Nutrition in early life, from preconception through to lactation, can influence the growth, development and long-term health of children( Reference Osmond and Barker 1 ). Many studies have examined nutrient intakes during pregnancy in association with pregnancy or birth outcomes or have assessed adherence to nutrient recommendations( Reference Blumfield, Hure and Macdonald-Wicks 2 , Reference Berti, Biesalski and Gärtner 3 ). While these studies are useful for identifying the importance and deficiencies of key nutrients, studies focusing on food intake and dietary patterns of pregnant women often have more practical applications in terms of conveying the dietary changes required to improve nutritional status. Given that individuals generally purchase and consume foods, not nutrients, dietary recommendations that focus on intake of foods and food groups are considered more practical and easy to follow for women than recommendations focusing on nutrients.
Healthy dietary patterns during pregnancy have been associated with reduced risk of adverse pregnancy and birth outcomes( Reference Thompson, Wall and Becroft 4 , Reference Brantsaeter, Haugen and Samuelsen 5 ). It is therefore concerning that suboptimal dietary quality has been consistently reported during pregnancy, reflecting poor adherence with dietary guidelines( Reference Hure, Young and Smith 6 , Reference Bodnar and Siega-Riz 7 ). Moreover, studies from Australia and other developed countries including New Zealand, the UK, the USA and Canada have consistently shown poor adherence to food group recommendations during pregnancy( Reference Bodnar and Siega-Riz 7 – Reference Wen, Flood and Simpson 12 ).
To help women achieve a nutritionally adequate diet during pregnancy, most countries have dietary guidelines that recommend the number of daily servings that should be consumed from each of the core food groups, namely grain foods, vegetables, fruit, dairy/alternatives and meat/alternatives( 13 , 14 ). The Australian Dietary Guidelines (ADG) were recently updated, in February 2013, with changes made to the recommended number of servings from some of the ‘Five Food Groups’ in pregnancy( 13 ). To date, no Australian studies have reported pregnant women’s adherence to the current recommendations for the Five Food Groups. The most recent Australian data regarding compliance with dietary guidelines during pregnancy were collected in 2008, prior to the introduction of the current dietary guidelines( Reference McLeod, Campbell and Hesketh 15 ). However, that study assessed maternal dietary intake over the previous 12 months, not exclusively during pregnancy, with mean postnatal age being 3·8 (sd 1·4) months at assessment; and compared daily food group servings with the minimum amount recommended for women aged 19–60 years, not pregnant women( Reference McLeod, Campbell and Hesketh 15 ). As the dietary requirements for many nutrients including folate, iodine and Fe increase during pregnancy, women often need to make dietary changes to meet their increased requirements.
Additionally, to the best of our knowledge, no previously published nationwide studies have examined whether pregnant women in Australia make dietary changes or studied their reasons for not making dietary changes. Furthermore, there are no known studies which examine women’s perceptions regarding their dietary quality during pregnancy. The present study provides a better understanding of women’s dietary behaviour in pregnancy. Its aims were to: (i) assess adherence to the current ADG with respect to the Five Food Group recommendations for pregnancy; and (ii) determine predictors of adherence.
Methods
Sample and study design
The questions used to address the aims of the current paper were part of a large web-based cross-sectional survey designed to assess the nutrition knowledge, attitudes and practices of pregnant women. The survey was administered to two cohorts of pregnant women. A national cohort of Australian pregnant women was recruited using a reputable online consumer panel provider (Pureprofile; www.pureprofile.com/au). A South Australian (SA) cohort of pregnant women was recruited by a member of the study team approaching women attending routine antenatal appointments at a tertiary public maternity hospital (the Women’s and Children’s Hospital in Adelaide, SA). Word of mouth and study posters displayed around the Women’s and Children’s Hospital were also used to recruit the SA cohort. Both cohorts were included to determine whether responses from pregnant women recruited via an online panel provider differ from those of the general population of pregnant women attending antenatal care at a public hospital. Eligibility criteria were: currently pregnant; able to give informed consent; aged 18–49 years; and not working in the nutrition industry, in market research or in nutrition-related health research. All participants received a unique URL (web address) to the survey. Estimated completion time for the overall survey was 35–45 min depending on responses provided, and no time limit was set for survey completion. A reminder email was sent to women in the SA cohort who did not complete the survey within two weeks of receiving the URL. All data were collected between June and November 2013.
Information about the study was provided and consent was obtained from all participants before completing the survey questionnaire. Ethics approval for the study was obtained from the University of Adelaide Human Research Ethics Committee and the Women’s and Children’s Health Network Human Research Ethics Committee.
Data collection
The overall survey included questions regarding nutrition knowledge and information sources, dietary practices and perceptions, use of and preferences for dietary supplements, attitudes and practice regarding gestational weight gain, and sociodemographic and pregnancy-related characteristics. The content of the survey was informed by findings from individual interviews and focus group discussions with women who were pregnant or who were less than 12 months postpartum and breast-fed their infant( Reference Malek, Zhou and Makrides 16 ); the ADG and nutrition recommendations for pregnancy( 13 , 17 – 20 ); and a review of the literature regarding factors influencing dietary intake during pregnancy and question format( Reference Malek, Umberger and Zhou 21 , Reference Williams, McHenery and McMahon 22 ). The present paper reports results from thirty questions related to the aims of the current study, including seven questions regarding sociodemographic characteristics, eight questions regarding pregnancy-related characteristics, twelve questions regarding dietary intake during pregnancy and three questions regarding perceived healthiness of dietary intake.
Sociodemographic questions assessed maternal age, educational attainment, area of residence (living in v. outside metropolitan area), gross annual household income, living arrangements (living with v. without a partner), whether women were Australian-born, ethnicity and usual physical activity level prior to pregnancy (based on the national physical activity guidelines for adults). Pregnancy-related questions assessed gestational age, gravidity, parity, planned/unplanned pregnancy, pre-pregnancy weight and height (used to calculate pre-pregnancy BMI), and maternal smoking status and alcohol consumption during pregnancy.
Dietary intake questions assessed number of daily servings consumed from each food group during an average week of pregnancy; and changes in intake of selected high-listeria-risk, allergenic and Hg-containing foods. Information was also collected on whether deliberate changes were made to dietary intake specifically for pregnancy (excluding changes made due to morning sickness); timing of dietary changes; reasons for not making dietary changes; usual bread and dairy choices with respect to fibre and fat content; women’s perceptions of the healthiness of their diet during pregnancy (‘healthy’, ‘unhealthy’ or ‘neither healthy nor unhealthy’); whether they believed their diet during pregnancy was ‘more healthy’, ‘less healthy’ or whether there was ‘no change in healthiness’ compared with their usual pre-pregnancy diet; and whether their level of concern about healthy eating changed as their pregnancy progressed.
A brief six-item FFQ was developed for the purpose of the study, which assessed intake from the Five Food Groups defined in the ADG. Women were asked to estimate the number of servings consumed from each of the Five Food Groups and ‘discretionary choices’ during an average week of their pregnancy. Examples of the amounts and types of foods equivalent to one serving from each food group were provided( 13 ). For each food group, responses could be recorded as number of servings ‘per day’ or ‘per week’. The average number of daily servings was calculated for each food group prior to data analysis. This allowed comparison of actual intake with the recommended intake for pregnancy from each food group in the current ADG.
Statistical analysis
Data were analysed using the statistical software package IBM SPSS Statistics version 20·0 and the level of significance was set at P<0·05. Descriptive statistics were calculated for all variables including frequencies for categorical variables; means and standard deviations for normally distributed variables; and medians and interquartile ranges for non-normally distributed variables. Differences in categorical variables between the two cohorts were investigated using the Pearson χ 2 test; and differences in medians were investigated using the Mann–Whitney U test. For each food group, adherence was defined as consuming the recommended number of daily servings. Logistic regression analyses were used to identify independent predictors of adherence to the recommendations for each of the Five Food Groups. The independent variables used in the regression analyses were those that previous studies have found to influence dietary intake in pregnancy and were variables that in the present study were correlated with adherence to the food group recommendations at the 20 % level of significance, as recommended by Maldonado and Greenland( Reference Maldonado and Greenland 23 ). The included independent predictors were: maternal age, education level (four categories), household income (five categories), area of residence (metropolitan v. other), born in Australia (yes, no), ethnicity (six categories), living with a partner (yes, no), planned pregnancy (yes, no), pre-pregnancy compliance with national physical activity guidelines (yes, no), pre-pregnancy overweight or obesity (yes, no), nulliparous (yes, no), first pregnancy (yes, no) and smoking during pregnancy (yes, no). Cohort membership was not significantly correlated with adherence to the recommendations for any of the Five Food Groups. Thus, findings are presented for both cohorts together with regard to predictors of adherence. Additionally, the Pearson χ 2 test was used to determine whether perceived healthiness of dietary intake was associated with adherence to the recommendations for the Five Food Groups( Reference Rea and Parker 24 ).
Five previous studies showed that adherence to the recommendations for the core food groups ranged from 3 % to 85 %. To detect an average adherence rate of 40 % with 80 % power and accuracy of ±5 %, a sample size of 369 was required( 25 ). Further, based on Hosmer and Lemeshow’s( Reference Hosmer and Lemeshow 26 ) guideline of ten cases per independent variable for logistic regression analysis, our sample size was considered adequate to examine predictors of adherence for all food groups.
Results
Participants
In total, 857 respondents completed the online survey (national cohort, n 455; SA cohort, n 402). Overall completion rate was 57 % (857/1493) and did not differ between cohorts. The participants’ characteristics are shown in Table 1 and there were some differences between the two cohorts. Compared with the national cohort, the SA cohort had a statistically higher proportion of nulliparous women, women living in metropolitan areas and supplement users.
Table 1 Participant characteristics of the samples of pregnant women living in Australia, June–November 2013
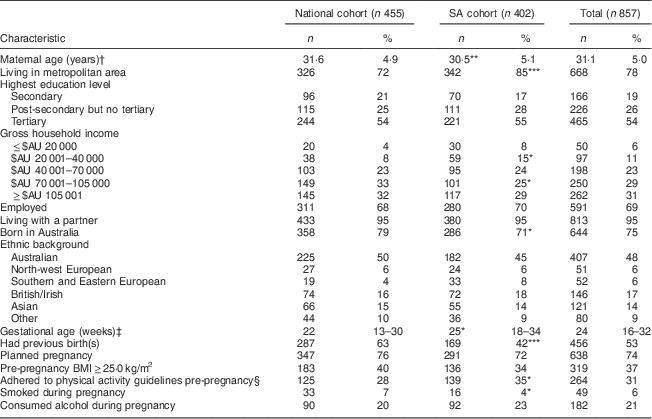
SA, South Australian.
*P<0·05, **P<0·01, ***P<0·001 (for difference between national and SA cohort).
† Data are mean and standard deviation.
‡ Data are median and interquartile range.
§ Defined as ≥30 min of exercise on ≥5 d each week( 38 ).
Dietary changes for pregnancy
Sixty-three per cent of women reported making some changes to their usual pre-pregnancy diet, specifically for pregnancy. Dietary changes were significantly more common among women in the SA cohort compared with the national cohort (73 % v. 54 %, P<0·001) and among nulliparous women compared with multiparous women (73 % v. 55 %, P<0·001). Of the women who reported making dietary changes, about one-half started making changes as soon as they found out they were pregnant (55 %). For those who reported not making any dietary changes, the main reason was the belief that their diet was already healthy and balanced (61 %). One-third of the sample also did not think they needed to make any changes (33 %), and about one in ten thought diet change was too difficult (8 %) or did not know what changes they should be making (7 %). Reasons for not making dietary changes did not differ significantly between cohorts. One-half of the women reported being more concerned about healthy eating as their pregnancy progressed, 41 % reported no change in their level of concern and the remaining 9 % reported being less concerned.
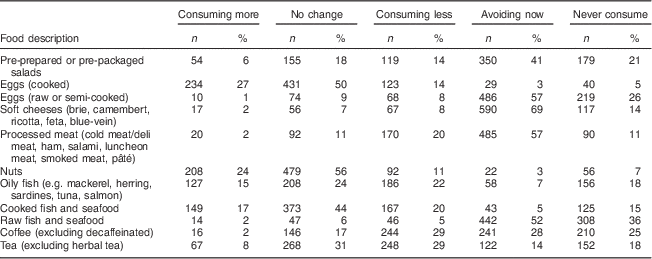
Table 2 compares the women’s intakes of selected high-listeria-risk, allergenic and Hg-containing foods during pregnancy with their usual intakes before pregnancy/before planning pregnancy. Over half of the women surveyed reported avoiding or eating less pre-prepared or pre-packaged salads, soft cheeses, processed meat, raw or semi-cooked eggs, and raw fish and seafood. About one-half also reported avoiding or drinking less caffeinated tea and coffee in pregnancy. Additionally, cooked fish and seafood, and specifically oily fish, were avoided or consumed in smaller quantities by one-quarter to one-third of women.
Table 2 Current intakes of selected high-mercury, high-listeria-risk and allergenic foods compared with usual intakes before pregnancy and before planning pregnancy for the total sample of pregnant women living in Australia (n 857), June–November 2013
Food group intake during pregnancy and adherence with the recommendations
Median daily servings consumed from each food group during a typical week of pregnancy and the proportions of women meeting the serving recommendation are shown in Table 3. Of the Five Food Groups, the greatest adherence was with the recommendations for the fruit and dairy groups, with 56 % and 29 % of the total sample meeting the minimum recommended servings for pregnancy, respectively. Less than 10 % of women met the minimum recommendations for each of the other food groups. Overall, 37 % of the women did not meet any of the Five Food Group serving recommendations for pregnancy, 35 % met one, 21 % met two, 6 % met three and 1 % met four; none of the women met all five recommendations. Adherence rates did not differ significantly between cohorts (data not shown). The meat group was the only food group for which median daily servings differed significantly between cohorts (national cohort: median=1·0 (interquartile range 1·0–2·0) servings/d v. SA cohort: median=1·0 (interquartile range 0·7–2·0) servings/d, P=0·010). Although statistically significant, the actual difference in servings was small.
Table 3 Median (IQR) daily servings from food groups during pregnancy and adherence to serving recommendations for the total sample of pregnant women living in Australia (n 857), June–November 2013

IQR, interquartile range.
† Recommendations for pregnancy as specified in the 2013 Eat for Health Australian Dietary Guidelines( 13 ).
‡ Example serving: 1 slice bread; ½ medium bread roll or flat bread; ½ cup porridge; ¾ cup breakfast cereal flakes or ¼ cup muesli; 1 crumpet, small English muffin or plain scone; ½ cup cooked rice, pasta, noodles, other grains; 3 crisp breads.
§ Example serving: ½ cup cooked orange (e.g. carrots or pumpkin) or cruciferous (e.g. broccoli, cauliflower or cabbage) vegetables; 1 cup green leafy vegetables or salad vegetables (raw); 1 small–medium tomato; ½ cup cooked or canned beans, peas or lentils; 1 small or ½ medium potato or other starchy vegetable, e.g. sweet potato, sweet corn, taro or cassava.
|| Example serving: 1 medium piece (e.g. apple, banana); 2 small pieces (e.g. apricots, kiwi fruit); 1 cup diced pieces/canned fruit; ½ cup juice; dried fruit (e.g. 4 dried apricot halves, 1·5 tablespoons sultanas).
¶ Example serving: 1 cup milk (250 ml); ½ cup evaporated milk; 2 slices cheese or 4 pieces (3 cm×2 cm); 1 tub yoghurt (200 g); 1 cup custard (250 ml); 1 cup soya, rice or other cereal drink with at least 100 mg added Ca per 100 ml.
†† Example serving: 65 g cooked meat (e.g. ½ cup lean mince, 2 small chops or 2 slices roast meat); 80 g cooked poultry (e.g. ½ chicken breast); 100 g cooked fish fillet or small can of fish; 2 eggs; 1 cup cooked or canned beans, peas, lentils or tofu; ⅓ cup nuts; ¼ cup seeds.
Of the women who reported consuming bread, the majority usually chose high-fibre (‘wholemeal, whole/multi grain, rye’) bread over white bread (70 % v. 30 %). About one-half of the women who reported consuming milk and yoghurt usually chose reduced-fat varieties (51 % and 49 %, respectively), while only one-third of those who ate cheese usually chose reduced-fat cheese (33 %). This did not differ significantly between cohorts.
Predictors of adherence to recommendations for each of the Five Food Groups
The predictors of adherence to the food group recommendations are shown in Table 4. Women living outside metropolitan areas were more likely to meet the daily serving recommendation for the ‘vegetables and legumes/beans’ group than women living in metropolitan areas. Women who did not smoke during pregnancy, were not overweight or obese prior to pregnancy and who had annual household incomes of ≥$AU 20 000 were more likely to meet the recommendation for the ‘fruit’ group. Being Australian-born and complying with the national physical activity guidelines prior to pregnancy positively predicted adherence to the recommendations for the ‘fruit’ and ‘milk, yoghurt, cheese and/or alternatives’ groups. There were no significant independent predictors of adherence to the recommendations for the ‘grain (cereal) foods’ or the ‘lean meat and poultry, fish, eggs, nuts and seeds, and legumes/beans’ group.
Table 4 Odds ratios for adherence to food group serving recommendations for the total sample of pregnant women living in Australia (n 857), June–November 2013
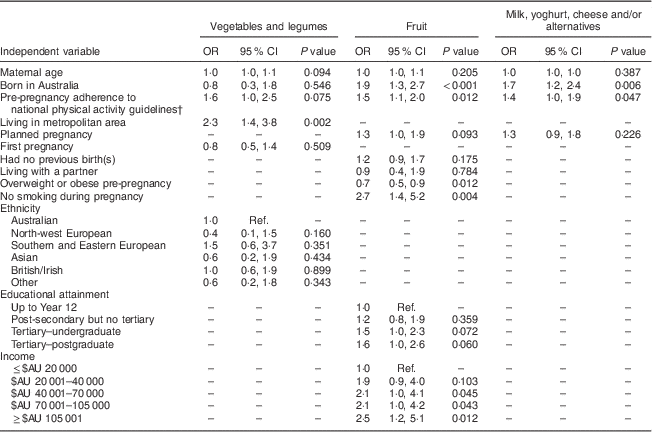
Ref., reference category.
† Defined as ≥30 min of exercise on ≥5 d each week( 38 ).
Perceptions of dietary quality during pregnancy
Almost two-thirds (61 %) of the women surveyed believed their diet during this pregnancy was healthy; one in ten believed it was unhealthy; and the remaining 29 % believed it was neither healthy nor unhealthy. Further, one-half believed that their diet during pregnancy was healthier and 10 % believed their diet was less healthy now, compared with their usual diet pre-pregnancy. There were no significant differences between cohorts with the exception that more women in the SA cohort perceived their diet during pregnancy as ‘healthy’ compared with the national cohort (66 % v. 56 %, P=0·005).
Perceived healthiness of diet was significantly associated with meeting the recommended servings of fruit (χ 2 (1, n 857)=19·77, P<0·001) and dairy (χ 2 (1, n 857)=3·88, P=0·049). In other words, women who perceived their diet as healthy were more likely to consume the recommended servings from these two food groups. The same associations were seen in both cohorts, with the exception of the dairy association, which was absent in the SA cohort. No other significant associations were found between perceived healthiness of diet and adherence to the recommendations for the other food groups.
Discussion
The present study provides the first Australian national data regarding adherence to the current Eat for Health ADG for pregnancy. Overall, poor adherence to the recommendations for the Five Food Groups was revealed among pregnant women, with no women meeting all Five Food Group recommendations. The highest adherence to recommendations was for the ‘fruit’ and ‘milk, yoghurt, cheese and/or alternatives’ food groups; and adherence was considerably lower for the remaining food groups. These latter food groups therefore warrant particular attention in healthy eating interventions targeting pregnant women. Factors found to predict adherence to daily serving recommendations varied considerably between food groups, with fewer predictors identified for the food groups with the lowest adherence rates.
Adherence to dietary guidelines
Our findings regarding adherence to food group recommendations are largely consistent with previous research conducted prior to the introduction of the current ADG in 2013( Reference Blumfield, Hure and MacDonald-Wicks 8 ) and with large US( Reference Bodnar and Siega-Riz 7 ), New Zealand( Reference Morton, Grant and Wall 10 ) and European( Reference von Ruesten, Brantsæter and Haugen 27 ) studies, most of which assessed dietary intake using validated methods. The only exception was the meat/alternatives group, with lower adherence to the recommendations found in our study compared with the Australian Longitudinal Study on Women’s Health (ALSWH) due to the increase in recommended daily servings from one-and-a-half to three-and-a-half in the current guidelines to help meet the increased requirements for protein, Fe and Zn in pregnancy( Reference Blumfield, Hure and MacDonald-Wicks 8 , 13 ). It is possible that women may not be aware of the increased servings required from the meat/alternatives group in pregnancy, they may not know how to achieve this additional intake and/or other psychosocial factors may be acting as barriers to adherence. Further exploratory research would be required to determine likely causes. Importantly, the low adherence to the meat/alternatives serving recommendation does not necessarily indicate inadequate intake of key nutrients like protein, Fe and Zn. Rather, women may be deriving these nutrients from processed meat and meat products (e.g. salami, mettwurst, sausages, meat pies) that are higher in fat and salt and are not included in the meat/alternatives food group.
Additionally, although the six-item FFQ used in our study included specific examples of core foods commonly consumed by Australians for each of the Five Food Groups, our results may have underestimated true adherence rates if women did not count additional foods for each food group that were not listed as specific examples in the survey. A more comprehensive list of foods may be required to adequately capture this information in the six-item FFQ. On the other hand, the present study sample over-represented women with higher educational attainment and higher household incomes, as well as women who planned their pregnancy and who did not smoke (factors generally associated with healthier dietary intake). Thus, these characteristics of the sample may lead to overestimation of the true adherence rates among pregnant women in general. On balance, the overall adherence with the food group recommendations is still poor. This suggests a need to improve knowledge and adherence to the recommendations for all Five Food Groups in pregnancy in general.
Predictors of adherence to dietary guidelines
The finding that the variable ‘being Australian-born’ was able to help predict adherence to the dairy recommendation is comparable with results of a New Zealand study which found ethnicity to be an independent predictor of adherence to the dairy recommendation during pregnancy( Reference Morton, Grant and Wall 10 ). Notably, while individuals living outside metropolitan areas have generally been shown to have poorer dietary quality or to be at greater risk of poor dietary intake( Reference Asirvatham 28 ), we found that living outside metropolitan areas positively predicted adherence to the recommendations for the ‘vegetables and legumes/beans’ group in pregnancy. It is possible that the women living outside metropolitan areas who participated in the survey grow their own vegetables, make a more conscious effort to consume more vegetables, are more health conscious in general and/or have more time for meal preparation. This finding should however be interpreted with caution as further research is required to confirm and, if warranted, explain this finding.
Our identification of considerably fewer predictors of adherence for the three food groups with the lowest adherence rates has a number of possible explanations. For example, this could be due to the low adherence rates (1·5–9·5 %) necessitating much larger sample sizes for logistic regression than we had in our analyses( Reference Peduzzi, Concato and Kemper 29 ). Alternatively, this finding may suggest that factors other than sociodemographic and pregnancy-related characteristics influence adherence to the recommendations for these ‘low adherence’ food groups. Influential factors could include psychosocial variables such as attitudes; perceptions regarding norms, behavioural control and risk of adverse outcomes; and stress( Reference Malek, Umberger and Zhou 21 ). Thus, as well as recruiting larger study samples, future studies investigating predictors of adherence to the food group recommendations in pregnancy should consider including psychosocial factors in their analyses.
Perceptions of dietary quality during pregnancy
Although reaching statistical significance, the strength of the associations between perceiving dietary intake to be healthy and adhering to the fruit and dairy recommendations was weak or negligible. Furthermore, almost two-thirds of women believed their diet was healthy during pregnancy, yet the majority did not consume the recommended daily servings of the Five Food Groups. This suggests that pregnant women were not able to judge the quality of their diet. This is especially concerning in light of our finding that the main reason for not making dietary changes specifically for pregnancy was the belief that dietary intake was already healthy.
While women’s knowledge regarding the dietary guidelines was not specifically assessed in our study, a recent review highlighted that nutrition education is generally inadequate during pregnancy despite health-care providers considering it important( Reference Lucas, Charlton and Yeatman 30 ). Thus, increasing awareness and understanding of dietary guidelines may be an important step towards improving women’s ability to evaluate their dietary quality against a ‘healthy balanced diet’, as defined by the ADG. This may then prompt women to make positive dietary changes.
In providing nutrition education, emphasis should also be placed on obtaining nutrients from the more nutrient-dense foods (included in the five core food groups) rather than non-core foods, which tend to be higher in fat, salt and or/sugar and, in the case of grain foods, lower in fibre. Previous research indicates that main health-care providers during pregnancy (including general practitioners, obstetricians and midwives) may be best suited to providing this information, although they may require additional resources (including time and training) to do so( Reference Malek, Umberger and Zhou 21 , Reference Lucas, Charlton and Yeatman 30 ). The effectiveness of such strategies among women who have poor dietary quality but perceive their diets to be healthy may, however, be influenced by their willingness to increase their nutrition knowledge and understanding of a healthy diet, as suggested by Kearney and McElhone’s( Reference Kearney and McElhone 31 ) findings.
As in previous research, women in our study reported avoiding or eating less high-listeria-risk foods during pregnancy and eating less fish and seafood( Reference Morton, Grant and Wall 10 , Reference Martin, Savige and Mitchell 32 ). Considering the following factors, it may be timely to reconsider how messages around fish intake during pregnancy are framed and delivered to the public: seafood has a relatively small impact on maternal blood Hg levels (accounting for approximately 9 % of the variation in whole-blood total Hg levels)( Reference Golding, Steer and Hibbeln 33 ); fish is rich in n-3 fatty acids and other essential nutrients such as iodine and vitamin D; and the positive associations found between fish intake during pregnancy and fetal neurodevelopmental outcomes( Reference Starling, Charlton and McMahon 34 ).
Overall, despite almost two-thirds of women reportedly making dietary changes specifically for pregnancy, the extent to which dietary quality changed from before to during pregnancy cannot be determined from the available data. Previous research, however, indicates that dietary changes are minimal( Reference Crozier, Robinson and Godfrey 35 ). Furthermore, a recent Australian study among overweight and obese women showed that dietary quality decreased as pregnancy progressed( Reference Moran, Sui and Cramp 36 ). This suggests that women need greater support making healthy dietary changes and maintaining healthy eating patterns throughout pregnancy.
Study strengths and limitations
Overall, use of an online survey for data collection enabled more efficient collection of national data and made survey completion more convenient for respondents. It did, however, exclude women without Internet access from participating in the study. As with all survey research, there is also the issue of self-selection bias, with those more interested in nutrition more likely to complete the survey. It is not surprising then that the study sample over-represented women who had a post-secondary education, were from higher-income households, had planned their pregnancy, had used dietary supplements and did not smoke during pregnancy. Nevertheless, the sample was fairly representative of the population of women giving birth in Australia during 2012 with respect to mean maternal age and the proportion of women who were nulliparous, Australian-born and living in metropolitan areas( 37 ). Additionally, in the national cohort, the relative proportion of respondents obtained from each state and territory was similar to the distribution of births in Australia in 2012( 37 ). Although the FFQ used to assess dietary intake in the present study has not been validated, our findings regarding rates of adherence with food group recommendations are largely consistent with previous studies. This brief FFQ was included in the survey in place of a more complex, detailed instrument as it was simple, based on the Five Food Groups defined in the ADG, allowed participants to be categorised as adhering/not adhering to food group serving recommendations and minimised respondent burden. With further fine-tuning and validation of the short FFQ, it could be used as a quick and simple screening tool to assess dietary quality of pregnant women in both community and clinical settings, and could potentially be developed into an online or mobile phone application for self-monitoring.
Conclusion
Our study shows that the majority of pregnant women in Australia perceive their diets to be healthy, yet most do not consume the recommended daily servings from the Five Food Groups. Intervention strategies aiming to increase women’s ability to evaluate their diet quality against the dietary guidelines are warranted. Findings from this research suggest that intervention strategies should target women born outside Australia, from lower-income households, smokers, less physically active women, and women who are overweight and obese. If successful, such interventions may encourage positive dietary changes that lead to increased adherence to the food group recommendations in pregnancy and optimise pregnancy and long-term health outcomes.
Acknowledgements
Acknowledgements: The authors thank the women who participated in this study. Financial support: This work was supported by a Women’s and Children’s Health Research Institute and University of Adelaide Faculty of Health Sciences Divisional Scholarship; a Women’s and Children’s Hospital Foundation Population Health PhD Top-Up Scholarship; and a CSIRO Preventative Health Flagship Grant. The University of Adelaide Faculty of Health Sciences, the Women’s and Children’s Hospital Foundation and CSIRO had no role in the design, analysis or writing of this article. Conflict of interest: None. Authorship: L.M., S.J.Z., W.U. and M.M. designed the study reported in this manuscript. L.M. coordinated data collection and analysed the data. L.M., S.J.Z., W.U. and M.M. interpreted the data. L.M. drafted the manuscript which was revised by all of the authors. All authors have given their final approval for the submitted manuscript. Ethics of human subject participation: This study was conducted according to the guidelines laid down in the Declaration of Helsinki and all procedures involving human subjects were approved by the University of Adelaide Human Research Ethics Committee and the Women’s and Children’s Health Network Human Research Ethics Committee. Written informed consent was obtained from all participants.







