Introduction
Patients who are diagnosed with advanced cancer are confronted with an uncertain future (Shilling et al. Reference Shilling, Starkings and Jenkins2017). Information about prognosis helps patients to adjust to the last phase of life emotionally (Butow et al. Reference Butow, Clayton and Epstein2020; van der Velden et al. Reference van der Velden, Meijers and Han2020). The majority of patients with advanced cancer want prognostic information (Innes and Payne Reference Innes and Payne2009; van der Velden et al. Reference van der Velden, van Laarhoven and Burgers2022b). Those who prefer not knowing often want to stay optimistic and foster hope (van der Velden et al. Reference van der Velden, van Laarhoven and Burgers2022b).
Prognostication is difficult, as it is hard to predict when individual patients will die from their cancer and group-level survival data may be limited. While oncologists recognize the importance of prognostic information (Liu et al. Reference Liu, Landrum and Weeks2014), they regularly report discomfort with disclosing prognosis (Butow et al. Reference Butow, Clayton and Epstein2020). They worry about undermining patients’ hope and fighting spirit or may not know how to respond to the expected raise in negative emotions, such as anxiety (Hancock et al. Reference Hancock, Clayton and Parker2007). Oncologists furthermore fear that prognostic disclosure harms patients’ trust in them, patients’ appreciation of the consultation, or the therapeutic relationship (Daugherty and Hlubocky Reference Daugherty and Hlubocky2008; Gordon and Daugherty Reference Gordon and Daugherty2003; Sisk and Mack Reference Sisk and Mack2018).According to observational studies, oncologists often explicate the unpredictability of prognosis or forgo prognostic discussions altogether (Chou et al. Reference Chou, Hamel and Thai2017; Derry et al. Reference Derry, Epstein and Lichtenthal2019a; Gordon and Daugherty Reference Gordon and Daugherty2003; Sisk and Mack Reference Sisk and Mack2018; van der Velden et al. Reference van der Velden, van der Kleij and Lehmann2021). In case of disclosure, oncologists’ estimates are usually imprecise (e.g., “months to years”) and framed optimistically (e.g., best-case scenarios), possibly to protect the patient (Chou et al. Reference Chou, Hamel and Thai2017; Derry et al. Reference Derry, Epstein and Lichtenthal2019a; Gordon and Daugherty Reference Gordon and Daugherty2003; Sisk and Mack Reference Sisk and Mack2018; van der Velden et al. Reference van der Velden, van der Kleij and Lehmann2021). The influence of oncologists’ current communicative behavior on affective outcomes is relatively unknown (van der Velden et al. Reference van der Velden, Meijers and Han2020).
Although emotional reactions to bad news are natural (Derry et al. Reference Derry, Epstein and Lichtenthal2019a), more insight into how oncologists’ communicative behaviors affect patients is necessary to facilitate prognostic disclosure without doing unnecessary harm. This is important, as prognostic disclosure concerns sensitive and potentially confrontational information for patients in a vulnerable position, and negative emotions may inhibit patients’ processing of information (Derry et al. Reference Derry, Reid and Prigerson2019b). Indeed, researchers often appeal for honest, empathetic prognostic communication that balances realism with hope (Campbell et al. Reference Campbell, Carey and Jackson2010; Parker et al. Reference Parker, Clayton and Hancock2007; van Vliet et al. Reference van Vliet, Francke and Tomson2013a). In an era of patient-centeredness, not only the instrumental but also the affective purposes of medical communication are considered essential, satisfying patients’ cognitive needs for information and emotional needs for support (van Vliet et al. Reference van Vliet, van der Wall and Plum2013c). Yet, evidence-based guidelines for such prognostic communication are lacking, as recommendations are frequently expert opinion-based (Gilligan et al. Reference Gilligan, Coyle and Frankel2017).
Existing studies cannot indisputably confirm or deny that prognostic disclosure versus non-disclosure evokes emotional suffering; evidence for influences on patients’ appreciation of the consultation is limited (van der Velden et al. Reference van der Velden, Meijers and Han2020). Little attention has been paid to how prognostic disclosure might affect patients’ way of coping with cancer, while such coping influences patients’ emotional adjustment to the disease and their psychological well-being (Johansson et al. Reference Johansson, Rydén and Finizia2011; Nipp et al. Reference Nipp, El‐Jawahri and Fishbein2016). Notably, current knowledge mostly relies on non-causal associations with prognostic disclosure, and the impact of communicating unpredictability of prognosis seems unstudied altogether (van der Velden et al. Reference van der Velden, Meijers and Han2020). Apart from the types of disclosure, little is known about effects of the content of oncologists’ messages, when they do disclose prognosis. Qualitative research suggests that both vague word-based information and precise numbers could harm patients (Westendorp et al. Reference Westendorp, Evers and Stouthard2022). Two experiments, however, found that numerical prognostic estimates decrease patients’ uncertainty and increase satisfaction, without inducing anxiety (Mori et al. Reference Mori, Fujimori and van Vliet2019; van Vliet et al. Reference van Vliet, van der Wall and Plum2013c). Also, explaining multiples of the estimated group-level median overall survival as best-case, most likely and worst-case survival scenarios are presumed to be less upsetting and more hopeful than disclosing a median overall survival estimate only (Kiely et al. Reference Kiely, McCaughan and Christodoulou2013).
The shift toward patient-centered care advocates tailoring prognostic information to individuals, given that patients may differ in their information preferences, ability to understand prognostic estimates, and personalities (Hoesseini et al. Reference Hoesseini, Dronkers and Sewnaik2020). Indeed, effects of different prognostic messages could vary by moderating individual background characteristics. Scant evidence suggests that higher-educated patients particularly appreciate receiving standard, best- and worst-case survival scenarios (Kiely et al. Reference Kiely, McCaughan and Christodoulou2013). Personal characteristics like dispositional optimism or uncertainty tolerance may shape patients’ affective responses to prognostic communication too, as may patients’ preferences for striving for life-extension and for knowing prognosis (van der Velden et al. Reference van der Velden, van Laarhoven and Nieuwkerk2022a; van Vliet et al. Reference van Vliet, van der Wall and Plum2013c). To illustrate, researchers found that patients’ approaches to deal with threatening situations influence the effects of numerical estimates on patients’ feelings of anxiety, uncertainty, and satisfaction (van Vliet et al. Reference van Vliet, van der Wall and Plum2013c). While moving away from a one-size-fits-all approach seems relevant, scientific knowledge on how to best communicate prognosis to whom remains scarce (Gilligan et al. Reference Gilligan, Coyle and Frankel2017; van der Velden et al. Reference van der Velden, Meijers and Han2020).
When manipulating communication in reality is considered unethical, video-vignette studies offer a validated design that has been shown appropriate to demonstrate the effects of communication strategies on affective outcomes, including emotions (Mori et al. Reference Mori, Fujimori and van Vliet2019; Nishioka et al. Reference Nishioka, Okuyama and Uchida2019; van Osch et al. Reference van Osch, Sep and van Vliet2014, Reference van Osch, van Dulmen and van Vliet2017; van Vliet et al. Reference van Vliet, van der Wall and Plum2013c; Visser et al. Reference Visser, Tollenaar and van Doornen2019). Video-vignettes are short visual depictions of scripted events (e.g., physician–patient conversations), rated by analogue patients (APs). APs are defined as patients, former patients, or healthy people who are instructed to imagine themselves in the shoes of the patient in the video (Hillen et al. Reference Hillen, van Vliet and de Haes2013b, Reference van Vliet, van der Wall and Albada2012; van Vliet et al. Reference van Vliet, Hillen and van der Wall2013b). Cancer-naive APs can serve as valid proxies for patients from the general population (van Vliet et al. Reference van Vliet, van der Wall and Albada2012), which prevents confounding influences of actual patients’ prior personal experiences and burdening them with reliving a bad news conversation. Hence, we examined the independent, causal effects of various prognostic communication strategies in the advanced cancer setting on emotions (positive affect, negative affect, and state anxiety), coping (helplessness/hopelessness and fighting spirit), and appreciation of the consultation (trust in the oncologist; uncertainty, satisfaction, and desirability regarding provided prognostic information) among APs, i.e.:
(1) The type of disclosure: prognostic disclosure vs. communication of unpredictability vs. non-disclosure.
(2) The content of disclosure: framing (standard vs. standard and best-case vs. standard, best- and worst-case survival scenarios) and precision (numerical vs. word-based estimates) of prognosis.
(3) The influence of individual characteristics (i.e., background, personal, and patient preferences) on effects of the type and content of disclosure (see Table A.1, Appendix, for hypotheses).
These scientific efforts could provide preliminary data to inform evidence-based guidelines to navigate oncologists in the challenging task of prognostic communication.
Methods
Study design
The current paper reports on 1 of 2 sets of planned analyses on data collected in a randomized controlled experimental study, using video-vignettes of a simulated consultation (van der Velden et al. Reference van der Velden, Smets and van Vliet2024). In our video-vignettes, professional actors portrayed a male patient with metastatic esophageal cancer, his daughter and a female oncologist, having a scripted discussion about treatment options with and without chemotherapy. Communication was standardized, yet we systematically manipulated the type and content of disclosure of prognosis.
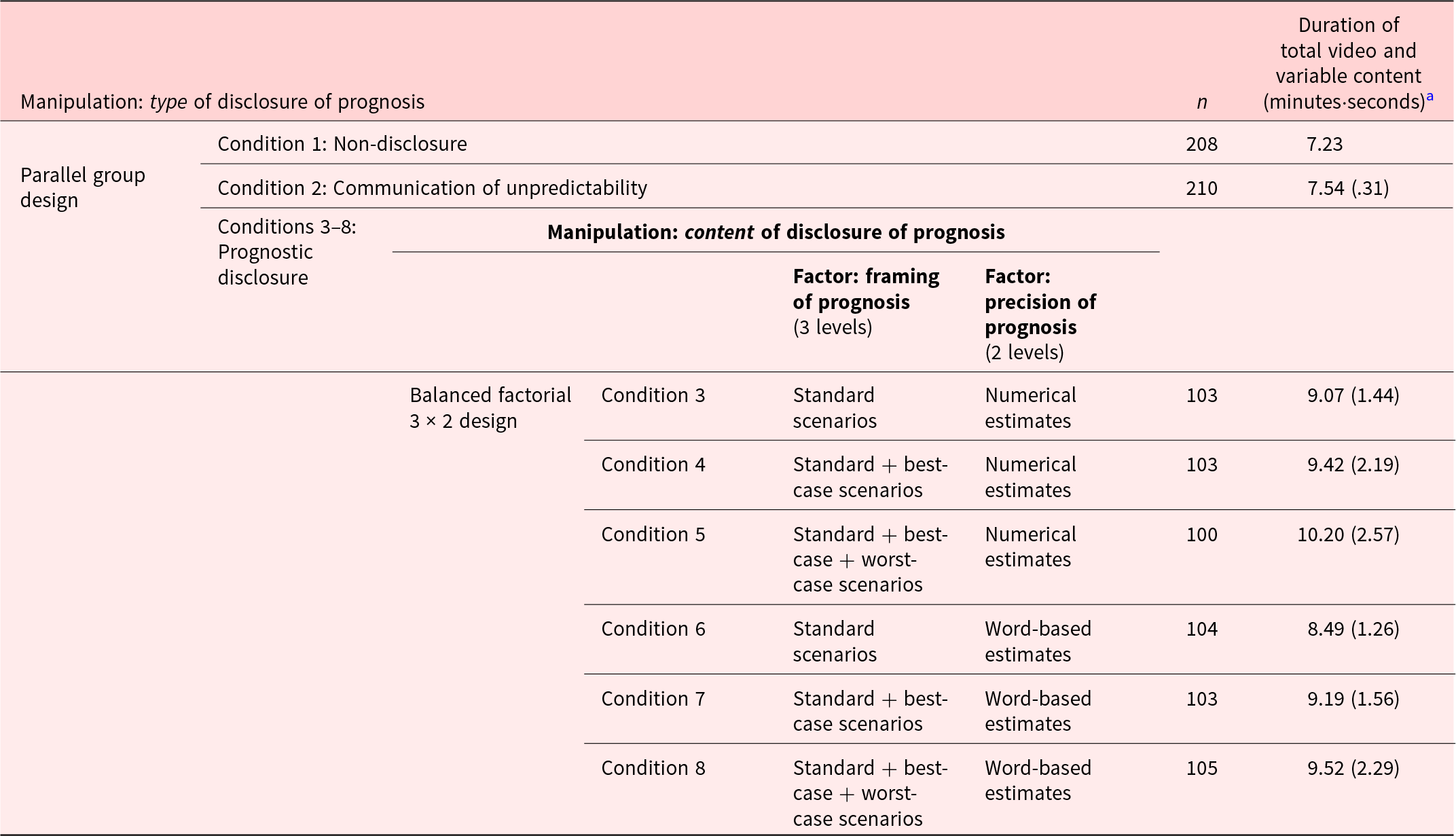
We adopted a parallel group design to examine the type of disclosure: prognostic disclosure vs. communication of unpredictability vs. non-disclosure. We further manipulated the content of disclosure conditions in a balanced factorial design, combining 2 factors: framing with 3 levels (standard vs. standard and best-case vs. standard, best- and worst-case survival scenarios) and precision with 2 levels (numerical vs. word-based estimates). This led to a total of 8 conditions, as shown in Table 1. Figure A.1 (Appendix) presents a visual overview.
Overview of conditions, including number of participants (van der Velden et al. Reference van der Velden, Smets and van Vliet2024)

n = sample size.
a The minutes and seconds between parentheses present the time of the video that includes variable content (i.e., manipulated prognostic communication).
Numerical estimates were derived from published clinical trial data (Cunningham et al. Reference Cunningham, Starling and Rao2008; Ter Veer et al. Reference Ter Veer, Haj Mohammad and van Valkenhoef2016). We used the group-level median overall survival for metastatic esophageal cancer with and without chemotherapy as standard scenarios and 90th and 10th percentiles of these curves as best- and worst-case scenarios, respectively (see Table A.2, Appendix, for the script including these manipulations).
Participants
Individuals were eligible for participation if they were ≥18 years and had Dutch proficiency, internet access, no audiovisual impairments, and no self-reported (previous) cancer diagnosis.
Study procedures
The institutional medical ethics review board provided exemption from formal approval (W20_347 # 20.385app). Recruitment of APs and data collection were handled by an independent research agency (Flycatcher Internet Research). The agency stratified eligible APs in their panel by sex, age (5-year interval groups), and education prior to recruitment, to include a sample representative of our target population, i.e., Dutch patients with stage-IV cancer. Data from Netherlands Cancer Registry and Statistics Netherlands were used for stratification.
The research agency sent baseline surveys (T0) to the stratified sample in their private, secure, digital platform. APs who provided informed consent and completed T0 received an outcomes survey (T1) after ≤3 weeks. APs responded to items immediately before (T1, pre-video) and after (T1, post-video) watching 1 randomly assigned video. APs were allocated to 1 condition upon starting the video, using blocked randomization with a predetermined fixed size and sequence, i.e., 1122345678. An allocation ratio of 2:1 was used for conditions 1 and 2 (non-disclosure and communication of unpredictability) to enable detection of effects of the type of disclosure. APs were compensated within a digital reward system. The research agency executed data validity checks after finishing data collection.
Development and piloting
Table A.3 (Appendix) describes development and piloting processes in detail, including example items and Cronbach’s alphas.
Study materials
Video-vignettes were developed by medical communication researchers and oncologists, consistent with published recommendations (Hillen et al. Reference Hillen, van Vliet and de Haes2013b; van Vliet et al. Reference van Vliet, Hillen and van der Wall2013b). The script (see Table A.2, Appendix) was based on previously audio-recorded oncological consultations, past video-vignette studies, and existing communication guidelines (Clayton et al. Reference Clayton, Hancock and Butow2007; Henselmans et al. Reference Henselmans, Smets and Han2017; Mori et al. Reference Mori, Fujimori and van Vliet2019; van der Velden et al. Reference van der Velden, van der Kleij and Lehmann2021; van Vliet et al. Reference van Vliet, van der Wall and Plum2013c).
Video-vignettes included an introductory waiting room scene, in which a voice-over conveys the backstory of the patient and instructs APs to imagine themselves being in the depicted situation. In a subsequent consultation-scene, the oncologist discusses treatment options. Except the non-disclosure condition, all conditions included supplementary content, comprising either communication of unpredictability or prognostic disclosure for treatment with and without chemotherapy. We created a script with standard survival scenarios, which could be supplemented with best-case scenarios only or also with worst-case scenarios (framing), and developed versions with either numerical or word-based estimates (precision).
We evaluated manipulation success, credibility, medical content, and overall quality of the script with video-vignette experts and oncologists and organized rehearsals with professional actors. Next, we recorded and piloted 8 test videos. We evaluated manipulation success, credibility, comprehensibility, emotional load, and overall quality of test videos, using semi-structured interviews (n = 13 cancer patients, 2 videos each) and online surveys (n = 120 cancer-naive individuals, 1 video each). After agreeing on an adjusted, final script, we professionally recorded 8 new videos and conducted semi-structured interviews with 5 more cancer patients for a “go or no-go” decision. Average video duration was 9 minutes and 3 seconds (range: 7.23–10.20 minutes/seconds).
Surveys
Surveys were piloted among 8 cancer-naive individuals (n = 2/8 providing “think-aloud” feedback (Eccles and Arsal Reference Eccles and Arsal2017); n = 6/8 providing feedback retrospectively) and pre-tested by the research agency.
Study procedures
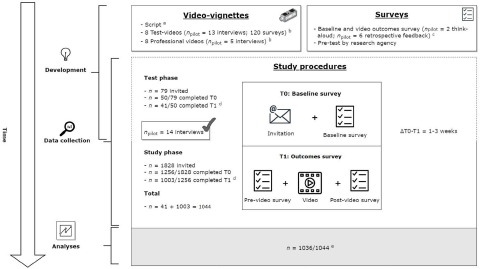
A subgroup of eligible APs took part in a test phase (April 2021; n = 41/79 completed participation) to enable evaluation of study procedures (n = 14/41 telephonic interviews). Hereupon, we slightly adjusted some survey instructions. As our study proved feasible, we proceeded with the study phase (May 2021; n = 1003/1828 completed participation). Figure 1 presents an overview of our study.
Overview of phases and procedures of this study (van der Velden et al. Reference van der Velden, Smets and van Vliet2024).

Measurements
Table A.4 (Appendix) describes all measures in detail.
Individual characteristics
We measured the following background characteristics (T0): sex, age, religion, education, knowledge of cancer, and experience with oncological consultations for a loved one. Regarding personal characteristics, we assessed trait optimism (Life Orientation Test-Revised (Scheier et al. Reference Scheier, Carver and Bridges1994)) and uncertainty tolerance (Tolerance for Ambiguity Scale (Geller et al. Reference Geller, Tambor and Chase1993)). After instructing APs to imagine being diagnosed with cancer, we measured patient preferences: prognostic information preference (“are you a person who wants to know your life expectancy? Yes/No” (Hagerty et al. Reference Hagerty, Butow and Ellis2004)) and attitude toward striving for length of life (Quality Quantity Questionnaire subscale (Stiggelbout et al. Reference Stiggelbout, Dehaes and Kiebert1996)).
Validity checks
To examine if manipulations were perceived as intended (T1, post-video), we assessed APs’ perceptions of the type and content of disclosure of prognosis. We also measured APs’ engagement with videos (shortened Video Engagement Scale [VES] (Lehmann et al. Reference Lehmann, Hillen and Verdam2023) and perceived video realism (Fruijtier et al. Reference Fruijtier, van der Schaar and van Maurik2022; Hillen et al. Reference Hillen, van Vliet and de Haes2013b; Lehmann et al. Reference Lehmann, Hillen and Verdam2023; Medendorp et al. Reference Medendorp, Visser and Hillen2017, Reference Medendorp, Hillen and Visser2021a; Visser et al. Reference Visser, Tollenaar and Bosch2017, Reference Visser, van der Velden and Smets2022, Reference Visser, Hillen and Verdam2016a, Reference Visser, Tollenaar and Bosch2016b, Reference Visser, Bol and Hillen2018). The shortened VES involves a screener item (i.e., “I was fully concentrated on the video while watching”; 1–7, “totally disagree” to “totally agree”); APs scoring ≤2 are excluded from analyses (Lehmann et al. Reference Lehmann, Hillen and Verdam2023).
Outcomes
Primary outcomes included APs’ emotional reaction (T1, pre-video; T1, post-video): differences in pre- and post-video scores on positive affect, negative affect (Positive and Negative Affect Scale (Watson et al. Reference Watson, Clark and Tellegen1988a)), and state anxiety (Spielberger State-Trait Anxiety Inventory-Short Form State subscale (Marteau and Bekker Reference Marteau and Bekker1992)). APs reported how they felt at that very moment (i.e., “now”).
For our secondary outcomes, we instructed APs to imagine being the depicted patient once again. We assessed APs’ coping with cancer (T1, post-video): helplessness/hopelessness (Mental Adjustment to Cancer subscale (Watson et al. Reference Watson, Greer and Young1988b)) and fighting spirit (Mini Mental Adjustment to Cancer subscale (Watson et al. Reference Watson, Law and Dossantos1994)). We also assessed APs’ appreciation of the consultation (T1, post-video): trust in the oncologist (Trust in Oncologist Scale-Short Form for APs (Hillen et al. Reference Hillen, Butow and Tattersall2013a, Reference Hillen, de Haes and Stalpers2014, Reference Hillen, Koning and Wilmink2012, Reference Hillen, Postma and Verdam2017)) and uncertainty (“the explanations this oncologist gives about my life expectancy seem hazy to me”; 1–5, “strongly disagree” to “strongly agree”), satisfaction (“how satisfied are you with the information you received from this oncologist about the general life expectancy of people with metastatic esophageal cancer?”; 0–10, “not at all satisfied” to “very satisfied”) and desirability (“would you like to receive information about life expectancy as was provided by the oncologist in the video?”; 1–5, “I certainly would not” to “I certainly would”) regarding provided prognostic information. Items on uncertainty, satisfaction, and desirability regarding provided prognostic information (adjusted from Mishel Uncertainty in Illness Scale (Mishel Reference Mishel1981; Mishel and Clayton Reference Mishel and Clayton2008) and Patient Satisfaction Questionnaire (Aalfs et al. Reference Aalfs, Oort and De Haes2007)) were omitted from the non-disclosure condition.
Statistical analysis
Power
Each of 6 prognostic disclosure conditions (videos 3–8; balanced factorial design) required 103 APs to detect main and moderating effects, based on a-priori G*Power analyses (f = .125, small–medium size; Analysis of variance (ANOVA); power: 80%; α = .05; df = 2). The non-disclosure and communication of unpredictability conditions (videos 1–2; parallel group design) each required 206 APs, resulting in a total sample of N = 1030.
Preparatory analyses
We checked scores for the screener item of the shortened VES. Manipulation success was examined by comparing proportions of APs who believed having watched a video with a certain manipulation among APs who truly watched a video with and without this manipulation (χ 2 tests). We tested differences between all 8 conditions for APs’ age, sex, and education (χ 2 tests, 1-way ANOVAs).
Primary analyses
To examine the independent effects of the type (prognostic disclosure vs. communication of unpredictability vs. non-disclosure) and content (framing and precision) of disclosure, we used separate multivariate analyses of variance (MANOVAs). For simultaneous significance testing of multiple outcomes, we clustered outcomes that were theoretically coherent and statistically correlated (r < .9) (Tabachnick et al. Reference Tabachnick, Fidell and Ullman2007). This led to 3 clusters: (1) emotional reaction (Δpositive affect, Δnegative affect, and Δstate anxiety, i.e., post-video scores minus pre-video scores; r = −.5 to .7); (2) coping with cancer (helplessness/hopelessness and fighting spirit; r = −.5); and (3) appreciation of the consultation (trust in the oncologist and uncertainty, satisfaction, and desirability regarding provided prognostic information; r = −5 to .5).
To investigate moderators, we added interaction terms of the type of disclosure, framing, and precision with APs’ individual characteristics. To prevent multiple testing, we chose unique interaction terms for each cluster of outcomes based on predefined hypotheses (see Table A.1, Appendix). We conducted mean centering for continuous moderators.
To determine significance of MANOVAs’ omnibus tests (α = .05), we evaluated Hotelling’s Trace test-statistic, given its alleged robustness for violation of multivariate normality and homogeneity of covariance matrices (Field Reference Field2005). If significant, we evaluated MANOVAs’ univariate follow-up tests, conducted post hoc analyses where necessary and reported statistics for models including moderators and interactions. We performed sensitivity analyses with Kruskal–Wallis and Mann–Whitney U tests for outcomes with distributions deviating from normality. Analyses were conducted with IBM-SPSS-26.
Results
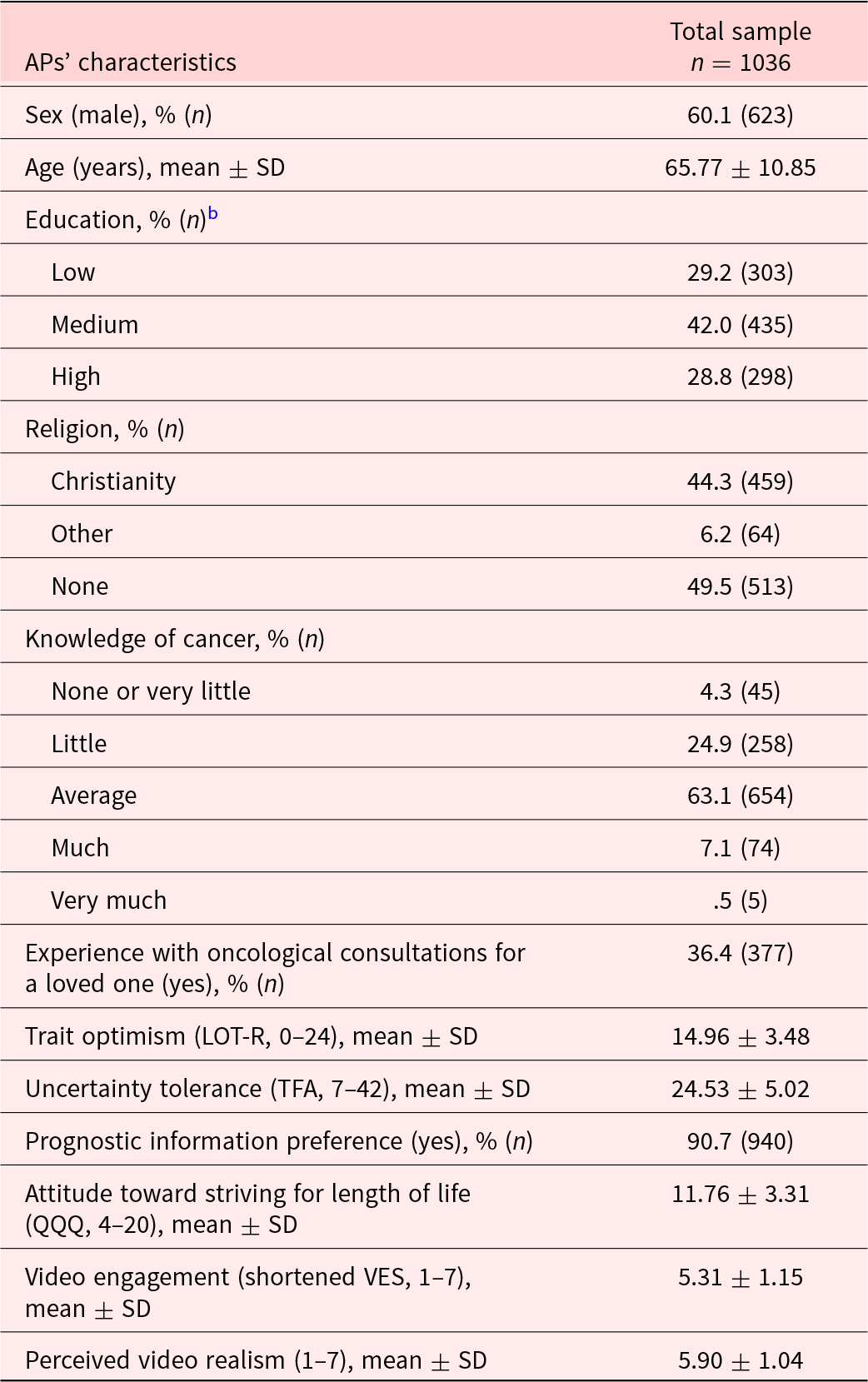
Of 1044 APs with complete data (response rate 55%; Figure A.2), we excluded 8 individuals with the shortened VES’ screener item (Lehmann et al. Reference Lehmann, Hillen and Verdam2023). Of 1036 APs in the analyses, 60% was male. Age ranged between 21 and 89 years (M age = 66). The majority of APs (63%) reported their cancer knowledge to be average. APs’ engagement with and perceived realism of videos were satisfactory (M Video engagement = 5.3, M Video realism = 5.9). Table 2 describes APs’ background characteristics.
Background characteristics of the total samplea

AP = analogue patient; n = sample size; SD = standard deviation; LOT-R = Life Orientation Test-Revised; TFA = Tolerance for Ambiguity Scale; QQQ = Quality Quantity Questionnaire; VES = Video Engagement Scale.
a The content of this table partly overlaps results of a different analysis (reported elsewhere (van der Velden et al. Reference van der Velden, Smets and van Vliet2024)) on the dataset used for the current paper.
b Low vocational education; medium level vocational education; high vocational or academic education.
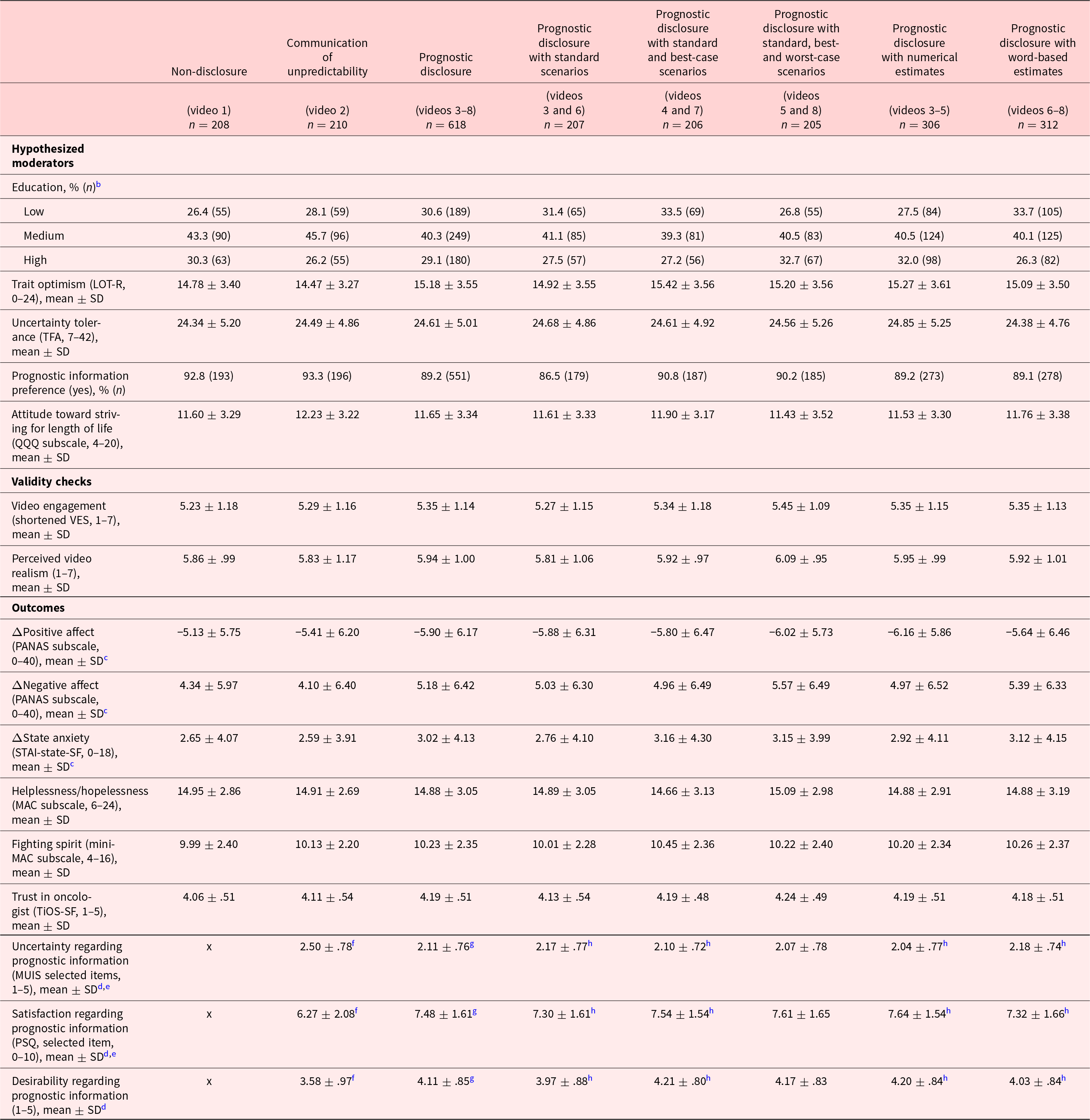
Manipulations were perceived as intended, although framing was less clearly perceived by APs than other manipulations, as shown in Table A.5. Table 3 describes the potential moderating characteristics (see Table A.1, Appendix, for hypotheses), validity checks and outcomes, stratified by manipulation. There were no significant differences in APs’ sex, age, or education between conditions.
Hypothesized moderators, validity checks, and outcomes (stratified by manipulation)a

n = sample size; SD = standard deviation; LOT-R = Life Orientation Test-Revised; TFA = Tolerance for Ambiguity Scale; QQQ = Quality Quantity Questionnaire; VES = Video Engagement Scale; PANAS = Positive and Negative Affect Scale; STAI-state-SF = State-subscale of the Spielberger State-Trait Anxiety Inventory-Short Form; MAC = Mental Adjustment to Cancer; TiOS-SF = Trust in Oncologist Scale-Short Form; MUIS = Mishel Uncertainty in Illness Scale; PSQ = Patient Satisfaction Questionnaire.
a The content of this table partly overlaps results of a different analysis (reported elsewhere (van der Velden et al. Reference van der Velden, Smets and van Vliet2024)) on the dataset used for the current paper.
b Low vocational education; medium level vocational education; high vocational or academic education.
c Difference scores were calculated by subtracting pre-video scores from post-video scores on positive affect (PANAS subscale), negative affect (PANAS subscale), and state anxiety (STAI-STATE-SF). Negative difference scores indicate reduced positive affect, negative affect, and state anxiety, respectively. Positive difference scores indicate increased positive affect, negative affect, and state anxiety, respectively.
d Items were not presented to APs in the condition with non-disclosure (video 1).
e Original (selected) items of the MUIS and PSQ were adjusted for this study’s purpose.
f 7 missings (n = 203/210 for communication of unpredictability).
g 6 missings (n = 612/618 for prognostic disclosure).
h 3 missings (n = 204/207 for disclosure with standard scenarios only; n = 203/206 for disclosure with standard and best-case scenarios; n = 303/306 for disclosure with numerical estimates; n = 309/312 for disclosure with word-based estimates). Missings occurred if APs indicated having watched a video without communication about prognosis.
The type of disclosure
Tables A.6–A.9 (Appendix) demonstrate all results. We found no significant overall effect of the type of disclosure on emotional reaction, nor significant moderating effects of APs’ prognostic information preference or uncertainty tolerance.
There was no significant overall effect of the type of disclosure on coping with cancer, nor significant moderating effects of APs’ trait optimism or attitude toward striving for length of life.
We found a significant overall effect of the type of disclosure on appreciation of the consultation (F(3, 807) = 3.932, p omnibus = .008, Hotelling’s Trace = .015). Univariate results showed that APs reported more satisfaction (F(1, 809) = 11.303, p < .001) with provided prognostic information after prognostic disclosure, compared to communication of unpredictability.
Confirming our hypotheses, we found a significant moderating effect of prognostic information preference (F(3, 807) = 3.451, p omnibus = .016, Hotelling’s Trace = .013). APs who preferred to know prognosis reported less uncertainty and more desirability regarding provided prognostic information after prognostic disclosure than communication of unpredictability, whereas APs who preferred not knowing reported less uncertainty and more desirability after communication of unpredictability instead (interactions: F uncertainty(1, 809) = 7.291, p = .007; F desirability(1, 809) = 6.268, p = .012).
Furthermore, we found a significant moderating effect of uncertainty tolerance (F(3, 807) = 2.794, p omnibus = .039, Hotelling’s Trace = .010). Opposing our hypotheses, APs with higher uncertainty tolerance considered information more desirable after prognostic disclosure than communication of unpredictability, whereas APs with lower uncertainty tolerance considered communication of unpredictability more desirable instead (interaction: F(1, 809) = 7.811, p = .005). Also contradicting our hypotheses, APs with higher uncertainty tolerance reported more trust in the oncologist after prognostic disclosure than non-disclosure, while APs with lower uncertainty tolerance reported more trust after non-disclosure instead (interaction: F(2, 1027) = 3.350, p = .035).
The content of disclosure
There were no significant overall effects of framing or the precision of prognosis on emotional reaction. We found a significant interaction between APs’ uncertainty tolerance and precision (F(3, 608) = 3.233, p omnibus = .022, Hotelling’s Trace = .016). Opposing our hypotheses, yet in line with aforementioned moderating effects, APs with higher uncertainty tolerance reported more positive affect, less negative affect, and less state anxiety after numerical rather than word-based estimates. APs with lower uncertainty tolerance reported more positive affect, less negative affect, and less state anxiety after word-based estimates instead (interactions: F positive affect(1, 610) = 5.983, p = .015; F negative affect(1, 610) = 7.867, p = .005; F state anxiety(1, 610) = 5.870, p = .016).
We found no significant overall effects of framing or the precision of prognosis on coping with cancer, nor significant moderating effects of APs’ trait optimism or attitude toward striving for length of life.
There was no significant overall effect of framing on appreciation of the consultation. However, we found a significant overall effect of precision (F(4, 593) = 2.978, p omnibus = .019, Hotelling’s Trace = .020). Univariate results showed that APs reported less uncertainty (F(1, 596) = 4.139, p = .042), more satisfaction (F(1, 596) = 7.791, p = .005), and more desirability (F(1, 596) = 5.792, p = .016) regarding provided prognostic information after numerical instead of word-based estimates. APs’ education or uncertainty tolerance did not moderate effects.
All aforementioned findings were confirmed in non-parametric sensitivity analyses.
Discussion
Prognostic information is important for patients with advanced cancer to accustom to the last phase of life (Butow et al. Reference Butow, Clayton and Epstein2020; van der Velden et al. Reference van der Velden, Meijers and Han2020). Disclosing prognosis, however, is challenging for oncologists and confrontational for patients (Franssen et al. Reference Franssen, Lagarde and Van Werven2009; Liu et al. Reference Liu, Landrum and Weeks2014). This study examined the effects of oncologists’ prognostic messages on affective outcomes, hereby advancing scientific guidance on treading the fine line between disclosing poor prospects and preserving patients’ emotional well-being. Overall, disclosure of (precise) prognostic estimates did not increase feelings of anxiety, negativity, or hopelessness nor decrease feelings of positivity or fighting spirit among APs. On average, individuals were more satisfied with prognostic disclosure than communication of unpredictability and generally considered numbers more satisfactory, desirable, and certain than word-based estimates. However, importantly, some of these effects depended on individuals’ prognostic information preference and uncertainty tolerance. Communication of best- and/or worst-case survival scenarios lacked effects on all outcomes.
Our finding that individuals with a preference for not knowing prognosis (comprising 9% of the sample) were less appreciative of prognostic disclosure makes sense, as they might feel that their needs were not met. Inherent to our design, the oncologist in the video disclosed prognosis irrespective of the (depicted or imagined) patient’s information preference. In clinical practice, overwhelming patients with more information than desired must be prevented at all times to avoid undue distress (Lehmann et al. Reference Lehmann, Labrie and van Weert2020). Our finding that disclosing (precise) prognostic information generally has no impact on individuals’ emotions or way of coping within an experimental setting, and that numbers yield more appreciation than words, resonates with van Vliet et al. (Reference van Vliet, van der Wall and Plum2013c), and with Mori et al. (Reference Mori, Fujimori and van Vliet2019). These video-vignette studies similarly found that numerical estimates do not evoke anxiety, yet do increase patients’ certainty and satisfaction (Mori et al. Reference Mori, Fujimori and van Vliet2019; van Vliet et al. Reference van Vliet, van der Wall and Plum2013c). Our interaction analyses revealed that prognostic disclosure leads to less desirability of information and trust in the oncologist, and numbers lead to more anxious, more negative, and less positive feelings in individuals who poorly tolerate uncertainty. Although these results contradict our hypotheses, the moderating effects of uncertainty tolerance show similar directions and, in fact, apparently corroborate previous research (van Vliet et al. Reference van Vliet, van der Wall and Plum2013c). Van Vliet et al. (Reference van Vliet, van der Wall and Plum2013c) found that numerical estimates increase anxiety and uncertainty and decrease satisfaction among “high monitors,” i.e., patients who, in the face of threat, seek ways to reduce uncertainty (van Vliet et al. Reference van Vliet, van der Wall and Plum2013c). We may speculate that individuals who dislike uncertainty do not benefit from prognostic estimates, because predictions about life expectancy are fundamentally uncertain (Han et al. Reference Han, Umstead and Bernhardt2017). More precise and/or extensive information does not necessarily decrease such uncertainty. Inspecting our manipulations, we may pose that the multiplicity of numerical estimates (e.g., survival with and without chemotherapy, survival gain, best-cases, and worst-cases) perhaps introduced complexity, which only added uncertainty (Han et al. Reference Han, Umstead and Bernhardt2017). Altogether, prognostic estimates possibly prompt more questions, which is unsettling to individuals with low uncertainty tolerance (Han et al. Reference Han, Klein and Lehman2009; Rains and Tukachinsky Reference Rains and Tukachinsky2015; Street et al. Reference Street, Elwyn and Epstein2012). Opposed to individuals with low uncertainty tolerance, individuals with a preference for knowing prognosis (comprising 91% of the sample) particularly appreciated prognostic disclosure, which implies that those who poorly tolerate uncertainty are not necessarily the same individuals as those who seek prognostic information. As researchers theorize that low uncertainty tolerance fuels the appraisal of threat, exacerbating distress, it could be that those individuals benefit from more affective communication (e.g., addressing emotions and reassuring continued care), alleviating distress, rather than more precise information (Chasiotis et al. Reference Chasiotis, Wedderhoff and Rosman2021; Reis-Dennis et al. Reference Reis-Dennis, Gerrity and Geller2021; Taha et al. Reference Taha, Matheson and Cronin2014).
Apart from aforementioned moderating effects, there was insufficient evidence for many predefined hypotheses about moderators. For example, opposing our expectations, individuals’ educational level did not influence responses to numerical estimates or different survival scenarios, which disaffirms the conception that highly educated patients specifically value more detailed prognostic information (Franssen et al. Reference Franssen, Lagarde and Van Werven2009; Kiely et al. Reference Kiely, McCaughan and Christodoulou2013; Loiselle Reference Loiselle2019; Mayer et al. Reference Mayer, Terrin and Kreps2007).
Our research has several limitations. First, our methodological choices engender limited ecological validity. For ethical reasons, we included disease-naive individuals, who are valid proxies for actual patients according to a previous meta-analysis (van Vliet et al. Reference van Vliet, van der Wall and Albada2012). While scores for perceived video realism and video engagement were satisfactory in the current study, watching a video-vignette clearly does not equal being in an actual consultation and cancer-naive individuals do not experience the physical, emotional, and existential burdens of advanced cancer. Hence, it is plausible that cancer-naive individuals may react less emotionally than patients, who need to reconcile their own existence with the inevitable state of nonexistence upon death. Clinical research previously observed mixed effects of prognostic disclosure on emotional well-being (Cripe et al. Reference Cripe, Rawl and Schmidt2012; Enzinger et al. Reference Enzinger, Zhang and Schrag2015; Fletcher et al. Reference Fletcher, Prigerson and Paulk2013; Nakajima et al. Reference Nakajima, Hata and Onishi2013; Shin et al. Reference Shin, El-Jawahri and Parkes2016), but those studies investigated delayed instead of immediate emotional responses and could not infer causality. Thus, although we recognize that extrapolation of our findings to clinical practice is speculative, we believe that manipulation of prognostic communication in a more ecologically valid way would not be ethically justified without at least some substantiation from experimental research with APs, especially since current evidence for this hard-to-study topic is at a preliminary stage. Future research can build on this video-vignette experiment through replication among individuals with a cancer diagnosis or a history of cancer to enhance real-world impact. Using more ecologically valid methods, virtual reality technologies allow systematic testing of prognostic communication elements within more realistic settings. Experiments may ultimately inform an intervention addressing prognostic communication skills for oncologists; its effectiveness could be tested in a clinical RCT. Researchers could audiotape oncologist-patient conversations to analyze whether the prognostic communication skills taught in the intervention are endorsed. A second limitation may be our manipulation of framing. Sixty percent of participants reported to recall additional survival scenarios on top of the standard scenarios, while viewing videos without such information (Table A.5). Perhaps, our standard survival scenarios essentially reflected a best-/worst-case format (e.g., “months to a few years”). More research is necessary to substantiate evidence on different survival scenarios. Third, we did not establish validity of items that were tailored to this study, i.e., appreciation of the consultation, nor did we determine thresholds for the clinical importance of statistical differences in our outcomes. Finally, given that prognostic communication is considered culturally sensitive, generalizability of our results may be restricted by the Dutch study setting. The Dutch culture places value on knowledge, autonomy, and straightforwardness. It is conceivable that patients from non-Western countries hold different attitudes toward prognostic communication (Surbone Reference Surbone2008). Unfortunately, our study lacks insight into participants’ demographic information like race, ethnicity, or immigration status. Also regarding systematic disparities in health care, it is important to note that we used (biological) sex-disaggregated data, which do not consider gender identity. Strengths include our ability to draw causal conclusions about the independent effects of prognostic communication strategies, extensive pilot-testing procedures, and use of a large, stratified sample.
Conclusion
Based on this experimental study, we tentatively conclude that the disclosure of prognosis does not necessarily cause more emotional harm than non-disclosure. Prognostic disclosure is particularly appreciated by patients who prefer to receive such information and those who tolerate uncertainty well. Generally, numerical estimates yield more appreciation than prognostic information in words. Yet, numerical estimates may evoke more negative emotions in patients with low uncertainty tolerance. When providing prognostic information in clinical consultations, it remains crucial that oncologists acknowledge and act on individual variation in patient preferences and personal characteristics.
Practice implications
Responding to oncologists’ discomfort with communicating prognosis, our results may potentially relieve worries about undermining hope or causing emotional harm. Despite the preliminary nature of findings, this study stipulates that oncologists’ fears must not preclude offering prognostic information. In line with previous literature and our findings on moderating effects of information preference, we advocate firstly asking patients if they want prognostic information, as well as assessing their preferences for the content and timing of disclosure (Clayton et al. Reference Clayton, Hancock and Butow2007; Gilligan et al. Reference Gilligan, Coyle and Frankel2017; Lehmann et al. Reference Lehmann, Labrie and van Weert2020; van der Velden et al. Reference van der Velden, van Laarhoven and Burgers2022b).
Our observation that prognostic disclosure versus communication of unpredictability and numerical versus word-based estimates generally promote satisfaction may stimulate provision of precise prognostic information. When navigating the delicate balance between realism and hope (Olsman et al. Reference Olsman, Leget and Onwuteaka-Philipsen2014), oncologists could allude to explaining different survival scenarios. Although the added value of this communication strategy remains unclear, it may be reassuring that disclosure of worst-case scenarios, in addition to best-case scenarios, is not necessarily upsetting. Importantly, our study does not imply that patients will not be moved by bad news. It is crucial for oncologists to allow space for emotions, listen and acknowledge patient concerns with empathy (Back and Arnold Reference Back and Arnold2006; Westendorp et al. Reference Westendorp, Evers and Stouthard2022).
Even more so, our results suggest sensitivity as to which prognostic communication strategies are beneficial for whom. Uncertainty tolerance appears to play an important role in how individuals react to prognostic information. It, therefore, seems valuable for oncologists to explore how patients generally deal with uncertainty, address the inherent uncertainty of prognostic estimates, and support patients in coping with prognostic uncertainty (Medendorp et al. Reference Medendorp, Stiggelbout and Aalfs2021b). Oncologists could, for example, accentuate controllable elements of an uncertain situation by making concrete follow-up plans and explicating their continued involvement in patient’s care (Medendorp et al. Reference Medendorp, Stiggelbout and Aalfs2021b). Future research must further clarify the mechanisms underlying the association between prognostic communication and uncertainty tolerance. Additionally, while we found no moderating effects of education, trait optimism, and attitude toward striving for length of life, more studies should increase knowledge on tailoring prognostic communication.
Supplementary material
The supplementary material for this article can be found at https://doi.org/10.1017/S1478951524000403.
Acknowledgments
The authors thank Onderwater Productions en Whaleshark Productions for developing the video-vignettes. The authors furthermore thank the individuals who took part in this study’s pilot tests and data collection.
Funding
This work was supported by the Dutch Cancer Society (grant number 11547).
Competing interests
The authors declare no conflicts of interest.