Highlights
-
Multiple sclerosis (MS) imposed an additional annual healthcare cost of $15,016 per person compared with controls.
-
$218 million/year in healthcare costs may be attributable to MS in Alberta.
-
The larger economic impact associated with greater disability among those living with MS underscores the importance of preventing/delaying disease progression in MS.
Introduction
Multiple sclerosis (MS) is a chronic disorder of the central nervous system. This disorder typically begins between the ages of 20 and 50 years, primarily affecting females, and is lifelong. 1 MS is the most common nontraumatic disabling neurological condition among working-age adults in Canada. Reference Trisolini, Honeycutt, Wiener and Lesesne2 The prevalence of MS in Canada is one of the highest in the world, with the province of Alberta reported to have a particularly large population living with MS (310 cases per 100,000 population). Reference Walton, King and Rechtman3–Reference Balcom, Smyth and Kate5 The most common form of MS is relapsing-remitting, in which individuals experience periods of neurological disability followed by complete or partial recovery over weeks to months. Reference Dutta and Trapp6 Some features of MS that negatively impact the physical and psychosocial well-being of people living with MS (pwMS) and increase healthcare resource utilization and associated costs include the frequency and severity of relapses and disability level. Reference Nicholas, Zhou and Deshpande7–Reference Gil-González, Martín-Rodríguez, Conrad and Pérez-San-Gregorio9
PwMS require complex care management involving pharmacological and nonpharmacological interventions to control symptoms, delay disease progression or accumulation of disability and manage comorbid conditions that are commonly present. Reference Marrie10 Consequently, pwMS utilize more healthcare services compared with those without MS, and advancing disease severity is associated with additional utilization and associated costs. Reference Amankwah, Marrie and Bancej11,Reference Schriefer, Haase, Ness and Ziemssen12 Relatively few studies have been conducted on the healthcare cost of MS in Canada; Reference Amankwah, Marrie and Bancej11,Reference Asche, Ho, Chan and Coyte13–18 even fewer have been conducted in the past decade, Reference Amankwah, Marrie and Bancej11,Reference Khakban, Rodriguez Llorian and Michaux17 during which numerous disease-modifying therapies (DMTs) have been introduced. DMTs are the current pharmacological standard of care for pwMS based on evidence that these treatments reduce the frequency and severity of relapses and may reduce disability over the long term. Reference Harding, Williams and Willis19–Reference Spelman, Magyari and Piehl21 A contemporaneous estimate of the healthcare cost of MS is needed to support decision and policymakers and prioritize resources. The objectives of this study were to estimate the incremental direct healthcare cost of MS among adults and according to disability level among pwMS in Alberta, Canada.
Methods
Ethics approval was received from the University of Alberta Research Ethics Board (Pro00116074) and the University of Calgary Conjoint Health Research Ethics Board (pSite-21-0031). No study participants were placed at risk, and a waiver of consent was applied. Data custodian approvals were received from Alberta Health and Alberta Health Services for the use of administrative health data for this study. This study was reported according to the Reporting of Studies Conducted Using Observational Routinely Collected Health Data guidelines. Reference Benchimol, Smeeth and Guttmann22
Study design
This retrospective, observational, population-based cohort study was conducted using administrative health data from Alberta between April 1, 1993, and March 31, 2021. Adult residents of Alberta living with and without MS on April 1, 2019 (index date), were included. Data back to April 1, 1993, were used for determining cohort selection and baseline characteristics, and a 1-year post-index observation period was used for determining outcomes (April 1, 2019, to March 31, 2020).
Data sources
Canadian provinces provide publicly funded health care for all residents. In Alberta, the fourth most populous Canadian province (4.4 million people in 2019/2020), 23 health care is administered under the Alberta Health Care Insurance Plan (AHCIP), of which over 99% of Albertans participate. Reference Jin, Elleho, Sanderson, Malo, Haan and Odynak24 A person-level data extract from the Discharge Abstract Database (DAD), National Ambulatory Care Reporting System (NACRS), Practitioner Claims (data available from January 1, 1994, onward), Alberta Continuing Care Information System (ACCIS), National Rehabilitation Reporting System (NRS), Pharmaceutical Information Network (PIN) and Vital Statistics was linked to the Population Registry using a unique individual identifier (Personal Health Number) and then deidentified and provided to the researchers by the data custodians. DAD and NACRS include demographic, administrative, diagnostic, procedural and resource intensity weight information on people discharged from hospital (DAD), emergency department (ED) and facility-based ambulatory care clinics (NACRS). Diagnostic fields for each visit include the most responsible diagnosis and room for up to 24 (DAD) and 9 (NACRS) secondary International Classification of Disease – version 10 – Canadian Enhancement (ICD-10-CA) codes. Physician visits were obtained from the Practitioner Claims database that includes patient, provider and service information such as demographics, physician specialty, date of service, amount paid to the service provider (on fee-for-service, alternative payment plan physician billing and shadow billing) and health service and diagnostic codes; up to three ICD – version 9 – Clinical Modification (ICD-9-CM; Alberta specific) diagnostic codes can be used per visit. ACCIS contains information on long-term care and professional community home care; elements include demographics, admission and discharge information and resource utilization groupers. NRS contains data on adult inpatient rehabilitation facilities and programs. The PIN contains information on all dispensed prescription medications from community pharmacies (including both retail and specialty). Vital statistics contains information on all events related to an individual’s entrance and departure from life. The Provincial Registry contains demographic information for all Albertans with AHCIP coverage; elements include migration in and out of the province and birth and death indicators. Records that were duplicates or contained an invalid Personal Health Number were discarded. Variables were checked for missing data and inconsistencies; inconsistent data were corrected using data logic or information majority.
Cohort selection
The MS cohort included those who (1) met a validated case definition for MS, defined as having ≥ 1 hospitalization (from April 1, 1993, onward) or ≥ 5 ambulatory care visits (from April 1, 1998, onward) and/or physician visits (from January 1, 1994, onward) with a recorded code for MS (ICD-10-CA G35, ICD-9-CM 340) located in any diagnostic field within a 2-year period between April 1, 1993, and March 31, 2021 (multiple outpatient visits by an individual within the same day were considered as one visit for case definition purposes); Reference Widdifield, Ivers and Young25 (2) had an MS incident date, defined as the first healthcare encounter with a recorded diagnostic code for MS or a related demyelinating disease of the central nervous system with none occurring ≥ 5 years beforehand (see Supplementary Table 1), occurring before the index date; (3) were aged ≥ 18 years and alive on the index date; and (4) had AHCIP coverage for ≥ 2 years before the index date and ≥ 1 year after the index date or until death whichever occurred first.
The case definition used in this study to identify pwMS was validated in Canada using electronic medical records linked to administrative data and resulted in high sensitivity (84%), specificity (100%) and positive predictive value (86%). Reference Widdifield, Ivers and Young25 This algorithm provided the shortest time interval (i.e., 2 years) to achieve > 80% for both sensitivity and positive predictive value compared with the other tested options (e.g., ≥ 1 hospitalization or 1–10 claims within 1–20 years) and can accurately identify pwMS using administrative data. Reference Widdifield, Ivers and Young25
The control cohort (adult residents of Alberta not living with MS) included randomly selected individuals from those who (1) were alive and aged ≥ 18 years on the index date; (2) did not have a hospitalization (from April 1, 1993, onward), ambulatory care visit (from April 1, 1998, onward) and/or physician visit that contained an MS code between April 1, 1993, and March 31, 2021; (3) did not have a DMT dispensation between April 1, 2008 (date from which data were available in PIN) and March 31, 2021; and (4) had AHCIP coverage for ≥ 5 years before the index date and ≥ 1 year after the index date or until death whichever occurred first.
Study measures
Sociodemographic characteristics recorded on the index date included age, sex, urban/rural residence (based on postal code) and Pampalon material deprivation index (includes education, employment status and average income); this index was derived from the Alberta general population at the dissemination area level that was linkable to postal code and presented based on quintiles from most well-off (quintile 1) to most deprived (quintile 5). Reference Pampalon, Hamel, Gamache and Raymond26 Clinical characteristics included the Charlson Comorbidity Index and specific MS-related comorbidities; Reference Magyari and Sorensen27,Reference Marrie, Patten and Tremlett28 the number of years living with MS (time between the MS incident date and the index date) and disability level were reported among the MS cohort. A Charlson Comorbidity Index score was determined during the 2-year pre-index period that was based on ICD-10-CA and ICD-9-CM codes of 17 different specific medical conditions weighted according to their potential for influencing mortality (Supplementary Table 2). Reference Charlson, Pompei, Ales and MacKenzie29,Reference Lix, Smith and Pitz30 MS-related comorbidities included anxiety, Reference Marrie, Fisk and Yu31 cardiovascular disease (atrial fibrillation, chronic heart failure, coronary artery disease, peripheral artery disease and stroke), 32–Reference Tu, Mitiku, Lee, Guo and Tu36 chronic obstructive pulmonary disease (COPD), Reference Gershon, Wang, Guan, Vasilevska-Ristovska, Cicutto and To37 depression, Reference Doktorchik, Patten and Eastwood38 diabetes Reference Hux, Ivis, Flintoft and Bica39 and hypertension; Reference Tonelli, Wiebe and Fortin35 each participant was classified with respect to the presence or absence of these conditions as measured during the 2-year period before the index date (Supplementary Table 3). A validated algorithm was used to estimate Expanded Disability Status Scale (EDSS) scores using age, specific healthcare service use (home care, long-term care and inpatient rehabilitation) and health conditions (visual disturbance, other paralytic syndromes and spasticity; Supplementary Table 4). Reference Kurtzke40,Reference Marrie, Tan, Ekuma and Marriott41 Disability level was defined in this study as mild (EDSS ≤ 3.5), moderate (EDSS 4–6.5) and severe (EDSS ≥ 7).
During the 1-year post-index observation period, healthcare resource utilization and costs were determined for acute care (hospitalizations, ED visits), outpatient care (ambulatory care, physician visits), supportive care (long-term care admissions, home care services) and pharmacy dispensed prescription medications (overall and subgrouped into DMTs [Supplementary Table 5] and all others). Acute and ambulatory care costs were derived by multiplying the associated resource intensity weight with the Canadian Institute for Health Information (CIHI) standardized cost for Alberta in 2019/2020. 42 Resource intensity weight is a measure to estimate healthcare resource use and represents the relative value of resources that a given patient, contingent on diagnostic case-mix, would be expected to consume relative to a standard patient; CIHI provides standardized average costs incurred through the direct care of a standardized patient. 43 Physician visit costs were based on the actual amount paid. Time residing in long-term care (e.g., nursing homes, auxiliary hospitals) was measured and cost estimated based on the average daily cost ($230.36 per day; from Alberta Health) of all such facilities in Alberta. Reference Tonelli, Wiebe and Joanette44 The total hours of home care encounters were measured, and the provider type was identified; estimated costs were based on the hourly wage of service providers in Alberta. 45 Drug costs were calculated using the drug product identification number and quantity dispensed, combined with the drug list price (from Alberta Blue Cross); a 3% per unit markup and a $12.15 dispensing fee were included. 46,47 Costs were reported in 2021 Canadian dollars ($CDN). 48
Statistical analyses
Descriptive statistics were reported as counts and percentages, means with standard deviations (SD) or medians with interquartile ranges (IQR), where appropriate. One- and two-part generalized linear models (GLM) were employed to examine cost differences. Function and distribution were determined based on results from several tests (Pearson correlation test, Pregibon link test, modified Hosmer and Lemeshow test, modified Park’s test). When minimal or absent zero cost values were present, a one-part GLM model with a gamma distribution and log-link function was used, producing cost ratios. When cost outcomes had prevalent zero values, a two-part GLM approach was adopted. Reference Duan, Manning, Morris and Newhouse49 The first part involved logistic regression to predict the odds of observing a nonzero cost (corresponding to the odds of having a cost occurrence), yielding odds ratios that quantify relative differences in odds of nonzero cost. The second part, conditional on a nonzero cost, involved a GLM with a gamma distribution and log-link function to predict the positive costs, producing cost ratios. Incremental cost (the incurred additional cost of pwMS compared to controls) was presented by cost ratios (accompanied by odds ratio in two-part models) and the difference between predicted costs using an average marginal effect approach. 50 The potential confounders of sociodemographic characteristics (age, sex, urban/rural residence and socioeconomic status) were included in the MS versus control model; sociodemographic characteristics and the number of years living with MS were included in the disability level model among pwMS. The healthcare cost attributable to MS in Alberta was estimated by multiplying the per person-year incremental cost of MS by the number of pwMS identified in this study. Analyses were performed using SAS 9.4 software (SAS Institute Inc., Cary, NC, USA) and Stata 18 (StataCorp LLC, College Station, TX, USA).
Results
Cohort selection
A total of 14,485 pwMS were identified on the index date, and 13,089 met the criteria for the MS cohort (Figure 1; Supplementary Figure 1 shows data linkages). Among the 3,238,045 individuals who met the criteria for the control cohort, approximately 11 were randomly selected for each individual within the MS cohort (n = 150,080); privacy compliance guidelines of the data custodians informed the number of controls. 51
MS and control cohort selection. AHICP = Alberta health care insurance plan; DMT = disease-modifying therapy; MS = multiple sclerosis; REG = the Provincial Registry.

Baseline characteristics
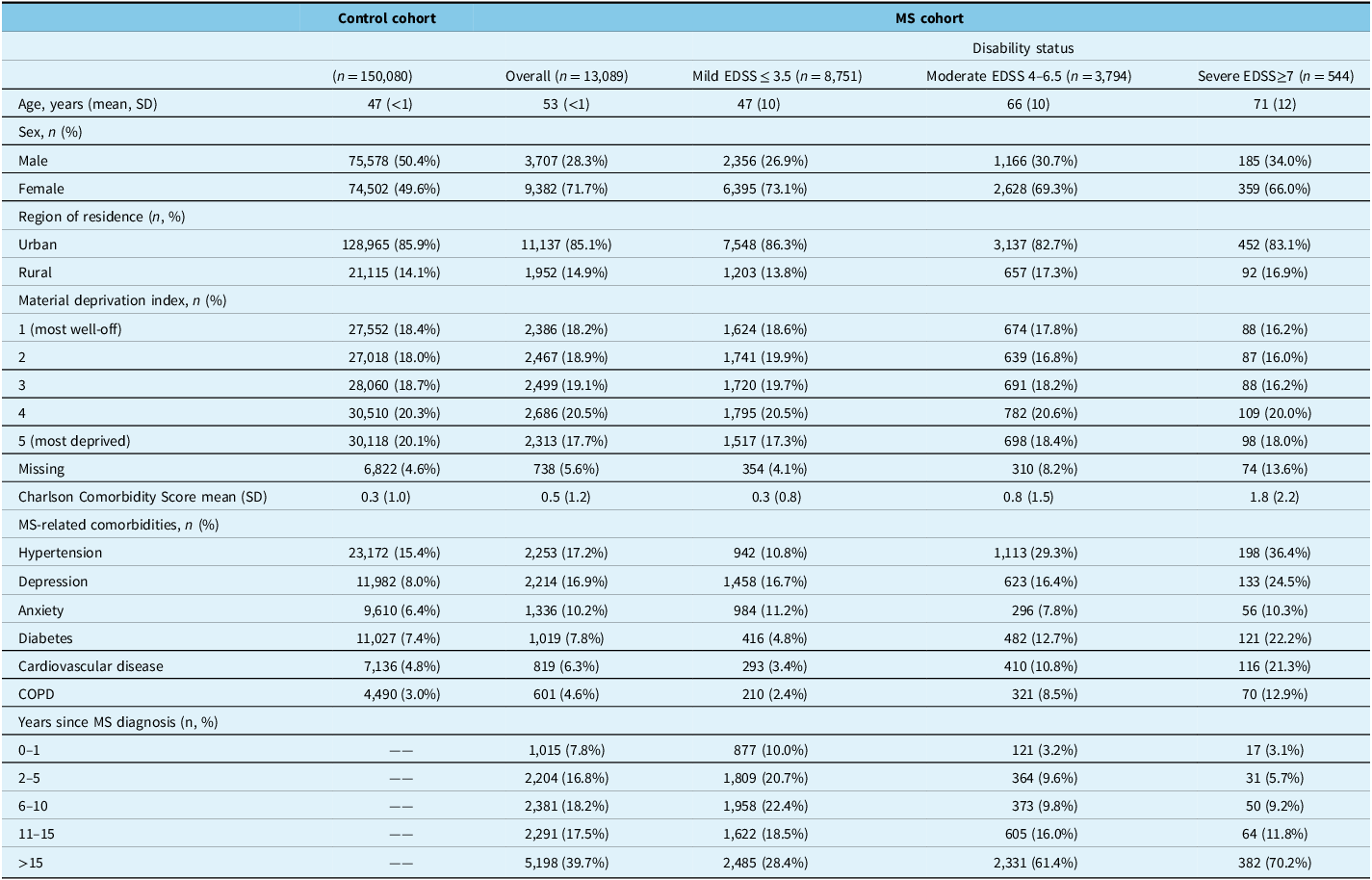
The MS cohort was older (53 [SD < 1] vs. 47 [SD < 1] years), predominantly female (71.7% vs. 49.6%), and experienced a higher overall burden of disease (Charlson Comorbidity Index score: 0.5 [SD 1.2] vs. 0.3 [SD 1.0]) than the control cohort (Table 1). The MS cohort was more likely to have hypertension (17.2% vs. 15.4%), depression (16.9% vs. 8.0%), anxiety (10.2% vs. 6.4%), cardiovascular disease (6.3% vs. 4.8%) and COPD (4.6% vs. 3.0%) compared with the control cohort (Table 1). Within the MS cohort, 24.6%, 35.7% and 39.7% had been living with MS for ≤ 5 years, 6–15 years and > 15 years, respectively (Table 1). Regarding disability status, 66.9% (n = 8,751) of the MS cohort had mild disability (EDSS ≤ 3.5; none had a score 0–1.5), 29.0% (n = 3,794) had moderate disability (EDSS 4–6.5) and 4.2% (n = 544) had severe disability (EDSS ≥ 7) (Table 1). Age, the overall burden of disease, the proportion living with specific MS-related comorbidities and the number of years living with MS were greater in those with more severe disability (vs. less disability) (Table 1).
Baseline characteristics

COPD = chronic obstructive pulmonary disease; MS = multiple sclerosis; SD = standard deviation.
Healthcare resource utilization
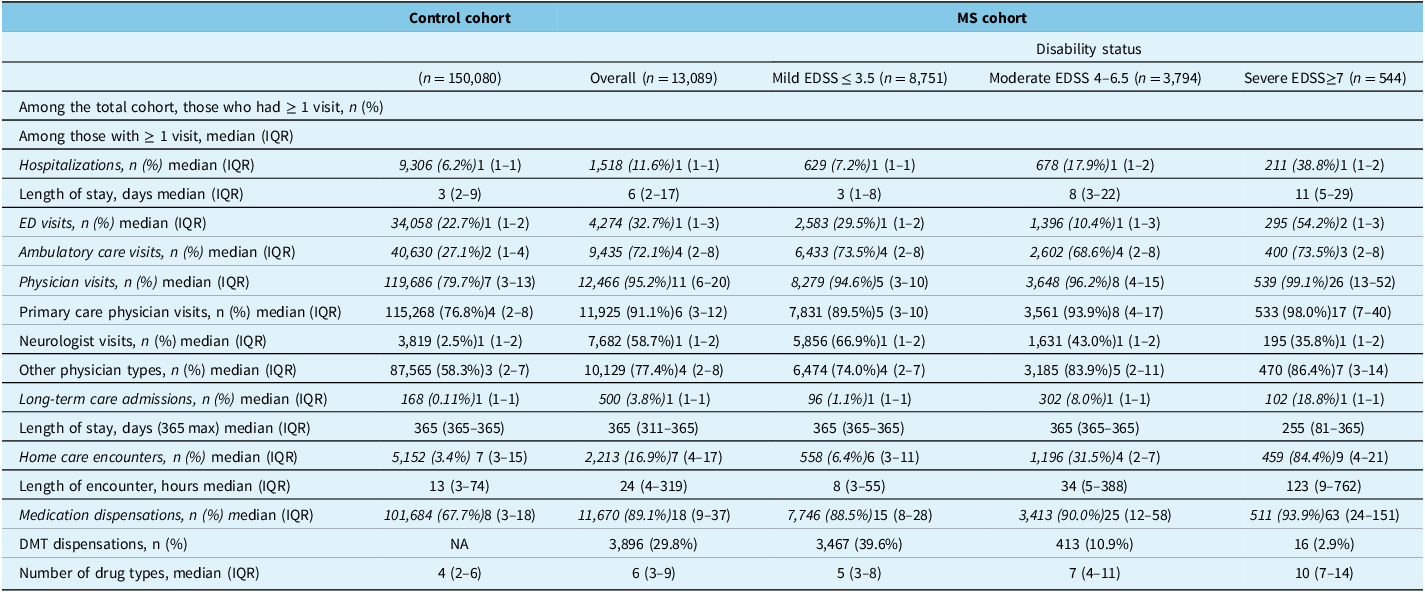
The MS cohort had a higher proportion with ≥ 1 hospitalization (11.6% vs. 6.2%), ED visit (32.7% vs. 22.7%), ambulatory care visit (72.1% vs. 27.1%), physician visit (95.2% vs. 79.7%), long-term care admission (3.8% vs. 0.1%) and home care encounters (16.9% vs. 3.4%) compared with the control cohort over the 1-year post-index observation period (Table 2). A greater proportion of the MS cohort also received ≥ 1 prescription medication dispensation (89.1% [29.8% received a DMT] vs. 67.7%) during the 1-year post-index observation period (Table 2).
Healthcare resource utilization during the 1-year post-index observation period

DMT = disease-modifying therapy; ED = emergency department; IQR = interquartile range; max = maximum.
Within the MS cohort, the proportion of those who had ≥1 hospitalization, ED visit, physician visit, long-term care admission and home care encounter was numerically greater among those with greater disability; those with moderate disability had a lower proportion with ambulatory care visits (68.6%) than those with lower or higher disability (73.5% each; Table 2). Among the different types of physicians, the proportion of those who visited primary care physicians and other types of physicians was greater, and those who visited neurologists were lower, among those with more severe disability (compared with those who had less disability) (Table 2). The proportion who received ≥ 1 DMT was greater in those with mild disability (39.6%) and lower in those with moderate (10.9%) and severe (2.9%) disability (Table 2).
Healthcare cost of multiple sclerosis
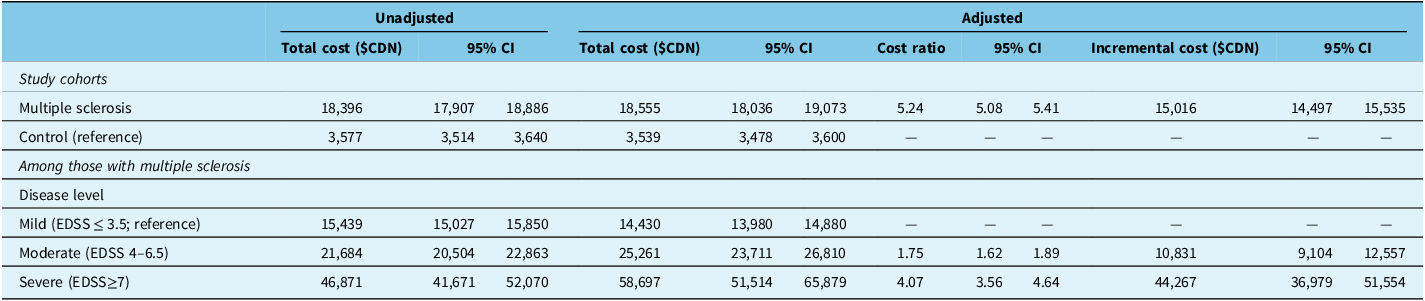
The total mean unadjusted healthcare cost of the MS cohort was $18,862 per person-year and $3,662 for the control cohort (Figure 2). Medication (43.5%) comprised the largest cost component of the total healthcare cost among the MS cohort, and physician visits (29.5%) and hospitalizations (28.4%) were the largest components among the control cohort (Figure 2). After adjusting for confounding sociodemographic factors (age, sex, urban/rural residence and socioeconomic status), total healthcare costs were 5.2 times higher (cost ratio: 5.24 [95% CI: 5.08, 5.41]) in the MS cohort versus the control cohort, with MS having a predicted incremental cost of $15,016 (95% CI: $14,497, $15,535) per person-year; the average adjusted annual per-person cost of MS was $18,555 (95% CI: $18,036, $19,073) versus $3,539 (95% CI: $3,478, $3,600) in the control cohort (Table 3).
Total mean unadjusted healthcare cost presented overall and by cost components. CDN = Canadian; DMT = disease-modifying therapy; ED = emergency department; EDSS = expanded disability status scale; MS = multiple sclerosis.

Total healthcare cost comparisons between the multiple sclerosis cohort and the control cohort

Individuals with a missing Pampalon material deprivation index were not included. Potential confounders that were adjusted for included age, sex, residence and socioeconomic status (multiple sclerosis cohort vs. control cohort), along with the number of years living with multiple sclerosis (moderate and severe vs. mild disability). Incremental costs (the incurred additional cost in pwMS compared to controls) were estimated using an average marginal effect approach based on predicted costs from generalized linear models with a log-link function and gamma distribution.
CDN = Canadian; CI = confidence interval; EDSS = expanded disability status scale.
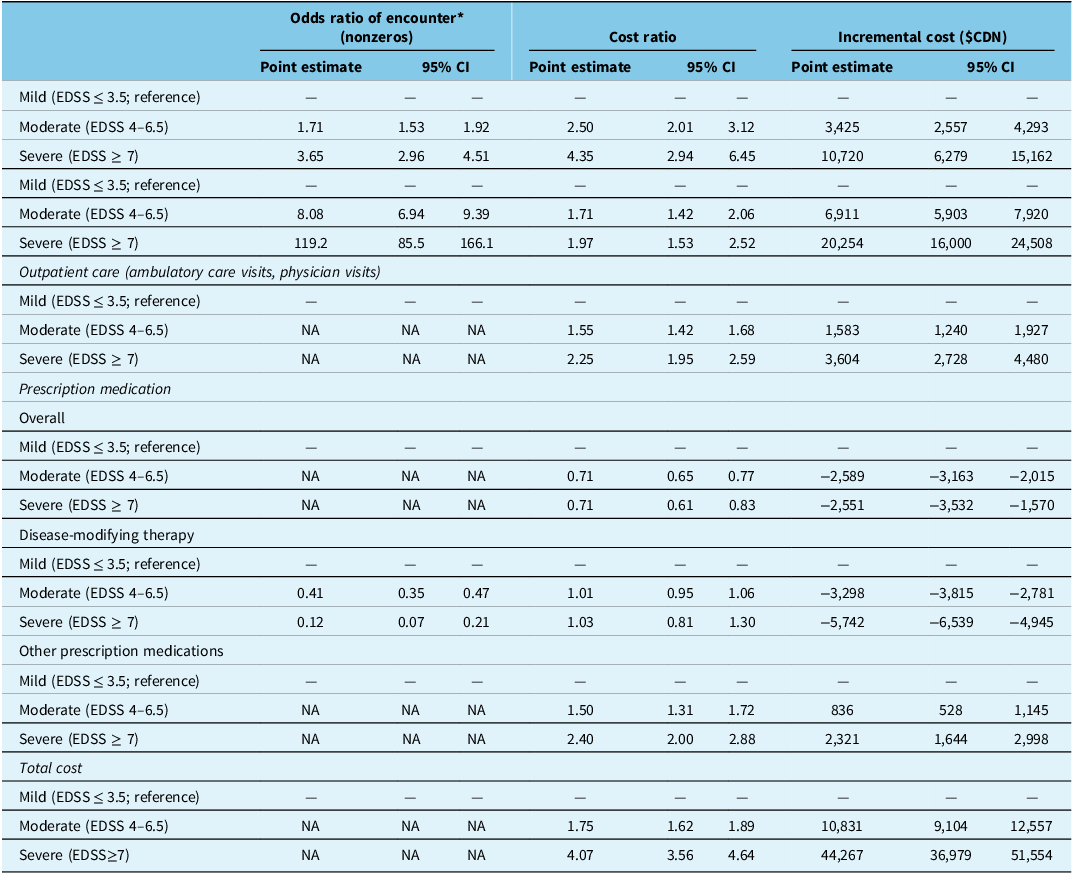
Within the MS cohort, the total mean unadjusted annual healthcare cost of those with mild disability was $15,594, moderate disability was $22,458 and severe disability was $46,353 (Figure 2). Medication (65.3% of total cost, of which DMTs encompassed 82.0%) comprised the largest cost component of those with mild disability; supportive care (long-term care and home care) was the largest cost component among those with moderate (40.1%) and severe disability (48.3%) (Figure 2). After adjusting for confounding sociodemographic factors and years living with MS, total healthcare costs were 1.8 times higher (cost ratio: 1.75 [95% CI: 1.62, 1.89]) for those with moderate disability and 4.1 times higher (cost ratio: 4.07 [95% CI: 3.56, 4.64]) for those with severe disability compared with mild disability (Table 4). The average adjusted annual per-person cost of pwMS with mild disability was $14,430 (95% CI: $13,980, $14,880) versus $25,261 (95% CI: $23,711, $26,810) for moderate disability and $58,697 (95% CI: $51,514, $65,879) for severe disability (Table 4). Acute care (hospitalizations, ED), supportive care (long-term care, home care) and outpatient care (ambulatory care, physician visits) contributed to the higher cost in those with greater disability, with supportive care being the primary driver; the cost of DMTs was lower in those with greater disability compared with those with mild or moderate disability (Table 4).
Healthcare cost comparisons of acute care, supportive care, outpatient care and prescription medications between disease severity levels within the multiple sclerosis cohort

* Estimated by gamma hurdle models (acute care, supportive care and disease-modifying costs) or a generalized linear model with log link and gamma distribution (outpatient care, overall and ‘other’ prescription medications and total costs). Incremental cost was the incurred additional cost of people living with multiple sclerosis compared to controls.
CDN = Canadian; CI = confidence interval, EDSS = expanded disability status scale; NA = not applicable.
Discussion
In this retrospective, observational, population-based cohort study of adults living with and without MS in Alberta, the incremental direct healthcare cost of MS and cost by disability level among pwMS was determined between April 1, 2019, and March 31, 2020, using administrative health data (reported in 2021 $CDN). The annual cost of MS was found to be more than five times higher than those not living with MS, with a predicted incremental cost of $15,016 per person-year. Extrapolating this cost to the population level, where 14,485 adults were identified as living with MS on the index date in this study (Figure 1), it is estimated that $218 million per year in healthcare costs were attributable to MS in Alberta during the observation period. This study also characterized the large economic burden associated with disability among pwMS, with total predicted direct healthcare costs greater by more than fourfold from $14,430 to $58,697 per person-year among pwMS with mild and severe disability, respectively; the primary cost component shifted from DMTs in mild disability to supportive care in moderate and severe disability. Collectively, this study provides insights into the healthcare costs associated with MS and the distribution of cost by levels of disability, highlighting the importance of preventing or delaying disability progression as an economic priority, in addition to being clinically significant and enhancing the health-related quality of life for pwMS.
Although Canada has one of the highest prevalence of MS in the world, relatively few studies have been conducted on the healthcare cost of MS in the country; Reference Amankwah, Marrie and Bancej11,Reference Asche, Ho, Chan and Coyte13–18 even fewer have been conducted in the past decade to capture the numerous DMTs and current pharmacological standard of care with this therapy. Reference Freedman, Devonshire and Duquette52 Among the more recent studies, Amankwah et al. (2017) applied a microsimulation model and found that the total direct healthcare cost, which included hospitalizations, physician services, prescription drugs and provincially funded supportive services (long-term and home care) and assistive devices, was estimated to be approximately $16,800 per person-year for pwMS aged 20 years and older (2011 CDN). Reference Amankwah, Marrie and Bancej11 The total direct healthcare cost of pwMS was similar to the current study when inflated to 2021 dollars (i.e., $18,782 CDN). 48 Recently, Khakban et al. (2023) conducted a retrospective population-based cohort study using administrative health data among 17,071 pwMS and 85,355 matched controls to determine the incremental healthcare cost of MS in British Columbia. Reference Khakban, Rodriguez Llorian and Michaux17 Based on inpatient, outpatient (ED and physician visits) and medication costs, the total excess cost of MS was estimated at $6,881 per person-year (2020 CDN). Reference Khakban, Rodriguez Llorian and Michaux17 The total incremental healthcare cost of MS estimated in the current study was more than twice as much, at $15,016 per person-year; this difference may be due to the more comprehensive capture of healthcare resources in this study, including ambulatory care, long-term care and home care. Of mention, the proportional contribution of medication and healthcare resources to the total direct healthcare cost of MS in the USA is similar to the current study but greater in terms of cost itself (e.g., $88,487 per person-year [2019 USD]). Reference Bebo, Cintina and LaRocca53,Reference Schauf, Chinthapatla, Dimri, Li and Hartung54
The extensive literature on the cost of illness in MS has shown that disability is a well-documented key driver of healthcare costs among pwMS; a significant increase in the total cost of MS, both direct and indirect, occurs with increasing disability from mild to severe, as measured by the EDSS. Reference Schriefer, Haase, Ness and Ziemssen12,Reference Kobelt, Thompson, Berg, Gannedahl and Eriksson55 This escalation in cost is coupled with shifts in the distribution of the economic burden of MS. Reference Patwardhan, Matchar, Samsa, McCrory, Williams and Li8,Reference Schriefer, Haase, Ness and Ziemssen12,Reference Kobelt, Thompson, Berg, Gannedahl and Eriksson55 However, large population-based studies using rigorous comparisons are very limited. Most studies use samples with relatively small numbers of participants and rely on self-reports of healthcare resource utilization, and recruitment occurs most often from specialized outpatient MS tertiary clinics, which introduces selection bias toward those with less severe disability and those more likely to use a DMT. Reference McKay, Tremlett, Zhu, Kastrukoff, Marrie and Kingwell56 Recognizing these limitations, studies conducted in a contemporaneous era consistently report DMTs as the main cost component at milder disability levels and supportive care or inpatient care as the primary cost driver at more severe disability levels. For example, Fogarty et al. (2014) recruited 214 pwMS from a specialized MS clinic and determined direct healthcare costs of inpatient, outpatient, medication, supportive care (long-term and home care), tests and assistive devices at different disease severity levels in Ireland. Reference Fogarty, Walsh, McGuigan, Tubridy and Barry57 The authors found that all cost categories were greater in those with severe disability (n = 27) compared with mild disability (n = 114), with the exception of medication and tests that were lower; the largest cost component of those with severe disability was supportive care followed by inpatient care. Reference Fogarty, Walsh, McGuigan, Tubridy and Barry57 Among 799 pwMS recruited from specialized MS and neurology clinics in Belgium (where almost half of the individuals received a DMT during the observation period), DMTs comprised 80% of the total direct healthcare cost in mild disability and 4% in severe disability; the cost of inpatient care was tenfold greater among those with severe disability compared with mild disability. Reference Kobelt58 Findings from the current study are consistent with previous reports; total direct healthcare costs were significantly greater at more severe disability levels, and the primary cost component shifted from DMTs in mild disability to supportive care in moderate and severe disability.
In the current study, the observed higher and lower DMT use and cost in those with mild and more severe disability, respectively, are in alignment with recommendations from the Canadian MS Working Group that state all individuals with relapsing-remitting MS should be encouraged to start treatment with a DMT soon after diagnosis (when disability is likely to be mild), and stopping a DMT can be considered among pwMS who are older than 60 years of age with prolonged stable disease. Reference Freedman, Devonshire and Duquette52,Reference Rae-Grant, Day and Marrie59 Older individuals appear to have an increased risk of infection and other adverse effects that may be due to age-related immunosenescence and therapy-induced alterations to the immune system, as well as a higher burden of comorbidities. Reference Graves, Krysko, Hua, Absinta, Franklin and Segal60 In this study, we found that those with mild disability had been living with MS for fewer years than those who had moderate and severe disability who in turn were older had a higher overall burden of disease and a greater proportion living with comorbidities. Other potential reasons for the observed lower DMT use among those with severe disability in this study may be attributed to a lesser perceived benefit given the already great amount of accrued disability, which is irreversible, and that provincial public coverage plans generally limit DMT coverage to those with an EDSS < 7.0. Recent studies have shown that early initiation of DMTs, particularly highly effective antibody-mediated therapies, reduces the frequency and severity of relapses and reduces disability, with the potential to lessen healthcare costs over the long term. Reference Harding, Williams and Willis19–Reference Spelman, Magyari and Piehl21,Reference Batcheller and Baker61 Further research is needed to delineate the cost-effectiveness of MS treatments aimed at delaying the progression of MS and reducing the frequency of relapses. Reference Navarro, Ordóñez-Callamand and Alzate62
Important strengths of this study are the large population-based design and high-quality source of administrative health data that contains information on comprehensive healthcare resources in Alberta. However, this study is also subject to a number of limitations that should be taken into consideration when interpreting results. Retrospective administrative claims-based studies use administrative data as opposed to medical records, and therefore, there is a potential for misclassification of the study groups or measures. To minimize the possibility of including individuals in the MS cohort who did not have the disease, a case-finding algorithm for MS was applied in the current study that was validated in Ontario and resulted in high sensitivity (84%), specificity (100%), positive predictive value (86%), negative predictive value (100%) and kappa (0.85). Reference Widdifield, Ivers and Young25 Although a validated algorithm was used to estimate the level of disease severity among pwMS based on EDSS, Reference Marrie, Tan, Ekuma and Marriott41 informal care and assistive devices were not included in the algorithm nor captured within provincial administrative data, and therefore, it is possible that some individuals with a higher EDSS score may have been misclassified as having a lower score. While individual-level direct healthcare costs would not be affected, the total healthcare cost of mild and moderate disability would be subject to potential overestimation and underestimation of severe disability. The algorithm also tends to overestimate EDSS scores at the lower end of the range as evidenced by the model intercept that exceeded 0 (i.e., 1.27) Reference Marrie, Tan, Ekuma and Marriott41 and was reflected in this study (none had EDSS scores 0–1.5). The PIN database only provides information on prescription medication dispensations from community pharmacies and therefore may not represent actual medication uptake by individuals. The use of over-the-counter medications and other non-pharmacotherapy management was not captured within the administrative data; prescription medications provided in a hospital or secondary care setting were not measured in this study. This study was conducted from the perspective of the Canadian healthcare system and did not include costs borne by individuals or indirect costs such as informal care and productivity loss (of the individual and/or caregiver). Previous studies have shown that when a societal perspective is considered, costs outside the health system increasingly outweigh direct healthcare costs as disability escalates, dominating total costs in severe disability. Reference Schriefer, Haase, Ness and Ziemssen12
Conclusions
This study provides insights into the direct healthcare costs associated with MS and the distribution of cost by disability status. Adults living with MS used greater healthcare resources and incurred higher incremental costs compared with those not living with MS, which may represent an additional $218 million per year in healthcare costs related to MS and associated comorbidities in Alberta. Health economic impact was apparent by disability status, underscoring the importance of preventing or delaying disability progression in MS. The observed shift in primary cost components with disability levels can be used to inform resource allocation planning.
Supplementary material
The supplementary material for this article can be found at https://doi.org/10.1017/cjn.2024.288.
Data availability statement
The data that support the findings of this study are available from Alberta Health Services and Alberta Health, but restrictions apply to the availability of these data, which were used under license for the current study and so are not publicly available.
Acknowledgments
We thank the participants of this study. This study is based in part on anonymized raw data from Alberta Health and Alberta Health Services, which were provided by the Alberta Strategy for Patient-Oriented Research Unit housed within Alberta Health Services. The interpretation and conclusions contained herein are those of the researchers and do not necessarily represent the views or opinions of the Government of Alberta or Alberta Health Services. Scott Klarenbach was supported by the Kidney Health Research Chair and the Division of Nephrology at the University of Alberta.
Author contributions
KV, KM, LR and SK contributed to the study concept and design. HS, KV and SAH conducted the analyses, PUN created the tables and figures and KM prepared the draft manuscript. All authors contributed to the interpretation of the data and critical revision of the report for intellectual content. SK provided study supervision.
Funding statement
This research study was funded by the University Hospital Foundation with contribution from Novartis; funds were held at the University of Alberta by SK. The funders had no role in the study design, analysis, interpretation of the data and drafting of the manuscript or in the decision to submit for publication. The funders were provided the opportunity to comment on the protocol and draft manuscript, with all final decisions remaining with SK.
Competing interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship and/or publication of this manuscript: HS, KV, HL, KM, SAH, PUN, LR, TW and SK are members of the Alberta Real World Evidence Consortium (ARWEC) and the Alberta Drug and Therapeutic Evaluation Consortium (ADTEC); these entities (comprised of individuals from the University of Alberta, University of Calgary and Institutes of Health Economics) conduct research including investigator-initiated industry-funded studies (ARWEC) and government-funded studies (ADTEC). EB, JM, PS and MK declare no competing interests. All authors of this study had complete autonomy over the content and submission of the manuscript, as well as the design and execution of the study.