For the past three decades, concerns have been raised in Europe and North America about ethnic/racial inequalities in access to mental healthcare, institutional racism, and cultural misunderstandings of idioms of distress based on ignorance, prejudice and racial stereotyping; these impinge on diagnostic accuracy and ultimately lead to the pathologisation of culture and culturally adaptive behaviours. Fundamental changes in routine clinical practice were called for, in order to address these concerns. Understanding explanatory models and eliciting them during assessment and treatment were suggested components of culturally competent practice.
The term ‘explanatory model’ was introduced by Reference Kleinman, Eisenberg and GoodKleinman et al (1978), who defined it as the complex, culturally determined process of making sense of one's illness, ascribing meanings to symptoms, evolving causal attributions, and expressing suitable expectations of treatment and related outcomes. More simply, explanatory models might be described as culturally determined beliefs that individuals hold about misfortune, suffering, illness and health. These models are shaped by and shape societal expectations of the sick role, individual illness behaviour and help-seeking. Research has shown that explanatory models are not static entities or single constructs, but can be fluid, multilayered and complex constructs that may change in response to a number of factors, including the type of questioning, the relationship with the clinician, mood and migration history (Reference Kirmayer, Bhugra, Salloum and MezzichKirmayer 2009; Reference Ghane, Kolk and EmmelkampGhane 2010). The exploration of explanatory models in the clinical encounter provides valuable information about the significance of the illness for the patient and their family, and helps to build an understanding of their wider beliefs systems, therefore allowing the richness of the patient's world views to emerge in a narrative form.
Cultural capability, defined as a set of skills enabling clinicians to work effectively with patients from a diversity of cultural and ethnic backgrounds, was proposed as a way of reducing ethnic variation in experience of healthcare and improving outcomes. Explanatory models have since been routinely included in most cultural capability training programmes. However, the routine exploration of explana tory models has not yet been fully integrated into common clinical practice, for a variety of reasons. In this article, we argue that the exploration of explanatory models should become part of the routine mental health assessment through the ‘cultural formulation’, given its importance for diagnostic accuracy. We also argue that culture shapes patients’ experience and expression of mental illness and their personal understanding of recovery. The routine exploration of explanatory models should therefore form the basic platform for formulating and implementing treatment plans. Yet, this is a complex task. Reference William and HealyWilliam & Healy (2001) showed that explanatory models, unlike cognitions, do not always consist of a concrete, fixed set of beliefs, but can be construed as multiple explanations, held simultaneously, some transient in nature. They recommended the term ‘explanatory map’ rather than explanatory model, to reflect the complexity of such belief systems.
Explanatory models and patient outcomes
It is commonly accepted among healthcare professionals, and emerging in the research literature, that exploring explanatory models can be a powerful tool to enhance clinical outcomes. There is a voluminous literature on how patients’ illness perceptions relate to illness outcomes, including emotional distress, recovery and treatment adherence. Most of this literature comes from the field of health psychology, where illness perceptions and their impact on patient outcomes have been researched extensively over the past 40 years. For example, the Illness Perceptions Questionnaire (IPQ), based on the cognitive model of illness representations (Reference Leventhal, Mever, Nerenz and RachmanLeventhal 1980), has been used with a number of illness groups (e.g. chronic fatigue syndrome, chronic pain, diabetes and stress) and has shown the importance of such representations in relation to outcomes. Psychiatric research into explanatory models, however, began a lot more recently and any research on their use in clinical practice is still very immature. Most has been focused on differences in explanatory models among ethnic groups, rather than on their relationship to clinical outcomes. Therefore, while more research is needed into the clinical use of explanatory models in mental healthcare, evidence from their clinical use in physical healthcare is particularly encouraging.
In health psychology, research into illness perceptions (which are similar to explanatory models) has been concerned with five illness dimensions: illness identity, time line, causes/attributions, consequences and control/cure. A meta-analysis found relationships between illness perceptions and psychological distress, perceived illness consequences, low control/cure beliefs, and longer perceived duration of illness (Reference Hagger and OrbellHagger 2003). A number of (mostly) more recent studies have also shown that illness perceptions are associated with future negative outcomes, including slow recovery (e.g. Reference Galli, Ettlin and PallaGalli 2010; Reference Kaptein, Bijsterbosch and ScharlooKaptein 2010), lack of adherence to treatment (Reference Weinman, Petrie and SharpeWeinman 2000; Reference Halm, Mora and LeventhalHalm 2006) and even mortality (Reference Chilcot, Wellsted and FarringtonChilcot 2011).
Explanatory models and the DSM
Psychiatry has long been suffering from an unspoken tendency to affirm its universal applicability. It was not until the publication of DSM-III-R (American Psychiatric Association (APA) 1987) that a cautionary note about the cross-cultural applicability of diagnostic categories was included in the manual's introduction. DSM-IV (APA 1994) acknowledged more clearly the role of culture through the inclusion of ‘culture-bound syndromes’ and (in Appendix 1) an outline for the cultural formulation, which offers a framework for assessment of the cultural aspects of an individual's mental illness structured in five domains. Within this framework, explanatory models feature as ‘cultural explanations of illness’ (domain 2). However, few clinicians used this outline, partly because of the lack of a set of standardised questions that could easily be used in routine clinical assessments.
Despite this progress in acknowledging the role of culture in clinical presentations, with its diagnostic and therapeutic implications, most of the original recommendations of the DSM task force on culture and psychiatric diagnosis were eventually rejected, and the task force's efforts to enhance the cultural validity of DSM-IV mostly failed (Reference Lewis-FernándezLewis-Fernández 1996). By substantially reaffirming the universal validity of its diagnostic categories, despite some cultural caveats, DSM-IV essentially failed to recognise that all psychiatric categories are culturally construed (Reference LittlewoodLittlewood 1996).
DSM-5 (APA 2013) shows further progress in acknowledging the cultural aspects of clinical symptoms, diagnosis and care planning. As in DSM-IV, the DSM-5 chapter on cultural formulation features a framework comprising five subsections for assessing the cultural features of mental health problems. DSM-5 also features a more prescriptive Cultural Formulation Interview, articulated in 16 questions that clinicians might use to elicit information about key cultural aspects of the clinical presentation. Explanatory models are elicited in section 2, through a sequence of four questions exploring the patient's, and their community's, causal attributions, perceived stressors and contextual support.
In the USA, DSM-5 is used for routine assessments regarding cultural formulations and interviews. In the UK, there is no formal procedure for implementing a cultural analysis in daily clinical practice. As a result, interest in the cultural aspects of mental illness and commitment among clinicians to search through this area can be variable. Overall, clinical encounters in mental health settings are still oriented towards making a diagnosis and formulating a treatment plan, managing risk, pursuing guideline adherence and efficiently administering the necessary outcome measures and administrative requirements; this inevitably leads to partial or total neglect of the complexity of the patient's total experience of illness and their world view.
The use of explanatory models
Since Kleinman et al's original formulation of explanatory models (1978), a number of tools have been developed to elicit explanatory models in the clinical interview (Table 1). Based on Reference KleinmanKleinman's (1980) pioneering work, Weiss developed the Explanatory Model of Illness Catalogue (EMIC), a semi-structured interview for systematically eliciting explanatory models to explore ethnic differences in patterns of distress, stigma towards illness, perceived causes of current problems and help-seeking practices (Reference WeissWeiss 1997).
TABLE 1 Instruments for assessing explanatory models
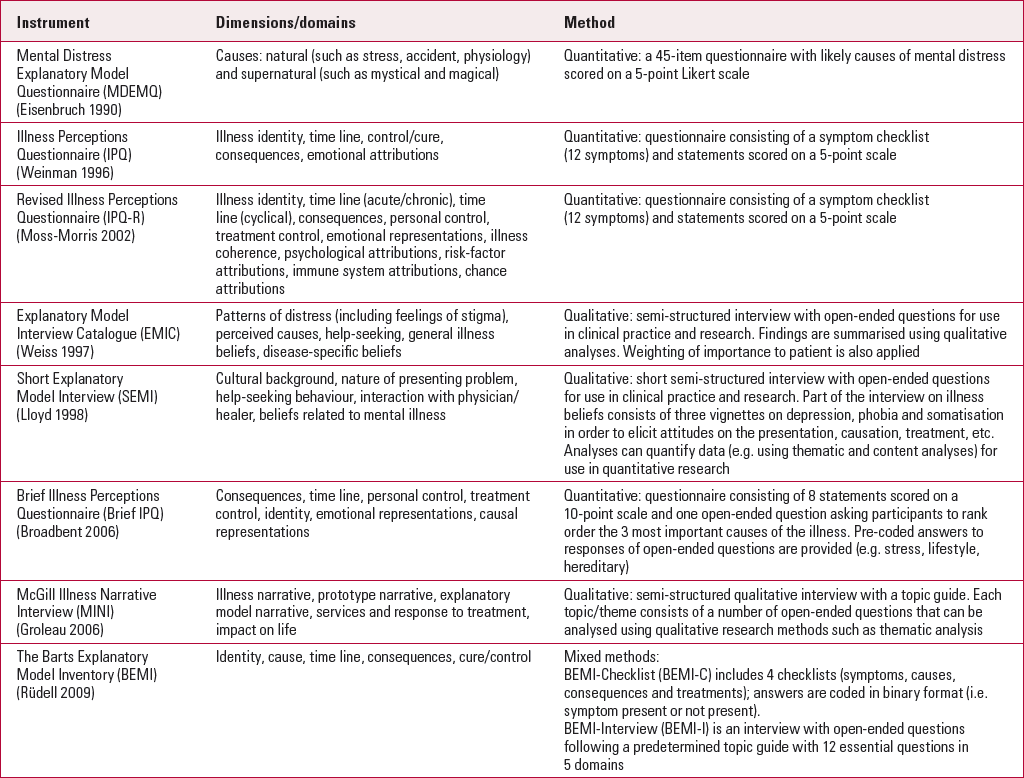
Another assessment tool, the Short Explanatory Model Interview (SEMI), was developed for use in epidemiological studies and has been used to explore explanatory models among patients and healthcare workers in a variety of settings (Reference Lloyd, Jacob and PatelLloyd 1998).
Explanatory models received a lot of attention in the field of health psychology and can be applied to a number of mental and physical illnesses. For example, the IPQ was developed to assess illness using five dimensions (identity, causal attributions, time line, consequences and cure) and has generated a lot of research (Reference Leventhal, Mever, Nerenz and RachmanLeventhal 1980; Reference Weinman, Petrie and Moss-MorrisWeinman 1996). A revised, more statistically robust version was introduced (IPQ-R; Reference Moss-Morris, Weinman and PetrieMoss-Morris 2002) and a shorter version, consisting of 9 items, was also developed (Reference Broadbent, Petrie and MainBroadbent 2006). Another tool, the McGill Illness Narrative Interview (MINI), is an open-ended semi-structured interview designed to elicit chain complexes, prototypes and explanatory models (Reference Groleau, Young and KirmayerGroleau 2006).
While these assessment tools have proved useful for research, they are rather complex for clinical use. To meet the need for an ethnographic method of assessing explanatory models that health professionals could administer quickly and with minimal training, Reference Rüdell, Bhui and PriebeRüdell et al (2009) developed a brief mixed-methods assessment tool, the Barts Explanatory Model Inventory and Checklist (BEMI), for use with any physical and mental disorder. This can be used in clinical settings to elicit both explicit and implicit illness perceptions such as illness experiences, causal attributions, symptoms, help-seeking behaviours, desired solutions and treatment response.
As Table 1 shows, there are a number of qualitative and quantitative instruments for measuring explanatory models and there is no accepted gold standard. It can be argued that those based on interviews would provide richer data and a better understanding of illness representations and experiences. However, qualitative designs are a lot more time-consuming in terms of both eliciting information and analysing the data, whereas quantitative designs can gather information about individuals much more quickly and can facilitate investigation of representations of illness in larger samples (Reference Weinman, Petrie and Moss-MorrisWeinman 1996).
Explanatory models in different diagnostic groups
The way people perceive, interpret and respond to suffering is mediated by both cultural and social contexts as well as the illness or disorder itself. We now set out examples of different diagnostic categories of mental illness and their relationship with explanatory models in different ethnic groups.
Medically unexplained somatic symptoms or somatoform disorders
Several studies suggest that a significant number of patients visiting primary care services are diagnosed with medically unexplained symptoms or, as such symptoms are often labelled, somatoform disorders (Reference Kirmayer, Groleau and LooperKirmayer 2004). Many medically unexplained symptoms have a cultural basis and incorporate or are mediated by cultural beliefs and idioms of distress (Reference Bhui and DinosBhui 2008). Such beliefs can be related to causal attributions of symptoms, which can influence how such symptoms are presented in a clinical setting (Reference Bhui, Bhugra and GoldbergBhui 2002).
Cultural, social and contextual factors can also influence what is acceptable or ‘normal’ in a given context in terms of disclosure of symptoms. In particular, emotional and/or psychological expressions of distress have a significant cultural component attached to them in terms of acceptability and stigmatisation, and therefore physical expressions of symptoms may be deemed more acceptable (Reference Groleau and KirmayerGroleau 2004). Research in the UK and elsewhere suggests that the majority of patients presenting with unexplained somatic symptoms have common mental disorders (e.g. Reference Weich, Lewis and DonmallWeich 1995; Reference Nambi, Prasad and SinghNambi 2002). An international study among 14 countries reinforces clinical impressions that unexplained somatic symptoms are associated with psychiatric illness (Reference Kisely, Goldberg and SimonKisely 1997).
Common mental disorders
Common mental disorders such as anxiety and depression vary considerably across cultural and social contexts in terms of prevalence, symptomatology, treatment and help-seeking behaviour (Reference Kirmayer, Jarvis, Stein, Kupfer and SchatzbergKirmayer 2006). Studies in India have shown that common mental disorders are not understood as ‘mental illness’ – that term is used mostly to refer to psychotic disorders (Reference Patel, Todd and WinstonPatel 1997). Many of the causes and symptoms of common mental disorders are not only related to cultural norms, but can also be shaped by how cultural values influence and attach meaning to self-related concepts and psychological constructs such as guilt, blame, trust, self-esteem and locus of control (Reference Bhugra, Gupta and WrightBhugra 1997). For example, explanatory models that invoke an external locus of control have been found to be significantly related to poor prognosis in depression (Reference Bann, Parker and BradwejnBann 2004). Culture, society and religion attach different meanings to such constructs and therefore influence how information is processed and filtered through cognitive schemas. These constructs may also be central to symptoms associated with anxiety and depression.
According to Reference Henningsen, Jakobsen and SchiltenwolfHenningsen et al (2005), causal attributions for common mental disorders are significantly related to functional and social impairment and prognosis. Evidence suggests that symptoms associated with common mental disorders may not be labelled or recognised as mental health problems, but either explained in somatic terms or attributed to social, contextual, religious or spiritual factors (Reference Bhui and DinosBhui 2008). This is not necessarily a problem, since many of these attributions may elicit coping responses that can help the individual to manage depressive or anxiety-related symptoms. The challenge arises when explanatory models recommend treatments that are not congruent with clinical practice. Hence, interventions that include an understanding of causal attributions in a particular cultural context can be clinically effective (Reference Hinton, Chhean and PichHinton 2005).
A study conducted to assess explanatory models for common mental disorders among different ethnic groups in the UK found that, irrespective of ethnicity, all groups were more likely to explain consequences in behavioural and financial terms and to prefer complementary treatments (Reference Bhui, Rüdell and PriebeBhui 2006). However, compared with the White British group, respondents in the Bangladeshi and Black Caribbean groups were more likely to make causal attributions in spiritual and/or supernatural terms and showed a preference for medical and spiritual treatments. Making causal attributions using spiritual and supernatural explanations is frequently found in schizophrenia (e.g. Reference McCabe and PriebeMcCabe 2004) as well as in common mental disorders (Reference Lloyd, Jacob and PatelLloyd 1998; Reference Bhui, Bhugra and GoldbergBhui 2001).
Studies conducted outside of the UK have found causal attributions to be related to social factors, rather than spiritual or supernatural factors. For example, a study conducted in Zambia to explore causal explanatory models among low-income women with depression and/or stress found that the most significant causes identified as contributing to the illness were material factors and relationships (Reference Aidoo and HarphamAidoo 2001). In addition to poverty, material factors also included lack of education and economic opportunities. Relationships were mostly translated into unhappy marital relationships, very often involving violence. Similar results have been found in India, where the majority of patients with common mental disorders made psychosocial causal attributions for their illness (Reference Andrew, Cohen and SalgaonkarAndrew 2012), poor marital relationships, interpersonal difficulties, financial strain and violence in their daily lives (Reference Rodrigues, Patel and JaswalRodrigues 2003; Reference Patel, Kirkwood and PednekarPatel 2006; Reference Kermode, Herrman and AroleKermode 2007; Reference Pereira, Andrew and PednekarPereira 2007; Reference Shidhaye and PatelShidhaye 2010).
Psychotic disorders
The exploration of explanatory models in psychotic disorders is of particular importance as research has shown that ethnic minorities are significantly more likely to be diagnosed with a psychotic disorder (Reference DinosDinos 2014). Additionally, they express significantly more dissatisfaction with mental health services; such findings are evident in Europe and the USA (e.g. Reference Bhugra and BhuiBhugra 1998; Reference Selten, Veen and FellerSelten 2001; Reference Bhui, Stansfeld and HullBhui 2003). A lot of the literature has been preoccupied with the cultural context of what would be described as psychotic symptoms rather than cultural idioms of distress. Possession by demons, as well as experiences involving God, spirits or other extra-mundane phenomena, are some explanations that can be influenced and vary by social, cultural and subcultural contexts and that can also reflect psychopathology (Reference Kirmayer, Santhanam, Halligan and BassKirmayer 2001; Reference Saravanan, Jacob and JohnsonSaravanan 2007). In many cultures, such experiences can be described or understood through religious and cult practices. For such experiences to be labelled as psychotic, they need to be unexplainable from a cultural perspective or in terms of what would be considered acceptable in a local context and by the patient's peer group. The suggestion that such experiences reflect explanatory models privileges the idea of cultural and subcultural influences rather than a psychotic illness (Reference Seligman and KirmayerSeligman 2008).
Reference McCabe and PriebeMcCabe & Priebe (2004) compared explanatory models of illness in schizophrenia among four cultural groups in the UK: White, Bangladeshi, African Caribbean and West African. Results showed that concepts of illness and labels given to the illnesses were not statistically significantly different among the four groups, whereas the perceived cause of illness was both significantly different and significantly related to treatment satisfaction. In particular, those in the White group were more likely to attribute the illness to biological causes, whereas those in the other three groups were more likely to attribute it to supernatural forces. Among the latter groups, Bangladeshis were more likely to prefer either non-medical treatments (e.g. religious activities) or no treatment, whereas Whites were more likely to prefer medical treatments, including counselling. Interestingly, individuals who used biological explanatory models as opposed to social ones were significantly more satisfied with the treatment they were receiving and reported more satisfactory relationships with healthcare professionals.
It can be argued that the more positive results for those with biological explanatory models may stem from the fact that, in the UK, patients would be receiving treatments based on the medical/biological model (Reference McCabe and PriebeMcCabe 2004), a finding that has support in earlier research (Reference Callan and LittlewoodCallan 1998). A more recent study (Reference Owiti, Ajaz and AscoliOwiti 2014) found that ethnic minority patients in secondary care attributed causes of illness mainly to emotional and psychological factors, perhaps reflecting that, over the generations and with acculturation, the explanatory models of ethnic groups evolve and move towards the dominant cultural types.
Routine exploration of explanatory models in clinical work: usefulness, dilemmas and limitations
The psychiatric institution within the UK's National Health Service (NHS), with its wide variety of clinical presentations, culturally diverse patients and staff, and multiple care settings, offers a unique position from which to study explanatory models, their course over time, and their dependence on cultural and social contexts. When a patient's explanatory model significantly differs from or clashes with the standard Western psychiatric paradigm, such that treatment preferences are not easy to fulfil within the NHS, significant dilemmas arise as to the extent to which clinicians should modify their practice and accommodate the explanatory model in a treatment plan. Another interesting aspect of the public psychiatric institution is the cultural diversity of its staff, explanatory models being sometimes held with equal strength by both the patients and the workforce. This organisational context offers opportunities for the exploration and the resolution of ethical and cultural dilemmas within clinical teams and contradictory explanatory models.
The following fictitious case vignettes illustrate the clinical dilemmas that can arise from lack of knowledge and skills in engaging with cultural experiences in the clinic.
Case vignette: Psychotic illness makes a patient vulnerable to spirit possession
FN is a 55-year-old Nigerian man who belongs to a Christian Pentecostal religious group. He has a schizoaffective disorder and was brought to hospital for an acute relapse characterised by auditory hallucinations of religious content, agitation, hyperactivity, elated mood, religious delusions, formal thought disorder bordering on a confusional state, and disorganised and chaotic behaviours such as defecating in the ward corridor and stripping naked in public spaces. After 6 weeks of insufficient improvement on generous doses of psychotropic medications, his wife requests a consultation with the treating team. She states that she is well aware of the diagnosis of schizoaffective disorder and the importance of regular adherence to medication, which has kept her husband well for many years. However, besides the symptoms of the mental condition, she can also detect clear signs of spirit possession, for example, when her husband claims to be able to hear the voices of deceased family members. The wife asks the treating team to address the clinical symptomatology more aggressively with psychotropic medications, so that when her husband is ‘mentally stronger’ she will be able to bring in their pastor for a religious healing ceremony. She believes it was the psychotic relapse that increased her husband's vulnerability to spirit possession, hence she requests that the doctors address the former to enable the pastor to take care of the latter.
This case illustrates how explanatory models are complex, multifaceted, dynamic and fluid; they develop following the life vicissitudes of people inhabiting and moving within a globalised world, where migration allows access to multiple remedies (Western medicine, religious healing, ‘alternative medicine’, etc.). Patients will therefore ‘shop around’, experiment with what is available to treat their ailments and, in the process, they will incorporate effective interventions of different nature based on multiple explanatory models, allowing them to resort to various sources of help and treatment. The idea of treating the psychotic illness more effectively in order to make the patient accessible to the pastor's exorcism is typical of non-conflictual explanatory models that motivate the patient to receive medical treatment.
Case vignette: The importance of attending to multiple explanatory models held by patients and staff
NP is a 19-year-old man of Somali origin who presents to services for the first time because of an acute manic episode with psychotic symptoms. His presentation is characterised by agitation, insomnia, highly elated mood, logorrhoea, flight of ideas, formal thought disorder, and auditory hallucinations, delusions and delusional interpretations, all of a religious content. On the day of the admission to hospital, NP attacks a woman on the street on the grounds that a dog barking at her signifies that she is evil and must be killed. NP is admitted to the psychiatric intensive care unit, where he spends a few weeks experiencing a florid set of symptoms that appear to be resistant to generous doses of antipsychotics and mood stabilisers. NP's family accepts that they have a strong family history of affective disorders, with NP's first-degree relatives all affected by bipolar disorder (types 1 and 2), recurrent depression and dysthymia. However, they are shocked by the strength of the religious content of NP's symptoms (hearing the voice of God, praying excessively, questioning the interpretation of the Quran by the Imam at the mosque) and they come to the conclusion that he is possessed by an evil jinn (spirit). After a prolonged lack of success with medications, the family requests the intervention of an Islamic religious healer. An agreement between the clinical team and family is made on the acceptable healing procedures. When the healer attends the ward, the nurses refuse to give any assistance to the procedure, out of the concern that once the spirit leaves NP's body, it might possess a staff member. A second healing ceremony is agreed and carried out with the help of different nurses. Following a slow clinical improvement and subsequent discharge, NP is readmitted within 2 weeks with an identical set of symptoms, after the community psychiatrist halves the dose of NP's medications at the request of NP and his family. The clinical team wonders whether, in an effort to explore and accommodate the family's explanatory models, the necessary psychoeducation about the biological aspects of mania and the importance of treatment adherence was neglected during NP's inpatient stay.
This case shows how resorting to a particular explanatory model can be linked to a variety of factors, such as the particular type of clinical presentation as well as the lack of response to a specific treatment. Different explanatory models, such as the biomedical and the spiritual, can coexist without clashing. Staff equally hold beliefs and explanatory models outside of their professional training and codes of practice. Furthermore, well-intended efforts to accommodate culturally related explanatory models by focusing on one particular model (the spirit possession) to the detriment of others (the biological component of affective disorders and the importance of treatment adherence) may lead to less favourable outcomes, despite contributing to the building of a solid therapeutic relationship with patients and their families.
Mental health services have over the years tried to address cultural diversity in a number of ways. Historically, ethnic matching between patients and clinicians within mainstream services has been one of the most commonly proposed solutions to the problem cast as cultural misunderstanding of normative behaviours, misdiagnosis and poor treatment adherence. A second common strategy has been to resort to culture-specific services, mainly through voluntary sector provisions of ethnic-specific services. We argue that such approaches do not translate to any improvement in the cultural capability of the general workforce.
More recently, mandatory training events in cultural competence have populated the timetables of the NHS workforce (Reference DinosDinos 2015). The widespread cultural adaptation of existing evidence-based interventions, however, is still to be achieved. Explanatory models can and should be an integral part of both cultural adaptations and cultural competence: not only can they provide health professionals and researchers with culture- and context-specific information, to the benefit of diagnostic accuracy, but more importantly they provide them with more fine-grained information about subcultural beliefs and values, for the purposes of both research and clinical outcomes assessment. For some groups or individuals belonging to ethnic minorities, their primary identity may be related to the mainstream culture in which they reside, whereas their racial identity may be secondary or irrelevant (Reference DinosDinos 2015). An unintended consequence of both cultural adaptation and cultural competence can be the application of assumed stereotypical identities to all patients from a particular ethnic group, creating further alienation between health professionals and patients in already high-risk populations.
Conclusions
Explanatory models need to become an integral part of the DSM assessment framework in order to avoid a classification system that is either too Western-centric or that uses a Western-centric ideology to classify culture-bound syndromes. Explanatory models are not static constructs. Rather, they are fluid and they can be influenced by a number of factors, including the type of clinician/interviewer and the questions asked, the symptoms of the illness, and the patient's outlook/mood and migration history. Such factors may change during the course of an illness, and as a consequence explanatory models can also be subject to change. Therefore, explanatory models need to be revisited throughout the course of the illness, so that therapeutic management and therapeutic relationships can be reconceptualised and realigned.
A culturally sensitive clinical approach based on the exploration of explanatory models during assessment and treatment is an effective way of dealing with the complexity of patients’ and families’ needs by putting culture and narratives at the forefront of care. Not only can this help to identify more effective treatment plans for patients, it also works at all levels within an organisation. This requires clinicians to ensure that their assessments include investigation of explanatory models, and that they are open to considering their own culturally held beliefs and the influence of these on their preferred paradigms of assessment and treatment.
MCQs
Select the single best option for each question stem
-
1 Explanatory models can be defined as:
-
a culturally determined beliefs that individuals hold about themselves
-
b culturally determined beliefs that health professionals hold about their patients
-
c culturally determined beliefs that health professionals hold about themselves
-
d culturally determined beliefs that individuals hold to explain other people's behaviours
-
e culturally determined beliefs that individuals hold about illness and health.
-
-
2 The Cultural Formulation Interview involves a number of questions that clinicians might use to elicit information about:
-
a cultural aspects of a patient's lifestyle
-
b a patient's predominant cultural identity
-
c cultural aspects of the clinical presentation
-
d a patient's understanding of how culture influences one's illness presentation
-
e a patient's preference for a culturally matched health professional.
-
-
3 In relation to White British, research has shown that ethnic minorities are significantly more likely to be diagnosed with:
-
a psychotic disorders
-
b eating disorders
-
c personality disorders
-
d suicidal ideation
-
e anxiety disorders.
-
-
4 DSM-IV and DSM-5 acknowledge the role of culture in mental health through the inclusion of:
-
a culture-bound illness representations
-
b culture-bound syndromes
-
c culture-bound health beliefs
-
d culture-bound disorders
-
e culture-bound illnesses.
-
-
5 Research suggests that the majority of patients presenting with unexplained somatic symptoms have:
-
a post-traumatic stress disorder
-
b a personality disorder
-
c common mental disorders
-
d a physical illness
-
e a family history of mental health problems.
-
MCQ answers

| 1 | e | 2 | c | 3 | a | 4 | b | 5 | c |



eLetters
No eLetters have been published for this article.