Mental illness often constitutes a double jeopardy for those affected because of stigmatisation by members of the community (Reference Corrigan and WatsonCorrigan & Watson, 2002). Studies conducted in North America and western Europe suggest that stigma is a major problem in the community (Reference Taylor and DearTaylor & Dear, 1980; Reference Brockington, Hall and LevingsBrockington et al, 1993; Reference HuxleyHuxley, 1993; Reference Jorm, Korten and JacombJorm et al, 1999; Reference Crisp, Gelder and RixCrisp et al, 2000). Negative views such as those implying that people with mental illness are irresponsible and therefore incapable of making their own decisions, or are dangerous and are to be feared, are widespread. Since negative beliefs often lead to discrimination, there is little wonder that studies have also shown that people with mental health problems living in the community experience rampant harassment (Reference Kelly and McKennaKelly & McKenna, 1997; Reference Berzins, Petch and AtkinsonBerzins et al, 2003). Some studies conducted in Africa have suggested that the experience of stigma by people with mental illness may be common (Reference Awaritefe and EbieAwaritefe & Ebie, 1975; Reference Shibre, Negash and KullgrenShibre et al, 2001), but there is no information on how widespread negative attitudes to mental illness may be in the community. As noted by Corrigan & Watson (Reference Corrigan and Watson2002), it is unclear whether the lack of empirical data partly explains the speculation that stigmatisation of mental illness may be less common among Africans (Reference FabregaFabrega, 1991).
METHOD
Sample characteristics
The survey was conducted in three Yoruba-speaking states in south-western Nigeria (Ogun, Oyo and Osun) between March and August 2002. The survey on stigma was a segment of a much larger survey of mental disorders in the community (the Nigeria Survey of Mental Health and Well-being) and was administered by trained lay interviewers from the Department of Psychiatry, University of Ibadan. Both studies were approved by the University of Ibadan and University College Hospital joint ethics committee.
The study was based on a stratified, multistage clustered probability sample of household residents aged 18 years or older in the selected states. First, stratification was based on states (three categories) and size of the primary stage units, which were the local government areas (two categories). The second stage was to select two primary stage units per stratum, with probability of selection proportional to size. The third stage was the random selection of four enumeration areas from each local government area; these are geographical units demarcated by the National Population Commission, each consisting of about 60–80 household units. We enumerated the households in each selected area and randomly selected the number of households required to meet our desired sample size. One resident aged 18 years or over was approached for participation in each selected household. We used the Kish method to identify the potential respondent (Reference KishKish, 1995) and no replacement was made for refusals. A total of 2040 persons participated in the survey on stigma, representing a response rate of 74.2%. The results presented here have been weighed to reflect the within-household probability of selection and to incorporate a post-stratification adjustment such that the sample is representative of the age by gender distribution of the projected population of Nigeria in 2000.
Income was categorised into four groups: ‘low’ (defined as less than or equal to median or the pre-tax income per household), ‘low average’ (greater than ‘low’ up to twice the median value), ‘high average’ (greater than ‘low average’ up to three times median value) and ‘high’ (greater than ‘high average’). Residence was classified as rural (fewer than 12 000 households), semi-urban (12 000–20 000 households per local government area) and urban (more than 20 000 households).
Assessment
A modified version of the questionnaire developed for the World Psychiatric Association Programme to Reduce Stigma and Discrimination Because of Schizophrenia was used (Reference Stuart and Arboleda-FlorezStuart & Arborleda-Florez, 2001; World Psychiatric Association, 2002). The questionnaire is focused mainly on knowledge of and attitude to schizophrenia. It was modified largely to take account of the focus of this survey, which was on mental illness rather than schizophrenia. Thus, in addition to substituting the term ‘mental illness’ for ‘schizophrenia’, specific items relating to the symptoms of schizophrenia were deleted. The questionnaire was translated into Yoruba by a panel of four bilingual mental health research workers using the iterative back-translation method. In the translation, particular care was made to convey a broad idea of ‘mental illness’ (arun opolo), differentiating it from psychosis (iwin or were) and mental retardation (ode or odoyo).
Analysis
Simple cross-tabulations were used to calculate proportions and their distributions in different groups. To take account of the sampling procedure, with clustering and weighting of cases, standard errors of proportions were estimated with the jackknife method implemented in the STATA software (StataCorp, 2001). Statistical significance was evaluated at the 0.5 level and was based on two-sided design-based tests.
RESULTS
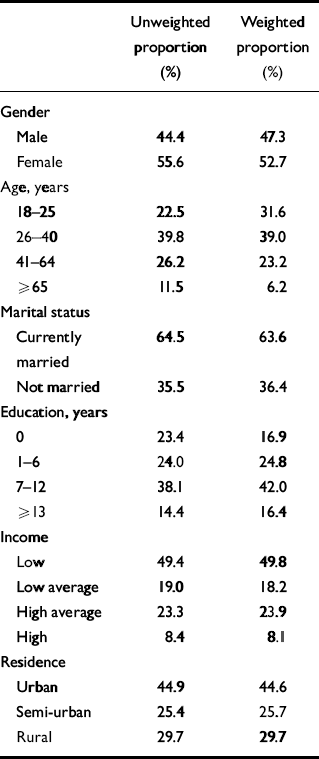
Table 1 shows the socio-demographic attributes of the sample. In keeping with the demographic and economic profile of Nigeria, the sample was predominantly young and most came from low or low average income households. The population of Nigeria is predominantly rural, but the south-western area where the study was conducted is more urban than the rest of the country and this is reflected in the table.
Table 1 Demographic profile of the sample (unweighted n=2040)
| Unweighted proportion (%) | Weighted proportion (%) | |
|---|---|---|
| Gender | ||
| Male | 44.4 | 47.3 |
| Female | 55.6 | 52.7 |
| Age, years | ||
| 18-25 | 22.5 | 31.6 |
| 26-40 | 39.8 | 39.0 |
| 41-64 | 26.2 | 23.2 |
| ≥ 65 | 11.5 | 6.2 |
| Marital status | ||
| Currently | 64.5 | 63.6 |
| married | ||
| Not married | 35.5 | 36.4 |
| Education, years | ||
| 0 | 23.4 | 16.9 |
| 1-6 | 24.0 | 24.8 |
| 7-12 | 38.1 | 42.0 |
| ≥ 13 | 14.4 | 16.4 |
| Income | ||
| Low | 49.4 | 49.8 |
| Low average | 19.0 | 18.2 |
| High average | 23.3 | 23.9 |
| High | 8.4 | 8.1 |
| Residence | ||
| Urban | 44.9 | 44.6 |
| Semi-urban | 25.4 | 25.7 |
| Rural | 29.7 | 29.7 |
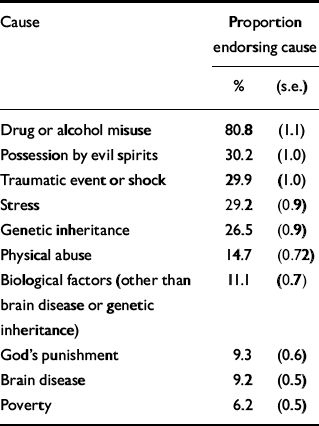
Most respondents expressed the view that substance misuse (alcohol or drugs, but mainly the latter) could result in mental illness (Table 2). The next most commonly endorsed cause of mental illness was a belief that it could be due to possession by evil spirits. Following this, trauma, stress and heredity were about equally ascribed as possible causes. Only about one in ten respondents believed that biological factors or brain disease could be the cause of mental illness. Confirming a stronger belief in supernatural causation, over 9% thought mental illness could result from punishment from God, whereas only about 6% thought poverty could cause mental illness.
Table 2 Ten most commonly reported causes of mental illness (weighted n=1661)
| Cause | Proportion endorsing cause | |
|---|---|---|
| % | (s.e.) | |
| Drug or alcohol misuse | 80.8 | (1.1) |
| Possession by evil spirits | 30.2 | (1.0) |
| Traumatic event or shock | 29.9 | (1.0) |
| Stress | 29.2 | (0.9) |
| Genetic inheritance | 26.5 | (0.9) |
| Physical abuse | 14.7 | (0.72) |
| Biological factors (other than brain disease or genetic inheritance) | 11.1 | (0.7) |
| God's punishment | 9.3 | (0.6) |
| Brain disease | 9.2 | (0.5) |
| Poverty | 6.2 | (0.5) |
The views about mental illness were generally negative (Table 3). People with mental illness were believed to be mentally retarded, to be a public nuisance and to be dangerous. Less than half of the respondents believed that such people could be treated outside hospital and only about one-quarter thought they could work in regular jobs. Poor knowledge about mental illness seemed to pervade all segments of the community: no consistent association was observed between the predominantly negative views of mental illness on the one hand and gender, age, education, income or residence on the other hand.
Table 3 Views of respondents about people with mental illness

| Item | Overall | Proportion endorsing item, % (s.e.) | ||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Gender | Age group, years | Education years | Household income1 | Urbanicity | ||||||||||||||
| Male | Female | 18-25 | 26-40 | 41-64 | ≥ 65 | 0 | 1-6 | 7-12 | ≥ 13 | L | LA | HA | H | Urban | Semi-urban | Rural | ||
| Can be treated outside hospital | 45.0 (1.4) | 42.6 | 47.2 | 42.6 | 45.9 | 45.7 | 49.2 | 49.1 | 43.1 | 45.5 | 42.4 | 44.3 | 49.3 | 42.6 | 48.1 | 48.4 | 43.7 | 41.1 |
| (2.1) | (1.8) | (2.3) | (2.2) | (3.0) | (5.5) | (3.4) | (3.5) | (1.7) | (3.2) | (1.7) | (2.3) | (3.4) | (4.6) | (2.7) | (2.8) | (2.4) | ||
| χ2=4.34, P=0.10 | χ2=2.611, P=0.60 | χ2=3.87, P=0.49 | χ2=4.38, P=0.32 | χ2=7.93, P=0.16 | ||||||||||||||
| Tend to be mentally retarded | 91.5 (0.8) | 90.5 | 92.4 | 93.0 | 90.6 | 91.5 | 89.5 | 92.8 | 90.2 | 92.1 | 90.4 | 92.4 | 91.1 | 90.5 | 91.6 | 90.8 | 92.3 | 91.7 |
| (1.2) | (1.1) | (1.8) | (1.0) | (1.3) | (3.4) | (1.7) | (1.5) | (1.0) | (2.1) | (1.2) | (1.8) | (1.8) | (2.2) | (0.9) | (1.8) | (1.6) | ||
| χ2=2.37, P=0.29 | χ2=3.26, P=0.54 | χ2=2.50, P=0.58 | χ2=1.52, P=0.77 | χ2=1.04, P=0.76 | ||||||||||||||
| Are a public nuisance | 95.2 (0.6) | 95.5 | 95.0 | 92.7 | 95.8 | 97.5 | 96.4 | 96.9 | 93.0 | 96.7 | 93.1 | 95.1 | 93.9 | 97.3 | 92.6 | 94.1 | 96.1 | 96.2 |
| (0.8) | (0.9) | (1.2) | (1.1) | (0.8) | (1.1) | (1.1) | (1.5) | (0.7) | (2.0) | (1.0) | (1.4) | (1.2) | (3.0) | (1.2) | (1.4) | (0.7) | ||
| χ2=0.36, P=0.62 | χ2=14.45, P<0.03 | χ2=14.29, P<0.05 | χ2=7.97, P=0.28 | χ2=4.46, P=0.30 | ||||||||||||||
| Can work in regular jobs | 25.5 (0.8) | 26.7 | 24.3 | 22.6 | 28.4 | 24.7 | 24.5 | 28.0 | 20.3 | 27.2 | 27.0 | 26.6 | 17.5 | 26.6 | 32.8 | 25.0 | 22.1 | 29.3 |
| (1.5) | (1.5) | (2.8) | (1.6) | (1.9) | (3.3) | (2.8) | (1.6) | (1.9) | (3.3) | (1.7) | (2.4) | (1.3) | (4.3) | (1.4) | (2.3) | (1.7) | ||
| χ2=1.47, P=0.35 | χ2=9.52, P=0.12 | χ2=9.52, P=0.12 | χ2=17.21, P<0.01 | χ2=7.50, P=0.06 | ||||||||||||||
| Are dangerous because of violent behaviour | 96.5 (0.5) | 95.6 | 97.2 | 96.1 | 96.2 | 97.3 | 96.8 | 97.8 | 96.6 | 95.7 | 96.9 | 97.2 | 96.7 | 96.0 | 93.1 | 95.9 | 97.3 | 96.7 |
| (0.9) | (0.6) | (1.2) | (0.7) | (0.7) | (1.1) | (0.9) | (1.0) | (1.0) | (1.2) | (0.8) | (1.0) | (1.3) | (2.0) | (0.9) | (1.1) | (0.7) | ||
| χ2=3.55, P=0.14 | χ2=1.44, P=0.62 | χ2=3.23, P=0.55 | χ2=7.10, P=0.20 | χ2=1.98, P=0.54 | ||||||||||||||
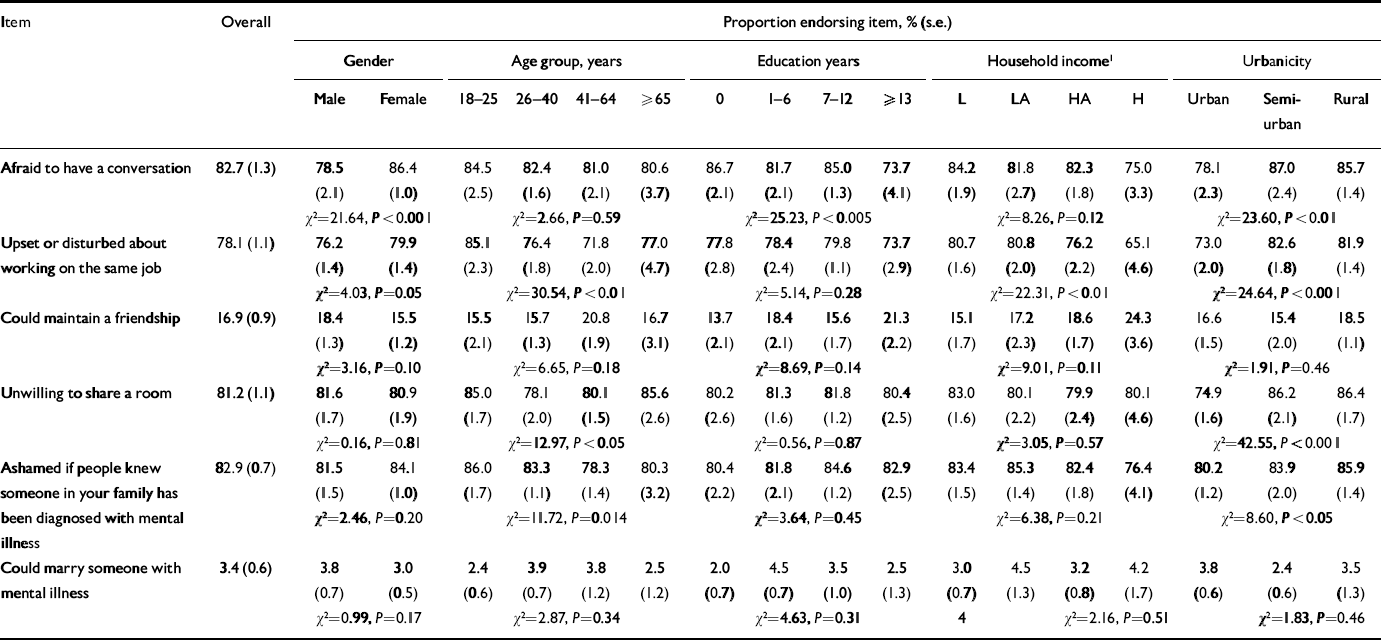
Table 4 shows that most respondents were unwilling to have social interactions with someone with mental illness. Most would be afraid to have a conversation and would be disturbed to work with a person with mental illness. Only a few would be willing to maintain a friendship and fewer still would consider marrying such a person. There were also inconsistent associations of socio-demographic attributes with negative attitudes to mental illness. As shown in Table 4, apart from evidence of a somewhat more liberal attitude of men and those residing in urban areas, negative attitude to mental illness seems to be highly prevalent across many different groups in the community.
Table 4 Attitude of respondents towards a person with mental illness
| Item | Overall | Proportion endorsing item, % (s.e.) | ||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Gender | Age group, years | Education years | Household income1 | Urbanicity | ||||||||||||||
| Male | Female | 18-25 | 26-40 | 41-64 | ≥ 65 | 0 | 1-6 | 7-12 | ≥ 13 | L | LA | HA | H | Urban | Semi-urban | Rural | ||
| Afraid to have a conversation | 82.7 (1.3) | 78.5 | 86.4 | 84.5 | 82.4 | 81.0 | 80.6 | 86.7 | 81.7 | 85.0 | 73.7 | 84.2 | 81.8 | 82.3 | 75.0 | 78.1 | 87.0 | 85.7 |
| (2.1) | (1.0) | (2.5) | (1.6) | (2.1) | (3.7) | (2.1) | (2.1) | (1.3) | (4.1) | (1.9) | (2.7) | (1.8) | (3.3) | (2.3) | (2.4) | (1.4) | ||
| χ2=21.64, P<0.001 | χ2=2.66, P=0.59 | χ2=25.23, P<0.005 | χ2=8.26, P=0.12 | χ2=23.60, P<0.01 | ||||||||||||||
| Upset or disturbed about working on the same job | 78.1 (1.1) | 76.2 | 79.9 | 85.1 | 76.4 | 71.8 | 77.0 | 77.8 | 78.4 | 79.8 | 73.7 | 80.7 | 80.8 | 76.2 | 65.1 | 73.0 | 82.6 | 81.9 |
| (1.4) | (1.4) | (2.3) | (1.8) | (2.0) | (4.7) | (2.8) | (2.4) | (1.1) | (2.9) | (1.6) | (2.0) | (2.2) | (4.6) | (2.0) | (1.8) | (1.4) | ||
| χ2=4.03, P=0.05 | χ2=30.54, P<0.01 | χ2=5.14, P=0.28 | χ2=22.31, P<0.01 | χ2=24.64, P<0.001 | ||||||||||||||
| Could maintain a friendship | 16.9 (0.9) | 18.4 | 15.5 | 15.5 | 15.7 | 20.8 | 16.7 | 13.7 | 18.4 | 15.6 | 21.3 | 15.1 | 17.2 | 18.6 | 24.3 | 16.6 | 15.4 | 18.5 |
| (1.3) | (1.2) | (2.1) | (1.3) | (1.9) | (3.1) | (2.1) | (2.1) | (1.7) | (2.2) | (1.7) | (2.3) | (1.7) | (3.6) | (1.5) | (2.0) | (1.1) | ||
| χ2=3.16, P=0.10 | χ2=6.65, P=0.18 | χ2=8.69, P=0.14 | χ2=9.01, P=0.11 | χ2=1.91, P=0.46 | ||||||||||||||
| Unwilling to share a room | 81.2 (1.1) | 81.6 | 80.9 | 85.0 | 78.1 | 80.1 | 85.6 | 80.2 | 81.3 | 81.8 | 80.4 | 83.0 | 80.1 | 79.9 | 80.1 | 74.9 | 86.2 | 86.4 |
| (1.7) | (1.9) | (1.7) | (2.0) | (1.5) | (2.6) | (2.6) | (1.6) | (1.2) | (2.5) | (1.6) | (2.2) | (2.4) | (4.6) | (1.6) | (2.1) | (1.7) | ||
| χ2=0.16, P=0.81 | χ2=12.97, P<0.05 | χ2=0.56, P=0.87 | χ2=3.05, P=0.57 | χ2=42.55, P<0.001 | ||||||||||||||
| Ashamed if people knew someone in your family has been diagnosed with mental illness | 82.9 (0.7) | 81.5 | 84.1 | 86.0 | 83.3 | 78.3 | 80.3 | 80.4 | 81.8 | 84.6 | 82.9 | 83.4 | 85.3 | 82.4 | 76.4 | 80.2 | 83.9 | 85.9 |
| (1.5) | (1.0) | (1.7) | (1.1) | (1.4) | (3.2) | (2.2) | (2.1) | (1.2) | (2.5) | (1.5) | (1.4) | (1.8) | (4.1) | (1.2) | (2.0) | (1.4) | ||
| χ2=2.46, P=0.20 | χ2=11.72, P=0.014 | χ2=3.64, P=0.45 | χ2=6.38, P=0.21 | χ2=8.60, P<0.05 | ||||||||||||||
| Could marry someone with mental illness | 3.4 (0.6) | 3.8 | 3.0 | 2.4 | 3.9 | 3.8 | 2.5 | 2.0 | 4.5 | 3.5 | 2.5 | 3.0 | 4.5 | 3.2 | 4.2 | 3.8 | 2.4 | 3.5 |
| (0.7) | (0.5) | (0.6) | (0.7) | (1.2) | (1.2) | (0.7) | (0.7) | (1.0) | (1.3) | (0.7) | (1.3) | (0.8) | (1.7) | (0.6) | (0.6) | (1.3) | ||
| χ2=0.99, P=0.17 | χ2=2.87, P=0.34 | χ2=4.63, P=0.31 | 4 | χ2=2.16, P=0.51 | χ2=1.83, P=0.46 | |||||||||||||
DISCUSSION
To our knowledge, this is the first large-scale study of knowledge of and attitudes towards mental illness in sub-Saharan Africa. Previous studies have either been on a much smaller scale (Reference Awaritefe and EbieAwaritefe & Ebie, 1975; Reference Odejide and OlatawuraOdejide & Olatawura, 1979), or have examined the perception of stigma by relatives of people with mental illness (Reference Shibre, Negash and KullgrenShibre et al, 2001) or the views of mental illness among special groups (Reference BinitieBinitie, 1970). Large-scale community studies have been lacking. Such studies are of obvious importance for any policy aimed at promoting better knowledge and tolerance of mental illness by the public.
Caveats in interpreting the findings
In interpreting the results of the survey, cognisance should be taken of its limitations. Even though the sample was selected to be representative of the adult population of the Yoruba, who make up about 22% of the Nigerian population, the views expressed may not necessarily reflect the views of the other ethnic groups in the country. Nigeria is a culturally diverse country and its various parts are dissimilar in their access to mental health services (Reference Ayonrinde, Gureje and LawalAyonrinde et al, 2004), both of which factors may affect views about and attitude to mental illness. Nevertheless, a few studies conducted among other ethnic groups in Nigeria, albeit on a much smaller scale, suggest that the findings here with regard to widespread poor knowledge of and attitude towards mental illness may not be peculiar to the Yoruba ethnic group (Reference BinitieBinitie, 1970; Reference Awaritefe and EbieAwaritefe & Ebie, 1975). Also, we have focused on mental illness generally, not on specific mental disorders. In answering questions about mental illness, respondents might have done so with a mind-set on a particular group of mental disorders, probably psychotic disorders, even though our translation sought to capture the specific focus of our interest on mental illness. Although this might have biased their responses in one direction, it would still be remarkable if the public view of what constitutes mental illness was a narrow one.
Causes of mental illness
The common views about what causes mental illness provide a basis for setting other findings of our study in context. This is because views about causation are strongly associated with stigmatising attitudes to mental illness (Reference BhugraBhugra, 1989; Reference Hayward and BrightHayward & Bright, 1997; Reference HaghighatHaghighat, 2001). Our results suggest that knowledge about mental illness is very poor in the Nigerian community. The widespread belief that misuse of drugs is the cause of mental illness may be regarded as good, in view of its possible restraining effect on the use of illicit or psychoactive substances. However, since this is only true for a very limited number of mental disorders, and since the public often views the misuse of substances as a moral failing, this belief may translate to a notion of mental illness as being self-inflicted. Such a view is more likely to elicit condemnation rather than understanding or sympathy (Reference Weiner, Perry and MagnussonWeiner et al, 1988). Other than alcohol, the most commonly used psychoactive substance in Nigeria is cannabis. It is not uncommon for the public in Nigeria to make the assumption that anyone using cannabis will have a mental illness or that anyone with mental illness has used cannabis. Indeed, criminality is also often included in the causal link. Thus, the use of cannabis is often seen as implying a criminal predisposition and vice versa. Next in importance in the list of possible causes of mental illness was a belief that it could be due to possession by evil spirits, and this view was expressed by as many as a third of our respondents. Also, almost one in ten in the community thought mental illness might be a divine punishment. Such views, apart from further implying that people with mental illness might in some way be deserving of their lot, have important ramifications for the seeking of medical care by persons affected. A supernatural view of the origin of mental illness may imply that orthodox medical care would be futile and that help would be more likely to be obtained from spiritualists and traditional healers. Indeed, previous studies in Nigeria have suggested that care for mental illness is most often sought from these providers (Reference Gureje, Odejide and AchaGureje et al, 1995) and that a view about supernatural causation of mental illness is shared by them. In proffering a ‘biological’ or ‘brain disease’ causation for mental illness, our respondents could have meant any of several things. Poisoning, either deliberate or by eating dangerous herbs, is commonly seen as a possible cause of mental illness. There is also a cultural understanding that some emotionally trying traditional rites or rituals could lead to mental illness in those who are not psychologically or physically prepared. Childbirth can also upset the body mechanisms and lead to mental health problems.
Views about mental illness
Negative views about individuals with mental illness were widely held. Less than half of the respondents thought that people with mental illness could be treated outside a hospital or other health facility, implying a belief that community-based care is unlikely to be feasible and might even be dangerous for the public. Only about a quarter thought that mentally ill people could work in regular jobs. Most respondents thought that people with mental illness were mentally retarded, were a public nuisance and were dangerous because of their violent behaviour. These negative views were uniformly expressed by all groups in our study, and there was no clear gender, age, educational or economic correlate of poor knowledge. Negative views of mental illness have been reported in some studies to be more common among the poorly educated, those of low social class and persons aged 50 years and above (Reference Wolff, Pathare and CraigWolff et al, 1996); our study did not identify such associations.
Attitudes towards people with mental illness
The negative views expressed by respondents were indicative of the degree of tolerance they might have of people with mental illness. In particular, views such as those of dangerousness and low intelligence have been found to fuel community resentment of people with mental illness (Reference Hayward and BrightHayward & Bright, 1997; Reference Corrigan and WatsonCorrigan & Watson, 2002). Consequently, the attitudes of our survey respondents to people with mental illness were not surprising. We found that most people in the community would be afraid to have a conversation with someone known to have a mental illness and only a few would consider such a person for friendship. The closer the intimacy required for the interaction, the stronger the community's desire to keep a distance. Thus, less than 4% would consider marrying anyone with mental illness. Here again, the associations with demographic or residential features were very few indeed. Other than a somewhat more tolerant attitude to people with mental illness shown by respondents residing in urban areas and by men, there was no interpretable relationship between negative attitudes to those who are mentally ill on the one hand, and age, education or income on the other hand. Previous studies of selected groups in Nigeria have suggested that negative attitude to mental illness may be less pervasive among the well educated (Reference Odejide and OlatawuraOdejide & Olatawura, 1979). Our findings suggest that the attitudes of such groups do not reflect those of the community at large.
The universality of stigma
The findings of this survey do not support the claim that mental illness is less stigmatised in developing countries (Reference FabregaFabrega, 1991). Although developing countries constitute a diverse group in terms of culture and social norms, it is nevertheless true that our findings are in broad agreement with the observations made by others working in places such as India and Ethiopia (Reference Thara and SrinivasanThara & Srinivasan, 2000; Reference Shibre, Negash and KullgrenShibre et al, 2001). Indeed, as noted by Murthy (Reference Murthy2002), stigmatisation of mental illness probably exists everywhere, even though the form and nature of it may differ across cultures. Our observations suggest that poor knowledge of the causes of mental illness, especially an attribution to supernatural causation, as well as very negative views of persons with mental illness, may indeed be more common in African communities than hitherto realised. Attitude to mental illness is consequently characterised by intolerance of even basic social contact with people known to have such illness. In a society in which poor health facilities and poverty make the care of people with mental illness a major burden for both patients and their families, the degree of stigma experienced by individuals with mental illness suggest an unusual level of illness-related burden.
The need for the development of a well-articulated mental health policy has been identified for most African countries where none exists (Reference Gureje and AlemGureje & Alem, 2000). Findings such as those of our study suggest that a strong emphasis on public education should be an important component of any such policy.
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
▪ In Nigeria, poor knowledge about the cause and nature of mental illness is common in the community.
-
▪ Negative attitudes to mental illness are widespread and may impair the social integration of those with mental illness.
-
▪ Public enlightenment to foster community acceptance of people who are mentally ill is required for all sections of the community, especially for residents of rural areas and the young.
LIMITATIONS
-
▪ The study did not determine attitude to people with different mental disorders. It is possible that attitude is not uniformly poor for all mental disorders.
-
▪ The study was conducted in one language group in Nigeria. Other ethnic groups may have different views about and attitudes to mental illness.
-
▪ The information was obtained through a self-report interview; self-report of attitude and knowledge might have been influenced by a need to conform to perceived cultural norms.







eLetters
No eLetters have been published for this article.