Introduction
Seniors’ care for those unable to manage on their own generally comprises facilities offering residential care, such as long-term care (LTC) homes and retirement homes, and home or community care, where seniors receive services in their homes or within their local community. In addition, numerous supportive housing programs are available to seniors in designated residential buildings for those who require daily personal support and essential homemaking to live independently. In Ontario, all seniors’ care options are expected to face severe capacity challenges in coming years, with the result that many seniors may go without the services they need or default to hospitals that have neither the budgets nor the programs to serve them. By one estimate, the population of Ontario’s seniors over age 85 is expected to quadruple in the 20-year period from 2011 to 2031 (Ontario Association of Non-Profit Homes and Services for Seniors, 2016).
In the case of LTC homes, the supply of beds is failing to keep up with demand, resulting in longer waitlists in many parts of Canada. The province of Ontario provides a clear example. Faced with excess demand, government-subsidized LTC homes have a waitlist that is fully one-third the number of residents living in these homes, all of whom have been assessed as eligible for admission. At the same time, the unmet demand for beds in long-term care must be absorbed by other residential alternatives, among them retirement homes, which do not receive provincial subsidies for care.
This study compared the care service offerings of Ontario’s LTC homes and retirement homes regarding the similarity in service offerings. LTC homes and retirement homes are two of the main congregate residential care settings for seniors in Ontario who may be unable to manage on their own. Both settings (a) cater primarily to seniors, (b) are residential/institutional in nature, (c) involve the provision of care, and (d) are regulated by the Ontario government specifically with regard to the care provided.
To the extent there is overlap in services between the two sectors, issues arise with respect to equity of access to seniors’ care, since the government funding regimes applicable to each sector differ profoundly. This raises concerns of a two-tier system, where some residents are subsidized and some are not. There is a dearth of research examining the care services offered by retirement homes or comparing service offerings supplied by the two sectors.
Background
In Canada, health care primarily falls under provincial and territorial jurisdiction. Individual jurisdictions thus have considerable discretion over policy in this area. In Ontario, provincial regulation affects all care services provided in seniors’ residential care. These include nursing and personal support services, which range from medical care to assistance with more routine activities of daily living (ADLs) such as dressing, bathing, and ambulation. LTC homes and retirement homes are also required to perform assessments and devise care plans for all residents. In addition to care, matters related to accommodation are regulated and, for LTC homes, the amounts that may be charged.
Ontario’s regulatory framework for residential care facilities includes a number of dimensions. LTC homes which provide nursing care must be licensed to operate, as must all retirement homes that provide two or more care services, including meals or ADLs. In the case of LTC homes, the issue of new licenses may be restricted by number or geography by Ontario’s Ministry of Health and Long-Term Care (MOHLTC). Another dimension involves control over which residents may be admitted and, in the case of LTC homes, whether homes are required to admit them. Regulators may also manage which services may or must be offered, who can (or cannot) provide them and, for LTC homes, how much providers are allowed to charge. A further dimension involves what the government agrees to fund, which differs markedly between LTC homes and retirement homes.
Health care in Canada uses what the Organisation for Economic Co-operation and Development (OECD) calls a public contract model whereby the government pays for certain “insured” services, which are largely privately delivered (Docteur & Oxley, Reference Docteur and Oxley2003). Although health care is under provincial and territorial jurisdiction, for many decades the federal government has provided some funding to the provinces and territories to help support their health care expenditures. The current model sends these funds into provincial general revenues (currently in the form of the Canada Health Transfer), rather than earmarking them for particular expenditures. However, the Canada Health Act (1985) places some terms and conditions which the provincial and territorial insurance plans must meet in order to obtain full federal funding. In particular, the Canada Health Act requires that all provincial and territorial health plans fully insure all Canadian residents (“insured persons”) for all “insured services”, but defines these as “medically necessary” services provided within hospitals or by physicians. Provincial and territorial plans can, but do not have to, insure services that do not meet this narrow definition of medical necessity. The Canada Health Act specifically places nursing home and adult residential care services within the definition of “extended health care services”, which are not required to be insured.Footnote 1 As noted below, Ontario has chosen to pay for some of the care services provided in non-hospital settings, including LTC homes and retirement homes, but these vary with the type of facility.
LTC homes and retirement homes are regulated through separate pieces of legislation in Ontario. LTC homes fall within the purview of the Long-Term Care Homes Act (2007) and Ontario Regulation 79/10 (O. Reg. 79/10, 2010). Ontario brought its first retirement homes legislation into force with the Retirement Homes Act (2010), established the Retirement Homes Regulatory Authority (RHRA) in 2011, and began licensing retirement homes in 2012. The primary regulations under the Retirement Homes Act, which provide the detail under the legislative framework, are Ontario Regulations 166/11 and 53/12 (O. Reg. 166/11, 2011; O. Reg. 53/12, 2012).
When the Long-Term Care Homes Act came into force in 2007, it consolidated and replaced three statutes that governed long-term care homes in Ontario: the Charitable Homes Act, the Homes for the Aged and Rest Homes Act, and the Nursing Homes Act. By contrast, retirement homes in Ontario were not regulated as an entity prior to 2010, although the rights and obligations of their residents and operators were the subject of legislative oversight in numerous areas. Homes were governed by the Residential Tenancies Act (2006) and at least a dozen other Ontario statutes applied – and still apply – to the residents, employers, and buildings involved.
Numerous factors led to the enactment of the Retirement Homes Act. These included long-simmering issues such as the increase in the seniors’ population and the growth in care services within retirement homes. However, events that fast-tracked the matter to the policy agenda included media coverage of alleged abuse, neglect, and substandard health care quality. Several interests expressed views on the appropriate governance regime for retirement homes (Advocacy Centre for the Elderly, 2007; Ontario Nurses’ Association, 2010; Registered Nurses Association of Ontario, 2011). In addition, heated debates regarding content and oversight ensued in the provincial legislature (Hansard Ontario 140, 2010) before the Retirement Homes Act was finalized.
Methods
The study involved gathering descriptive data for both LTC homes and retirement homes in Ontario regarding (a) the regulatory framework, including purpose, funding, governance, care services, residents’ rights and remedies, safety, and security; (b) numbers and locations of homes and residents, including geographic dispersion; (c) prevalence of care services and amenities; (d) costs of accommodation and care; and (e) occupancy rates, vacancy rates, and waiting lists. We collected much of the data in July and August of 2016. We obtained data for the 728 retirement homes and 641 LTC homes that were licensed at that time; we drew data from public and private databases, reports, statutes, and regulations.
Analysis involved descriptive summaries of the data in accordance with the categories listed above, as well as assessment of the similarities and differences between LTC homes and retirement homes by category. The data were collected and analysed principally by the lead author (BR) with analysis review by the co-authors.
With regard to the statutory and regulatory framework (purposes, funding, governance, residents’ rights and remedies, safety and security, care services, staffing), the principal statutes we examined were the Long-Term Care Homes Act (2007) and the Retirement Homes Act (2010) as well as accompanying regulations listed in Table 1. All statutes and regulations are available publicly.
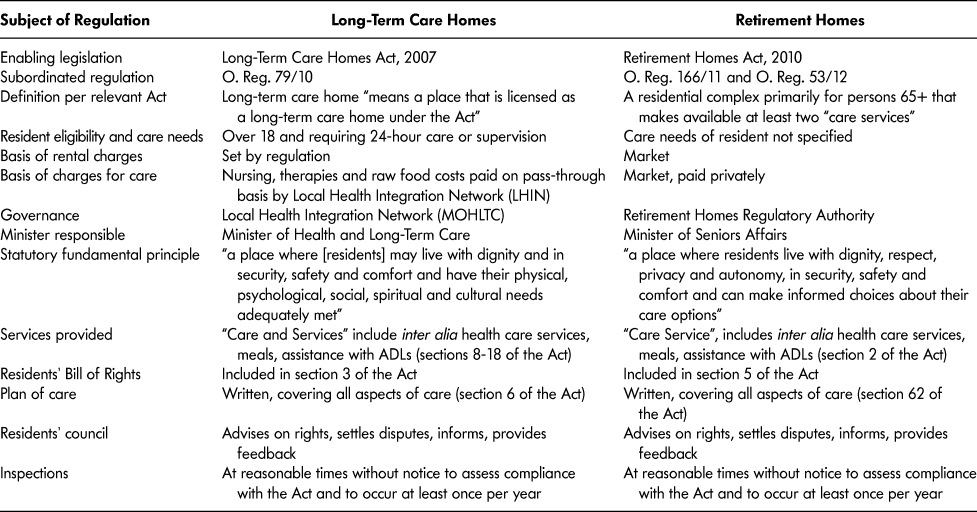
Table 1: Statutory and regulatory comparison of retirement homes and long-term care homes
For the numbers and locations of homes, beds, and residents, our principal source for LTC homes was Ontario’s Ministry of Health and Long-Term Care’s reports on long-term care homes (Ministry of Health and Long-Term Care, n.d.). For retirement homes, our data came primarily from the public register of the Retirement Homes Regulatory Authority (RHRA) (Retirement Homes Regulatory Authority, n.d.).
Data regarding the prevalence of care services and amenities for retirement homes were sourced from the RHRA public register; from the 2016 Seniors’ Housing Report for Ontario by the Canada Mortgage and Housing Corporation (CHMC) (Canada Mortgage and Housing Corporation, 2016) and from the Collaborative Retirement Econometrics (CORE) database (https://www.corecanada.com/), which contains property, operational, and financial information regarding Canadian retirement homes. The CMHC report is done annually for the purpose of informing industry stakeholders and the general public of trends in the market across Canada. The CORE database was developed cooperatively between (a) Ontario Retirement Communities Association (ORCA), a not-for-profit association representing members of the retirement home industry in Ontario, and (b) ProMatura Group, LLC, a global market research firm focused on the age-qualified housing industry.
Financial data regarding costs of accommodation and care for LTC homes were provided by MOHLTC bulletins and level-of-care per diem funding summaries (Ministry of Health and Long-Term Care, 2016a). For retirement homes, relevant data were available from the CMHC (2016) and from the CORE database.
For data regarding occupancy rates, vacancy rates, and waiting lists, we obtained LTC home data primarily from the MOHLTC’s Long-Term Care Home System Reports for October 31, 2015 (Ministry of Health and Long-Term Care, 2015a), with comparisons to October 31, 2010 (Ministry of Health and Long-Term Care, 2010) and from the MOHLTC’s LTC Home Occupancy Targets Policy (Ministry of Health and Long-Term Care, 2014). For retirement homes, data were available principally from the CORE database and from the CMHC (2016).
Statistics regarding LTC homes were from MOHLTC reports. With respect to retirement homes, the RHRA data best define the population of homes that are of interest in this study, as these data include all licensed retirement homes that provide two or more care services, in accordance with the legal definition used in this study. The CMHC report and the CORE database use slightly different definitions of retirement homes than are used by the RHRA. As such, these data are considered to be descriptive of the retirement home sector and relevant to this inquiry, although less definitive of the relevant population of retirement homes. We found no significant conflicts in the information obtained from these various sources for retirement homes.
The study data presented in this article pertain to services offered by residential care homes, rather than the health characteristics of the residents themselves. In addition, although the study described the features, costs, and availability of care services, it did not evaluate the quality of the services provided. Limitations of the research undertaken are described more fully in the Limitations section.
Findings
Statutory and Regulatory Framework
Table 1 highlights certain statutory and regulatory provisions concerning LTC homes and retirement homes. Under the public contract model, residential care delivery in Ontario is private, but government can use regulatory and financial policy instruments to control many aspects of how homes operate.
Residents of an LTC home are subject to certain eligibility criteria, based primarily on assessed care needs. Applicants are required to demonstrate a need for 24-hour-a-day nursing care, supervision, or monitoringFootnote 2 in order to be admitted.
The Retirement Home Act defines “retirement home” as a residential complex that is occupied primarily by persons who are 65 years of age or older, where there are at least six occupants unrelated to the operator of the home, and where the operator makes at least two care services available to the residents.Footnote 3 Defined in this way, the Retirement Home Act does not stipulate eligibility criteria for retirement home residents based on care needs. Retirement homes can provide a spectrum of offerings, ranging from independent living to care services that are comparable to those in LTC homes. Although retirement homes are required to assess each resident and implement an individual plan of care, these assessments are not publicly available. As a result, the care needs required are best inferred from the services provided by each home, which are listed in the RHRA database.
The Long-Term Care Homes Act gives authority to the MOHLTC for matters related to care and accommodation in LTC homes and how these services are funded. Funding for LTC homes generally flows from the MOHLTC through the 14 Local Health Integration Networks (LHINs), each of which has a distinct geographic area within the province and is responsible for the planning, integrating, and funding of health care in their respective regions. For retirement homes, it is the RHRA, rather than the MOHLTC, whose objects are to administer the RHA and regulations, grant licenses, oversee compliance and enforcement, conduct inspections, and maintain a public register.
The Acts (Long-Term Care Homes Act and the Retirement Homes Act) and their underlying regulations address the licensing of homes as well as residents’ rights, care standards, safety and security, protections against abuse and neglect, powers of inspectors, and the establishment of offences, penalties, appeals, and enforcement. As is evident from Table 1, the retirement home regulatory regime drew heavily from the LTC home regime in requiring a residents’ bill of rights, assurances that residents may participate in their own plan of care, and a residents’ council for each home.
Numbers and Locations of Homes and Residents
There are approximately 640 LTC homes in Ontario with a total of more than 78,000 beds, and approximately 730 retirement homes with a total of more than 72,000 beds. Although the MOHLTC regulates the number and location of new LTC home licences, the RHRA has generally maintained a policy of licensing retirement home applicants that can demonstrate adherence to regulations. Table 2 shows the distribution of LTC home and retirement home beds according to the 14 LHIN regions throughout the province. When the numbers of LTC homes and retirement homes are compared with the population of Ontarians over the age of 75, it is clear that LTC homes are more evenly distributed in accordance with the seniors’ population than is the case with retirement homes. As the table shows, there are approximately 12.3 Ontarians over age 75 per LTC home bed in Ontario, with a range from 9.2 in the North East LHIN to 17.0 in Mississauga Halton. The corresponding ratio for retirement homes is similar on a province-wide basis at 13.4, but there is considerable variability among LHINs, ranging from 7.1 seniors over age 75 per retirement home bed in the Champlain LHIN to over 30 in the Central West and North West LHINs.
Table 2: Numbers and locations of homes and beds (LTC homes and retirement homes)
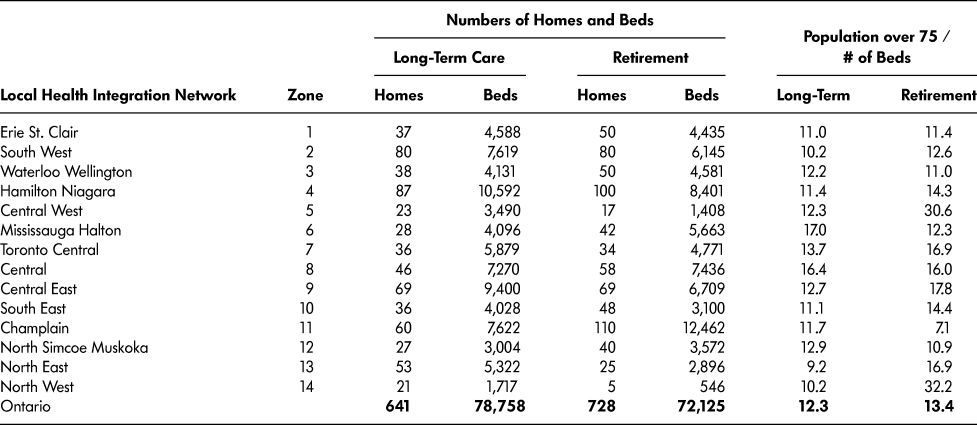
Note. LTC home data from MOHLTC’s reports on long-term care (MOHLTC, n.d.); retirement home data from RHRA public register (Retirement Homes Regulatory Authority, n.d.); population statistics from Statscan census data are as provided by the Ministry of Finance to the MOHLTC and referenced in the Health Data Branch’s Long-Term Care Homes Report (MOHLTC, 2015a)
The more even dispersion of LTC homes may be a function of government policy to have equal access across the province. The Long-Term Care Homes Act states that the Minister, in determining whether there should be an LTC home in an area, and how many beds there should be, is to consider the public interest, including (a) the existing LTC home bed capacity in the area or other areas, (b) the other facilities or services available, (c) the current and predictable continuing demand for LTC home beds in the area, and (d) the funds available for LTC homes in Ontario.Footnote 4
Based on a comparison of LTC home statistics for 2010 with 2015, the number of licensed LTC home beds in Ontario grew by only 1.5 per cent over the 5-year period, compared to an increase of 12 per cent in the population of people over age 75 (Ministry of Health and Long-Term Care, 2010; 2015a). By contrast, the number of retirement home licenses increased substantially from 565 in 2012–2013 to 716 in 2014–2015 and increased further to 728 as of July 2016 (Retirement Homes Regulatory Authority, n.d.).
Occupancy Rates, Vacancy Rates, and Waitlists
Occupancy rates tend to be significantly higher among LTC homes than retirement homes in Ontario with correspondingly long waitlists for LTC homes. The MOHLTC’s Long-Term Care Homes Financial Policy (Ministry of Health and Long-Term Care, 2014) includes certain occupancy targets for all LTC homes, which, in turn, affect their funding. Essentially, the Ministry requires all homes to maintain the occupancy rate of their long-stay beds at a minimum of 97 per cent in order to receive 100 per cent of the per-person-per-diem-funding, according to the funding envelopes. Per-person-per-diem funding reduces on a sliding scale as occupancy rates decline below 97 per cent. According to MOHLTC’s System Report, (Ministry of Health and Long-Term Care, 2015a), the average long-stay utilization exceeded 98 per cent in all LHINs as of October 2015. This utilization level was fairly consistent across all levels of accommodation in LTC homes, including basic, semi-private, and private accommodation. Because the demand for these LTC home beds exceeds supply, there are high occupancy rates in LTC homes.
The Ministry’s System Report also indicates that the long-stay waitlist in October 2015 totalled about 27,500 people, compared with approximately 77,000 existing beds. This equates to a waitlist of 36 per cent in excess of existing beds in the province, although the percentage ranged from 13 per cent in the Erie St. Clair LHIN to a high of 58 per cent in the Central LHIN. This waitlist excludes those who are already residing in an LTC home and waiting to transfer to a preferred location. The number of clients being placed in LTC homes in the month of October 2015 totalled approximately 1,400, or approximately one-twentieth of the people on the waitlist at the time.
The RHRA does not track occupancy rates in retirement homes, although data from CMHC and CORE are indicative of the supply versus demand balance. With some exceptions, the population of residences covered by CMHC is similar to that of the RHRA. In Ontario, the overall seniors’ housing vacancy rate as determined by CMHC was 10.7 per cent in 2016, which compared with rates over 15 per cent in 2010 and 2011, and was the lowest level recorded since the standardized survey for Ontario began in 2001. In 2016, vacancy rates in semi-private and ward accommodation were the highest at 18.2 per cent. CORE data indicate similar, although slightly higher, vacancy rates than the CMHC data.
Care Services
Both LTC home and retirement home statutory regimes prescribe standards for care services. In addition, both statutes designate the plan of care as the focal point for the provision of care, which begins with an assessment of the resident. Under the Long-Term Care Homes Act, a placement coordinator determines eligibility for admission based on the physical and mental health of the applicant based on functional capacity and requirements for personal care and behaviour,Footnote 5 and RAI MDS 2.0 acts as the standardized assessment tool, according to MOHLTC’s Guide to the Long-Term Care Homes Act (Ministry of Health and Long-Term Care, 2011). Under the Retirement Homes Act, an assessment of the resident is to be performed on admissionFootnote 6 according to criteria listed in the regulations,Footnote 7 which are similar to those in the Long-Term Care Homes Act. Although registered nurses are not required to be on staff, the Retirement Homes Act stipulates that the plan of care must be approved by a person acting under the supervision of a member of the College of Physicians and Surgeons of Ontario or the College of Nurses of Ontario.Footnote 8
In principle, every LTC home must provide a care service offering that is comprehensive for residents of all levels of need, recognizing the generally high acuity needs of residents in LTC homes. O. Reg. 79/10 lists the requirements for all nursing and personal support services, such as bathing, personal hygiene, oral care, foot and nail care, dressing, and bedtime routines. The regulation also contains specific provisions for four “Required Programs”, including (a) falls prevention and management, (b) skin and wound care, (c) continence care and bowel management, and (d) pain management.
Because retirement homes are permitted to choose which services to provide their residents, retirement homes need meet only the standards that are specific to the particular services provided in the home. As an example, regulations under the Retirement Homes Act require that a home providing a dementia care program be able to monitor the resident’s safety and well-being, offer appropriate therapies, develop adequate strategies for communicating with the resident, and strategies for identifying and addressing triggers for responsive behaviours.Footnote 9 Similarly, if the home provides skin and wound care, regulations require the home to have programs and strategies for skin and wound care assessment and intervention, prevention of infection, and appropriate transferring and positioning, with all programs incorporated into the plan of care.Footnote 10
Regulations under the Retirement Homes Act list care standards for 10 care categories,Footnote 11 and the RHRA website indicates, as disclosed by each licensed retirement home, the availability of each of these care services in every home. Table 3 is a compilation showing the percentage of homes in Ontario that provide each of the care services listed. It is not possible to determine from the table how many living units within each home use the indicated service – only that it is offered in the home and is being utilized by some residents. As the table indicates, all 728 licensed retirement homes provide meals, and virtually all (99%) offer assistance with the administration of drugs. Services that are less prevalent include feeding, wound care, and dementia care, which are available in 34 per cent, 27 per cent, and 15 per cent of homes respectively. The average number of services offered across all homes is seven of the 10 care service categories.
Table 3: Percentage of retirement homes providing care services – RHRA data

Note. Data compiled from RHRA website (Retirement Homes Regulatory Authority, n.d.)
The CMHC categorizes care services differently than the RHRA data and includes data on the percentage of retirement homes with on-site medical services (74%), nursing (68%), call bell (94%), and pharmacy services (9%).
The CORE database classifies levels of care in retirement homes according to independent living (IL), independent supported living (ISL), assisted living (AL), and memory care (MC). Table 4 shows the percentage of homes in the CORE database that provide each of these levels of care. IL units are defined as those that offer meals, housekeeping, and laundry services without the availability of personal care services or other personal assistance. Only 23 per cent of homes in the CORE database offer units without any personal care or assistance; that is, the balance of 77 per cent of homes provide some level of personal care or assistance for all units in the home. Approximately 79 per cent of homes have units that provide ISL, which offer some level of personal care or assistance in addition to meals, housekeeping, and laundry. Homes that offer AL make up 33 per cent of homes, where AL involves an addition to the base fee for more personal assistance services in a separate wing, floor, or building. Homes with MC represent about 13 per cent of all homes and include services in the base fee for persons with dementia, provided in a separate, secured area. In addition to these services in retirement homes, 7.5 per cent of homes have beds that are licensed as LTC home beds within the same residential complex.
Table 4: Percentage of retirement homes providing levels of care – CORE data

Note. Data compiled from CORE database (CORE, n.d.)
According to the CMHC data, average residence sizes have been increasing in recent years, and older homes have been expanding their capacity, partly as a means to accommodate people with higher needs. This includes a trend in the market for older homes to add a new wing or floor for residents who need high levels of care such as assisted living and memory care.
Government Funding for Care Services
Operational funding constitutes a major differentiator between the regulatory regimes of LTC homes and retirement homes. Under the current Ontario funding policy, Ontario has established per diem rates paid to LTC homes which are expected to cover the cost of nursing care, therapies, and food, although residents must still pay a monthly accommodation fee (rent). The rental fee is based on the level of accommodation (ward or basic, semi-private, private) and MOHLTC subsidies are available for residents who qualify on the basis of low income. Government does not fund the equivalent services in retirement homes, although retirement home residents may be eligible for other government-funded programs, such as home care, which, if received, can cover costs associated with ADLs and some nursing and therapies. LTC homes are also eligible for certain government-sponsored funding programs for capital that are not available to retirement homes.
For LTC homes, the MOHLTC’s long-term care homes financial policy (Ministry of Health and Long-Term Care, 2016a) delineates level-of-care funding on a per-person-per-diem basis, which provides base-level care funding for nursing and personal care (NPC), programming and support services (PSS), and raw food (RF). As of July 1, 2016, the stipulated daily rates were $94.37 (NPC), $9.42 (PSS), and $8.33 (RF). In addition, homes may not charge residents for any services with respect to which these funding envelopes apply.
According to MOHLTC’s policy for Eligible Expenditures for Long-Term Care Homes (Ministry of Health and Long-Term Care, 2016b), eligible NPC and PSS expenditures must be for (a) compensation to direct care staff in connection with a plan of care, (b) training, or (c) equipment, supplies, and devices used by staff as outlined in residents’ plans of care. The retirement home envelope includes expenditures for the purchase of food materials, condiments, and therapeutic food supplements (as distinct from the cost of food preparation, which homes may include in the accommodation charge to residents).
Cost of Accommodation and Care
As indicated, costs for care in LTC homes are paid through the MOHLTC per diem funding envelopes, but LTC homes may charge residents for accommodation. The maximum charges in LTC homes vary according to the level of accommodation, the design standard and the age of the home.Footnote 12 As of July 1, 2016, theses rates ranged from $1,794.28 for a basic, shared room, to $2,563.22 per month for a private room (Ministry of Health and Long-Term Care, 2016c). The Long-Term Care Homes Act further permits low-income residents to apply for a reduced payment for basic accommodation in LTC homes.Footnote 13
Retirement home residents pay for both accommodation and care services at market rates. Charges for the two categories are typically combined and vary according to the size of the unit and the level of care provided. Table 5 presents data from CMHC and CORE in terms of these two variables.
Table 5: Total monthly costs ($) by accommodation and care service level in retirement homes
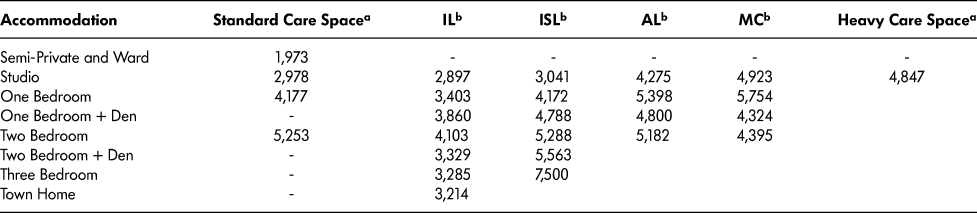
a CMHC (2016). CMHC reports the cost of a heavy care space at $4,847 per month but does not specify a unit type. It is likely that these units are studios, or possibly one-bedroom.
b IL = independent living; ISL = independent supported living; AL = assisted living; MC = memory care (CORE, n.d.).
CMHC data record the cost of retirement residence spaces according to unit type (semi-private through to two-bedroom) and distinguish between standard spaces and heavy care spaces, the latter involving a minimum of 1.5 hours of care per day (Canada Mortgage and Housing Corporation, 2016). Average monthly rents across the province for standard care spaces range from $1,973 for semi-private and ward accommodation to $5,253 per unit for a two-bedroom space. There is a wide range in rents by geographic location, with the Greater Toronto Area being about $650 more per month than the provincial average, for a standard space. CMHC does not provide cost data by unit type for heavy care spaces, though it calculates the average cost per unit at $4,847 per month in Ontario. Since heavy care spaces tend to be the smaller units (e.g., private studio), this represents a premium of approximately $1,900 per month over the cost of a standard space of the same size.
Similar to the CMHC data, the CORE data in Table 5 include the cost of accommodation and care on a combined basis and delineate care levels according to the IL, ISL, AL, and MC categories described above. As can be seen, the CMHC data show cost amounts at the standard care level (first column) that are similar to the CORE data for IL and ISL at the same accommodation level. Correspondingly, the CMHC data show the cost amounts at the heavy care level (last column) that are similar to the CORE data for AL and MC.
The all-in cost of care and accommodation in an LTC home can be compared with the cost in a retirement home, using both the CMHC and CORE data, although units may not be of identical size. CORE data indicate that the average studio unit in AL accommodation measures 351 square feet. For LH units, the MOHLTC regulates minimum space requirements for Resident Home Areas, as defined in MOHLTC’s Long-Term Care Home Design Manual, 2015 (Ministry of Health and Long-Term Care, 2015b), employing the concept of usable net floor space, which excludes the area associated with closets, washrooms, and vestibules. Using private studio accommodation in a retirement home as a comparator to private accommodation in an LTC home, the all-in costs are shown in Table 6. It should be noted that the first line in Table 6 (Cost of Accommodation) represents the cost paid by the individual resident in both LTC home and retirement home settings, while the second line (Cost of Care) represents the portion paid by the Ontario government for care. Since the care portion for retirement homes is included in the first line, and is not subsidized by government, the result is that retirement home residents pay almost double the amount personally that LTC home residents pay for a similar basket including accommodation and care. However, the all-in cost of care and accommodation in the retirement home setting is actually lower than in the LTC home when the total cost is calculated (including individual and government expenditures).
Table 6: Monthly care and accommodation costs: LTC home (private) vs. retirement home (studio)
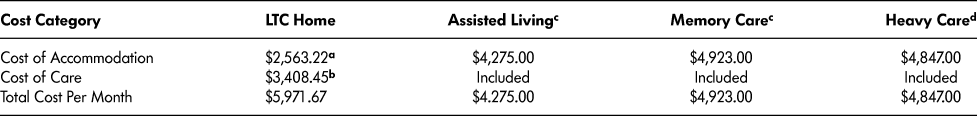
a Monthly cost of private room in LTC home (MOHLTC, 2016c).
b Monthly cost of care is based on per diem funding for nursing and personal care (NPC) ($94.37), programming and support services (PSS) ($9.42), and RF ($8.33) multiplied by 30.4 days per month (MOHLTC 2016a).
c Retirement home studio accommodation in assisted living and memory care (CORE, n.d.).
d Retirement home studio accommodation in heavy care (CMHC, 2016).
Although Table 6 gives an indication of relative costs of accommodation and care between LTC homes and retirement homes, it may underestimate total retirement home costs on a comparable basis. CMHC’s heavy care category, which includes a minimum of 1.5 hours of care per day, may still offer fewer care services or time than LTC home service levels provide. Similarly, the CORE figures for assisted living (AL) and memory care (MC) do not specify the average levels of care provided, and the CORE definition for AL, for example, states that additional care services may be added on top of the base fee.
Discussion
From a policy perspective, there is strong rationale for funding LTC homes and retirement homes in the same way to the extent that they provide similar services. This study examined the services offered in both settings, highlighting the overlap in care services between the two. Although retirement homes may be perceived within the residential care sector as catering to more independent seniors, the data indicate that they provide services across a wide spectrum of care levels, and a substantial portion of retirement homes provide services at levels similar to LTC homes.
In comparing the service offerings of retirement homes to those of LTC homes, it is instructive to distinguish between services that (a) are legally required to be provided as a minimum (by statute or regulation); (b) are actually provided, as evidenced by public or private reports or databases; and (c) may be provided, as permitted by law, and within the capacity or willingness of homes to provide. In the category of services legally required, LTC homes must provide the services described in regulations, which essentially comprise all care needs for residents requiring 24/7 care or monitoring: that is, the criteria upon which residents are admitted. Retirement homes, by contrast, are not required to provide any care services by law, although regulation requires that they conduct assessments of all residents on admission; that they admit only those for whom they can meet the requisite plan of care; and that they meet standards with respect to the care services they decide to provide.
In terms of services actually provided, LTC homes provide their legally required services, whereas retirement homes differ by owner and by home in the extent of services offered, as shown in Tables 3 and 4. The RHRA data (Table 3) show that retirement homes offer a broad array of care services similar to LTC homes, including ADLs, wound care, continence, feeding, and dementia care, and the CMHC data indicate that most retirement homes provide on-site medical or nursing services. It is also apparent that the availability of more complex services in retirement homes (e.g., wound care, dementia) is lower than for ADLs. However, the CORE database (Table 4) indicates that 77 per cent of retirement homes provide some level of personal care or assistance to all residents. Limitations of the data are the details of certain services provided. For example, retirement homes may be identified as providing ambulation, feeding, and assistance with medication, although information was not available regarding the use of hoyer lifts, tube feeding, or infusion therapies, which would imply more complex care offerings in relation to each of these services respectively.
Regarding care services that retirement homes may provide, there do not appear to be any provisions in the Retirement Homes Act or in accompanying regulations that would limit the array of services compared with those in the Long-Term Care Homes Act or O. Reg. 79/10. In addition, if the particular retirement home does not provide for certain care services, the Retirement Homes Act requires the home to allow residents to apply for and receive care services in the home from an external care provider of the residents’ choosing.Footnote 14 Although the data sources used in this study do not examine particular offerings of individual homes, some retirement homes clearly offer services that include palliative care (http://www.centralhealthline.ca/displayservice.aspx?id=131120), which may include pain medication, tube feeding, infusion therapies, and the use of lifting devices.
Given the statutory foundations that govern the two sectors, the degree of convergence in service offerings should not be a surprise. The retirement home regulatory regime drew quite clearly from precedents in the LTC home regime in requiring a bill of rights, a residents’ council for each home, and – perhaps most importantly – the placement of the plan of care as central to the residents’ care and well-being in the home. The statutes pertaining to LTC homes and retirement homes delineate the same fundamental principles of dignity, safety, security, and comfort for their residents. Both also mandate regulations that determine licensing of homes, residents’ rights, care standards, protections against abuse and neglect, inspection, and enforcement.
Despite the overlap in service offering, government funding is a stark differentiator between the two sectors. LTC homes receive funding from government with respect to operations (nursing, therapies, and food) and also for limited capital expenditures, whereas retirement homes receive virtually no direct funding of either type. Furthermore, although retirement home residents are eligible for publicly funded home care, research in Ontario indicates difficulties in accessing home care in retirement homes. A 2017 study (Poss et al., Reference Poss, Sinn, Grinchenko, Blums, Peirce and Hirdes2017) conducted in the Hamilton Niagara Haldimand Brant LHIN showed that despite significantly higher acuity levels among the retirement home residents (as measured by health conditions, incidence of dementia, use of medication, and ADL assistance), they received fewer hours of publicly funded support service than those in private homes and apartments, and substantially less nursing time. The study also concluded that seniors in retirement homes, unlike their counterparts in private homes, were paying privately for a significant portion of their services, particularly nursing. Although residents of retirement homes may be perceived as being able to afford greater amenities in their home environment, principles of health care equity should ensure that everyone has equal access to government-funded services.
When similar levels of accommodation and care are compared between LTC homes and retirement homes (using heavy care spaces from the CMHC data, or AL and MC accommodation from the CORE data), there is a marked difference in cost from the resident’s perspective. Although the total cost of care and accommodation in retirement homes appears quite competitive with that in LTC homes, the lack of direct government care funding in retirement homes leaves the retirement home resident with a monthly bill that is, on average, almost double that in an LTC home.
In Ontario, those seniors who are able to secure a bed in an LTC home are a shrinking subset of those assessed as eligible for admission on the basis of need. Those unable to gain admission must find alternative sites for care either permanently or until a room opens up. Where the alternatives involve private pay, a two-tier system results, in which some seniors pay for their care and others do not. A two-tier system, in itself, may not be a concern. Many developed countries have operated successfully with a mix of public and private pay options for residential care, although most offer a minimum threshold of public coverage or require some form of means testing to determine eligibility for public coverage.
A 2011 OECD study (Colombo, Llena-Nozal, Mercier, & Tjadens, Reference Colombo, Llena-Nozal, Mercier and Tjadens2011) examined universality and comprehensiveness of long-term care benefits, where universality implies that all seniors are eligible for the same coverage of government-funded services on the basis of need, whereas comprehensiveness considers both the breadth of services funded by government and the depth of coverage; that is, after which there must be some form of private cost-sharing of long-term care benefits.
With regard to eligibility for coverage, many countries now employ the interRAI Resident Assessment Instrument (interRAI) to assess care needs and devise care plans. The interRAI uses a range of standardized assessment instruments that apply to different care settings, including residential care (Poss et al., Reference Poss, Sinn, Grinchenko, Blums, Peirce and Hirdes2017). Most provinces in Canada are members of interRAI, including Ontario, wherein the RAI Long-Term Care Facilities Assessment System is used to assess eligibility for the LTC home waiting list. With respect to the breadth of coverage, jurisdictions vary greatly within the OECD, since long-term care comprises multiple services (e.g., supportive care, nursing care, assistive devices, social work) delivered by different providers (e.g., professional nurses, personal support workers) and applied to diverse settings (home, LTC home, community).
Regarding the depth of coverage, the Colombo et al. study (2011) noted a convergence in recent years in OECD countries towards providing a basic floor for coverage, but with public-coverage systems requiring users to share part of the cost of personal care. Some countries have used means-tested systems, as evidenced by income or asset thresholds, below which government will make its contribution. Countries that have used such a system include the United Kingdom and the United States (i.e., Medicaid). Others set an amount for the public contribution, with cost sharing applied to the residual. Australia, Germany, and France are in this category. A third group, including Japan, Korea, and Belgium, applies flat cost sharing, where a set percentage of the cost is paid by the user.
In Ontario, the breadth and depth of public coverage of seniors’ care varies markedly depending on the site of care. For those seniors residing in LTC homes, care is quite comprehensive, comprising nursing and support care, food, and certain therapies. Furthermore, although there is means testing applied to the accommodation portion in LTC homes for those with low income, there is substantial depth of coverage for the care component, with no contribution from residents and no assessment of means. Conversely, for seniors residing in retirement homes, public coverage of care services depends on the ability of the resident to access publicly funded home and community care, with services that are less extensive or consistent.
In terms of the policy options available in Ontario, the universality principle would dictate that retirement home residents of the same care needs as LTC home residents be accorded equal coverage. This might, for example, be done on the basis of interRAI assessment. However, given how comprehensive the care services are in LTC homes, this would require significant increases in government expenditures to bring qualifying retirement home residents to the same funding eligibility, possibly combined with a reduction in the existing coverage in the LTC home setting. The former could be financially onerous for government whereas the latter may be politically untenable. Given the current inequities in coverage and recognizing fiscal restraints, policy options may gravitate towards some form of means testing on residents, or a formula that sets a base level of government funding, over which private contributions are required.
Study Limitations
The study data presented in this article pertain to services offered by residential care homes, rather than to the health characteristics of the residents themselves. The conclusion that care services offered reflect actual care needs of the resident populations would need to be based on the assumption that the services offered to residents are in accordance with the plan of care and based on proper assessment and administration.
Although our study described the characteristics, costs, and availability of care services, we did not evaluate the quality of the services being provided. There is extensive literature examining the quality of care in seniors’ residential homes, primarily in long-term care. Much of this research relates quality of care to differences in ownership models (Cabin, Himmelstein, Siman & Woolhandler, Reference Cabin, Himmelstein, Siman and Woolhandler2014; McGregor et al., Reference McGregor, Tate, McGrail, Ronald, Broemeling and Cohen2006; Shapiro & Tate, Reference Shapiro and Tate1995). According to MOHLTC’s Health Data Branch (Ministry of Health and Long-Term Care, 2015a), 57 per cent of LTC homes are owned by for-profit firms, while 27 per cent are owned by not-for-profits and 16 per cent by municipalities. Similar data are not reported for retirement homes, although the vast majority are considered to be for profit.
Cost data compared LTC homes and retirement homes on the basis of accommodation and service levels that were similar but not identical. Room sizes, precise care services, and other amenities differed somewhat between LTC homes and the higher-level retirement home offerings. Comparisons were, nevertheless, considered instructive.
Suggestions for Future Research
Future research should examine policy options to alleviate inequities in access to care funding for seniors. At present, all LTC home residents in Ontario receive full care funding regardless of how wealthy, and retirement home residents receive no care funding regardless of how poor. As we have discussed, viable options should foster greater universality with more even eligibility. At the same time, limits may need to be placed on the public cost burden, either by setting ceilings on base funding or introducing a form of means testing. As noted, means testing is already being employed in LTC homes for accommodation – as distinct from care – with subsidies for those in financial need. This discussion of means testing challenges people’s attitudes about health care funding, and it poses practical obstacles as well. Means testing of assets (as opposed to income) is inherently harder to implement, although many seniors are asset rich and income poor.
In addition, research should explore alternative mechanisms by which funding is disbursed. Funding of seniors’ residential care does not have to involve payments to the residence providing care. Viable options also include self-directed funding by which individuals, assessed for their needs, can apply public funding to approved providers – including perhaps retirement homes – that offer the care they need. This would allow the senior to determine what organization provides the care rather than competing for a place where the care is available.
Finally, there is value in studying how owners and operators of residential care make decisions around location and, in the case of retirement homes, what services and amenities to offer. Since seniors typically have little discretion concerning their location or their health condition, policy geared towards improving residential care options may be best directed at shaping how and where services are made available from the supply side.
Conclusion
In the LTC home sector, demand for long-stay beds continues to grow, with consequent stress on existing supply. Shifting age demographics across many jurisdictions suggest that the challenges experienced in Ontario may have relevance for other regions, and that residential care will continue to play an important role in meeting the housing and care needs of many seniors. Accordingly, retirement homes can be expected to continue to grow in number, with their suite of care services allowing them to absorb much of the demand in the system for seniors requiring a high level of care. Cost data suggest that retirement home care and accommodation services are competitive with those in LTC homes when government funding is ignored. The implications of this study suggest that funding policies that differentiate between high-need residents in LTC homes and retirement homes will become a growing policy dilemma.








