LEARNING OBJECTIVES
After reading this article you will be able to:
• understand primary hyperparathyroidism (PHPT), including its causes, signs and symptoms
• understand the relationship between PHPT and psychiatric illness
• know when to refer and how to support management of a patient with PHPT within mental health settings.
This article reviews the psychiatric manifestations, causes and management of primary hyperparathyroidism (PHPT), focusing on the key areas outlined in the learning objectives above. The article is based on our systematic review of the literature (Box 1) and our focus in this narrative review is on depression and dementia, and their potential relation to PHPT, as these areas have the most available data. We did not explore PHPT and psychosis, as literature in this area is limited to case reports. Our review was prompted by the presentation of several patients with PHPT or lithium-associated hyperparathyroidism (LAH) in our practice and it aims to update clinicians on PHPT.
The literature search
We searched Google Scholar, PubMed, MEDLINE and PsycINFO using the major terms ‘depression’, ‘anxiety’, ‘delirium’, ‘cognitive impairment’ and ‘dementia’, in conjunction with ‘primary hyperparathyroidism’ (PHPT).
The search spanned from 1 January 2014 to 12 February 2024 and included only English-language papers, excluding case reports or case series of few or single cases. We also referenced some older literature, published before 2014, where relevant. Forty-two full-text articles were reviewed.
Prevalence and aetiology of primary hyperparathyroidism
Primary hyperparathyroidism (PHPT) is a relatively common disorder, with an estimated overall prevalence of 0.84–0.86% (Soto-Pedre Reference Soto-Pedre, Newey and Leese2023). It is the most common cause of persistent hypercalcaemia (Bilezikian Reference Bilezikian2018) and the third most common endocrine condition after diabetes and thyroid disease (Madkhali Reference Madkhali, Alhefdhi and Chen2016), although it tends to be underdiagnosed. Although PHPT can occur across all ages, it usually manifests in later life, with a mean age at diagnosis of 65 (Soto-Pedre Reference Soto-Pedre, Newey and Leese2023). It affects women three to four times more often than men (Bilezikian Reference Bilezikian2018). As awareness of the need to test for PHPT increases, so too will the numbers of people receiving mental health treatment who have PHPT. This underscores the importance of improving psychiatrists’ knowledge of this important topic.
There are two pairs of parathyroid glands, each about the size of a grain of rice, located adjacent to the two thyroid gland lobes in the neck, although the anatomy can be highly variable. In healthy individuals, the glands sense serum calcium levels and act to prevent them from falling too low. They do this by releasing parathyroid hormone, which increases calcium by increasing the action of osteoclasts in bone, increasing renal reabsorption of calcium in the distal convoluted tubule and collecting duct, as well as activating vitamin D to promote calcium absorption in the gut. In PHPT there is a failure of this Mechanism and the secretion of parathyroid hormone becomes dysregulated, resulting in hypercalcaemia. This is most commonly due to the development of a single parathyroid adenoma (about 80% of cases), but may also result from gland hyperplasia (about 15%), multiple adenomas (about 5%) or, rarely, parathyroid carcinoma (less than 1%) (Walker Reference Walker and Silverberg2018).
PHPT is usually sporadic, but it may be inherited as part of a genetic condition that may be syndromic (i.e. associated with other features) or non-syndromic. Patients with genetic forms of PHPT may present differently and require different management, which is beyond the scope of this article.
Lithium-associated hyperparathyroidism (LAH) is clinically indistinguishable from PHPT. While the exact mechanisms of LAH remain unclear, hypothetical mechanisms are discussed in greater detail below.
Symptoms
Advances in testing methods have led to the identification of many asymptomatic cases of hyperparathyroidism. Most biochemical diagnoses are made incidentally following a routine blood test. The classic textbook description of PHPT symptoms, often summarised by the mnemonic ‘bones, stones, groans and psychic moans’, is rarely relevant in the Western world today, although it remains a useful way to remember the core symptoms. Hypercalcaemia may produce a range of symptoms, including anorexia, nausea, vomiting, thirst, polyuria, constipation, fatigue and hypotonicity. Gastrointestinal issues such as dyspepsia and peptic ulcers may also occur (‘groans’). Psychiatric symptoms may occur, such as depression, anxiety and confusion (‘psychic moans’). Additionally, increased calcium absorption from bones results in reduced bone density and increased fracture risk, which may lead to fragility fractures. Despite increased calcium reabsorption in the kidney, most patients will still have hypercalciuria, which can lead to nephrocalcinosis and renal stones.
Psychiatric manifestations (‘psychic moans’)
Serdenes et al (Reference Serdenes, Lewis and Chandrasekhara2021) reviewed the literature on neuropsychiatric features of primary hyperparathyroidism, covering reports of symptoms such as depression, anxiety, mania, psychosis, delirium, catatonia, but excluding dementia or mild cognitive impairment in 76 papers (including case studies). They noted that many of the papers reviewed were over 10 years old and were limited by small sample sizes and the poorly defined methodologies employed. They report on mechanisms inducing these symptoms. The direct impacts of both parathyroid hormone and hypercalcaemia in the brain may explain the breadth of neuropsychiatric manifestations of PHPT. Hypercalcaemia and parathyroid hormone can affect monoamine transmission through the following mediators: tyrosine hydroxylase, interleukin-6 (IL-6), monoamine oxidase (MAO), calcium and sodium–potassium adenosine triphosphatase transporter (Na/K-ATPase). The interested reader should refer to this review for further discussion on possible mechanisms. The authors concluded that the most effective treatment for neuropsychiatric symptoms is parathyroidectomy.
Our own literature review found that in studies of patients undergoing parathyroidectomy for PHTP, 43–53% of individuals report suffering from anxiety, 37–47% report impaired cognition and 32–62% report depression (Parks Reference Parks, Parks and Onwuameze2017). PHPT can be associated with a range of severe mental health or non-specific symptoms, including depressive symptoms, anxiety, fatigue and forgetfulness. These non-specific complaints are difficult to recognise but can be captured by quality of life measures, with some studies showing improvements in quality of life after surgery. A detailed discussion of post-operative quality of life is beyond the scope of this article but is well covered in a recent narrative review (Reference Carsote, Nistor and StanciuCarsote 2023) and Cochrane review (Pappachan Reference Pappachan, Lahart and Viswanath2023) demonstrating inconclusive results. The available evidence is limited, owing to the use of numerous different instruments (Carsote Reference Carsote, Nistor and Stanciu2023), as well as differences between studies regarding the domains of quality of life that improve post-operatively (Pappachan Reference Pappachan, Lahart and Viswanath2023).
A retrospective cohort study investigating the prevalence and sequalae of delays to diagnosis of PHPT in people over the age of 40 found that those whose diagnostic workups or time from diagnosis to treatment exceeded 1 year had higher rates of major depressive disorder, anxiety disorder and reported fatigue and malaise (Reference Lorenz, Beauchamp-Perez and ManniLorenz 2022). Some authors therefore encourage psychiatrists to approach PHPT as a predominantly asymptomatic condition and to have a low threshold for testing of calcium levels, especially in elderly patients (Bilezikian Reference Bilezikian2018). Patients often report psychiatric manifestations such as depression, anxiety and cognitive issues and the extent to which these symptoms relate to parathyroid disease remains controversial, as discussed in detail below.
Depression
Depression is the most prevalent affective disorder among people with PHPT. Nevertheless, the relationship between depressive symptoms and PHPT remains unclear, given the high prevalence of depression in the general population. Many earlier studies were confounded by a lack of control groups, small sample sizes or other methodological issues, leading to conflicting results. A helpful and more modern approach is to examine whether depressive symptoms or a fully defined depressive disorder resolve after parathyroid surgery compared not only with general population controls but also with groups undergoing thyroid surgery (usually for benign thyroid nodules). More recent studies have used the Patient Health Questionnaire-9 (PHQ-9) as a proxy to examine whether a depressive disorder, rather than solely depressive symptoms, resolves post-surgery. Kroenke et al (Reference Kroenke, Spitzer and Williams2001) demonstrated that a PHQ-9 score ≥10 had a sensitivity of 88% and a specificity of 88% for major depression. Although some studies using self-rated scales have reached similar conclusions to those using the PHQ-9, these scales make it harder to infer a depressive syndrome and some have been shown to be insufficient (Kunert Reference Kunert, Gawrychowski and Sobiś2020) so we have not included studies using self-rated scales in our discussion.
Several studies pre-dating our literature search supported the idea that depression improved post-surgery. In their seminal study, Joborn et al (Reference Joborn, Hetta and Johansson1988) found that 18% of 441 patients with primary hyperparathyroidism experienced pre-surgery depression and anxiety and that symptoms did not relate to the degree of hypercalcaemia. These symptoms, as well as low monoamine metabolites (5-hydroxyindoleacetic acid (5-HIAA) and homovanillic acid (HVA)) in the cerebrospinal fluid improved post-surgery. Wilhelm et al (Reference Wilhelm, Lee and Prinz2004) noted in their study (n = 360) that 10% of the patients met DSM-IV-TR criteria for major depression pre-operatively. Post-operatively, 90% of these patients said that depression no longer impaired their ability to work or to perform activities of daily living. Furthermore, 27% were able to discontinue antidepressant use. Weber et al (Reference Weber, Eberle and Messelhäuser2013), in a study of 194 individuals receiving parathyroidectomy surgery and a control group of 186 individuals undergoing benign non-toxic thyroid surgery, demonstrated that post-surgery, the parathyroidectomy group showed significant declines in symptoms of in depression and a 51% reduction in the prevalence of suicidal thoughts, as well as improvements in quality of life.
Based on our literature search we report on two further studies since 2014 that used current surgical criteria and biochemistry, appropriate control groups and objective rating scales. Liu et al (Reference Liu, Peine and Mlaver2021) and Kearns et al (Reference Kearns, Espiritu and Vickers Douglass2019) showed that pre-surgery patients with PHPT were more symptomatic (using PHQ-9) than those having thyroid surgery. Both studies also demonstrated that patients with PHPT had significant improvement in terms of depressive symptoms post-surgery, although there were no significant differences in symptoms between the two groups post-operatively.
In the Liu et al (Reference Liu, Peine and Mlaver2021) study, 27.5% of the 244 patients with PHPT experienced moderate to severe depression pre-operatively, compared with 18% of the 161 who underwent thyroidectomy. After surgery, this dropped to 8.2% in the PHPT group and 5.3% in the thyroid group (P < 0.01). The study was well-conducted, across multiple centres and employed modern objective rating scales. A limitation of the study was that the authors did not comment on the use of antidepressants or other psychotropics and or how these were managed post-surgery. In addition, follow-up was conducted in the very short term, 2–3 weeks post-surgery.
Kearns et al (Reference Kearns, Espiritu and Vickers Douglass2019), in a smaller single-centre study, also showed that depressive symptoms were higher in the PHPT group than in control thyroid group pre-surgery, with median scores on the PHQ-9 of 7.5 and 3.0 respectively. Both groups showed significant improvements post-surgery, with median PHQ-9 scores of 2 and 1 respectively. This study did assess antidepressant use and correlated this with PHQ-9 scores, and had longer-term follow-up of patients (12 months). Baseline parathyroid hormone levels, but not calcium levels, had a weak relationship with change in PHQ-9 score after parathyroid surgery (P = 0.003). The authors suggested that such depression scores should be a relative indication for surgery.
Both the Liu et al (Reference Liu, Peine and Mlaver2021) and Kearns et al (Reference Kearns, Espiritu and Vickers Douglass2019) studies provided supportive evidence that parathyroidectomy improves symptoms measured using symptomatic rating tools such as the PHQ-9 or Generalised Anxiety Disorder Questionnaire (GAD-7). The findings were not conclusive, given that psychiatric clinical diagnoses were not formally made pre- or post-surgery. It would be helpful to have more research on whether parathyroid hormone or adjusted calcium levels correlate with depressive symptoms pre-surgery, although research thus far has not shown such correlations to be evident (Joborn Reference Joborn, Hetta and Johansson1988; Kearns Reference Kearns, Espiritu and Vickers Douglass2019; Kunert Reference Kunert, Gawrychowski and Sobiś2020).
The National Institute for Health and Care Excellence (NICE) does not currently recognise depression in PHPT as a criterion for surgical intervention (NICE 2019), but there is growing evidence that it should be considered, particularly if it meets criteria for moderate or severe illness. It seems likely that individuals with PHPT meeting current criteria for surgery who also have a moderate or severe depressive disorder can be advised that these depressive symptoms may improve post-surgery. However, we cannot be sure that all depressive symptoms will resolve, as even in studies with well-defined criteria not every patient improves. Further research in this field needs to be more meticulous in determining pre- and post-operatively whether patients have depressive symptoms rated on an objective scale like the PHQ-9 or, preferably, diagnosed using ICD or DSM criteria for depressive disorder. Greater attention should also be paid to any treatments for depression provided pre- and post-operatively. A recent prospective cohort study examining the use of selective serotonin reuptake inhibitors (SSRIs) and benzodiazepines showed that benzodiazepine use declined post-surgery whereas SSRI use remained unchanged (Koman Reference Koman, Bränström and Pernow2022). Therefore, the current literature remains unclear regarding when or how a clinician might approach cessation of antidepressant medication.
Cognitive impairment and dementia
Two systematic reviews have examined the question of whether PHPT impairs cognition. Lourida et al (Reference Lourida, Thompson-Coon and Dickens2015) covered studies up to 2014 and Jiang et al (Reference Jiang, Hu and Li2020) updated the literature to 2020. Both reviews noted that the studies used widely varying methods of cognitive assessment, making meta-analysis impossible and therefore only narrative synthesis was possible. Neither review felt able to state that any of the studies were of high quality although some were of good quality. Methodological issues, such as various sample sizes and the inconsistent use of controls, hampered the ability of these reviewers to reach definitive conclusions.
In terms of prospective follow-up studies examining the effects of raised parathyroid hormone levels in the community, there are three main large, long-term prospective studies highlighted in the review by Jiang et al (Reference Jiang, Hu and Li2020). Kim et al (Reference Kim, Zhao and Schneider2017) demonstrated in a very large sample (n = 12 964) over 20 years that there was cognitive decline but no independent effect of parathyroid hormone on this cognitive decline. Hagström et al (Reference Hagström, Kilander and Nylander2014), in a fairly large sample (n = 998), found an association between elevated parathyroid hormone levels and the development of vascular dementia, but not Alzheimer's disease, over a 15.8 year follow-up period. Björkman et al (Reference Björkman, Sorva and Tilvis2010) showed a correlation between parathyroid hormone and memory at 1 year which is not upheld at 10 years. Cross-sectional studies in this area have demonstrated mixed results. Therefore, we agree broadly with the conclusions of Jiang et al (Reference Jiang, Hu and Li2020) and Lourida et al (Reference Lourida, Thompson-Coon and Dickens2015) that there is only weak and inconsistent evidence for an association between PHPT and impaired cognitive function.
A number of smaller prospective cohort studies have been conducted that used more detailed neuropsychological testing. Lourida et al (Reference Lourida, Thompson-Coon and Dickens2015) found 13 pre-/post-surgery studies involving patients with PHPT. In the eight studies that had control groups, patients improved in at least one cognitive domain. Five of the eight studies reported improvement on at least some memory tests, but often not all of the memory subtests. Studies by Walker et al (Reference Walker, Mcmahon and Inabnet2009) and Roman et al (Reference Roman, Sosa and Pietrzak2011) had large sample sizes (n = 128 and n = 159) and showed marked improvement in memory tests post-surgery. None of the five studies that examined executive function showed any post-surgery improvement, and attention improved in one of the studies. In contrast, more recent work by Lightle et al (Reference Lightle, Zheng and Makris2024) showed improvement post-surgery relative to the general population across a neuropsychological battery (BrainCheck). The sub-analysis showed improvement in executive functioning specifically, with adjustment for ethnicity, gender, diabetes, hypertension, hypothyroidism, history of renal calculi and osteoporosis. Nevertheless, this study did not account for depression or anxiety as possible confounders. Lourida et al (Reference Lourida, Thompson-Coon and Dickens2015) were correctly concerned by the lack of control groups in earlier post-surgical studies and that testing was completed too early, so that the effects of surgery were difficult to differentiate from practice effects. Some more recent studies did examine patients later after surgery. They show improvements on the Mini-Mental State Examination (MMSE) at 2 months (Wang Reference Wang, Xin and Zhao2023) and 6 months post-operatively (Trombetti Reference Trombetti, Christ and Henzen2016). Nevertheless, studies lack sufficient control groups or examination of medical and psychological confounding symptoms to be fully conclusive.
Although earlier work tended to focus on the potential impact of surgery, more recent work by Koman et al (Reference Koman, Bränström and Pernow2021) demonstrates that there may be a beneficial effect of calcimimetic therapy alongside surgery, with benefits measured by the Montreal Cognitive Assessment (MoCA) after 4 weeks of calcimimetic therapy, and then at 6 weeks and 6 months post-operatively (n = 110). Reference Koman, Bränström and PernowKoman et al found a positive response to cinacalcet to be a predictor of improvement post-parathyroidectomy.
As noted in the earlier Lourida et al (Reference Lourida, Thompson-Coon and Dickens2015) review, there remains an ongoing issue that few studies of cognition adjust or control for age, gender, education, anxiety, depression, or calcium and vitamin D levels. Like Lourida et al (Reference Lourida, Thompson-Coon and Dickens2015), we agree that there is certainly a suggestion from these pre- and post-surgical studies that surgery improves at least some cognitive domains, and in particular some memory tests, which is highly clinically relevant for patients and their clinicians. However, to be conclusive about this, more robust research is needed involving larger numbers, at least 6-month follow-up post-surgery to avoid practice effects, and appropriate adjustments for calcium levels, vitamin D levels, age, gender, education, and medical and psychiatric comorbidities. We suggest that future studies should include both bedside tests to examine for obvious cognitive changes and which could be utilised by all clinicians, and more sophisticated neuropsychological batteries to examine for more subtle changes. In addition, future studies need to be multicentre with a matched non-cancer thyroid control groups to consider medical and psychological confounding factors and matched healthy controls to determine whether neuropsychological function is significantly impaired.
Lithium-associated hyperparathyroidism
Lithium has a long history of use for mood disorders, although there is evidence that it has recently been underused owing to concerns about side-effects. Hypercalcaemia can emerge as a side-effect at any point of treatment (Meehan Reference Meehan, Udumyan and Kardell2018), with an estimated prevalence of 10% in longer-term users (Szalat Reference Szalat, Mazeh and Freund2009). This is usually asymptomatic or mild and is associated with an inappropriately normal or elevated parathyroid hormone level.
Lithium-associated hyperparathyroidism (LAH) occurs in around 4–6% of patients taking the medication (Szalat Reference Szalat, Mazeh and Freund2009) and occurs at a female:male ratio of 3:1 (McHenry Reference McHenry and Lee1996). The absolute risk of PHPT is 100 times greater with lithium use (10%) compared with risk in the general population (0.1%).
Underlying mechanisms
The mechanisms underlying the occurrence of hyperparathyroidism with lithium use are poorly understood. There are three theories currently in contention. According to the set-point theory, lithium disrupts calcium-sensing receptors (CaSR) on the parathyroid glands, increasing the calcium set point at which suppression of parathyroid hormone release occurs. This compromises sensitivity to negative feedback, with a net effect of increased gland activity for any given serum calcium level (Shen Reference Shen and Sherrard1982; Lehmann Reference Lehmann and Lee2013). Another theory suggests that lithium aggressively ‘unmasks’ a parathyroid gland's existing predisposition for disease (Nordenström Reference Nordenström, Strigård and Perbeck1992; Livingstone Reference Livingstone and Rampes2006; Meehan Reference Meehan, Humble and Yazarloo2015). Finally, a third theory suggests that lithium directly stimulates increased parathyroid hormone secretion which, over time, results in gland hyperplasia. Supporting this theory, one study demonstrated that mean parathyroid volume was three times larger in long-term users of lithium (more than 3 years) compared with short-term users (less than 6 months) and healthy controls (Mallette Reference Mallette, Khouri and Zengotita1989).
Prevalence and monitoring
Studies have correlated lithium use with increased serum calcium and parathyroid hormone levels (Christiansen Reference Christiansen, Baastrup and Lindgreen1978). The largest comprehensive review monitored 423 lithium users in two different locations (Meehan Reference Meehan, Humble and Yazarloo2015). Of these, 18% (n = 77) were identified as suffering from LAH. Those with LAH had a median age of 65 years and the majority were women (n = 58). Around 20% of patients receiving lithium treatment experienced an episode of hypercalcaemia. On average, parathyroid hormone levels were 32 ng/L higher in patients with LAH than in those without. Furthermore, a positive correlation was identified between duration of treatment and the risk of developing LAH. The study's authors advocate for long-term clinical surveillance of female lithium users and acknowledge that their results did not account for the effects of polypharmacy (Meehan Reference Meehan, Humble and Yazarloo2015).
Most current guidelines on lithium prescribing recommend monitoring of patients, including calcium levels, every 3 months in the first year and then 6 monthly as a minimum during the maintenance phase and more often if calcium is raised. This is even more relevant with ageing and in women. In National Health Service practice in the UK, endocrinologists will usually continue to monitor patients with LAH. In patients who have been on lithium for many years, parathyroid hormone-dependent hypercalcaemia is unlikely to resolve with dose reduction or cessation of the drug, and reduction or cessation are often undesirable when weighing up the risk of deterioration in their mental health. Lithium-associated hyperparathyroidism is best managed by endocrinologists. Surveillance with cinacalcet treatment, if indicated, is often preferred over parathyroidectomy as most patients will have multi-gland disease.
Management of suspected primary hyperparathyroidism
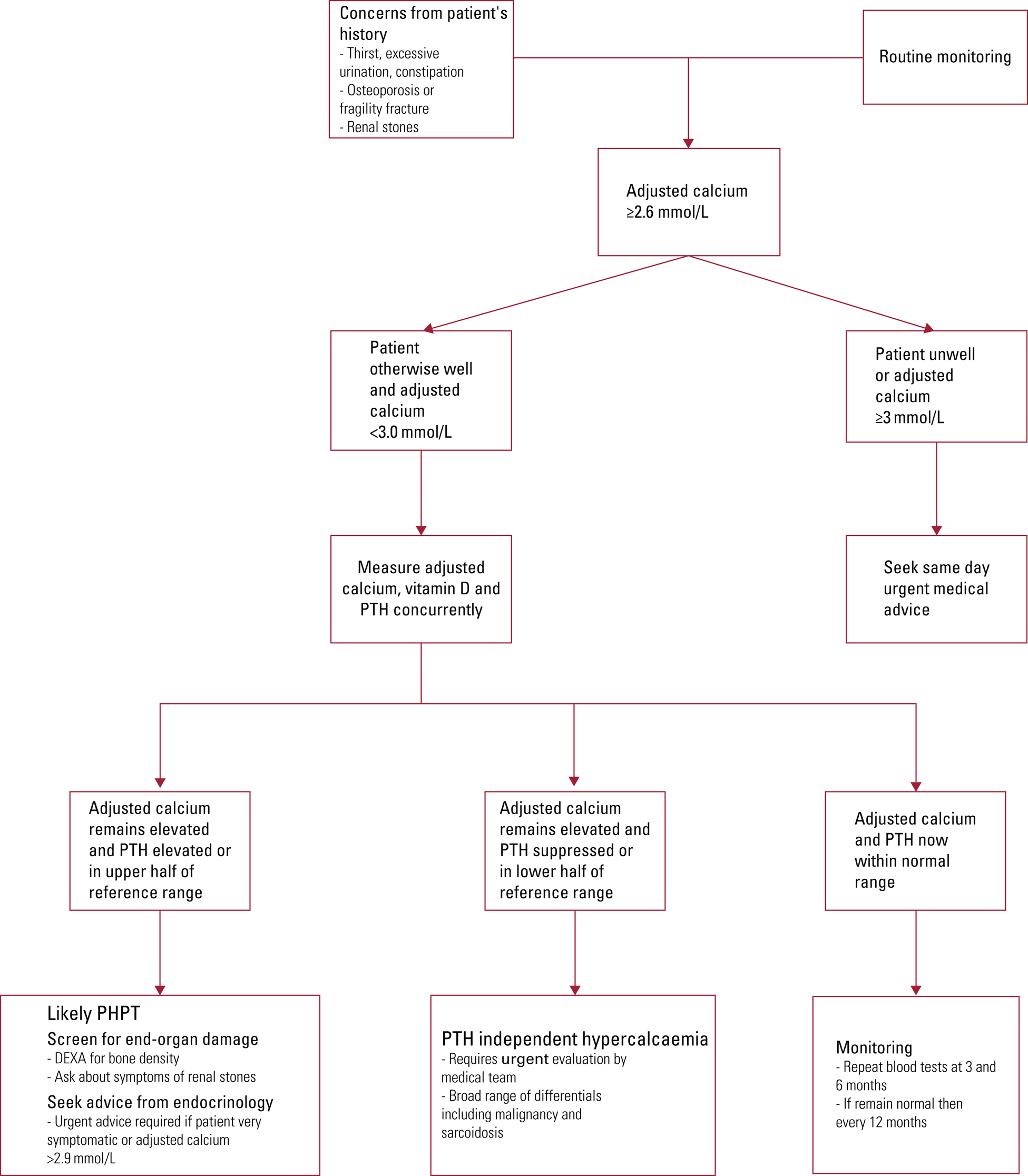
A psychiatrist may suspect PHPT owing to concerns about their patient's general health or because of an incidental finding of hypercalcaemia as part of routine blood monitoring. A proposed algorithm for the psychiatrist to manage the condition is outlined in Fig. 1.
Protocol for the management of suspected hyperparathyroidism for psychiatrists. DEXA, dual-energy X-ray absorptiometry; PTH, parathyroid hormone; PHPT, primary hyperparathyroidism. Based on guidelines developed by the American Association of Endocrine Surgeons (Wilhelm Reference Wilhelm, Wang and Ruan2016) and the National Institute for Health and Care Excellence (2019).

Patients who are medically unwell or who have a new finding of an adjusted calcium level above 3 mmol/L should be discussed urgently with a medical specialist.
If the adjusted calcium levels remain persistently elevated (≥2.6 mmol/L), although not dangerously so, then serum parathyroid hormone, vitamin D and calcium levels should be checked again concurrently, i.e. on the same day. In addition, if vitamin D levels are low (<30 nmol/L) or insufficient (<50 nmol/L), it is recommended that supplements are offered (NICE2019).
Further specialist management
Endocrinologists confirm the diagnosis of PHPT and screen for complications by taking a careful history to look for symptoms of hypercalcaemia, dual-energy X-ray absorptiometry (DEXA) scanning of the lumbar spine, distal radius and hip to screen for low bone density, as well as ultrasound of the renal tract if kidney stones are suspected. Patients will also be screened for factors that may point towards a genetic cause. In 3–5% of cases of PHPT there may be an inherited cause that warrants further investigation, such as multiple endocrine neoplasia type 1.
There is broad consensus that surgery remains the best and only definitive treatment for PHPT when indicated. Current NICE criteria for surgical intervention include symptoms such as thirst, frequent or excessive urination or constipation, as well as end-organ disease (e.g. renal stones, fragility fractures or osteoporosis) or an adjusted serum calcium level of 2.85 mmol/L or above (NICE 2019). Surgery is also generally recommended in patients presenting under the age of 50. Patient preference and comorbidities are considered when evaluating the suitability of surgery. Antidepressants should be considered by psychiatrists or in general practice to treat depression and/or anxiety disorders pre-surgery and ongoing use post-surgery should be re-evaluated. Patients with PHPT symptoms tend to experience clear benefit from parathyroidectomy, and patients who do not experience classic symptoms of PHPT do also tend to report improvements in quality of life post-surgery (Wilhelm Reference Wilhelm, Wang and Ruan2016). Although NICE does not include depression as an indication for surgery, there is a consensus among panels who have developed guidance that non-specific symptoms such as depressive symptoms and fatigue do appear to improve after surgery, making it a potentially cost-effective intervention to prevent further deterioration in health (National lnstitute for Health and Care Excellence 2019).
For those who are unwilling or unable to have surgery, observation can be considered. This should include annual biochemical monitoring and DEXA scans every 2–3 years, as there is evidence that bone mineral density reduces over time with untreated PHPT. Specific treatment can be considered with cinacalcet, a calcimimetic agent that inhibits parathyroid hormone secretion. This is indicated for those with adjusted calcium levels above 2.85–2.90 mmol/L (depending on local agreed protocols) and symptoms of hypercalcaemia, or those with adjusted calcium above 3.0 mmol/L, irrespective of their symptom status. Cinacalcet should be initiated by an endocrinologist. Bisphosphonates are also considered in people with PHPT who have an increased fracture risk (Wilhelm Reference Wilhelm, Wang and Ruan2016; NICE2019).
Case vignettes
The following fictitious case vignettes illustrate various presentations of hyperparathyroidism on an old age psychiatry ward.
Case 1
Mrs A, an 89-year-old woman with no history of depression, presented with confusion, aggression and low mood to an acute medical hospital. She was investigated for her acute confusion and found to have significant hypercalcaemia with an adjusted calcium level of 2.9 mmol/L (normal range 2.2–2.6 mmol/L) and raised parathyroid hormone level of 14 pmol/L (normal range 1.48–7.63 pmol/L). Her vitamin D levels were in the normal range.
Mrs A was reviewed by an endocrinologist, who confirmed the diagnosis of primary hyperparathyroidism (PHPT). She was treated urgently with cinacalcet and her confusion and aggression improved. Her calcium levels improved to 2.4 mmol/L, which is within the normal range. She had liaison psychiatry input for her mood, which remained depressed and she was suicidal, and she was transferred to an acute psychiatric ward for further management of her depression.
She was reviewed by an endocrinologist a month into her psychiatric admission. They explained to her that she had PHPT and that mood disorder was often driven by hypercalcaemia, which was now normal on cinacalcet. The possibility of surgery was discussed with her, but she was not keen on this at her advanced age. She had responded well to cinacalcet so was felt to be unlikely to benefit greatly from surgery in terms of her mood. She was offered ongoing follow-up by the endocrinology clinic. Over several months Mrs A gradually improved from her depression on venlafaxine and aripiprazole. She remained normocalcaemic on cinacalcet.
Case 2
Mr B, a 70-year-old man, presented to an in-patient old age psychiatry service with severe depression in the context of a bipolar disorder and hyperparathyroidism. The latter was diagnosed on completing routine admission bloods. His psychiatric history included a severe suicide attempt in the context of depression at the age of 25, with an episode of mania a year later, after which he had been started on lithium. He had remained on lithium since that episode (he recalled being told to ‘never stop the lithium’ by his psychiatrist) but continued to be symptomatic all his life. Unfortunately, his bipolar disorder became even more turbulent with age.
Despite the development of lithium-associated hyperparathyroidism (LAH) in later life, he did not want to consider stopping lithium and refused parathyroidectomy. His endocrinologists prescribed cinacalcet, which controlled his hypercalcaemia. He made a slow recovery from his depression with a combination of low doses of lithium, antidepressant treatment, antipsychotics and psychology input.
Case 3
Mrs B, a 68-year-old woman with a long-standing history of schizophrenia, had stopped her regular long-acting injectable antipsychotic 6 months prior to admission. She was detained in a psychiatric hospital for becoming increasingly anxious about neighbours, whom she accused of shining lights into her house every night and interfering with the sewers. She had started to shout and swear at them and threatened to harm them. She had also not been eating well and neglecting her self-care for several months.
Routine blood tests on admission revealed an adjusted calcium level of 2.69 mmol/L and elevated parathyroid hormone level of 18.9 pmol/L, consistent with primary hyperaparathyroidism. With further investigation of her vitamin D levels, she was noted to be deficient at 12 nmol/L. A decision was made to start her on standard replacement doses of vitamin D (cholecalciferol 1000 IU once daily) because of the risk of exacerbating hypercalcaemia with high-dose replacement therapy. After 4 months of cholecalciferol her vitamin D was sufficient at 59 nmol/L, her parathyroid hormone level had reduced to the upper limit of normal at 8 pmol/L and her calcium had remained similarly mildly elevated at 2.70 mmol/L. She started to feel better. Her psychosis improved on a long-acting injectable antipsychotic and she returned home with support of the community psychiatric team and a package of care. The psychosis was not considered to be related to her initially raised calcium levels.
Conclusions
Psychiatrists need to be vigilant for hyperparathyroidism, which may easily go undetected unless serum-adjusted calcium levels and subsequent parathyroid hormone levels are investigated. The prevalence of primary hyperparathyroidism (PHPT) is higher in older people, especially in women.
In PHPT, moderate to severe depressive symptoms occur pre-parathyroidectomy in roughly a quarter of individuals and approximately two-thirds improve a year after surgery. We would advocate that depression is taken into account when considering indications for surgery, provided patients are carefully counselled regarding the poor-quality evidence in this area. Further research is needed to guide antidepressant treatment, particularly regarding when to withdraw this post-surgery if the depression may be attributed to PHPT.
In our view, the pre- and post-parathyroidectomy studies for PHPT demonstrate that some cognitive domains may improve post-surgery, although findings regarding which domains improve remain inconsistent across studies. More recently, there is a suggestion that a response to cinacalcet may predict improvement after parathyroidectomy, although this requires further study. Further research is needed in larger sample sizes, incorporating testing completed pre-operatively and at least 6 months post-operatively to be more conclusive regarding whether there is improvement in cognition, independent of mood changes. The research on the longer-term effects of having chronically raised parathyroid hormone over 10–20 years has methodological constraints preventing conclusive statements, but suggests that parathyroid hormone alone is unlikely to have an independent effect on cognitive decline.
Data availability
Data sharing is not applicable to this article as no new data were created or analysed in this study.
Acknowledgements
We thank Trisha Moore, librarian at Fulbourn Hospital, Cambridgeshire and Peterborough NHS Foundation Trust (CPFT), for her invaluable support in helping with the literature search and access needed to read papers for this article. We also thank Dr Marija Farrugia, consultant psychiatrist, CPFT, for her earlier support and discussion of the article.
Author contributions
S.S.: conceptualisation, writing, reviewing, redrafting, editing. V.S.: redrafting, reviewing, editing. A.H.E.K.: conceptualisation, redrafting, reviewing, editing. J.S.R: conceptualisation, writing, reviewing, editing and supervision.
Funding
This work received no specific grant from any funding agency, commercial or not-for-profit sectors.
Declaration of interest
None.
Multiple choice questions
Select the single best option for each question stem:
1 For which of the following indications do the NICE guidelines recommend surgery in people with PHPT?
a psychosis
b mild depression
c osteoporosis
d dementia
e fatigue.
2 Which of the following symptoms is a feature of PHPT?
a brittle nails
b weight loss
c renal stones
d tachycardia
e night sweats.
3 Lithium-induced hyperparathyroidism:
a presents with different biochemical features to primary hyperparathyroidism
b usually emerges in the first month of treatment
c is more common in men taking lithium
d should be discussed with an endocrinologist
e should lead to immediate cessation of lithium.
4 For a patient with depression and an adjusted calcium of 2.7 mmol/L, the most appropriate option would be:
a immediate referral for surgery
b urgent referral for in-patient medical management
c identifying whether they are taking calcium supplements and stopping these if present
d testing the patient's vitamin E levels
e initiation of cinacalcet immediately.
5 As regards patients with PHPT going for parathyroidectomy surgery:
a depression occurs in one-third to two-thirds of patients
b depression always resolves post-surgery
c studies show that surgery leads to resolution of dementia
d psychiatric symptoms are currently part of the NICE criteria for surgery
e stopping antidepressants is recommended.
MCQ answers
1 c 2 c 3 d 4 c 5 a



eLetters
No eLetters have been published for this article.