About 75 % of older adults have ≥2 concurrent chronic health conditions, referred to as ‘multiple chronic conditions’ (MCC)( Reference Wolff, Starfield and Anderson 1 – Reference Vogeli, Shields and Lee 3 ). Because the prevalence and burden of MCC are anticipated to escalate with an increasing ageing population, MCC is growing as a significant public health and clinical care problem( Reference Wolff, Starfield and Anderson 1 – Reference Vogeli, Shields and Lee 3 ). Older adults with MCC experience increased demands on their household budgets, including increased health-care expenditures and increased food expenditures necessary to meet the relatively expensive nutritional recommendations for conditions such as diabetes and hypertension( Reference Vogeli, Shields and Lee 3 , Reference Fried, Bernstein and Bush 4 ). These households may therefore be at greater risk of food insecurity, defined as the uncertain or limited access to nutritionally adequate and safe foods( Reference Seligman, Laraia and Kushel 5 – Reference Olson 7 ).
From 2001 to 2015, the number of older adults who were food insecure more than doubled to 5·4 million individuals( Reference Ziliak and Gundersen 8 ). Individuals living in food-insecure households must sometimes reduce food intake, miss meals or alter dietary intake by shifting to less expensive foods, often including those high in added sugar, salt and fat( Reference Seligman, Laraia and Kushel 5 , Reference Olson 7 , Reference Kendall, Olson and Frongillo 9 – Reference Lee and Frongillo 12 ). Thus, not only may MCC increase risk of food insecurity, but the resulting food insecurity could then contribute to the development or exacerbation of chronic diseases such as diabetes( Reference Seligman, Laraia and Kushel 5 , Reference Seligman, Jacobs and Lopez 6 ). Multiple studies have demonstrated that the added economic vulnerability of food insecurity can lead to trade-offs with chronic disease management, including cost-related medication non-adherence (e.g. skipping or reducing medication doses) and suboptimal chronic disease management( Reference Schoenberg, Kim and Edwards 2 , Reference Tarasuk, Mitchell and McLaren 13 – Reference Sattler and Lee 16 ).
Among older adults, little is known about the relationship between food insecurity and MCC. In an analysis of the Canadian Community Health Survey focused on adults up to age 64 years, Tarasuk et al. reported an increased odds of food insecurity for respondents with 1, 2 or ≥3 chronic conditions compared with respondents with no chronic conditions( Reference Tarasuk, Mitchell and McLaren 13 ). Whether MCC increases the risk for food insecurity in vulnerable geriatric populations or in the USA remains unclear. Using the 2013 Health Care and Nutrition Study (HCNS), a supplemental survey of the national and population-based Health and Retirement Survey (HRS), we investigated the relationship between food insecurity and MCC among older adults living in the USA.
Methods
Study design and sample
We conducted a secondary cross-sectional analysis of the HRS, a national, population-based, longitudinal study of community-dwelling adults aged 50 years or older( 17 ) linked to the HCNS, which includes questions on food insecurity. The HCNS was mailed in 2013 to a sub-sample of HRS respondents (n 12 418) and had a response rate of 65 % for a final study population of 8073 HRS participants( 18 ). We excluded 165 (2·2 %) respondents from our analytic sample who did not complete the core 2012 HRS in which health and sociodemographic factors were assessed and another 474 (6·2 %) respondents who did not have valid food insecurity responses in the 2013 HCNS. In an effort to minimize unmeasured socio-economic confounding factors, we also restricted our analysis to those participants whose reported 2012 household income was under 300 % of the federal poverty line. Publicly available de-identified data were used for all analyses.
Food insecurity
The outcome of interest was food insecurity, assessed using the six-item Short Form of the US Household Food Security Survey Module( Reference Blumberg, Bialostosky and Hamilton 19 ). The raw score of food security status was calculated as a sum of affirmative responses with a range of 0–6. Food insecurity status was assigned based on two or more affirmative answers (no food insecurity=score of 0–1; food insecurity=score of 2–6), based on official scoring recommendations from the US Department of Agriculture( Reference Blumberg, Bialostosky and Hamilton 19 ).
Multiple chronic conditions
The main independent variable was MCC, defined as the number of self-reported co-morbid conditions, a commonly used measure for MCC( Reference Huntley, Johnson and Purdy 20 ). We included self-report of fifteen conditions available in HRS: hypertension; diabetes; cancer (except skin); chronic obstructive pulmonary disease; heart disease; cerebrovascular artery disease; arthritis or rheumatism; urinary incontinence; osteoporosis; depression; emotional, nervous or psychiatric problems; cognitive impairment defined as Alzheimer’s disease, dementia, senility or any other serious memory impairment; vision impairment (fair or poor self-rated vision or being legally blind); hearing impairment (fair or poor self-rated hearing); and significant pain, defined as self-report of often troubled by moderate or severe pain. We created a categorical variable based on the number of co-morbid chronic conditions present (0–1, 2–4, ≥5).
Sociodemographic and health measures
We included the basic sociodemographic variables, as well as all the variables that were significantly associated with both MCC and food insecurity and might confound the relationship between MCC and food insecurity. We included age, sex, race/ethnicity, marital status, socio-economic status, health insurance, self-rated health, tobacco use, measured BMI and cost-related medication non-adherence. Socio-economic status variables included highest education level, wealth, household size, current employment status and housing type (own, rent or other arrangement). Cost-related medication non-adherence was defined as self-report of taking less medication than prescribed within the last 2 years due to cost.
Statistical analyses
We compared characteristics of participants with and without food insecurity using χ 2 tests for categorical variables and Kruskal–Wallis tests for continuous variables. To assess collinearity of variables, we examined the pairwise correlations and variance inflation factor for all variables; no adjustments were needed. Next, we examined unadjusted and adjusted association of food insecurity and MCC using logistic regression. In adjusted analysis, we adjusted for the following confounders: age, sex, race/ethnicity, marital status, health insurance status, self-rated health, employment status, household size, education, wealth, household size, smoking status and BMI. Age and household size were included as continuous measures. We used the HRS sampling and design weights provided to account for the probability of selection and clustering in the HRS( 21 ). Statistical significance was assessed at the 0·05 level. The statistical analyses were performed using the statistical software packages STATA version 13 (2015) and SAS version 9.4 (2013).
Results
Table 1 presents the sociodemographic and health characteristics of the 3552 respondents with an annual household income under 300 % of the federal poverty level included in the analysis. The overall prevalence of food insecurity was 27·8 %. Compared with respondents without food insecurity, food-insecure respondents were younger (mean 61·9 years old v. 69·4 years old) and more likely to be Black, Latino or Other/Unknown race/ethnicity. Food-insecure respondents were also more likely to be unmarried, have completed less than high-school education, have a larger household size, rent their primary housing and be currently employed. Food-insecure respondents reported a median wealth of $US 8500 compared with a median wealth of $US 135 000 among respondents without food insecurity. Among food-insecure respondents, almost a quarter reported no health insurance and more than 50 % reported fair or poor self-rated health.
Sociodemographic and health characteristics of study participants with household income under 300 % of the federal poverty line by food insecurity status: respondents to the 2013 Health and Retirement Study (HRS) Health Care and Nutrition Study (HCNS), USA
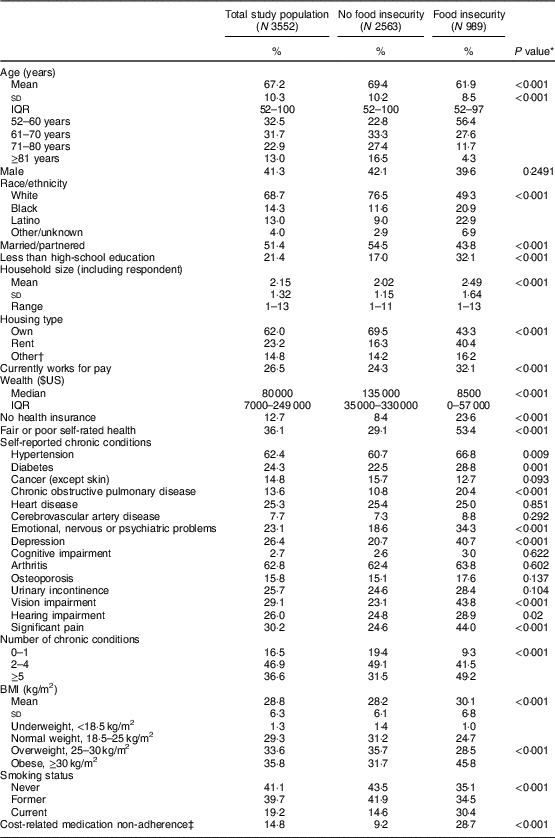
IQR, interquartile range.
* P value compares respondents with no food insecurity with respondents with food insecurity.
† Other includes those living on ranch, mobile home, with friends or relatives, or unspecified.
‡ Cost-related medication non-adherence is defined as taking less medications than prescribed in the last 2 years because of the cost.
In this study sample, the most prevalent chronic conditions were hypertension (62·4 %), arthritis (62·8 %), significant pain (30·2 %) and vision impairment (29·1 %). About a quarter reported diabetes, heart disease, depression, urinary incontinence and hearing impairment. Hypertension, diabetes, depression, vision impairment and significant pain were more prevalent among those reporting food insecurity compared with those without food insecurity. Food-insecure respondents were more likely to report ≥2 chronic conditions (90·7 % v. 80·6 %, P<0·001), be obese (mean BMI 30·1 kg/m2 v. 28·2 kg/m2, P<0·001), be current smokers (30·4 % v. 14·6 %, P<0·001) and report cost-related medication non-adherence (28·7 % v. 9·2 %, P<0·001) compared with those reporting food security.
The multivariate logistic model examined the association between MCC and food insecurity (Table 2). Compared with those having 0–1 chronic conditions, respondents with ≥2 chronic conditions were more likely to have food insecurity (adjusted OR (AOR)=2·12; 95 % CI 1·45, 3·09 for 2–4 chronic conditions; AOR=3·64; 95 % CI 2·47, 5·37 for ≥5 chronic conditions). Respondents reporting cost-related medication non-adherence were about 1·9 times as likely as those without to be food insecure.
Adjusted odds for food insecurity by multiple chronic condition categories and sociodemographic and health measures among respondents to the 2013 Health and Retirement Study (HRS) Health Care and Nutrition Study (HCNS), USA

Ref., referent group.
* Other includes those living on ranch, mobile home, with friends or relatives, or unspecified.
† Cost-related medication non-adherence is defined as taking less medications than prescribed in the last 2 years because of the cost.
Discussion
To our knowledge, the present study is the first to examine the association between MCC and food insecurity in a representative population of older adults over 50 years of age in the USA. We found that among low-income older adults, older adults with two or more chronic conditions are at increased risk of food insecurity. We also found that food insecurity is associated with increased cost-related medication non-adherence.
In the current study of a diverse, nationally representative sample of older adults in the USA, the prevalence of food insecurity was 27·8 %, higher than in other population-based studies( Reference Ziliak and Gundersen 8 , Reference Lee, Fischer and Johnson 11 ). Consistent with national data, our study found that older adults aged <70 years with less than high-school education and lower income are at higher risk of food insecurity( Reference Lee and Frongillo 10 – Reference Lee and Frongillo 12 ). Our finding of increased risk for food insecurity with two or more chronic co-morbid conditions is consistent with analyses conducted in Canada showing similar relationships among younger adults( Reference Tarasuk, Mitchell and McLaren 13 ). In addition, a small study in the USA (North Carolina) has shown that food-insufficient homebound older women are more likely to report at least three chronic conditions( Reference Sharkey 22 ).
The mechanism by which MCC is associated with food insecurity is likely bidirectional( Reference Tarasuk, Mitchell and McLaren 13 ). A high chronic disease burden could exert added financial strain on the household budgets of low-income older adults, contributing to an increased risk for food insecurity and subsequent cost-related challenges to medication adherence( Reference Jeon, Essue and Jan 23 , Reference Valtorta and Hanratty 24 ). Alternatively, sustained economic hardship including food insecurity can contribute to the development of chronic conditions and poor health status( Reference Seligman, Laraia and Kushel 5 , Reference Seligman, Jacobs and Lopez 6 , Reference Lynch, Kaplan and Shema 25 ).
Screening for food insecurity in clinical settings among low-income older adults with high chronic disease burden may be warranted to reduce the effects of food insecurity on chronic disease management. Food insecurity can be reduced by participating in food assistance programmes, such as the governmental Supplemental Nutrition Assistance Program (SNAP), which can improve access to food( Reference Gundersen 26 – Reference Mabli, Ohls and Dragoset 28 ). However, SNAP is underutilized among older adults, with only 40 % of eligible older adults enrolled to receive benefits( 29 ). In the primary care clinical setting, food-insecure older adults can be referred to social workers or case managers to facilitate enrolment into SNAP and connections to community-based food assistance programmes including food banks and pantries, hot meal sites and at-home delivery of meals( Reference Cannon 30 , Reference Torres, De Marchis and Fichtenberg 31 ). In addition, clinicians can strategize to reduce out-of-pocket medication costs in order to support food security, such as minimizing medication co-payments and discontinuing non-essential medications( Reference Schoenberg, Kim and Edwards 2 , Reference Berkowitz, Seligman and Choudhry 14 ).
The present study has several limitations. First, the findings are based on self-report of chronic conditions and the available chronic conditions in HRS for analysis are not comprehensive of all possible chronic conditions. Second, food insecurity defined through the US Household Food Security Survey Module does not account for other ageing-related risk factors for malnutrition among older adults such as disability, functional limitations, poor dentition and change in taste that affect food choices and access to food. Future research should examine how these ageing-specific factors impact food insecurity among older adults with MCC.
Conclusion
In conclusion, our study demonstrates that low-income older adults with MCC in HRS have an increased risk for food insecurity, with more chronic conditions being associated with a higher risk. Screening for food insecurity in the primary care of older adults, especially those with substantial chronic disease burden, could identify at-risk older adults who could benefit from existing community and governmental food resources and programmes that could improve access to food and reduce the health effects of food insecurity. Food insecurity is a significant social determinant of health that has clinical implications in the chronic disease management and quality of life of this vulnerable population.
Acknowledgements
Financial support: This work was supported by the National Institute on Aging at the National Institutes of Health (W.J.B. and C.S.R., grant number P30 AG044281), (J.J., grant number R03 AG050880). The National Institute on Aging had no role in the design, analysis or writing of this article. Conflict of interest: H.K.S. receives funding from Feeding America, a 501c3 non-profit dedicated to ending hunger in the USA, to serve as its Lead Scientist and Senior Medical Advisor. All other authors declare no conflicts of interest. Authorship: J.J. and I.S.-C. led in writing the manuscript. I.S.-C. completed the data analysis. All authors contributed to the design of the study, interpretation of data, and participated in revising the content and approving the final version of the manuscript. Ethics of human subject participation: It was determined that the study did not meet the definition of human subjects research based on guidelines provided by the University of California San Francisco Institutional Review Board.



