Mental health services have been challenged to meet increasing demand and improve outcomes with decreased real-term funding.Reference Gilburt1, Reference Crisp, Smith and Nicholson2 Given that in-patient bed days are the most expensive units of mental health activity, reducing inappropriate admissions is key to improved productivity.Reference Crisp, Smith and Nicholson2–4 Hospital bed numbers have been reduced, and a recent survey found that less than a third of consultants had enough capacity to meet demand.Reference Crisp, Smith and Nicholson2 Nevertheless, around the country there is marked variation in in-patient bed use,Reference Crisp, Smith and Nicholson2, 5 and the same survey suggested that if appropriate community services were available, almost a sixth of acute admissions could be prevented, echoing past research.Reference Crisp, Smith and Nicholson2, Reference McDonagh, Smith and Goddard6, 7 However, little is known about these individuals or the treatment and support that they require. Against this background, a balance of care (BoC) approach was used to explore whether the needs of certain in-patients could be met in alternative ways and, if so, which individuals require what services, at what cost.
Method
Setting
The research was undertaken in a large mental health trust in the north of England and formed part of a wider study of the best mix of services to provide for working age adults with mental health problems currently receiving community mental health team (CMHT) or in-patient services. This paper focuses on the latter population. In addition to CMHTs, core community services included home treatment and early intervention teams, as well as psychiatric liaison services based in general hospitals.
The BoC approach
The BoC approach is a long-standing, strategic planning framework that identifies patients whose needs could be met in more than one setting (for example hospital or home) and explores the potential costs and consequences of the different care options in a simulation exercise grounded in the knowledge of experienced frontline practitioners.Reference Mooney8–Reference Tucker, Brand, Wilberforce and Challis10 As such, it provides service planners and commissioners with important information to underpin decisions about resource allocation. The six interlinked activities are described below.
Stage 1: patient profiling
Anonymised data on in-patients' sociodemographic, clinical and service receipt characteristics were collected for a 7-week series of consecutive admissions to the Trust's acute mental health wards in 2013/14 (plus a 16-week series of consecutive referrals to CMHTs). Interward transfers and patients aged under 18 or over 64 were excluded. As the unit of analysis was the care episode, individuals could appear in the sample more than once.
The data-collection proforma was based on a modified version of the Matching Resources to Care (MARC-2) instrument, which encompasses the main items characterising severe mental illness specified in the academic and policy literature.Reference Huxley, Reilly, Gater, Robinshaw, Harrison and Mohammed11, Reference Huxley, Evans, Munroe and Cestari12 The majority of data (over 40 items), including the Health of the Nation Outcome Scale (HoNOS)Reference Wing, Curtis and Beevor13 and other items utilised within the Mental Health Clustering Tool,14 were extracted from the Trust's electronic record system by National Health Service (NHS) information technology staff and, where data permitted (just one or two items were missing), multiple imputation was used to fill missing HoNOS values. All data items were those closest to the date of in-patient admission. Six additional variables critical to the profiling exercise and the reason for admission were collected by practitioners at point of hospital entry. Further information on the data collection exercise is available in Supplementary online file 1 available at https://doi.org/10.1192/bjo.2018.60.
Stage 2: case-type development
The sample was divided into 48 subgroups (‘case types’) using five variables deemed likely to be important in determining the locus, extent and cost of their care: affect/self-harm, other risks, psychotic symptoms, drug/alcohol misuse and relationship difficulties (see Supplementary online file 2). The selection of attributes followed a sequential process. First, a list of potential attributes was compiled from discussions with the study's Patient and Public Involvement Group and experienced Trust practitioners, plus a review of the wider BoC literature and mental health policy. Subsequently, an iterative approach was taken to prioritise these attributes in order to develop a typology whereby each of the most commonly populated groups captured at least 2.5% of the wider study sample (in-patient and CMHT patients), was broadly homogeneous on a number of other attributes, and was clinically meaningful. Together the most populated groups were required to capture at least two-thirds of the wider study sample.
Stage 3: formulation of vignettes
With the help of Trust personnel (a psychiatrist, ward manager, nurse, social worker and occupational therapist) a series of anonymous vignettes were drafted to represent the most prevalent case types in the wider study sample, ensuring their content validity. These were based on exemplar patients in the dataset and took the form of short case histories. Each vignette incorporated information about the five key variables employed in the case typology as well as the individual's mental health history, living situation, clinical state and service receipt. An example of a vignette is given in the Appendix.
Stage 4: generation of alternative care options
A range of staff from organisations involved in the provision of mental healthcare were invited to two locality-based care-planning workshops. These explored the most appropriate ways to meet the needs of the patients depicted in the vignettes.
Workshop participants were divided into small multidisciplinary groups, each of which was allocated a subset of seven vignettes. Following a modified nominal group approach,Reference Bowling and Bowling15 participants were asked to indicate, first individually and then in their small groups, where they believed each depicted individual would be most appropriately supported – in hospital or the community. For those case types for whom community care was preferred (hereafter referred to as ‘marginal’ case types) they then specified the services required on care-planning sheets. These were based on local Trust documentation and differentiated between the input recommended in weeks 1 and 2 and weeks 3 to 8, respectively. To encourage participants to think beyond current practice, groups were provided with details of services available elsewhere.
Stage 5: cost analyses
The estimated weekly costs of the proposed community care plans were compared with the costs of in-patient care using publicly available excel-based cost-modelling templates.Reference Tucker, Brand, Wilberforce and Challis16, Reference Brand, Tucker, Wilberforce and Challis17 Costing employed a public-sector approach focusing on the most important (expensive or commonly incurred) costs borne by health and social care services. Wherever possible, the analysis drew on national unit costs and other publicly available sources.Reference Curtis18, 19 If national costs were unavailable, local information was employed. All costs related to 2013.
The aggregate annual cost differences that might result from substituting the recommended community arrangements for in-patient admission were then estimated. Information about the likely number of admissions in each marginal case type was estimated from the patient profiling exercise (assuming current conditions prevailed), with the potential diversion period assumed to equate to the mean length of in-patient stay for each case type (excluding outliers). Confidence intervals were calculated to reflect uncertainty about the quantity and cost of resources used in the alternative planning scenarios. The possibility of cost-shifting between health and Social Services was examined and sensitivity analyses were undertaken to explore the impact of changing a number of structural aspects of the model, including the proportion of in-patients in each case type who might realistically be cared for in the community.
Stage 6: validation of results
A range of service commissioners, managers, providers and frontline practitioners were invited to a validation workshop. This had two parts. First, the researchers presented the findings from the patient profiling exercise, care-planning workshops and cost analyses. Second, participants commented on the validity of the findings; identified what they perceived to be the main issues they raised for the Trust; and highlighted their priorities for service improvement.
Ethics
The study received ethical approval from the University of Manchester Research Ethics Committee (ref. 13076). It was also approved by the Trust, adopted by the Mental Health Research Network and supported by the Association of Directors of Adult Social Services. The patient profiling information provided by the Trust was fully anonymised and the research team had no patient contact. Written informed consent was obtained from participants at the care-planning and validation workshops.
Results
In-patient characteristics
Information was collected on 315 care episodes relating to 300 individuals; 287 people had one admission, 11 had two, and two had three. Table 1 details their key sociodemographic, functional and clinical characteristics. Admissions of men outnumbered that for women by approximately three to two, and most individuals were White, over 30 years old and unemployed. Of those admissions for whom information was available (all HoNOS and related care cluster data were missing for almost 25% of the sample), nearly 60% were classified as having a psychotic disorder, and the majority had a complex mix of clinical and social problems.
In-patient admissions: sociodemographic, functional and clinical characteristics

a. Health of the Nation Outcome Scale score of ≥2.
Timing and source of admissions
Most (80%) admissions occurred on weekdays. However, 58% of these were outside normal working hours (09.00–18.00 h). The most common sources of referral were accident and emergency (24%) and psychiatric liaison services based in general hospitals (19%).
Reasons for admission
Information on the reason for admission was available for 290 admissions. As might be expected, most (90%) had experienced a substantial deterioration in their mental health/social functioning, while approaching three-quarters (72%) were considered at increased and substantial risk of harm to themselves or others. In total 30% were reported to be at increased and substantial risk of self-neglect, and a similar proportion was considered at significant risk of injury or abuse. Breakdown of support was said to have contributed to around a fifth (18%) of admissions, and 79% were deemed to require an immediate change of management.
Prior service receipt
Most (85%) in-patients were known to the Trust before the current care episode. Although some individuals had been out of contact with Trust services for many years, more than three-quarters had been seen by community services in the past month (mean 4.4 service contacts excluding patients with no contact), and over a third had been admitted to a mental health bed in the previous year.
Case-type distribution
Of the 48 case types used to characterise the sample, 44 were populated. These captured 75.6% of admissions (76 admissions lacked sufficient HoNOS data to include in the categorisation, and one lacked other necessary information.) As expected, some case types were more prevalent than others, and following the above criteria, 17 case types were selected for exploration in the BoC analysis (Table 2). Together these represented 63% of the admissions included in the categorisation.
Characteristics and size of the 17 case types depicted in the vignettes
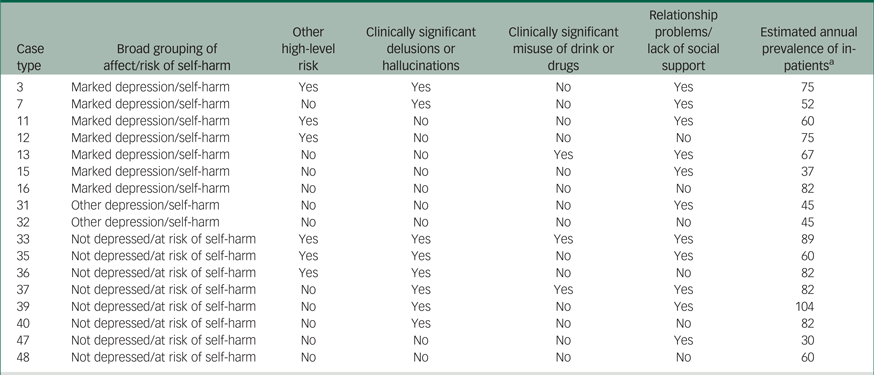
a. Based on individuals it was possible to categorise.
Alternative care options
A total of 58 staff participated in the care-planning exercise. Nurses were the most frequently represented discipline; others included consultant psychiatrists, occupational therapists, social workers, service managers and commissioners. More staff worked in community than in-patient settings (27 v. 20); 11 covered both.
Individual professionals made a total of 406 placement recommendations, and each case type (vignette) was considered by at least 22 participants. Multidisciplinary groups made a total of 40 recommendations and each case type was considered by at least eight groups.
Focusing on the multidisciplinary groups' recommendations, four case types (33, 35, 36 and 37) were overwhelmingly perceived to be most appropriately treated in hospital, and the majority of groups also recommended in-patient care for a further three (7, 39 and 40). In contrast, if enhanced community services were available, five case types were unanimously perceived to be more appropriately supported in the community (11, 12, 32, 47 and 48), and the vast majority of groups favoured community care for a further two (15 and 16). Views about the remaining three (3, 13 and 31) were more mixed, albeit most groups favoured community care (Table 3).
Multidisciplinary groups' placement recommendations
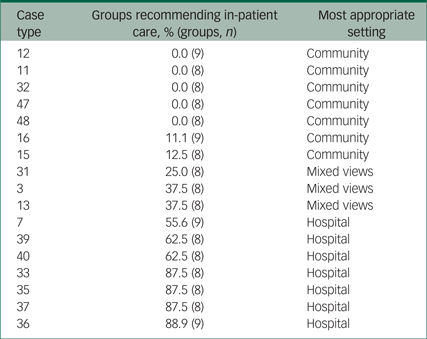
The seven case types for whom hospital care was seen as most appropriate typically represented people with schizophrenia who exhibited psychotic symptoms, posed a high risk to themselves or others, had limited understanding of their illness and were reluctant to adhere to treatment. Two represented people with marked drug/alcohol misuse problems, and five represented people who were socially isolated or had complex social problems. The majority of these patients were well-known to mental health services, and had had several (often involuntary) past admissions. Projections suggested the Trust had at least 550 admissions in these case types each year.
In contrast, the five case types for whom community support was unanimously recommended represented people with mild-moderate depression in combination with an eating or personality disorder, or individuals with schizophrenia that had deteriorated in the presence of a specific stressor. None had a history of substance misuse or current psychotic symptoms, and most had reasonably settled social circumstances. Analysis suggested there were approximately 270 such admissions in the Trust each year.
The five case types for whom the vast majority of groups recommended community care, or about whom views were mixed, typically included patients with more marked depression against a background of recent life stress, repeat self-harm, a suicide attempt and/or volatile relationships. Just one of these case types had active psychotic symptoms and another had alcohol misuse problems. Projections suggested there were over 300 such admissions in the Trust annually.
As logically any attempt to change the BoC would focus on those case types considered least appropriate for hospital, only those ten case types for whom the majority of groups favoured community care were included in the remaining analysis. These represented 32% of the in-patient admissions categorised in the case typology, and 24% of all admissions. Forty-two care plans were proposed for these case types, ranging from two for case type 47 to seven for case types 12 and 16 (with particular effort made to cover those case types representing higher numbers of in-patients). In the main, these plans drew on existing mental health services in weeks 1 and 2, supplemented by a wider range of health, social, employment, housing and welfare services in the medium to long-term. The six most common services/professional inputs in the short term were carer support services, CMHTs, consultant psychiatrists, general practitioners, intensive home treatment teams and mental health support workers, whereas additional services employed in weeks 3 to 8 included community groups, peer support, benefit and psychology services. Analysis suggested intensive home treatment teams and CMHTs would need to be able to deliver at least twice daily and twice weekly support, respectively.
Cost comparisons
Considerable variation was found in the cost of the proposed community care packages, both within and between case types, dependent on the nature and extent of the services used (see supplementary online file 3). Thus, although the costs of the three care plans for case type 13 were very similar (£550, £587 and £601 per week), the costs of the seven packages for case type 12 ranged from £333 to £2959 per week. That said, all bar three of the 42 care packages were less expensive than hospital admission (estimated at £2456 per week), with a mean cost difference of £1626 per week. Furthermore, despite the use of multiple community staff and intensive input, most of this difference was attributable to the relatively low costs of providing specialist mental healthcare in the community rather than in hospital. In contrast, social care costs increased in most plans (mean cost increase £61 per week).
Table 4 details the potential aggregate annual cost differences that might result from diverting some or all of these admissions over the course of a year. The key variables in these calculations are the number of in-patient admissions represented by each case type projected over a 12-month period; the estimated costs of the proposed community care packages; and the length of in-patient stay. For example, if it proved possible to provide appropriate community care for all 60 admissions in case type 11, with each prevented admission releasing approximately £7200 compared with a 24-day hospital stay, this could in theory save local agencies almost £430 000 per year. However, although the estimated weekly cost of supporting an individual in case type 11 in the community is lower than that of a person in case type 12, because the latter represents a larger number of individuals with a longer hospital stay, the potential aggregate cost difference of diverting people in case type 12 is greater. Sensitivity analysis indicated that even if it only proved possible to divert 50% of admissions in case type 12 (the case type considered most appropriate for community care), the resulting cost difference might be as much as £600 000, whereas if it proved possible to provide appropriate community support for 50% of the people in all ten case types, the cost difference would approach £2 000 000.
Estimated savings from successful diversion from in-patient care (£s)
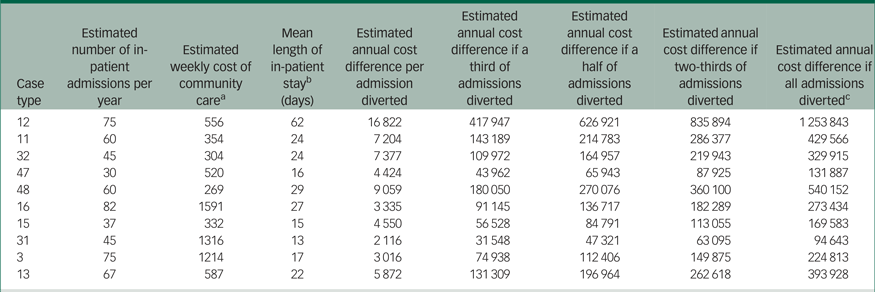
a. With the exception of case types 15 and 47, for which there were just two alternative care plans, these calculations are based on the median cost alternative care package. For case types 15 and 47 the higher cost proposal was used.
b. Excluding outliers.
c. Note the last column is not an exact multiple of the second and fourth because both numbers are rounded.
Validation and interpretation of results
Fifteen personnel attended the validation workshop, including consultant psychiatrists, senior mental health and local authority managers, CMHT, psychiatric liaison and ward staff. The discussion highlighted four issues. First, participants agreed that there were currently many inappropriate hospital admissions. Second, attendees were surprised by the proportion of hospital admissions outside of normal working hours, which they related to a lack of community services after 18.00 h and at weekends. Third, the costs of the proposed community care packages were perceived as modest and it was suggested that staff participating in the care-planning workshops had been unconsciously constrained by their experience of resource limitations. Fourth, there was widespread consensus on the need to increase out-of-hours community services and improve service access, including developing more flexible service boundaries between primary and secondary mental health services and health and social care.
Discussion
Main findings and comparison with findings from other studies
This study supports previous research that indicates that if the necessary community resources were available, a significant minority of in-patients could be more appropriately supported in less restrictive settings.Reference Crisp, Smith and Nicholson2, Reference McDonagh, Smith and Goddard6, 7 Moreover, it starts to identify the characteristics of those subgroups of in-patients for whom community care is considered more appropriate, and to enumerate the resources required in order to meet their needs, the costs of which appear relatively modest. This does not necessarily mean that the level of in-patient beds could be reduced, for there will always be a cohort of patients who require care in hospital with the intensive levels of assessment, monitoring and treatment this offers,Reference Crisp, Smith and Nicholson2, 20, Reference Thornicroft and Tansella21 and the presented data say nothing about the number of community patients for whom hospital admission would be more appropriate (the extent of unmet demand). However, the findings do suggest that existing beds could be used more efficiently and highlight the need for any new mental health strategy to focus on the whole care system.
Whereas several past studies have highlighted a lack of interprofessional consensus as to who needs hospital admission,Reference Gorrindo, Goldfarb, Chevalier, Hoeppner, Birnbaum and Meller22–Reference Phillips, Gerdtz, Elsom, Weiland and Castle24 this research found considerable agreement on those admissions for whom community care was deemed more appropriate. It is thus important to consider why, in reality, such patients are being admitted to hospital, incurring high human and financial costs. The first thing to say is that the findings do not automatically imply that actual placement decisions were incorrect, for, in reality practitioners’ decisions are constrained by the availability of alternative resources.
At the validation workshop, it was noted that the high proportion of admissions outside of normal working hours was at least partly related to the unavailability of community services at such times, and nationally it has been reported that only half of CMHTs offer a 24/7 service for people in crisis.25 Recent policy guidance has committed to ensuring all crisis response and home treatment teams can provide a 24/7 alternative to acute in-patient admission by 2020/21.26 However, there are questions about the funding for such new services, which it has been suggested will arise from the reinvestment of savings and efficiencies generated by improved mental healthcare.26 Compared with the costs of in-patient care, the costs of the community care packages proposed in this study appeared relatively low, and, interestingly, patient representatives and carers who considered the needs of a subset of the vignettes in a mirror exercise (not reported here) typically endorsed still lower cost options than those employed here. Nevertheless, it is important to note that the identified cost differences do not directly equate to cost savings, for in order to release significant monies, the number of hospital admissions prevented would need to reach a critical mass facilitating the closure of beds/wards. Furthermore, at least in the short term any large-scale change would require additional investment (bridging funds), since any new provision must be in place before existing services close.
Methodological considerations
Service planning for people with mental health problems is not easy.Reference Mooney27 This is a heterogenous population with fluctuating needs, multiple organisations are engaged in service provision, and there is relatively little evidence about the comparative cost-effectiveness of institutional and non-institutional services. Moreover, outcomes are complex and difficult to measure, and processes to support strategic development are not well developed. Against this background, this research demonstrates the potential of the BoC approach to provide a transparent and systematic framework to support local decision-making and service redesign that starts not with the available services, but with patients' needs. Further, in bringing together stakeholders from different agencies, the approach promotes staff ownership and generates momentum for change since local staff members inform the study's scope, suggest alternatives and help identify solutions.Reference Tucker, Hughes, Brand, Buck and Challis28
That said, there are a number of reasons to treat the study's findings with caution. First, in seeking to maximise the use of routinely available data, the analysis was unable to categorise nearly a quarter of in-patient admissions because of the lack of information. Individuals with missing HoNOS data were less likely than other patients to have had a previous hospital admission. However, there was no way of knowing whether they were more, less or equally appropriate for in-patient care than those for whom data were available. Second, the presented costs were all best or central estimates (although even the highest costs employed in the sensitivity analyses suggested that the proposed alternative community care would be considerably less expensive than hospital admission).
Third, in taking a public-sector costings approach, no account was taken of the costs of the (often substantial) assistance provided by informal carers. Fourth, ideally one would want to incorporate robust evidence about the effectiveness of care in different locations into the approach. However, to date no easy way has been found to do this,Reference Tucker, Brand, Wilberforce and Challis10 and in light of this gap, the method assumes that in appraising alternative settings practitioners consider patients' best interests. Fifth, the use of vignettes cannot, of course, fully represent real-world decisions. Nevertheless, they provide a cost-effective way of investigating professional decision-making and enable existing conventions and constraints to be challenged.
Sixth, although the mix of services available in the study area and the sociodemographic and clinical characteristics of the patient population appeared largely typical of provision nationwide, it is not clear to what extent the study's findings can be generalised to other localities. However, the search for the most appropriate ways of supporting adults with mental health problems is certainly not just of local interest, while continuing financial pressures and increasing demand mean that the need to improve quality and efficiency is unlikely to go away any time soon.
Although originally developed as a national policy analysis tool in the 1970s,Reference McDonald, Cuddeford and Beale29 the BoC approach has subsequently been used for a wide variety of patient groups in a number of different settings. However, two systematic literature reviews identified only one previous (somewhat specialised) study that had employed the approach in adult mental health services,Reference Knapp, Chisholm, Astin, Lelliott and Audini30 and highlighted a number of methodological problems with its use to date, including its typically heavy reliance on bespoke data collections.Reference Tucker, Brand, Wilberforce and Challis10, Reference Tucker, Hughes, Brand, Buck and Challis28 Against this background, it is hoped that this paper serves to demonstrate the potential utility of the BoC approach to improve services for working age adults with mental health problems, and to use routinely collected electronic data for local service planning. As such, the presented analysis could now usefully be replicated in other areas.
Acknowledgements
We thank the members of the Lay Reference Group (R Hanlon, M Mistry and J Smith) for their committed and insightful collaboration on this study.
Funding
This article presents independent research funded by the National Institute for Health Research (NIHR) School for Social Care Research (SSCR). The views expressed in this article are those of the authors and not necessarily those of the NIHR SSCR or the Department of Health, NIHR or NHS.
Supplementary material
Supplementary material is available online at https://doi.org/10.1192/bjo.2018.60.
Appendix
An example of a vignette: Carolyn (vignette 11)
Sociodemographic information
Age, gender, employment status: 38-year old unemployed woman.
Living situation: Is currently living with her parents, having broken up with her partner. Accommodation reasonably acceptable.
Past mental health history
Past service use: Has had frequent contact with the specialist mental health services over the past 10 years, including a number of in-patient admissions with repeat self-harm (cutting and overdoses) and destruction of property. Was last discharged from hospital approximately 10 months ago. Adherence to medication is described as ‘fair’; attendance at appointments ‘good due to help’.
Diagnosis: Depression/anxiety/borderline personality disorder. Has limited ability to protect herself, posing definite risks to her health, safety and well-being (significant – severe vulnerability).
Current presentation
Mental health:
(a) Irritable and agitated; verbally abusive;
(b) Frequent panic attacks with shortness of breath and palpitations;
(c) Marked depression; feelings of emptiness and hopelessness; disturbed sleep;
(d) Threatening to harm herself (overdose);
(e) No psychotic symptoms.
Activities of daily living: No marked self-neglect but looks slightly dishevelled. Has ongoing problems with budgeting/use of money/forms etc.
Physical health: No long-standing physical health problems.
Use of alcohol/drugs: No history of illicit drug or alcohol misuse.
Social support: Long-standing problems making and sustaining relationships, which tend to be stormy and intense. Has a complex and difficult relationship with her parents. No current safeguarding concerns.
Reason for referral: Low mood and threat of self-harm further to break-up of recent relationship.






eLetters
No eLetters have been published for this article.