyses were run on a complete case basis (all eligible clients referred into the pathway with sufficient data). A secondary sensitivity analysis was run on the subset of individuals with valid data who met criteria for higher severity PGD on the BGQ (scoring ≥8). To benchmark outcomes against previous trial findings a validated imputation method widely used in the meta-analytic literature (e.g. Cuijpers et al., Reference Cuijpers, Karyotaki, Ciharova, Miguel, Noma and Furukawa2021; Furukawa et al., Reference Furukawa, Cipriani, Barbui, Brambilla and Watanabe2005) was used to estimated response and remission rates for each outcome in each arm of previous PGDT trials (Shear et al., Reference Shear, Frank, Foa, Cherry, Reynolds, Vander Bilt and Masters2001; Shear et al., Reference Shear, Frank, Houck and Reynolds2005; Shear et al., Reference Shear, Wang, Skritskaya, Duan, Mauro and Ghesquiere2014). This imputation method assumes a normal distribution of the rating scale across the sample, proposes a common raw response threshold as a 50% reduction from baseline mean score of the sample, and then computes the percentage of participants in the sample who would fall to the left of the normal curve of this value (see p. 210, Samara et al., Reference Samara, Spineli, Furukuwa, Engel, Davis, Salanti and Leucht2013).
Ethics and consent
All clients referred into the NHS-TT service are routinely asked if they provide consent for the storage and use of data in line with the Trust’s information governance structures (including use of data for audit purposes). Only clients who gave this consent were included in this evaluation. As this is evaluation of a routine quality improvement initiative using data captured as part of regular service function, clients did not have to give written, informed consent to take part in this specific evaluation project and NHS ethics approval was not required or sought to take part. However, ethics approval was sought and granted from the University of Exeter School of Psychology ethics committee (reference: 525159) to ensure best practice was followed.
Results
Sample characteristics
Ninety-one clients completed treatment in the pathway between April 2022 and April 2024, 80 of whom met all formal pathway criteria and were included in the audit analysis (see Table 1 for a summary of demographic and clinical characteristics). Of the 11 clients set aside, these all showed a significant prolonged grief reaction but did not meet NHS-TT caseness criteria for depression and/or anxiety.
Clinical and demographic characteristics of clients at first session in entire sample and higher severity subsample

Continuous variables are mean (1 SD) values; categorical variables are number (%) values; PHQ-9, Patient Health Questionnaire; GAD-7, Generalised Anxiety Disorder; WSAS, Work and Social Adjustment Scale; NHS-TT, National Health Service Talking Therapies; BGQ, Brief Grief Questionnaire; PTSD, post-traumatic stress disorder; higher severity subsample, those scoring at least 8 on BGQ; a time since death not recorded for one client; bBGQ only completed by 58/80 clients.
The audit sample (n=80) was predominantly female, were aged on average in their fifties, with variable time since being bereaved. The sample identified almost entirely as of White British or White other ethnicity, with only two clients identified as other ethnic backgrounds (and ethnicity data not being available for some clients). The relationship to the deceased was most commonly parent (30/80; 38%), partner (20/80; 25%), child (11/80; 14%), other (10/80; 13%), or a combination of these in those experiencing multiple losses (9/80; 11%). The cause of death was predominantly through illness or medical conditions (61/80; 76%), with a small number of losses through accident (4/80; 5%), suicide (4/80; 5%), homicide (1/80; 1%), or overdose (1/80; 1%), or a combination of these causes in those experiencing multiple losses (9/80; 11%).
At intake assessment, 58/80 of clients (73%) completed a BGQ, 57/58 of whom (98%) met criteria for PGD (BGQ≥4). The one client scoring beneath the BGQ caseness cut-off (with a score of 3) reported ongoing difficulties around loss in the assessment. Co-morbid PTSD had been queried and assessed at the grief intake assessment for 17 clients, 15 of whom scored above caseness criteria on the PCL-5 scale and then opted for the grief pathway rather than the PTSD pathway in the service when offered the choice.
Of the 57 clients who had completed the BGQ, 40 met the more stringent criteria for the secondary sensitivity analyses (higher severity PGD based on a BGQ score ≥8 at assessment). This subsample (relative to the remaining 40 clients) had significantly greater anxiety and grief symptom severity and were more likely to be in the clinical range for anxiety, but did not significantly differ on any other demographic or clinical characteristics (see Table S2 in the Supplementary material).
Pathway feasibility
Of the 17 therapists trained in PGDT, 14 (82%) were still actively delivering the treatment at the point this paper was submitted (October 2024). Of the three therapists who stopped delivering PGDT, two had gone on maternity leave and one had stepped back due to too many other work commitments. Over a 2-year period, 92 patients were recruited into the PGDT pathway, an average rate of 3.84 clients per month. Of these 92 clients, 80 met full pathway eligibility criteria (87%). Seventy-nine out of these 80 clients completed two or more treatment sessions and so potentially had intake and last-sessions outcome measures. All 79 had first and last session PHQ-9, GAD-7, and WSAS data (100%). On the BGQ, 58/79 clients (73%) had intake data, 48/79 clients (61%) had last-session data, and 48/79 clients (61%) had data at both time points. In terms of intervention safety, there were no reported treatment related adverse or serious adverse events and rates of reliable deterioration were low (one participant deteriorating on PHQ, GAD-7 and WSAS and with no BQG data; one participant deteriorating on GAD-7, not improving on PHQ-9 or GAD-7, and not having BGQ data). Treatment engagement was satisfactory.
In the complete sample, the mean number of sessions completed was 10.29 (SD=5.81), with 68/80 clients (85%) completing four or more sessions and 51/80 clients (64%) completing eight or more sessions (liberal and conservative estimates of minimum adequate dose, respectively); 56/80 clients (70%) completed therapy with a planned discharge, 11/80 clients (14%) finished therapy with an agreed early ending, and 13/80 clients (16%) dropped out of treatment. Reasons given for early ending included having improved and requested to end (n=7), experiencing external stressors (n=2), being referred onto other services for a separate problem (n=1), and finding the homework tasks too difficult (n=1). Reasons given for dropping out included experiencing external stressors (n=5), feeling it was not the right therapy (n=2), not feeling ready to process the loss (n=1), deciding to try medication instead of therapy (n=1), or no reasons given (n=4).
In the subgroup analysis of clients with higher severity PGD (n=40), the mean number of sessions attended was 11.38 (SD=5.55), with 36/40 of clients (90%) completing five or more sessions; 32/40 of clients (80%) completed therapy with a planned discharge, 2/40 clients (5%) finished therapy with an agreed early ending, and 6/40 clients (15%) dropped out of treatment.
Treatment outcomes
Table 2 summarises continuous and binary treatment outcomes and results for the overall sample and the secondary sensitivity analysis subsample. Paired sample t-tests showed statistically significant, large magnitude pre–post treatment effect size reductions in depression, anxiety, grief, and functional impairment in both the overall sample and the sensitivity analysis subsample (with effects being numerically larger in the latter relative to the former).
Clinical outcome data for each sample
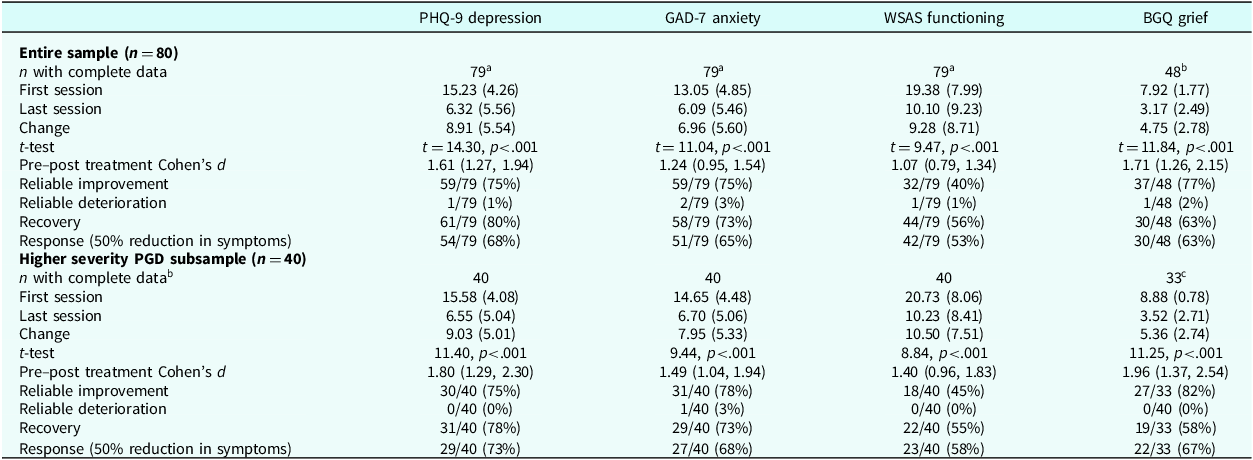
Continuous variables are mean (1 SD) values; categorical variables are number (%) values; Cohen’s d effect sizes have 95% confidence interval in parentheses; PHQ-9, Patient Health Questionnaire; GAD-7, Generalised Anxiety Disorder; WSAS, Work and Social Adjustment Scale; BGQ, Brief Grief Questionnaire (≥8 indicating higher severity); PGD, prolonged grief disorder; aone individual only attended a single session, so had no post data for PHQ-9, GAD-7 and WSAS; bin the entire sample, 48 participants had first and last session BGQ scores; cin the higher severity PGD subsample, 33 had first and last session BGQ scores.
In the entire sample, for the PHQ-9, GAD-7, WSAS and BGQ rates of reliable improvement were 75, 75, 40, and 77% respectively; rates of reliable deterioration were ≤3% across measures; rates of recovery were 80, 73, 56 and 63%, respectively; and rates of response were 68, 65, 53, and 63%, respectively. Using NHS-TT metrics (restricting this to 79 clients with data from at least two sessions), rates of reliable improvement were 65/79 (82%), rates of recovery were 57/79 (72%), and rates of reliable recovery were 54/79 (68%).
In the higher severity PGD subsample, for the PHQ-9, GAD-7, WSAS and BGQ rates of reliable improvement were 75, 78, 45, and 82%, respectively; rates of reliable deterioration were ≤3% across measures; rates of recovery were 78, 73, 55 and 58%, respectively; and rates of response were 73, 68, 58, and 67%, respectively. Using NHS-TT metrics, rates of reliable improvement were 34/40 (85%), rates of recovery were 29/40 (73%), and rates of reliable recovery were 28/40 (70%).
Rates of remission and response were equivalent or superior to PGDT arms of previous trials (and superior to control arms of these trials; see Table 3 for a summary of benchmarking analyses). An exploratory subgroup analysis found similar clinical outcomes in clients presenting with (n=14) versus without (n=65) co-morbid PTSD (see Table S3 in the Supplementary material).
Benchmarking rates of remission and response relative to imputed estimates from PGDT randomised controlled trials
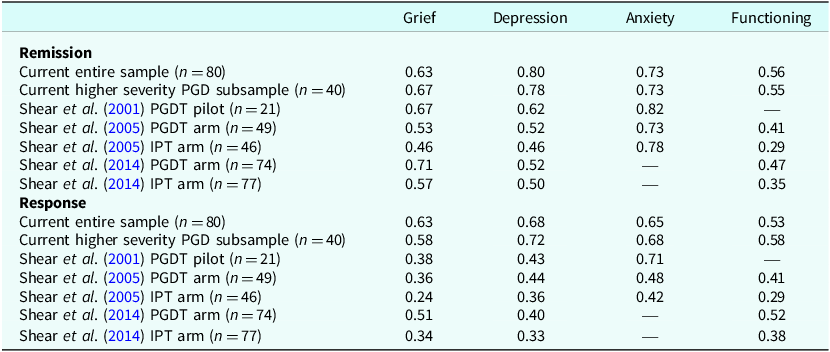
Data are proportion values; PGD, prolonged grief disorder; PGDT, prolonged grief disorder therapy; IPT, interpersonal therapy; anxiety data not available for Shear et al. (Reference Shear, Wang, Skritskaya, Duan, Mauro and Ghesquiere2014), functioning data not available for Shear et al. (Reference Shear, Frank, Foa, Cherry, Reynolds, Vander Bilt and Masters2001).
Discussion
The current evaluation aimed to investigate the feasibility and effectiveness of implementing a grief treatment pathway in an NHS-TT context to support clients with a prolonged grief reaction alongside symptoms of anxiety, depression and/or PTSD. Experienced high-intensity therapists in a single NHS-TT setting in Devon were trained to deliver PGDT, which has been shown in a series of RCTs to be effective at working with prolonged or complicated grief reactions (Shear et al., Reference Shear, Frank, Foa, Cherry, Reynolds, Vander Bilt and Masters2001; Shear et al., Reference Shear, Frank, Houck and Reynolds2005; Shear et al., Reference Shear, Wang, Skritskaya, Duan, Mauro and Ghesquiere2014; Shear et al., Reference Shear, Reynolds, Simon, Zisook and Wang2016).
Findings suggest that it is feasible to implement a PGDT pathway in an NHS-TT context, with 17 therapists being trained and then treating 91 PGD clients over 2 years alongside their routine depression and anxiety caseloads. Seventeen therapists expressed interest in learning PGDT, 14 (82%) were still actively delivering it after 2 years (two having gone on maternity leave and only one having withdrawn from delivering it due to other work commitments), suggesting it is acceptable to therapists. The pathway eligibility criteria functioned satisfactorily, with all clients exhibiting prolonged grief symptoms and 80/91 (87%) clients also meeting NHS-TT caseness criteria for depression and/or anxiety. Levels of data completeness were excellent for depression, anxiety and functioning measures (100% of clients), although there were relatively high levels of missing data on the grief measures (the BGQ), reflecting that this is not part of the standard NHS-TT minimum data set and is not made available on electronic data capture systems in an easily deployable fashion. It would be useful to embed the BGQ in a form that can be more easily administered in service to increase data completion rates. There was no evidence of intervention harms, with no treatment related adverse or serious adverse events being reported and only two clients (3%) exhibiting reliable deterioration on any outcome measures. This is lower than rates of reliable deterioration seen nationally in NHS-TT services (e.g. estimated at 6%; Clark, Reference Clark2018).
There were high rates of engagement with PGDT. Using NHS-TT routine care estimate of four or more sessions (cf. Robinson et al., Reference Robinson, Delgadillo and Kellett2020), 85% of clients received a minimum adequate dose of therapy. Using a stricter definition of 50% of protocol specified dose sometimes used in trials (in this case at least eight out of 16 sessions), 64% of clients received a minimum adequate dose of therapy. As this was a routine audit and not a clinical trial, the routine care estimate is the more appropriate metric to use. Furthermore, rates of drop-out were 16%, which compares favourably with drop-out rates observed in psychotherapy trials generally (estimates ranging from 19 to 46% across psychotherapies; Salmoiraghi and Sambhi, Reference Salmoiraghi and Sambhi2010; Swift and Greenberg, Reference Swift and Greenberg2012; Wierzbicki and Pekarik, Reference Wierzbicki and Pekarik1993) and drop-out rates specifically in NHS-TT services (e.g. Moller et al., Reference Moller, Ryan, Rollings and Barkham2019). High engagement and low levels of drop-out can be viewed as a proxy for clients finding treatment acceptable. A companion qualitative study which interviewed a subset of therapists delivering PGDT and clients receiving PGDT in the pilot also revealed that most therapists and clients thought the treatment was highly acceptable (King et al., Reference King, Dunn and Artinian2024).
There was also encouraging evidence that PGDT was clinically effective at reducing symptoms of grief, depression and anxiety and improving functioning in an NHS-TT setting. There were large effect size and statistically significant improvements in all outcomes. The observed continuous standardized pre–post treatment effect size estimates (depression: d=1.80; anxiety: d=1.49; functioning: d=1.40) exceed those found in a systematic review and meta-analysis of studies examining NHS-TT routine practice outcomes (depression: d = 0.87; anxiety: d=0.88; functioning: d=0.55; Wakefield et al., Reference Wakefield, Kellett, Simmonds-Buckley, Stockton, Bradbury and Delgadillo2021) and national NHS-TT data for the 2022–2023 year (depression: d=0.8, anxiety: d=0.9, WSAS: d=0.6; National Health Service Digital, 2024). In terms of NHS-TT standard metrics, rates of reliable improvement (82%), recovery (72%) and reliable recovery (68%) benchmarked favourably against performance in other high-intensity pathways in the Devon service over the same period (66, 53 and 49%, respectively) and previously reported national outcomes for the 2022–2023 years across all high-intensity CBT offerings (61% reliable improvement, 45% recovery, and 42% reliable recovery across all high-intensity CBT offerings for all disorders; National Health Service Digital, 2024). A similar set of findings emerged in subgroup analyses on those with high severity PGD (BGQ≥8; n=40).
It is informative to compare the rates of response observed in the current sample to general findings in the psychological therapies literature. A recent meta-analysis reports rates of response (50% reduction in symptoms) observed to psychotherapy arms in RCTs across eight mental health problems (Cuijpers et al., Reference Cuijpers, Miguel, Ciharova, Harrer, Basic, Cristea, de Ponti, Driessen, Hamblen, Larsen, Matbouriahi, Papola, Pauley, Plessen, Pfund, Setkowski, Schnurr, van Ballegooijen, Wang and Karyotaki2024). These were found to be 42% for depression trials, 38% for PTSD, obsessive compulsive disorder (OCD) and panic disorder trials, 36% for GAD trials, 32% for social anxiety disorder trials, and 24% for borderline personality disorder (BPD) trials. The observed rates of response on the grief (BGQ) primary outcome in the current sample (63% for the overall sample) and on depression and anxiety secondary outcomes (68 and 65%, respectively, for the overall sample) are therefore encouraging.
The observed improvements in all outcomes in the current analyses also benchmark favourably to results from previous pilot studies and RCTs evaluating PGDT (Shear et al., Reference Shear, Frank, Foa, Cherry, Reynolds, Vander Bilt and Masters2001; Shear et al., Reference Shear, Frank, Houck and Reynolds2005; Shear et al., Reference Shear, Wang, Skritskaya, Duan, Mauro and Ghesquiere2014; Shear et al., Reference Shear, Reynolds, Simon, Zisook and Wang2016). In particular, within-arm pre–post treatment effect sizes were numerically larger and rates of remission (defined as scoring beneath clinical cut-offs on each measure) and response (defined as 50% reduction in symptoms on each measure) were greater in the current study than in PGDT arms (and the respective active and passive control arms) of a majority of these earlier trials. Similarly, the current within-arm effects are relatively larger than those observed in broader trials of grief interventions. A recent systematic review of within-arm outcomes across the active arms of trials for prolonged grief presentations revealed standardised pre–post treatment effect sizes (Hedges’ g) across treatment of 1.32 for grief, 0.87 for depression, 0.59 for anxiety, and 1.13 for PTSD (King et al., Reference King, Dunn and Artinian2024), which are smaller than those observed in the current study.
Superior outcomes in routine practice relative to RCTs is a relatively unusual pattern of findings, as what is typically seen is a reduction in effects as treatments on carefully selected clients in ideal treatment settings diminish when treatments are given to more heterogeneous and complex clients in routine care settings (cf. Ormel et al., Reference Ormel, Hollon, Kessler, Cuijpers and Monroe2022). While indirect comparisons of pre–post treatment effect sizes taken from different samples in different settings are unreliable, it is nevertheless important to consider what could drive these differential outcomes.
Across the previous PGDT trials, a majority of participants had complicated grief presentations with co-morbid levels of depression and anxiety of a similar level to those observed in the current sample, suggesting this is not a likely explanation. It is possible that the treatment protocol and supervision pipeline for PGDT has improved through multiple iterations since the trials were completed, in particular the development of an online training platform (Kobak et al., Reference Kobak, Shear, Skritskaya, Bloom and Bottex2023). However, offsetting this, the therapists in the current audit had less intensive and less expert grief supervision once introduced to the PGDT model, relative to those therapists in the earlier trials. It is also conceivable that the high-intensity therapists in the current study had broader experience of working with depression and anxiety co-morbidities associated with grief than those in the earlier trials, potentially increasing the efficacy of elements of the protocol (e.g., extensive experience of exposure in other PTSD approaches supporting exposure work in PGDT). It is also possible that the therapists in the current study had scope to show greater ‘flexibility within fidelity’ (i.e. choosing which elements of the PGDT protocol to use and weaving in elements from other treatments to tailor care to each client) than therapists in the RCTs (where adherence to the protocol is more strictly encouraged and monitored to ensure scientific rigour). As therapist competence and fidelity to the protocol were not assessed in the current audit, it is not possible to fully evaluate the plausibility of these alternative explanations.
It is noteworthy that a minority of clients in this audit had co-morbid PTSD and actively chose to engage with this grief pathway rather than standard trauma pathways available in the NHS-TT service. The outcomes of this subgroup were similar to those without PTSD, suggesting PGDT is an appropriate treatment offering for prolonged grief presenting with significant PTSD features.
The BGQ was originally designed solely as a screening instrument to detect prolonged grief. This study suggests its possible usefulness as a simple, easily administered outcome measure. However, it would be useful to better understand the relationship of the BGQ to established PGD measures used for outcome assessment in other interventions studies (e.g. the Inventory of Complicated Grief; Prigerson et al., Reference Prigerson, Maciejewski, Reynolds III, Bierhals, Newsom, Fasiczka, Frank, Doman and Miller1995).
The current audit focuses solely on a high-intensity treatment pathway for prolonged grief. It may also be useful to develop and evaluate low-intensity treatment pathways for individuals with less complex presentations to increase the scalability of the offering. For example, those with lower severity prolonged grief (BGQ scores 4–7) could be considered for a low-intensity offering, whereas those with higher severity prolonged grief (BGQ>8) could be considered directly for high intensity step-up.
There are several limitations of the present evaluation. First, this is a pre–post evaluation with no control group and so we cannot definitively state that improvements are a result of treatment rather than spontaneous improvement over time. However, given the mean length of time since loss across the sample was 82 months and the grief reaction had persisted for that duration, spontaneous recovery seems relatively unlikely. We also cannot comment on the extent to which the improvements observed here bench against other care options for this grief sample, for example referral into standard CBT protocols for depression, anxiety or PTSD or signposting to bereavement counselling. Second, we do not have data on the number of people assessed for eligibility for the pathway, only engagement and outcome data on those who chose to enter the pathway. To fully test acceptability of the pathway to service-users, future studies should track the proportion of clients potentially eligible for the pathway. Third, no data has been captured on cost or cost-effectiveness of the pathway. However, given that PGDT is of a similar duration to existing high-intensity therapies and can be delivered by the existing workforce with relatively modest amounts of additional training, the costs of delivery are likely to be comparable to existing high-intensity care. Given rates of clinical improvement exceeded national NHS-TT targets, the approach has potential to be cost-effective relative to existing high-intensity depression and anxiety pathways. Fourth, PGDT is underpinned by a dual emphasis on processing the loss and restoring wellbeing, but no wellbeing outcome measure was collected. Future studies should also track wellbeing gains, for example using measures like the Warwick Edinburgh Mental Wellbeing Scale (WEMWBS; Tennant et al., Reference Tennant, Hiller, Fishwick, Platt, Joseph, Weich, Parkinson, Secker and Stewart-Brown2007). Fifth, no longer-term follow-up measures were taken and it is important for future research to evaluate if treatment benefits persist over time. Sixth, the BGQ cut-off we used to differentiate milder from more severe PGD is somewhat arbitrary and has not previously been validated, so sensitivity analyses should be interpreted cautiously as a result. Seventh, we did not set any feasibility continuation criteria a priori to the evaluation and future work should evaluate pre-specified feasibility rules to avoid interpretative bias. Finally, it remains to be seen if these findings will generalise to other settings, given that the pathway has been evaluated in a single site in Devon and with an experienced therapist workforce who opted into learning the therapy. The population served by the Devon NHS-TT service is predominantly White British and it remains to be seen if similar benefits will accrue for more ethnically diverse populations.
Overall, the present evaluation found that it was feasible and probably effective to offer treatment for prolonged grief disorder in a Devon NHS-TT setting, requiring only modest additional training for the existing high-intensity therapy workforce to do so. A useful next step would be to conduct a pragmatic definitive RCT comparing the clinical- and cost-effectiveness of PGDT to treatment as usual in NHS-TT services to examine if these promising findings generalise and warrant broader implementation of this grief pathway.
Key practice points
-
(1) High-intensity CBT therapists can be trained to deliver PGDT effectively with a relative brief training and supervision model within NHS-TT.
-
(2) PGDT appears acceptable to clients, with high rates of engagement and low rates of drop-out.
-
(3) Clinical outcomes of PGDT in an NHS-TT setting are promising, exceeding performance for other routine high-intensity treatments offered in NHS-TT and those found in the initial PGDT trials.
Supplementary material
The supplementary material for this article can be found at https://doi.org/10.1017/S1754470X25000030
Data availability statement
The data that support the findings of this study will be made available by S.G. upon reasonable request and approval from TALKWORKS NHS Devon Talking Therapies service. The data are not publicly available as data relate to NHS staff and patients and HRA/NHS REC approval will be required prior to any data sharing for the purposes of research.
Acknowledgements
Thanks to TALKWORKS NHS Devon Talking Therapies service and the AccEPT Clinic for support of this project, and to Arabella Ayen for helping prepare the manuscript for publication. Thanks also to all the therapists delivering, and the clients receiving, PGDT whose data are included in this evaluation.
Author contributions
Sarah Goff: Conceptualization (equal), Data curation (lead), Formal analysis (equal), Project administration (lead), Supervision (equal), Validation (equal), Writing - original draft (equal), Writing - review & editing (equal); James Carson: Data curation (supporting), Formal analysis (equal), Writing - review & editing (supporting); Asha Ladwa: Data curation (supporting), Writing - review & editing (supporting); Megan Colletta: Supervision (equal), Writing - review & editing (supporting); Raluca Topciu: Conceptualization (equal), Supervision (equal), Writing - review & editing (equal); Katherine Shear: Conceptualization (equal), Supervision (equal), Writing - review & editing (supporting); Barnaby Dunn: Conceptualization (equal), Formal analysis (equal), Supervision (equal), Writing - original draft (equal), Writing - review & editing (equal).
Financial support
The time of B.D., A.L. and M.C. was partly supported via funding to the AccEPT clinic from the Mental Health Mission (joint funded by the National Institute of Health Research and Office for Life Sciences). The views expressed in this article are those of the authors and not necessarily those of the NHS, the NIHR, or the Department of Health or Social Care.
Competing interests
S.G. (TALKWORKS Operational & Professional Lead) led the implementation of the PGDT pathway, as a Quality Improvement project for TALKWORKS (the service that has been evaluated in this study). K.S. is the developer of PGDT and directs the Centre for Prolonged Grief at the University of Columbia.
Ethical standards
Authors have abided by the Ethical Principles of Psychologists and Code of Conduct as set out by the BABCP and BPS. The work described in this manuscript was carried out in compliance with local policy; and the audit was approved by both the clinical service (TALKWORKS) hosting the pathway and the University research clinic (AccEPT) supporting the pathway. The findings from this evaluation are not intended to be generalised and therefore is not considered research and did not require additional ethical approval from a NRES committee. As such, ethical approval for research was not applied for. As anonymised group level data from routine outcome data collection were used to assess client clinical outcomes, individual clients were not asked for consent for publication.





Comments
No Comments have been published for this article.