Since concern has been expressed that psychopharmacology is being neglected within psychiatric training (Reference Harrison, Baldwin and BarnesHarrison 2011), we present a framework which could deepen knowledge and inform clinical practice for trainees and established clinicians. Modern psychopharmacology is based on the assumption that psychiatric drugs work by modifying some underlying physiological mechanism that is thought to give rise to the symptoms of a particular disorder. The hypothesised mechanism may not be specified, but since the drug is thought to counteract an underlying abnormality, this ‘disease-centred’ model of drug action suggests that drugs help restore the body to a more normal or healthy state. It applies equally to ideas that drugs target the underlying basis of specific symptoms as well as collections of symptoms (disorders). An alternative way of understanding how drugs might affect the feelings and behaviours we call mental disorders is what we call the ‘drug-centred’ model (Reference Moncrieff and CohenMoncrieff 2005). This suggests that psychiatric drugs are psychoactive substances that modify symptoms through the characteristic alterations they produce in normal mental processes, emotion and behaviour. No disease theory is required so this is a non-diagnostic approach.
The disease-centred model is rarely set out explicitly, but its presence is manifested indirectly in systems that classify drugs according to the principle disorder they are thought to treat, and in much research and clinical practice where other possible mechanisms of action, such as the impact of psychoactive effects, are largely ignored. A rare discussion of the theory of drug action by two leading psychopharmacologists explained that psychiatric drugs ‘counter or compensate for the abnormal pathophysiology’ (Reference Hyman and NestlerHyman 1997). However, ideas that appear to explain psychiatric drug action in this way, such as the dopamine hypothesis of schizophrenia or psychosis and the monoamine theory of depression, remain at the level of hypotheses, with evidence of abnormalities not related to drug intake remaining weak and inconsistent (Reference Moncrieff and CohenMoncrieff 2005).
Whether there is evidence that could support a disease-centred model of drug action for any class of psychiatric drugs is an area that requires further debate, but the taken-for-granted nature of the disease-centred model means that little research has been conducted that has a direct bearing on theories of drug action (Reference Moncrieff and CohenMoncrieff 2005, Reference Moncrieff2008). However, the fact that psychiatric drugs undeniably have psychoactive effects that have an impact on symptoms and have not been accounted for in the randomised trials conducted to establish efficacy suggests that effects of drug treatment may be at least partially explained by a drug-centred model.
Drug-centred practice
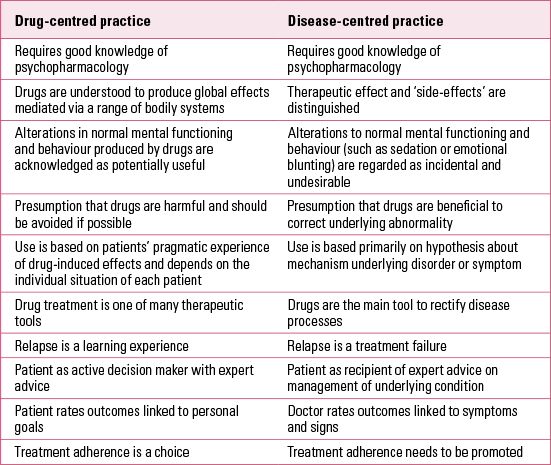
Table 1 shows some of the contrasting clinical implications that follow from the two models. According to the disease-centred model, prescribing should be driven primarily by diagnosis and theories about aetiology. A drug-centred approach, in contrast, focuses on making judgements about when drug-induced mental and behavioural modifications might be useful, bearing in mind the particular circumstances of each individual. In place of making a formal diagnosis, clarification of the patient’s particular and most pressing problems is required in order to evaluate whether known psychoactive effects of available drugs are likely to be useful. A drug-centred approach also highlights the harm that drugs can do, since it does not have the presumption of benefit inherent in the idea that drugs rectify an underlying abnormality. Under the drug-centred model, the desired effects of a drug are one of the consequences of the overall altered state the drug produces, and therefore they are not conceptually distinct from adverse or undesired effects.
TABLE 1 Comparison of drug-centred and disease-centred practice
Off-label prescribing
Many psychiatrists will have used the drug-centred model without explicitly acknowledging it as such, particularly in unlicensed or ‘off-label’ prescribing, where drugs are often used for their emotion- and behaviour-modifying effects. The UK’s Royal College of Psychiatrists’ guidance on using licensed medicines for unlicensed applications provides a pragmatic framework for drug-centred therapy, including advice to:
‘Familiarise yourself with the evidence about the proposed drug, including any possible drug interactions and potential adverse effects. […]
Consider the risks and benefits of the proposed treatment. Particular consideration is needed with children, older patients, and in those with impaired insight and judgement. […].
Give the patient (or his/her relative, when relevant) a full explanation […].
If agreement from the patient (or his/her relative, when needed) is obtained, document this approval. If a patient is unable to consent to a necessary treatment, note that it has not been possible to obtain consent.
Begin a cautious trial of treatment with the medicine. In out-patients, consider sending the patient a copy of any letter sent to his/her general practitioner, summarising why this approach has been adopted.
Monitor the patient closely. Continue with full documentation of [treatment] effectiveness and tolerance.
If the treatment proves unsuccessful, withdraw it, gradually if needed.’
(Royal College of Psychiatrists 2007: p. 7).
Prevalence and practice of off-label prescribing
Off-label prescribing was reviewed in this journal by Baldwin & Kosky in 2007. The four main forms of off-label prescribing they reported were: the lack of a licensed indication; drugs given outside the age range specified in the summary of product characteristics; doses that exceed the recommended maximum; and prescribing medication for longer periods than the marketing authorisation allows. They found that in general adult psychiatry unlicensed use of drugs was common. Around the world, off-label prescribing of antipsychotics in secondary care accounted for 40–66% of all antipsychotic prescriptions. Doctors also reported substantial amounts of off-label prescribing of antidepressants, psychostimulants and mood stabilisers. Off-label prescribing was also common with elderly patients, children, adolescents and people with intellectual disability – groups in which problems of capacity are prevalent. In these situations the evidence from disease-centred studies in general adult populations may have been extended uncritically to support prescribing in other groups where drug trials are unavailable.
Off-label prescribing using drug-centred principles
The drug-centred framework offers another way for clinicians to consider the appropriateness of prescribing in under-researched areas, in a cautious manner that balances the benefits and harms of drug use. The impact of the psychoactive effects of particular drugs needs to be carefully considered, along with the possibility of tolerance and dependence-inducing effects, as well as recognised adverse effects. By highlighting the mind- and body-altering effects of psychoactive substances, the drug-centred model also urges caution with respect to different age groups and untested drug combinations. When a drug is unlicensed for a particular age group it should not be prescribed in that age group on the assumption that effectiveness and safety established in general adult populations will apply equally, for example, to children or elderly people. Nor should trials of single drugs be used to assume that polypharmacy is safe or more effective when those drugs are used in combination.
Psychoactive effects of psychiatric drugs
As well as randomised trial evidence that drug treatment is superior to other strategies, a drug-centred approach requires a clear understanding of the psychoactive effects different drugs produce in order for a full assessment of the pros and cons of treatment to take place. Table 2 summarises the limited data available from studies with healthy volunteers and patients. Many psychiatrists will recognise the cognitive and emotional suppression produced by antipsychotic drugs. Evidence suggests that these effects are linked to a reduction in psychotic symptoms and associated emotional distress and behavioural disturbance in people with psychotic disorders (Reference HealyHealy 1989; Reference Mizrahi, Bagby and ZipurskyMizrahi 2005; Reference Moncrieff, Cohen and MasonMoncrieff 2009). The psychoactive effects of antipsychotics would also predict that they might be useful in other situations involving over-arousal or abnormal preoccupations, such as mania (Reference Prien, Caffey and KlettPrien 1972) and obsessive–compulsive disorder, and for some people diagnosed with personality disorder, as they are sometimes used currently.
TABLE 2 Psychoactive effects of psychiatric drugs
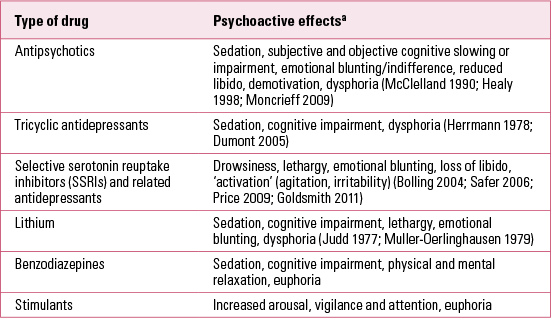
However, a drug-centred approach would also highlight the adverse functional consequences likely to be associated with the psychoactive effects of antipsychotics, in contrast to the current situation whereby patients’ complaints about them are still frequently minimised or dismissed (Reference Seale, Chaplin and LelliottSeale 2007; Reference Moncrieff, Cohen and MasonMoncrieff 2009). According to a drug-centred view, therefore, the possible benefits of maintenance treatment in reducing relapse in psychotic disorders may not outweigh the global adverse effects of the drugs. Indeed, a recent long-term follow-up of a randomised antipsychotic discontinuation study suggested that maintenance treatment may impair functioning and did not reduce relapse rates in the long term compared with a supported and flexible antipsychotic discontinuation programme (Reference Wunderink, Nieboer and WiersmaWunderink 2013).
Harm is magnified when drugs are taken over long periods, or in combination, as psychiatric drugs often are. Not only do the drugs themselves have toxic effects, but the body’s adaptations to the presence of a particular drug can counteract the desirable effects of that drug, produce physical dependence and withdrawal symptoms, and may produce irreversible physical dysfunction such as tardive dyskinesia.
The psychoactive effects of antidepressants are less familiar (Table 2). Taking a problem-based approach, drugs with sedative properties, including sedative antidepressants and benzodiazepines, might be useful for people who suffer from insomnia, anxiety or agitation, again reflecting current prescribing patterns, especially the off-label use of low-dose tricyclic antidepressants in general practice. Equally, however, these effects might be counterproductive in someone who is lethargic and socially withdrawn. The consequences of the emotional blunting that is reportedly associated with some antidepressants need further exploration. In theory, people suffering from overwhelming emotions may appreciate this effect, but some people experience it as unpleasant, and it has also been tentatively linked with suicidal impulses (Reference Price, Cole and GoodwinPrice 2009; Reference Goldsmith and MoncrieffGoldsmith 2011).
A collaborative approach
Although collaborative discussion and decision-making are desirable under any model of drug action, taking a drug-centred approach changes the relationship between patients and prescribers. If drugs act through altering normal mental functions, it is the individual’s experience of the whole range of drug-induced effects that should guide prescribing, rather than the doctor’s suppositions about the nature of the underlying disorder. For example, someone who has problems with mood or anxiety would be helped to evaluate how the altered state of mind produced by a particular drug affected all areas of functioning. Consistent with a recovery-based approach, the outcomes of achieving patient-identified goals, rather than just a reduction of symptoms, are the aims of treatment. The drug-centred model therefore advocates a collaborative form of self-medication, in which psychiatrists act as reservoirs of information on drugs’ psychoactive and physical effects, help to explore the likely overall impact and limitations of drug treatment and consider alternative, non-drug-based approaches.
Careful monitoring of patients’ experiences and reported outcomes of drug treatment should be a routine part of any prescribing practice. The drug-centred model highlights the importance of identifying the consequences of drug-induced alterations to normal mental and physical functioning. These alterations, which are often subtle, may not be detected through scant questioning about common side-effects. Detecting the long-term consequences of drug treatment is particularly important as the immediate psychoactive and physical effects of drugs change, underlying problems evolve and unpredictable outcomes may appear.
When pharmacotherapy might not be the answer
Doctors have a long history of using treatments that do not work (Reference Doust and Del MarDoust 2004). Reasons include patient expectations, a need to do something and an over-reliance on a pathophysiological model that is later shown to be incorrect. Historical examples include insulin for schizophrenia and leeches for almost everything.
The relational aspects of prescribing are very powerful and may outweigh the pharmacological effects of medications in some situations. Reference Martean and EvansMartean & Evans (2014) illustrated these issues in their examination of prescribing for personality disorder. Consultant psychiatrists can feel helpless in the face of ongoing suffering and find denying medication stressful. They feel an expectation to prescribe, and some patients view a prescription as an acknowledgement of their suffering and non-prescription as a denial of it. The disease-centred model reinforces these expectations, by endorsing the idea that drugs rectify underlying physiological abnormalities. Patients may therefore become trapped in a cycle of ever-increasing medication, in which one drug after another is tried or added. This effect can be further magnified by the currently fractured nature of mental health services that expose patients to multiple prescribers. The drug-centred model, in contrast, offers a way of exploring the potential benefits of drug therapy, without raising expectations that it is an essential part of the solution.
Ideally, a drug-centred framework would foster greater scepticism about medication and require stronger proof of the utility of drug treatment in individual cases. It could also support psychiatrists attempting to rationalise and reduce medications. A drug-centred model also provides a framework for stopping therapy when it is ineffective or harmful and for helping patients explore other ways of managing symptoms or of fulfilling the function that medication seeks to address.
A drug-centred approach could be useful when patients lack capacity or refuse to consent to treatment, by focusing attention on the purpose and desired outcome of treatment. Moreover, a degree of collaboration is often possible even in these circumstances (Reference Baker, Fee and BovingtonBaker 2013). By highlighting that drug treatment involves behavioural and mental modification, however, the drug-centred approach underlines the need for meaningful scrutiny of non-consensual administration of drug treatment.
A caveat
There is a danger that misinformed use of the drug-centred model could increase inappropriate prescribing, particularly in off-label scenarios. An uncritical assumption that most medication is restorative and safe, which is fostered by the dominance of the disease-centred model, coupled with a desire to do something, means that doctors and patients may wish to use medication for its psychoactive properties without paying sufficient attention to potential harmful effects, or to whether the medication helps patients achieve their specific goals. This may lead, for example, to long-term prescribing of antipsychotics for insomnia or the long-term use of benzodiazepines or other tranquillisers to relieve social stress. It is important therefore that the drug-centred model is employed to highlight the full effect that drug treatment can produce, and that drug use is properly evaluated against each individual patient’s objectives.
Case vignettes
In this section we give two case vignettes illustrating drug-centred psycho pharmacology in practice. The vignettes are composites, drawing on clinical experience with several different people.
Case vignette 1
Introduction
Ayesha is a 28-year-old single woman working as a manager in a medium-sized telecommunications business. She was encouraged by her sister to go to an accident and emergency (A&E) department because she had behaved oddly for a few days. She presented the following features on mental state examination.
Mental state examination
She was casually dressed but heavily made up with bright lipstick and thick eyeliner. She was irritable and intolerant of being interviewed. Her assessor reported that she had loud, pressured speech, spoke rapidly and tended to wander off the point of questions. Her mood appeared slightly elevated although she also cried several times. Ayesha felt her mood to be very unstable. She thought that a private security firm was monitoring her phone calls and that her boss was collaborating with an investigation. She said that she had seen people ‘tailing her’ in the past few days. She also reported that her TV reception had been interrupted by the security firm sending an unscheduled programme to her TV instead of the news. She was aware that her sister viewed these concerns as a sign of mental illness, and thought that her sister might be involved in the covert monitoring. No significant risks of harm to self or others were identified.
History
Ayesha had no history of mental health problems. She had had a good childhood and a good education. She did not take any drugs or drink alcohol. Her physical health was good. She had worked throughout her adult life, but recent changes of personnel at work had caused her problems. She had experienced bullying by her manager for around 12 months and had received a formal warning. Two of her peers had left the company because of bullying in the past 6 months, leaving her feeling exposed and unsupported. She had lost weight and was unable to sleep, reporting several completely sleepless nights. She was worrying about work and had no one to talk to. She was building a case for constructive dismissal.
Formulation and treatment
The doctor who assessed Ayesha in A&E formulated her presentation as mania triggered by stress; Ayesha herself had wondered whether she was experiencing bipolar disorder, having read up on her symptoms. The home-based treatment team identified a high degree of anxiety and offered Ayesha treatment with diazepam 10 mg at night. This helped her sleep for the first time in days and reduced her anxiety levels, but left her too sedated during the day. The following night the dose was reduced to 5 mg. This was acceptable to Ayesha, who responded positively to medication and contact with the treatment team. Within 2 days she felt a good deal better. She was less concerned about being investigated and felt protected by her contact with healthcare services. Her mood became more reactive and cheerful. She lost the irritable edge and no longer cried. Her speech remained fast and expressive and her sister confirmed that this was normal for Ayesha. A few days later Ayesha said that the private security thing was not real and was a product of long-standing work stress. She was able to talk through an approach to address her work problems and make a satisfactory plan. She found the diazepam helpful for 2 weeks and then followed advice to reduce and stop it. She was offered further follow-up from the community mental health team.
Drug-centred therapy
Ayesha had no desire to take on the diagnoses considered at presentation because she felt they were stigmatising. Clear diagnostic criteria had not been met. She received effective treatment without a diagnosis of a mental disorder. She was treated with diazepam because it was likely to reduce her anxiety rapidly and also help her sleep. Diazepam formed part of a care package that included daily home visits, problem-solving, relaxation therapy and regular review of outcomes. The rapid response and resolution of symptoms suggested that the treatment package was effective. The risk of dependency on diazepam was explained several times at the outset of treatment and a goal of no more than 2 weeks on the drug was set with Ayesha’s agreement. Ayesha experienced over-sedation and the response was to immediately reduce the dose of diazepam. Medication was discontinued successfully as planned. Ayesha remained well at 3-month follow-up and was discharged.
Case vignette 2
Introduction
Robert is 47 and at first contact with mental health services he was staying with his son to give his wife a break as his carer. He had not worked for nearly a year and could not imagine how he could get back to his job at the post office. His difficulties are longstanding but had become much more distressing in the past year. He is plagued by voices. He has heard them since he was a child.
History
Robert’s mother left the family home when he was 4 years old and he was raised by his father. He had normal development and schooling, but experienced a period of physical, emotional and sexual abuse from a babysitter. Since the age of 13 he has experienced clear hallucinatory voices, perceived in external space, that comment on his actions and order him to do things. He has always resisted the voices, despite frequently being ordered to stab himself or his family members.
His wife became very worried about this when he finally disclosed the voices after many years of marriage. The family agreed that he would move out and stay with his adult son to reassure his wife, who stayed at home. He found this decision very upsetting. He agreed to speak with his general practitioner (GP), who started him on antidepressants and referred him for a psychiatric assessment.
Mental state examination
In the clinic, mental state examination confirmed that Robert experienced second- and third-person auditory hallucinations, including frequent command hallucinations. He also had significant anxiety and depressive symptoms. Risk assessment involving family informants found no evidence of historical harm to self or others. However, Robert was worried that he might do something awful and was very distressed.
Goals, treatment and outcomes
Robert and his psychiatrist agreed to ‘co-produce’ a set of personal goals. Robert wanted to be able to lead a normal life at home with his family. He wanted to abolish, or at least live more comfortably with, the voices that he heard. Together they used the Health of the Nation Outcome Scales (HoNOS; Reference Wing, Curtis and BeevorWing 1996) component of the Mental Health Clustering Tool (Department of Health 2013) as a device to discuss his goal priorities and as a prospective outcome measure. This reflects an approach described by Malcolm Stewart (Stewart n.d.). The HoNOS has 13 scales that cover a broad range of experience, behaviour and functions in relation to mental health. A score can be allocated to each scale. The scales with the highest scores were considered as a starting point to set priorities for treatment.
Robert reported that his priority was to rid himself of the voices. He was rated at the maximum of 4 (i.e. severe to very severe problem) on HoNOS item 6 ‘Hallucinations and delusions’. The other HoNOS areas he wanted to give secondary priority also scored 4: ‘Relationship problems’ and ‘Cognitive problems’. He wanted to re-establish his settled family life and be able to think more clearly, with less distraction.
He talked about what he could do with his psychiatrist in the out-patient clinic. Conversation drew on the psychiatrist’s experience with other patients in order to illustrate the pros and cons of various therapy options. Consideration was given to adapting the social changes that Robert had already arranged with his family, having time away in day care or hospital, and adding medication and psychological therapy. Further support from an additional member of the community mental health team was offered and information given about a range of statutory and non-statutory services. Robert’s wife was present at these discussions.
Robert considered the advice and information, then at the second appointment he asked for antipsychotic medication to be started straight away, since he felt that this would have the best chance of stopping the voices. He declined further support beyond clinic appointments. He learnt about antipsychotic medication from his psychiatrist and explored its potential harms and as well as its potential benefits. This conversation pulled no punches. When Robert chose to take olanzapine, he did so believing that it could be effective at reducing the voices and also knowing that it was likely to cause him to put on weight and cause some sedation or mental ‘fuzziness’. Robert thought some fuzziness might be helpful. He knew about the risks of metabolic problems, including elevated cholesterol and diabetes. He also understood the value of baseline monitoring and agreed to be weighed in the clinic, and to have blood tests which were arranged as soon as possible afterwards, with the agreement of his primary care team.
After a week he met his psychiatrist again and there was not much improvement in the voices, although he had been sleeping better. He continued to stay with his son. His wife was pleased that something was being done. This was the same for the next week, but 3 weeks after starting treatment he reported a reduction in the voices and was less distressed by them. After further discussion Robert agreed to continue antipsychotic treatment for the next 2 months. He said that he had already stopped the antidepressant started by his GP without ill effects. At the next review he was content to continue with the olanzapine since his distress had diminished and his wife had agreed to him returning home. He did not put on significant weight and reported that he was being very careful to eat a sensible diet. Follow-up blood tests showed normal cholesterol, glucose, full blood count and liver function. He agreed to continue medication beyond 2 months.
At 4 months he was settling into a recovery of his usual functions. His family saw a distinct improvement in his mood and activities. He was very pleased that he was back home and that his wife trusted him to be there. He still heard vague voices but felt no pressure to harm himself or others. He had started visiting friends and was able to go out to the shops. He was considering a return to work and agreed to a referral to the local job retention service. The HoNOS scores were all reduced (i.e. improved) and no individual score was now above 2 (i.e. mild problem). He still experienced hallucinations but he found them less intense, less frequent and less distressing. He did not need to make a big effort to stay in control and concentrate and, as a result, felt more relaxed. He had thus achieved the outcomes agreed in advance.
Drug-centred therapy
At no point did Robert and his psychiatrist agree a diagnosis. He had talked about diagnosis with the psychiatrist and he had said he was not interested in having one. The psychiatrist could have made a diagnosis but did not feel that this was a necessary precursor to treatment. Treatment therefore followed a drug-centred approach. Beginning with an understanding of Robert’s needs and wishes, the psychiatrist used his knowledge of the pharmacological properties of medication and his experience of treating other patients to match the properties of olanzapine to those needs and goals. Care was taken to monitor for adverse outcomes as well as positive ones. Undoubtedly, other factors came into play as well as the medication. The engagement between the psychiatrist and Robert and his wife was probably quite important, as well as the family’s willingness to respond positively to Robert’s recovery. Robert achieved his personal goals and this achievement was reflected on the HoNOS outcome tool. He also began working with the job retention service. Treatment was continued for another 4 months without incident and then Robert was discharged (still using medication) with a primary care monitoring plan that included annual physical health monitoring and a versatile crisis plan. Robert was advised that long-term treatment might not be necessary and was informed further about long-term risks of medication. He was asked to think about seeking a re-referral to the clinic to support olanzapine discontinuation if he wanted to stop treatment in future.
Research and training
The dominance of the disease-centred model has resulted in much effort being devoted to identifying putative therapeutic targets. This had led to extensive theorising about pharmacodynamics and to narrowly focused pharmacological studies that tend to overshadow the gaps in our knowledge about the effects of psychiatric medications on the people taking them and on the whole range of neurotransmitters and physiological systems. Further research is needed from a combination of laboratory-based, animal and volunteer studies and research on objective and subjective effects in patients, to establish the full range of physical, behavioural, emotional and cognitive effects that drugs induce. We need to better understand their effects on different bodily systems and how these interrelate; how drug-induced effects change with continued use and how they are likely to interact with the various symptoms and manifestations of mental disorders. Prescribers could use this knowledge to improve their practice, taking into account evidence of the real-world experiences of psychiatric drug users, as well as data on short- and long-term systemic effects of different drugs.
Undergraduate and postgraduate training needs to equip doctors with this knowledge, and provide guidance on how they might use it to support patient autonomy following the principles advocated in government policy (National Institute for Mental Health England National Workforce Programme 2008; National Institute for Health and Care Excellence 2009). Doctors may need training to communicate uncertainties and risks, to use co-production to set goals and support personal choice, and to routinely monitor outcomes, whether good or bad. In line with the College’s guidance on using medicines for unlicensed applications (Royal College of Psychiatrists 2007), further training to help patients to withdraw from unhelpful psychotropic medication is also important, given the recognised discontinuation effects associated with all classes of drugs used in psychiatry.
Conclusions
The drug-centred model, which suggests that psychiatric drugs should be understood as producing altered states that may sometimes be useful in suppressing certain mental symptoms or unwanted behaviours, stresses that drugs should be understood more fully and used more cautiously. Use of drugs according to this model frees psychiatric practice from reliance on diagnosis, but emphasises the importance of a thorough and comprehensive knowledge of psychopharmacology. It provides an alternative framework to help personalise drug treatment, maximising benefits and reducing risks. Wherever possible, the prescription of a drug should be a collaborative decision, based on the range of effects the drug can induce and its likely impact in each individual’s unique situation. We think many psychiatrists will recognise that they already use elements of a drug-centred approach and hope this article provides an explicit basis for further discussion and exploration of this enduring practice.
MCQs
Select the single best option for each question stem
-
1 Psychiatrists:
-
a only prescribe within a drug’s product licence
-
b always stick to national guidelines when prescribing
-
c might use a drug-centred model when using off-label prescribing
-
d should clearly delineate therapeutic effects from side-effects
-
e must always make a diagnosis.
-
-
2 Collaborative decision-making between a psychiatrist and a patient:
-
a can occur only in a drug-centred approach
-
b supports the creation of patient-identified goals
-
c is impossible with people detained under the Mental Health Act
-
d cannot be monitored using outcome scales
-
e may suffer from an awareness of the relational aspects of prescribing.
-
-
3 The disease-centred model in psychiatry:
-
a affects the nature of research carried out on drug treatments
-
b is well established for depression
-
c is well established for psychosis
-
d focuses on the psychoactive effects of drugs
-
e is proven by randomised controlled trials.
-
-
4 Drug-centred psychopharmacology:
-
a has no scientific basis
-
b does not require a grounding in pharmacology
-
c requires treatment adherence
-
d assumes that drugs are beneficial because they correct an underlying abnormality
-
e sees drug treatment as one of many therapeutic tools.
-
-
5 Drug-centred practice:
-
a encourages a good knowledge of the psychoactive effects of drugs
-
b is grounded in aetiological theory
-
c encourages high-dose polypharmacy when used cautiously
-
d views relapse as treatment failure
-
e is always explicitly acknowledged when used.
-
MCQ answers
| 1 | c | 2 | b | 3 | a | 4 | e | 5 | a |





eLetters
No eLetters have been published for this article.