Sri Lanka is a developing country in South Asia undergoing rapid socio-economic transition in which both over- and undernutrition are serious health concerns. In 2005, the prevalence of hypertension, diabetes and dysglycaemia in Sri Lanka was nearly 20 %, 11 % and 20 %, respectively(Reference Wijewardene, Mohideen and Mendis1, Reference Katulanda, Constantine and Mahesh2). Although Sri Lanka is a developing country, it has recorded 524 deaths per 100 000 for mortality from cardiovascular and cerebrovascular disease, a figure which is considerably higher than the rate in many affluent countries such as the UK (427), the USA (397), Australia (308) and France (205)(Reference Abeywardena3). Despite Sri Lanka having a very high prevalence of non-communicable diseases (NCD) and associated mortality, little is known about the causative factors. It is widely believed that the NCD epidemic in the country is partially associated with unhealthy dietary habits(Reference Abeywardena3).
Food intake patterns play an essential role in the maintenance of health and well-being at both individual and population levels. Food products supply energy and essential macro- and micronutrients; however, over- or undernutrition has the potential to cause serious health consequences(Reference Krebs-Smith, Cleveland and Ballard-Barbash4). A national-level dietary survey has several important functions and provides valuable information. Survey data are also helpful to monitor nutritional status, observe dietary practices and study the relationships between diet and disease. The main objective of the present study was to identify food consumption according to servings in Sri Lankan adults. In addition, we aimed to derive serving sizes and food exchange information not presently available for some food groups in Sri Lanka.
Methodology
Participants
Participants for the present study were recruited based on the sample from the Sri Lanka Diabetes and Cardiovascular Study (SLDCS), a national study conducted between 2005 and 2006. Detailed sampling procedures used in the SLDCS have been previously reported(Reference Katulanda, Constantine and Mahesh2). The current study was conducted between January and March 2011 during which time the researchers were able to collect data from the previously missing North and Eastern provinces in the SLDCS because of the improved security situation. In the original study, researchers randomly selected 100 clusters consisting of fifty individuals according to the probability-proportional-to-size method, to gain a representative sample from seven of the nine provinces. From the 100 clusters, ten were randomly selected stratifying to the area of residence and ethnicity. To address the gap in national data from the remaining two provinces, we selected one cluster of fifty participants from the North and East by using ‘Village Office Units’ voter lists to randomly select one household. The remaining forty-nine households were selected applying the uniform method used in the SLDCS. In summary, the total sample in the present study comprised 600 individuals (500 from previous SLDCS areas and 100 additionally from the Northern and Eastern provinces). Those who were pregnant, lactating, acutely ill or on a therapeutic diet were excluded. The present study was approved by the Ethics Review Committee of the Faculty of Medicine, University of Colombo, Sri Lanka.
Procedure
The selected households were initially contacted via telephone by the study team who provided information regarding the study and verbal consent was taken. Where telephone facilities or contact telephone numbers were unavailable, households were visited by the study team with prior postal notice. Subsequently, households were visited on a random day to minimize bias for food selection. Dietary and demographic details were obtained after final written informed consent was obtained. An interviewer-administered questionnaire was used for data collection. Information regarding sociodemographic factors, timing of daily routines and meals was obtained.
24 h dietary recall
Two interviewers obtained dietary data by asking the participants what they ate in the previous 24 h in direct chronological order. To minimize the inter-personal variation, at the end of the day the two interviewers reviewed each other's work and maintained homogeneity of the recording procedure. Where there was a disparity in the dietary recalls, participants were re-contacted or the 24 h recall repeated on a different day. Food portion sizes were obtained using standard household measures such as plate, bowl, cup, glass and different spoons; these were clarified by demonstration using real utensils, a series of food portion size photographs and a food atlas(Reference Nelson, Atkinson and Meyer5, Reference Suzana, Noor Aini and Nik Shanita6). When participants recalled the amount of food consumed by weight, this value was entered.
Data entry and analysis
The daily food intake was divided into seven food groups: (i) cereal or equivalents (starchy foods); (ii) vegetables; (iii) fruits; (iv) meat or alternatives; (v) pulses; (vi) dairy; and (vii) added sugars. For the detailed methodology regarding the translation of food eaten into the respective food groups, see Supplementary Materials, Part 1.
Method for translating food consumed into food group servings
All food recorded in 24 h recall by each participant was assigned to one of the seven major food groups defined above. Food was recorded either in household measures (cups, spoons, etc.) or by weight in the 24 h recall and was translated into serving size for each food consumed. Thus, the weight of food in grams or the amount of household measure of food was divided by the weight of one serving or the amount of household measure for one serving and summed to derive servings of each food group. Food that was a mixture of several food types was disaggregated before ingredients were categorized into appropriate food groups. An example of disaggregation is illustrated in Fig. 1. A similar method was used for the US population for food grouping when food mixtures required disaggregation(Reference Cleveland, Cook and Krebs-Smith7). The servings of food consumed in mixed foods were calculated by modifying existing recipe files to develop a cascaded recipe file with multiple levels of breakdown. Common recipes were accepted after checking for face validity by consulting nutritionists; when in doubt, the respective households were contacted(Reference Dissanayake8). For uncommon food items, detailed recipes were collected at the time of the 24 h dietary recall from the participant or other responsible person in each household.

Fig. 1 Example of a disaggregated recipe showing multiple levels (Chicken Koththu)
Statistical analyses
Average daily portion sizes were calculated as the total portion size divided by the number of participants. The sum of vegetable and fruit portions was divided to obtain average daily fruit and vegetable consumption, and the same method was used to calculate average daily meat and pulse intakes. We analysed the mean daily consumption of each food group according to gender using the two-sample t test, to determine whether the mean values differed between genders. Data were analysed using the SPSS statistical software package version 14 (SPSS Inc.). In all analyses a P value <0·05 was considered statistically significant.
Results
Sample size was 490 (with a response rate of 82 %), of whom 34·5 % (n 169) were males. The sociodemographic profile of the study population is shown in Table 1.
Table 1 Demographic characteristics and BMI of the sample of Sri Lankan adults
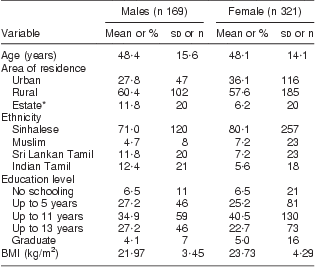
Data are presented as mean and standard deviation for age and BMI; otherwise as percentage and frequency.
*Tea and rubber plantation zones.
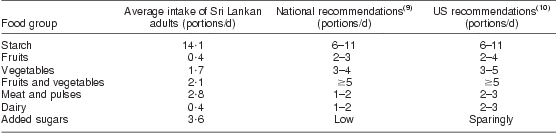
The estimated mean daily servings of the seven food groups from the random 24 h dietary recall, according to gender, are shown in Table 2. In addition, the combined categories of fruits and vegetables and meat and pulses are also reported. Mean daily intake of fruit (0·43) and vegetable (1·73) portions was well below minimum recommendations (fruits >2 portions/d; vegetables >3 portions/d). The total fruit and vegetable intake was 2·16 portions/d. Daily consumption of meat or alternatives was 1·75 portions and the sum of meat and pulses was 2·78 portions/d. On average, Sri Lankan adults consumed over 14 portions of starch/d; moreover, males consumed 5 more portions of cereal than females. Sri Lankan adults consumed on average 3·56 portions of added sugars/d. Table 3 compares the food consumption of Sri Lankan adults with national(9) and international (US) recommendations(10).
Table 2 Average dietary intake of different food groups (portions/d) among the sample of Sri Lankan adults
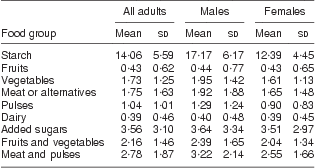
Table 3 Comparison of the average food intake of Sri Lankan adults with national and international recommendations
We identified considerable variations in consumption frequency for each food type and their portion size in the study population. Table 4 illustrates the distribution of participants according to the number of portions of the main food groups, and their combinations, consumed. Starchy foods were consumed by everybody; over 88 % met the minimum daily recommendations. Importantly, nearly 70 % of adults exceeded the maximum daily recommendation for starch (11 portions/d) and a considerable proportion consumed larger numbers of starch servings daily, particularly men. More than 12 % of men consumed ≥25 starch servings/d. In contrast to their starch consumption, participants reported very low intakes of other food groups (Table 4). Only 11·6 %, 2·1 % and 3·5 % of adults consumed the minimum daily recommended servings of vegetables, fruits and fruits and vegetables combined, respectively. Six out of ten adult Sri Lankans sampled did not consume any fruits. Milk and dairy consumption was extremely low; over a third of the population did not consume any dairy products and less than 1 % of adults consumed 2 portions of dairy/d. A quarter of Sri Lankans did not report consumption of meat and pulses. Regarding protein consumption, 36·2 % attained the minimum Sri Lankan recommendation for protein; and significantly more men than women achieved the recommendation of ≥3 servings of meat or alternatives daily (men 42·6 %, women 32·8 %; P < 0·05).
Table 4 Percentage distribution of the sample of Sri Lankan adults according to their consumption of food portions from different food groups

Discussion
Recently, the WHO STEP Survey reported on some dietary aspects from one health area in the Western Province(Reference Somatunga11) but, apart from this, the present study represents the first national-level dietary survey undertaken in Sri Lanka to obtain habitual dietary intake data of the general population. As the UK National Nutrition and Dietary Survey (NDNS) collected dietary details from 1724 participants from a population of 60 million, we believe that the sample size of 600 used in the current study is within adequate limits.
During the last 5 years, Sri Lanka has faced significant urbanization and this has resulted in some previous study clusters changing from rural to urban status. While the present study population is reasonably representative of all major ethnic groups in the country, there were higher proportions of urban living, aged and participants with a higher BMI compared with previous surveys(Reference Katulanda, Jayawardena and Sheriff12). Our results showed a low mean daily intake of fruits and vegetables among Sri Lankan adults (2·16 portions) compared with the USA (3·0) and France (3·6)(Reference Tamers, Agurs-Collins and Dodd13). The low intake of fruits and vegetables may be a contributing factor to the high prevalence of diet-associated NCD such as diabetes, non-alcoholic fatty liver disease and CVD in Sri Lanka compared with other countries(Reference Abeywardena3). The specific reason for the low intake of fruits and vegetables is unclear; studies from developed countries suggest a lack of perceived social pressure to increase fruit and vegetable intake and that increased public health efforts require stronger health messages that incorporate consumer awareness of the low consumption levels(Reference Levin14). Moreover, people's low purchasing ability and seasonal variation of fruit and vegetable prices may adversely affect consumption. Despite five servings of fruits and vegetables being considered the minimum daily intake by national dietary guidelines(9), nearly half of the population eats less than two portions of fruits and vegetables daily, with less than 4 % reaching the minimum recommendation. Somatunga reported that 96·9 % of Sri Lankan adults did not consume five fruits and vegetables daily in the WHO STEP Survey (2004) undertaken in the Western Province of Sri Lanka, comparable to our findings(Reference Somatunga11).
Pulses were the main source of protein, mainly as dhal, the most common curry in the local context, and boiled pulses eaten for breakfast. Although pulses are grouped in the protein category, the main nutrient is carbohydrate, and thus invariably consumption of pulses masks significant amounts of carbohydrate. There is no conclusive evidence regarding protein intake and disease risk in Sri Lanka. The MASALA (Metabolic Syndrome and Atherosclerosis in South Asians Living in America) Study reported that higher levels of protein consumption are associated with increased odds of diabetes in South Asians independent of age, sex, waist circumference and hypertension(Reference Wang, de Koning and Kanaya15). A significant proportion of Sri Lankan males (data not shown) consumed over 5 servings of meat/d.
Sri Lankans consumed large numbers of starch servings; nearly 65 % consumed well above the upper cut-off of the recommendations (food pyramid guidelines) and a considerable proportion of males consumed very high levels of starch. This is mainly due to the average person's meal comprising three-quarters rice with a small amount of vegetable curry (averaging 15 g), a small piece of meat or fish (15 g) and some starchy curry such as potato or dhal (see Supplementary Materials, Part 2). Relatively low levels of starch portions were consumed by females mainly due to low absolute food intake. A high-carbohydrate meal leads to negative metabolic consequences such as hyperinsulinaemia, high serum TAG and low HDL-cholesterol levels(Reference Misra, Khurana and Isharwal16). Most Sri Lankans consume the largest starch portion for lunch or dinner and limit themselves to three meals per day (data not shown), which may cause postprandial hyperglycaemia and hypertriacylglycerolaemia(Reference Misra, Khurana and Isharwal16). More than a fifth of Sri Lankan adults are dysglycaemic and the prevalence of diabetes is alarmingly high(Reference Katulanda, Constantine and Mahesh2); the high consumption of carbohydrate may be associated with the diabetes epidemic in the country.
Dairy products provide valuable nutrients such as Ca, which is important for building and maintaining strong bones. In addition, milk products provide several essential nutrients such as proteins, vitamins and minerals. Lekamwasam and colleagues reported a 45 % prevalence of osteoporosis among postmenopausal women in Sri Lanka(Reference Lekamwasam, Wijayaratne and Rodrigo17). The CARDIA (Coronary Artery Risk Development in Young Adults) Study revealed that dairy consumption was inversely associated with the incidence of all individual components of insulin resistance syndrome among individuals with a BMI≥25 kg/m2 and increased dairy consumption may reduce risk of type 2 diabetes and CVD(Reference Pereira, Jacobs and Van Horn18). Dairy intake in the present sample was substantially lower than Sri Lankan recommendations; over a third of the population did not consume any dairy products and only 5 % reached minimum levels. The main reason behind the low dairy consumption could be that dairy products are unaffordable; their price is high mainly due to the lack of local production and their consumption depends largely on imported milk powder(19).
This first national-level dietary survey provides a sound basis for future food policy as it affects Sri Lankan adults and for the development of relevant nutrition education programmes. Furthermore, the rational assessment of food portion exchange tables will offer health professionals, such as nutritionists, general practitioners and nurses, valuable insights into Sri Lankan meals and aid the development and prescription of meal plans in clinical and community settings. A major strength of our study was the recruitment of a representative group from all ethnic, education, areas of residence and age groups. Despite the relatively low participation of male participants, women's diet composition is similar to that of their male counterparts as most Sri Lankan men eat at home. Second, the use of a random 24 h dietary recall method helped to obtain accurate results regarding dietary habits. While a single day's food record cannot be used to generalize an individual's usual diet, 24 h recall data can provide estimates of group means. Third, disaggregation of food in Sri Lankan dishes into guideline-based food groups leads to the more accurate counting of small portions of foods in respective groups (as shown in Fig. 1). The main limitation of our data collection and analysis was the lack of data on oil consumption. Unlike meals in Western countries, coconut oil, coconut milk or scraped coconuts are included in most mixed dishes, which leads to significant methodological challenges in obtaining accurate measurements of fat intake(Reference Amarasiri and Dissanayake20). Second, portion sizes were estimated by recalling commonly used utensils and demonstrating standard spoons, cups and plates, in addition to series of food photographs.
Conclusions
Dietary guidelines have emphasized the importance of a balanced and varied diet. Meals that include no servings or very few servings of different food groups such as fruits and vegetables, dairy products, fish and meat and pulses, lack both balance and variety. It is evident that a substantial proportion of the Sri Lankan population does not consume a varied and balanced diet, which is suggestive of a close association between the nutrition-related NCD in the country and these unhealthy eating habits. We recommend that government, health institutions and organizations conduct larger national-level dietary and nutrition surveys periodically to identify associated disease conditions. This would allow practical public health initiatives to improve the quality of the Sri Lankan diet.
Acknowledgements
This research received no specific grant from any funding agency in the public, commercial or not-for-profit sectors. The authors declare that they have no conflicts of interest. R.J. contributed to the data collection, data analysis and drafted the manuscript. N.M.B., M.J.S., P.K. and A.P.H. were the supervisory team on the project and contributed to the study design, data interpretation and revision of the manuscript. All authors read and approved the final manuscript. The authors would like to acknowledge Miss Fathima Shakira and other members in the Diabetes Research Unit, Colombo, for their contribution in arranging logistics for the study. The authors also thank Dr Senarath Mahamithawa (Deputy Director – Nutrition, Ministry of Health, Sri Lanka), Mrs Thakshila Adikari (Head, Department of Applied Nutrition, Wayamba University of Sri Lanka) and Miss Jyh Eiin Wong (Public Health Nutritionist, Department of Human Nutrition, University of Otago) for their input on data interpretation and expert comments.
Supplementary Materials
For Supplementary Materials for this article, please visit http://dx.doi.org/10.1017/S1368980012003011







