The last decade has witnessed a surge in interest and research activity relating to the development of public health nutrition as a practice area and public health nutrition workforce development(Reference Hughes1–Reference Steyn and Mbhenyane5). Workforce development is a central strategy required to build capacity in individuals, organisations, health services and populations to effectively address nutrition issues(Reference Baillie, Bjarnholt and Gruber6). Workforce capacity is influenced by a range of determinants including workforce size, the quality of workforce preparation, continuing professional development, organisation and support(Reference Hughes1). As a consequence, workforce development requires multiple strategies and approaches that focus on determinants of workforce capacity.
In Australia, there has been a decade-old national mandate for workforce development to build capacity to deliver on a national public health nutrition strategy (Eat Well Australia)(7). This national strategy has been embraced by some, but not all, state government health systems to the point that they have developed state-level public health nutrition strategies(8, 9) that largely reflect the national agenda. In Australia, public health system workforces are developed, managed and supported by state governments rather than at a national level. As a result, the public health nutrition workforce has developed rapidly in some states(Reference Lee10) and has stagnated in others, as a result of differences in state-level systems and variable implementation of the national and state public health nutrition strategy agendas.
The Australian public health nutrition workforce for the last decade has been largely based on, and developed by, practitioners with nutrition and dietetic qualifications and few with formal postgraduate qualifications in public health(Reference Hughes11). This workforce has previously recognised the specific inadequacies of this preparation(Reference Hughes12) and the need for continuing professional development once in the work environment(Reference Hughes13). Public health nutrition as a mode of practice in Australia has and continues to evolve from community-based service delivery by dietitians(Reference Hughes14) to work functions that better reflect the core functions of public health(Reference Laurence and Worsley15). This practice reorientation requires workforce reorganisation and the development of new competencies among practitioners(Reference Hughes16).
Despite the central role of competency standards as the architecture for workforce development(Reference Hughes16) and the apparent consensus about the competencies required for effective public health nutrition practice(Reference Hughes17), there is a dearth of scholarship about how and when these competencies develop. Similarly, little published research to date has addressed the strategic questions of how best to build the existing workforce capacity, or measured the effectiveness of workforce development interventions that focus on competence development in the period following graduation and entry to the work environment. This period has been identified as a critical stage in public health nutritionist competence development, with exposure to a mentor/s and learning in a network of practitioner colleagues (teams) identified as key determinants of competence development among advanced-level public health nutritionists in Australia(Reference Hughes18, Reference Palermo and McCall19).
The present study aimed to evaluate a workforce development intervention for novice public health nutritionists based on a mentoring circle, a mix of mentoring and learning circle strategies, which was designed to enhance workforce capacity by facilitating and expediting public health nutrition competence development and practice reorientation.
Methods
Design
A retrospective post-intervention qualitative interview evaluation study was used to investigate the mentoring experience of participants(Reference Yin20, Reference Liamputtong21). Ethical approval was obtained from the relevant university human research ethics committee.
Recruitment
Purposive sampling using existing professional networks was used to recruit dietitians who were novice public health nutrition practitioners, employed in Victoria, with a component of their current work role, as defined by their job descriptions, in public health or community nutrition. Recruitment was via invitation with participants expressing an interest in participating in the intervention (self-selecting).
The mentoring circle
Mentoring has previously been proposed as a public health nutrition workforce development strategy(Reference Battams22), identified as a key determinant of competence development among advanced-level public health nutritionists(Reference Hughes18, Reference Palermo and McCall19) and is a common framework used for professional development in health professionals(Reference Morton-Cooper and Palmer23). A mentoring circle intervention (mix of mentoring and peer-group learning strategies) was selected as the practice improvement system in the present study to maximise mentor to mentee exposure and facilitate peer mentoring(Reference Darwin and Palmer24). Mentoring circles involve a mentor and a small group of colleagues who come together to support each other’s learning through the provision of effective feedback and advice(Reference Darwin and Palmer24, Reference Collay, Dunlap and Enloe25). The mentoring circle was led by the mentor (lead author – a public health nutritionist educator with experience in mentoring) and involved small groups of newly graduated dietitians working in public health and community nutrition practice settings.
Participants self-selected to one of three mentoring circles. Two face-to-face mentoring groups were conducted in two different metropolitan locations (Clayton and Melbourne) and participants from rural or regional areas were allocated to an electronic (video link) mentoring group for convenience and to enable a comparison of electronic communication compared to the face-to-face experience of the mentoring circle intervention. The mentoring circles were conducted every six weeks, for 2 h, over a 7-month intervention period.
Upon commencement, the participants were required to develop an individual learning plan, equivalent to a personal and professional development plan that used previously identified core competencies for public health nutrition practice(Reference Hughes17). The competencies were adapted to reflect the work roles of the participants and used to focus learning plan objectives. Learning plans included an explicit codification of competency elements to be developed, learning objectives, activities and an ongoing reflection of progress relevant to the practice issue. At each mentoring circle meeting, the participants used this learning plan to reflect and measure their progress or development and to discuss issues and experiences within the mentor circle peer group. The group discussions were facilitated by the mentor who used an appreciative enquiry framework to guide communication. Appreciative enquiry focuses on positive interactions to identify solutions(Reference Cooperrider, Whitney and Stavros26). Discussions focused on supporting reorientation of practice towards population-based prevention and a range of public health practice areas including policy development, capacity building and programme planning consistent with gaps in competence previously identified by this workforce(Reference Hughes13).
In-depth interviews
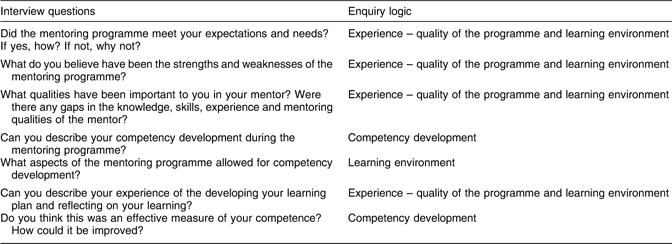
All participants were invited to partake in an in-depth interview that aimed to describe their experience of participating in the mentoring intervention. In-depth interviews were used to provide interpretation to the participant’s individual experience while reducing the influence of other participants(Reference Liamputtong21). An independent research assistant undertook the interviews to allow the participants the opportunity to speak freely about their experience of the intervention and the mentor and reduce acquiescence bias. Face-to-face interviews were conducted when possible and phone interviews were conducted when practically required. Interview questions were designed to elicit the participant’s experience of the learning environments during the mentoring intervention. The enquiry logic underpinning the evaluative interviews is summarised in Table 1. All participants gave permission to have their interviews audio-recorded, and written notes were also taken. Interviews lasted approximately 30 min and recordings of interviews were transcribed verbatim.
Table 1 Interview questions and enquiry logic, mentoring circle post-intervention interviews
Analysis
Basic descriptive statistics (Microsoft Excel 2003; Microsoft Corp., Redmond, WA, USA) were used to analyse demographic data. Qualitative data were managed using NVivo8 (QSR International, Doncaster, VIC, Australia). Data from interviews were analysed using a thematic analysis approach with a phenomenological lens focusing on the experience of participants in the mentoring circle intervention. Open coding was undertaken without the use of or reference to pre-established codes and a code list was created(Reference Huberman and Miles27). Codes were then grouped into categories. All authors independently analysed the data to assist in validating the findings. The key categories were then summarised and interpreted by the authors into themes and narrative scripts selected to represent these themes. An assessment of any difference in the experience of face-to-face compared to video-linked mentoring as well as urban and rural dietitians’ experience was conducted as part of the analysis.
Results and discussion
All thirty-two participants who commenced the mentoring circle completed 7 months of mentoring (Table 2). The majority (n 26, 81 %) of the participants had entered a career in community or public health nutrition directly upon graduation, had a mean length of practice experience <2 years and most (n 20, 63 %) were working within their first place of employment. These attributes reflect novice practitioners working in mixed service community-based roles (clinical and public health), reflective of much of the Australian public health nutrition workforce(Reference Hughes14).
Table 2 Demographics of mentoring circle participants

MPH, Master of Public Health; CH, community health; RH, rural health; PH, population health.
*Completed MPH during the 7-month programme.
All thirty-two participants completed the in-depth interview. Twenty-two interviews were conducted face-to-face and ten were conducted by telephone. The data revealed three key theme groupings related to the intervention experience and a number of interrelated sub-themes (Table 3). There was no difference in the volume or complexity of transcript data obtained from face-to-face v. telephone, consistent with what has been found in other studies(Reference Sturges and Hanrahan28).
Table 3 Qualitative evaluation themes and descriptors

Process, structure and function of the intervention
The participants reported that the group setting provided an effective means for learning that was potentially more effective than one-to-one mentoring due to the ability to network, share practice experiences and explore ideas in-depth. The participants explained that sharing of issues, ideas and strategies by drawing on each other’s experience and problem solving together increased the participant’s confidence and ability to deal with challenges in their work roles.
…having a group of [us] all together, for support…. Often in a hospital you’ll have a bigger team but in community health you can feel really isolated, so just that support was really good, and then I guess the fact that people were able to bring up an issue … something that was working in their workplace, and the whole team would discuss it so you could get extra ideas, and support through that, which was really good.
(Participant 3)
The participants reported that they valued the opportunity to engage in peer mentoring as it allowed them to contribute to others’ learning and problem solving rather than just being a recipient. The participants reported the importance of being able to access and utilise the mentor in a one-to-one relationship in addition to the group. The relationships developed as part of the group process, which facilitated additional networks in the field and the participants reported utilising these networks both inside and outside the group setting.
I thought it was really valuable being able to get together with a whole group of people and just talk through what everyone’s doing and having that person you can go up and ask questions of, that’s not to do with your work. I’ve already contacted others outside the group about a project they were involved in.
(Participant 29)
The participants reported that the group size (averaging eight participants per group) and frequency of contact were generally appropriate, although a few reported that a smaller group would have provided greater opportunity to contribute to discussion, problem solving and individual learning.
I think that maybe if it was a smaller size group there would have been more opportunities … to share … you can’t get everyone talking … and you really want to do something properly…you don’t want to give someone just ten minutes and … move to someone else.
(Participant 14)
A common recommendation from the participants was that the intervention period should have been extended for a longer period of time due to the nature of public health action taking longer to achieve than the 7-month intervention period.
I think longer, I think twelve months would be better… I think we would get more achieved ’cause there’s longer time to work on the goals.
(Participant 1)
The participants acknowledged that group dynamics and certain personalities within groups created challenges for mentoring circle operation and recognised that this will always be an issue when working in a group setting.
the group dynamics, there are all these people who are bigger talkers than others and who might dominate discussion quite a bit… that was a bit of a weakness, but then again that’s people… I don’t think it’s something you can do much about but I mention it I suppose because it detracted from what I was able to do.
(Participant 31)
The group make-up was felt to be appropriate by most of the participants being a relatively homogeneous mix of practice novices with similar levels of experience and work roles. However, the participants in the two metropolitan groups reported that there were some mismatches within the groups, with participants in full-time public health or community nutrition roles not feeling that the group discussions reflected these issues and challenges described by practitioners who had mixed-service roles and worked effectively part-time in public health nutrition. This issue was not reported by the rural group who reported great similarity within work roles.
…other people only have a few hours a week to do health promotion and so the issues and barriers that they brought to the table were completely different from my own… often about how to advocate for more health promotion hours or … how to get health promotion done in two hours a week …. that’s not sort of an issue I faced.
(Participant 31)
The advanced-level public health nutrition competencies embedded into a learning plan was viewed by the participants as effective in supporting advanced-level practice and as a measure of achievements. The public health nutrition core competencies were new to the participants, and were initially challenging to work but provided a useful, although initially daunting, framework and structure for focusing and reflecting on their learning goals. The learning plan, based on these competencies, was reported by the participants to be an effective tool to structure learning and development and facilitate and teach reflective practice.
…the actual template and things that we had to fill out were relatively straightforward it was really just getting your mind into the idea of what they were talking about initially… having to reflect on those goals and activities that you did really made you actually much more consciously think about the process and put a lot more thought into what you were doing and how you felt about it …. which I think … enhances your learning and indirectly means that hopefully next time you get better at that competency and you feel more confident.
(Participant 25)
These findings on the process, structure and function of the group are in line with adult learning principles as described by Knowles et al.(Reference Knowles, Holton and Swanson29). By asking participants to individually identify what they wanted to learn and why they needed to learn it, and then developing self-directed learning plans, or how they would learn the new knowledge or skill, taps into adult learning. The programme was self-selecting, recruiting only those with a motivation to develop, and was based on learning in the context of their work environments being problem-oriented and contextual(Reference Knowles, Holton and Swanson29). What was unique about the findings was the strong preference and effect of the group mentoring model, which facilitated networking and peer mentoring. This model of mentoring has the potential to increase coverage, reduce reliance and burden on mentors and support a culture of mentoring in a profession. The learning plan provided a useful framework to focus and structure learning and these findings support other work that supports the potential role of portfolio-based learning in developing professional practice(Reference Pitts30). The learning plan could be considered as part of a professional portfolio that includes a collection of material that provides evidence of learning and identifies future learning needs and opportunities(Reference Tochel, Haig and Hesketh31). Qualitative portfolios of evidence have been suggested as an effective means of facilitating and reliably assessing practice improvement(Reference Tochel, Haig and Hesketh31).
Safe and supportive learning environment
The environment in the group setting was reported by participants to be safe, secure and comfortable, and the face-to-face nature of the learning environment (even via electronic video link) reportedly enabled learning. The participants reported that the other groups they attend, which are larger and more diverse in membership, are not conducive to sharing or learning as they feel unable to talk in that daunting environment. The rural participants acknowledged that it was important to have met the mentor face-to-face before participating in video-linked discussions but reported no other disadvantages to participating in the mentoring via a video link.
considering I was five hours from Melbourne I felt like I was still supported and not forgotten, which is …what tends to happen with rural stuff.
(Participant 17)
The relationship between the mentor and all participants was viewed by the participants as strong and supportive of their development and this was due to a range of important qualities of the mentor. In referring to the role of the mentor in the programme, the participants reported the importance of having a mentor who is experienced, particularly in the areas they are working, but not so experienced that they could not relate to the participants. The mentor must be approachable, available and accessible to mentees and support a culture of trust and respect in the relationship. The ability to provide effective feedback is important. A friendly, warm and positive personality was reported as important and the mentor needs to be a role model who has a passion for public health and community nutrition. The mentor must have the ability to effectively facilitate a group, inspire and support creative thinking and learning through an equal relationship. These qualities were consistently reported by all participants and met their expectations of the mentor in the programme.
She’s lots of fun and that’s what makes it realistic as well … it’s not just her telling you, this is the way it should be done or you’re doing it wrong. …. She has a way of sort of saying things positively but with a negative spin on it, or making you question all the time which is really good, it makes you think outside of the square.
(Participant 30)
These results indicated that the mentoring circle and the mentor’s attributes and approach created a safe and supportive learning environment, which has been consistently documented in the literature as a key element required to ensure that learning takes place in small groups(Reference Jaques32). The qualities of the mentor reported by the participants in the present study are not unique and are comparable to those reported across the mentoring literature(Reference Morton-Cooper and Palmer23, Reference Walker, Kelly and Hume33). The important quality to note of the mentor in this study is the ability to facilitate group learning through an equal relationship. Traditional mentoring models are based on a much older and wiser mentor developing a partnership with a junior colleague(Reference Morton-Cooper and Palmer23). This programme used a mentor with only 6–10 years more experience than the participants in the programme. The teaching philosophy, experience and style of the mentor supported the collegial relationship and the focus of discussions supported a positive problem-solving culture within the group.
The phases of the mentoring relationship have been documented as initiation (establishment), cultivation (development), separation (change) and redefining (evaluation)(Reference Morton-Cooper and Palmer23). Effective mentoring relationships must have attraction (inspiration), action (investment) and affect (support)(Reference Walker, Kelly and Hume33). These data provide evidence of elements of these phases and components; however, they also demonstrate that mentoring relationships are not exact or linear and cannot be construed for professional development purposes. The personal qualities and professional skills and experience of the mentor are fundamental to successful relationships. These findings provide evidence to recommend that future mentoring programmes may need to ensure that mentors have appropriate teaching and learning skills together with the experience and expertise in the practice area.
Practice-based learning environment
The participants consistently acknowledged the important role of learning on the job or by experience.
On-the-job experience is really important. I find that if I learn things that are relevant to what I am doing at the time obviously it really sinks in and it’s a lot more useful that if you just try and learn things for the sake of it.
(Participant 22)
They described that the value of this learning was enhanced through reflective practice facilitated by mentoring. They acknowledged that they would have learnt as they progressed in their practice independent of the mentoring, but described the additional value in taking the time out to undertake reflective practice that was facilitated by mentoring.
I think reflection is pretty powerful in that sense of building up your capacities. …. sitting back and actually being able to be reflective you learn a lot about yourself and where your strengths are.
(Participant 11)
Participation in mentoring circle sessions varied between groups and individual participants, reflecting a range of participation barriers, most common of which was relative time poverty and the competing priorities of client or direct care work and personal or workplace issues. There were a range of workplace factors that influenced the participants’ ability to contribute to the programme and learn. Many of the participants experienced change in positions and/or organisations and/or role and responsibilities during the period of the programme and they reported frustrations in working in these constantly changing environments. This staffing turnover and role instability is a feature of the community and public health nutrition workforce in Australia(Reference Hughes11). The competing priorities of client or direct care work for some of the participants were a barrier to progressing through the tasks assigned in the mentoring circle process in the allocated time frame.
You always feel like you are under so much pressure to get things done and say yes to more things … you’re so busy, I just really struggled to actually, you know I had the time booked aside in my diary but things would come up or something would go wrong.
(Participant 4)
The role of experiential learning in competence development in public health nutrition had been previously identified(Reference Hughes18, Reference Palermo and McCall19). These results suggest that mentoring combined with practical, on-the-job experience facilitates reflective practice and thus has the potential to improve practice beyond what would be learnt independently. Barriers to on-the-job learning were predominantly related to workplace organisational issues and workplace time poverty. A previous study has acknowledged that workforce development strategies, such as mentoring, will be ineffective if there is no matching managerial support and strategies that free up staff time to upskill and reorientate practice, such as investment in increasing the workforce size and creating organisational mandates for work in public health nutrition(Reference Hughes and Woods34). The time to participate in the programme as part of on-the-job learning was a key determinant and consistent with the literature that describes time as one of the key factors impacting the success of relationships(Reference Johnson, Settimi and Rogers35, Reference Launer36). Organisations have a role in supporting employees’ learning through experience by allowing them time to dedicate to mentoring.
Conclusion
This qualitative evaluation of a workforce development intervention provides evidence of the utility of mentoring circle interventions to build up the capacity of the public health nutrition workforce, particularly in health systems reflecting the mixed-role function of novice public health nutritionists. The mentoring intervention provided and facilitated effective environments for learning. The process, structure and functioning of the mentoring circle and the safe and supportive environment for learning, facilitated by the mentor were viewed as important in contributing to the development of the participants. The learning plan, based on experiential learning, and the advanced-level public health nutrition competencies and reflective practice framework were generally considered to be effective in guiding learning. In addition, the participants recognised the importance of learning within the workplace environment to support their development but articulated a range of barriers within this environment. Mentoring circles may be an effective approach for the development of the public health nutrition workforce. This research provides evidence and guidance for those considering mentoring strategies for public health nutrition workforce development.
Acknowledgements
The present study received no specific grant from any funding agency in the public, commercial or not-for-profit sectors. The authors declare no conflict of interest. C.P., R.H. and L.M.C. designed the intervention and analysed the data. C.P. led the study and supported the collection of data. C.P. and R.H. drafted the manuscript and L.M.C. reviewed the drafts.





