Highlights
-
• Healthcare providers in Alberta reported dissatisfaction with referral processes and interdisciplinary communication pathways related to cerebral visual impairment.
-
• Healthcare providers described limited continuing education opportunities and educational resources for families affected by cerebral visual impairment.
-
• Healthcare providers highlighted inequitable access to resources based on geographic location.
Introduction
Cerebral visual impairment (also known as cortical visual impairment) (CVI) is a brain-based disorder that affects visual function and perceptual abilities in children with brain abnormalities or atypical brain development. Reference Chang, Merabet and Borchert1 CVI is the leading cause of visual impairment in children in developed nations Reference Fazzi, Signorini and Bova2 and can affect as many as one in every 30 school-aged children. Reference Williams, Pease and Warnes3,Reference Bennett, Tibaudo, Mazel and Y.4 CVI can present as visual field deficits (VFDs), oculomotor or perceptual impairments, Reference Chang and Borchert5,Reference Lueck, Dutton and Chokron6 all of which can impact typical activities in development such as reach and grasp, ambulation, seeing and understanding facial expressions, and school performance. Reference Belmonti, Cioni and Berthoz7–Reference Crotti, Ortibus and Ben Itzhak10 Despite this high prevalence, CVI is often mis- or under-diagnosed Reference Chang, Merabet and Borchert1,Reference Rice, Schwartz, Bulman, Lin and Harpster11 and there are currently no published best practice assessment guidelines to inform clinical practice. Literature suggests that a multi-disciplinary team approach, including pediatric neurology, ophthalmology and allied health (AH) professionals, is optimal for assessment of CVI. Reference Boonstra, Bosch, Geldof, Stellingwerf and Porro12,Reference Lehman, Yin and Chang13 Early identification and intervention for CVI is likely critical as the neuroplasticity of the young brain offers the highest potential to improve developmental outcomes. Reference Mercuri, Rutherford and Cowan14–Reference Purpura and Tinelli16 CVI has been identified as a priority area of research in both the United States and Europe, Reference Chang, Merabet and Borchert1,17 but knowledge of CVI within the Canadian context has been limited and best practices remain undefined.
Caregivers of children with visual impairments have highlighted concerns regarding the lack of knowledge of health providers related to their child’s condition, and have associated this with diagnostic delays. Reference Goodenough, Pease and Williams18–Reference Lupón, Armayones and Cardona20 Parents also reported being provided with insufficient educational information related to their child’s visual impairments and how it may affect future outcomes. Reference Goodenough, Pease and Williams18,Reference Lupón, Armayones and Cardona19 Our understanding of healthcare provider experiences working with children with CVI is not well explored in the current literature. Healthcare providers working with adults experiencing stroke-related visual impairments cited systemic concerns regarding inadequate referral processes and challenges with interdisciplinary communication. Reference Manhas, Brehon, Jiang, Damji and Costello21 This study was conducted within the public health care system of Alberta, Canada, where there is currently no defined pediatric vision care pathway specific to children with neurological injuries and there is no documented understanding of how Canadian healthcare providers are managing CVI care needs. In this study, we sought to describe the perspectives of multiple professional disciplines within the neuro-pediatric healthcare team regarding perceived barriers and facilitators in the assessment and treatment of CVI in children with suspected visual impairment related to early life brain injury.
Methods
Participants
Healthcare providers working with children with CVI in Alberta were eligible for inclusion in the study. Certified health professions included were licensed practical nurse, neurologist or neurology resident, occupational therapist, optometrist, ophthalmic technician, ophthalmologist or ophthalmology resident, optician, orthoptist, pediatric ophthalmologist, physiatrist or physiatry resident, physiotherapist, recreation therapist, registered nurse, social worker, speech and language pathologist, therapy assistant and vision loss specialist. Respondents working in pediatrics, but not directly with children with CVI, were excluded.
Study and survey design
This cross-sectional study used online surveys adapted from an adult stroke study identifying barriers to care for poststroke visual deficits. Reference Manhas, Brehon, Jiang, Damji and Costello21,Reference Manhas, Damji, Brehon, Jiang, Faris and Costello22 The survey developed for the adult stroke study was co-designed by a multidisciplinary group of patients and healthcare providers along the continuum of care. Reference Manhas, Brehon, Jiang, Damji and Costello21,Reference Manhas, Damji, Brehon, Jiang, Faris and Costello22 Consent, demographics and adaptive questions were required fields. The study received approval from both the University of Calgary Conjoint Health Research Ethics Board (REB24-1471) and institutional approval from the provincial health authority, Alberta Health Services (AHS), to distribute to healthcare staff via area management. Consent included information about the purpose of the survey, risks and benefits and processes for withdrawal of data. Respondents were required to click on a checkbox to express informed consent prior to proceeding.
Survey questions from the adult study were modified to consider additional issues relevant to the pediatric population, including family-centered care and collaboration with the education system. Both Likert scale and open-ended questions were used to enable a comprehensive understanding of provider perspectives, while also being able to analyze responses based on factors such as health discipline, location and years of experience. Reference Vedel, Kaur and Hong23 The survey was reviewed and edited by members of the research team, including a pediatric ophthalmologist (UD), pediatric neurologist (AK) and an occupational therapist (MG), and was tested prior to distribution. The online survey consisted of four sections: consent to participate, eligibility (includes demographics), screening and diagnosis of CVI, and rehabilitation and management of CVI. A 5-point Likert scale with free-choice format (inclusive of a “not applicable” option) and open-ended questions were used to understand current CVI assessment and treatment practices, and respondents ranked a list of priorities for a theoretical provincial working group (the full questionnaire is available as Supplementary material 1). Adaptive questioning was used to determine if healthcare providers engaged in either assessment and/or treatment of CVI prior to linking them to the appropriate Likert scale questions.
The Qualtrics (XM) platform was used to host the online survey and gather responses. 24 A link to the Qualtrics online survey was provided to management of pediatric medical, AH and vision care teams across the province as per provincial research processes and policies, and then distributed by management to front-line healthcare staff. Responses collected were anonymous and IP addresses were collected to prevent duplicate entries from the same user. Respondents were provided an optional link, which was not connected to survey responses, at the end of the survey to enter a draw for a $100 gift card to a vendor of their choosing. Responses were collected throughout April and May 2025.
Data analysis
The Jamovi platform was used to complete statistical analysis, 25 including descriptive statistics, frequencies, independent samples t-tests and analysis of variance (ANOVA) used to compare subgroups of respondents. Quantitative data were analyzed using student’s t-tests for normally distributed data and Mann-Whitney U test for non-parametric data. Responses to 5-point Likert scale questions were collapsed into three categories: “Agree” (including Agree and Strongly Agree), “Disagree” (Disagree and Strongly Disagree) and “Neither Agree or Disagree” for analysis to reduce the risk of type 1 errors. To compare subgroups of respondents, participants were classified as either a physician (neurologist, ophthalmologist, physiatrist or resident) or an AH care provider (OT, PT, SLP, RN, therapy assistant and orthoptists); having either more than or less than 10 years of experience; working in Northern Alberta (Edmonton, North and Central) versus Southern Alberta zones (Calgary and South) of the province; and working in Alberta’s large urban centers (Calgary and Edmonton) versus rural centers. As OTs historically play a key role in assessment and treatment of CVI in high-income countries, Reference Weden, DeCarlo and Barstow26 further analysis was completed to compare physicians, OTs and other rehabilitation personnel (a combined group of SLPs and PTs) using Welch’s ANOVA with Games-Howell post-hoc test for comparisons of the three groups. Ranked priorities for provincial action were calculated by generating a weighted composite score by multiplying the rank number by the number of respondents who gave that rank. The lowest score indicated the highest ranking.
Responses to open-ended questions were considered qualitative data and analyzed using conventional content analysis and an interpretivist paradigm. Reference Hsieh and Shannon27,Reference Graneheim and Lundman28 Codes for the data were created inductively in a step-by-step process that included data familiarization, code generation, theme generation and a collaborative review of themes. Reference Vaismoradi, Turunen and Bondas29 During the data familiarization stage of the analysis, responses to the three questions were noted to have overlapping keywords and codes and thus were analyzed together. Responses were excluded when researchers could not confidently interpret the comment due to lack of context. Regular research meetings occurred between the two coders (MM and AB) to determine consensus. Reference Graneheim and Lundman28 Themes were established and reviewed with an expert in the field to ensure accuracy and relatability (MG).
Quantitative results
Respondent demographics
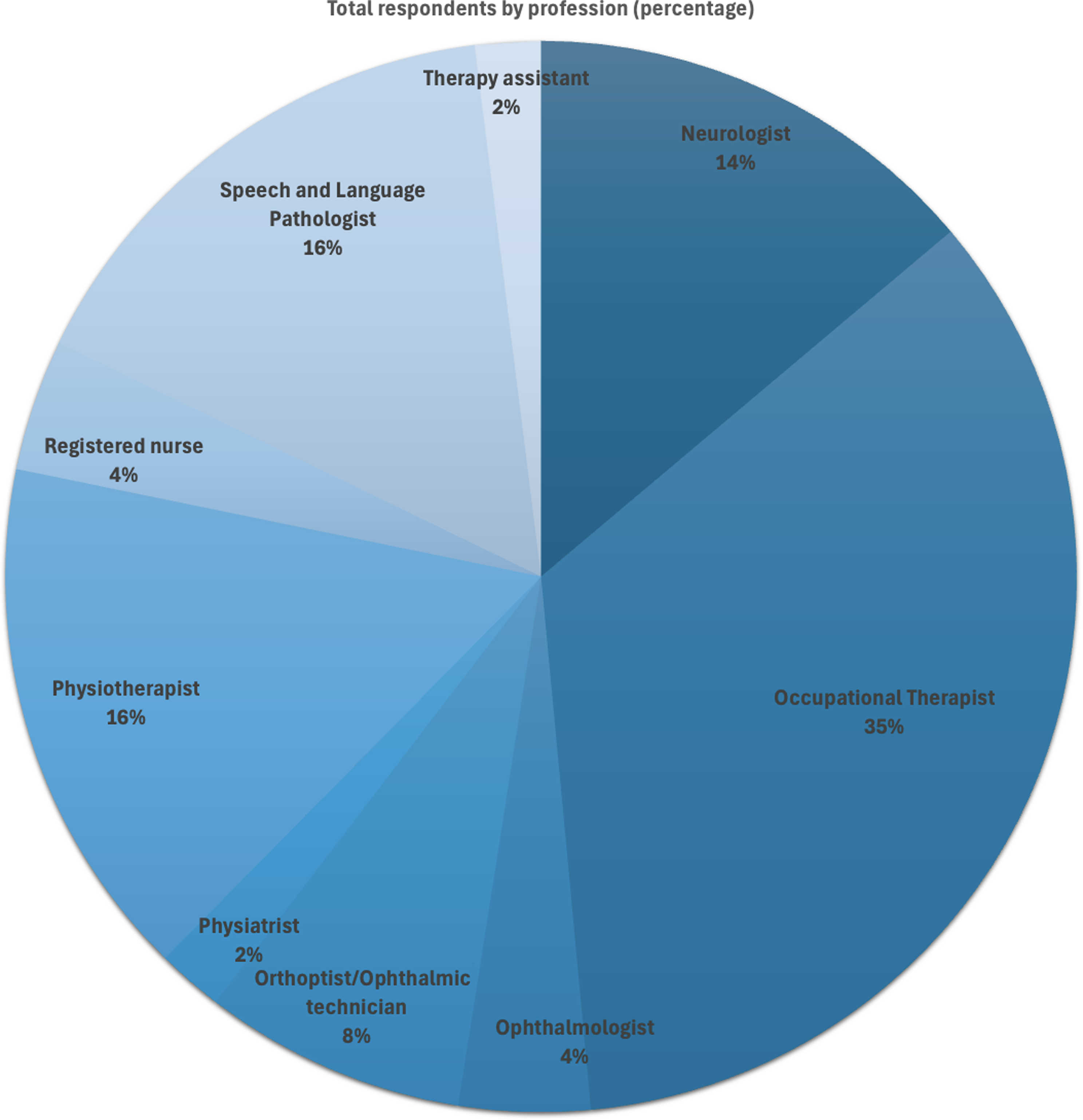
Sixty-two healthcare providers initially logged onto the survey between April and May 2025 with a completion rate of 87%. No duplicate entries were identified in the review. Three respondents were excluded after stating they did not work directly with children with CVI, for a total of 51 respondents. Surveys were completed by the following health professionals: occupational therapists (OT) (n = 18, 35%), speech and language pathologists (SLP) (n = 8, 16%), neurologists (n = 7, 14%), physiotherapists (PT) (n = 8, 16%), ophthalmic technician/orthoptist (n = 4, 8%), ophthalmologists (n = 2, 4%), registered nurses (RN) (n = 2, 4%), one physiatrist (2%) and one therapy assistant (2%) (Figure 1). Most respondents worked in the Calgary zone (n = 29, 56%), followed by Edmonton (n = 13, 25%), South zone (n = 4, 8%), Central zone (n = 4, 8%) and North zone (n = 3, 6%). One respondent reported working in multiple zones. Many respondents stated that they worked in multiple health care settings, with the highest percentage working in a hospital outpatient setting (n = 38, 75%), followed by acute/inpatient (n = 10, 20%) and community outpatient settings (n = 10, 20%), school-based care (n = 9, 18%), in-home care (n = 8, 16%) and inpatient rehabilitation (n = 6, 12%). Fifty respondents (93%) stated they provide care related to CVI assessment and diagnosis, and 29 respondents (54%) stated they provided rehabilitation and management of visual deficits in children with CVI. Most respondents providing rehabilitation and management of CVI were OT, PT and orthoptists. Twenty-eight respondents (46%) reported involvement in both assessment and management of CVI.

Figure 1. Pie chart showing the percentage of each health profession that responded to the survey.
Healthcare provider perceptions of CVI screening practices
Fifty of the 54 respondents who completed the survey reported involvement in assessment and screening of children with CVI. Response frequencies and percentages for each question are summarized in Table 1. Healthcare providers reported split confidence levels when screening for VFDs (46% agree and 50% disagree) and many did not feel confident in the process for confirming the presence of VFDs (45%). Slightly more than half of participants reported decreased confidence in screening for perceptual impairments (55%). Many respondents disagreed that current referral processes are adequate to obtain a diagnosis of CVI (VFD – 51%, perceptual impairment 60%), and indicated that communication pathways between healthcare providers are sub-optimal (62%). A slight majority of respondents reported dissatisfaction with current education and training opportunities (59%) and the adequacy of available resources for screening and diagnosis (55%).
Table 1. Healthcare provider (n = 50) perceptions of current practices regarding the assessment of children with CVI

Responses were split between AH professionals (OT, PT, SLP, orthoptist, RN and therapy assistant) and physicians, and then assessed for group differences using t-tests. When compared to physicians, AH team members were less likely to feel confident screening for VFDs (U(N AH = 36, N MD = 10) = 79.0, p = 0.006, r = 0.561), and reported decreased confidence in the continuing education available to them regarding assessment practices (U(N AH = 35, N MD = 10) = 73.0, p = 0.004, r = 0.583). When respondents were broken down further and OTs were compared to physicians and the PT/SLP group, there were significant differences between the three groups in the assessment of VFDs (F 2,23 = 29.0, p < 0.001, w 2 = 0.7) and perceptual impairments (F 2,23 = 7.4, p = 0.003, w 2 = 0.35). Using the Games-Howell post-hoc test to assess the non-parametric data, MDs reported the highest confidence in screening for VFDs compared to both OTs (p = 0.04) and PT/SLP (p < 0.001), while OTs had more confidence than the PT/SLP group (p = 0.003). When assessing for perceptual skills, MDs and OTs both had higher confidence than SLP/PT (p = 0.03 and p = 0.004, respectively) with SLP/PT feeling the least confident (F 2,27 = 7.0, p = 0.004, w 2 = 0.3).
Group differences were present when health providers were categorized based on their years of experience (more than 10 years versus less than 10 years). There was no difference in confidence levels in screening for VFDs, but less experienced care providers reported decreased confidence in the process for confirming a VFD diagnosis (U(N <10 = 28, N >10 = 19) = 185.5, p = 0.030, r = 0.360). Care providers with less than 10 years of experience reported decreased confidence in screening for perceptual impairments (U(N <10 = 28, N >10 = 19) = 159.5, p = 0.018, r = 0.400). Less experienced care providers also reported decreased clarity regarding the scope of practice of their team members (U(N <10 = 29, N >10 = 20) = 181.0, p = 0.023, r = 0.376), and decreased confidence in team members’ abilities to assess for CVI (U(N <10 = 28, N >10 = 20) = 142.0, p = 0.003, r = 0.493). Newer healthcare providers were less satisfied with referral processes (t 45 = 2.13, p = 0.038, d = 0.629), interdisciplinary communication pathways (U(N <10 = 27, N >10 = 20) = 175.5, p = 0.033, r = 0.350) and evidence-informed educational opportunities (U(N <10 = 26, N >10 = 20) = 159.5, p = 0.018, r = 0.387).
Perceived inequities were represented statistically, as healthcare providers in the southern half of the province were more likely to report that resources available to them were inadequate (U(N South = 26, N North = 17) = 130.0, p = 0.019, r = 0.412). Healthcare providers from rural centers were less likely to feel confident screening for visual field defects (U(N Urban = 36, N Rural = 9) = 60.0, p = 0.003, r = 0.630) and perceptual impairments (U(N Urban = 37, N Rural = 9) = 87.5, p = 0.024, r = 0.474), and less confident in the process for confirming a VFD diagnosis (U(N Urban = 39, N Rural = 9) = 99.5, p = 0.041, r = 0.433). Rural healthcare team members reported decreased clarity on the scope of practice between different professionals in the assessment of CVI (U(N Urban = 39, N Rural = 9) = 99.0, p = 0.038, r = 0.436).
Healthcare provider perceptions of CVI management and/or rehabilitation
Twenty-nine (54%) healthcare providers reported involvement in management and/or rehabilitation for children with CVI, with frequencies and percentages for each question summarized in Table 2. Two of these respondents were physicians and the remainder were AH team members. Respondents were split regarding confidence levels in VFD management (36% agree and 36% disagree) and treatment of perceptual impairments (32% agree, 43% disagree), and confidence in team members within AHS (38% agree, 35% disagree) or community organizations (38% agree, 35% disagree) to address these concerns. Respondents did not agree that communication pathways were adequate within AHS (48%), within the education setting (48%) or between AHS and the education setting (59% disagree). Healthcare providers reported that referral processes for obtaining treatment for CVI within AHS are inadequate (62%), and that they lacked confidence in available continuing education (62%) and in their ability to find educational resources for families (62%). Fifty-six percent of healthcare providers did not agree that they had access to the tools that they needed to provide adequate care to their patients with CVI.
Table 2. Healthcare provider (n = 29) perceptions of current care practices regarding the treatment and/or management of children with CVI

Care providers from rural centers reported decreased confidence in the ability to manage treatment for a child with a VF defect (t 45 = −2.956, p = 0.007, d = −1.468) along with decreased confidence in the role of other professional disciplines to manage care for a child with a VF defect (t 45 = −2.269, p = 0.033, d = −1.134).
Care providers with less than 10 years’ experience were more likely to report dissatisfaction regarding current communication pathways between the healthcare and education systems (U(N <10 = 16, N >10 = 10) = 29.5, p = 0.005, r = 0.631) than more experienced healthcare team members.
Ranking priorities for provincial action
Forty-five respondents (83%) ranked eight topics that could be the focus of a provincial working group. The top three priorities were (1) advancing care provision for CVI screening, (2) advancing care provision for CVI diagnosis and (3) advancing care provision for CVI management and rehabilitation (Figure 2). Priorities 4–6 were related to advancing knowledge of CVI via development of training for healthcare providers, educational resources for healthcare providers and educational resources for families, respectively. Of least priority were advancing access to equipment and resources as well as clarifying the scope of practice between professionals.
Qualitative results and content analysis of “Perspectives on assessment and treatment of cerebral visual impairment in children in Alberta”
Thirty-four respondents (63%) provided open text responses to at least one of three questions related to current gaps in practice regarding CVI assessment and treatment, and areas where provincial action could be taken. Responses were provided by OTs (n = 12), SLPs (n = 6), PTs (n = 5), ophthalmic technician/orthoptist (n = 4), neurologists (n = 3), ophthalmologists (n = 2), therapy assistants (n = 2), an RN (n = 1) and a physiatrist (n = 1). Four themes were generated from content analysis: health system challenges, resource availability, knowledge and education, and the need for a pediatric-specific focus in CVI care (summary in Table 3, entire codebook available in Supplementary material 2).
Table 3. Description of key themes and codes generated from content analysis

Theme: health systems challenges
This theme largely reflected the gaps and challenges that healthcare providers reported in providing care to children with CVI. Concerns were raised by both physicians and AH professionals regarding the lack of clarity in referral processes and challenges in having referrals accepted by professionals within the public health system and community organizations.
“I don’t know of the processes of referral, diagnosis or find more information to support vision in the outpatient setting. (Respondent 18, speech and language pathologist)”
“We live rural so getting our clients seen by anyone to confirm or refer on clients with any visual impairment is limited to local opticians who may or may not have the knowledge. It also costs families money to get a more involved assessment locally.” (Respondent 14, physiotherapist)”
These challenges were amplified by additional inequities, including rural access to care, perceived inequities between healthcare zones across the province and unclear communication pathways between healthcare providers and professionals in the education system.
“There is very little communication between various groups - health care, community supports such as VLR [referring to Vision Loss Rehabilitation Canada], and school staff. I feel like families are often then functioning as middlemen between the various groups. (Respondent 4, ophthalmic technician/orthoptist)”
Theme: Resource availability
Respondents identified challenges accessing tangible resources such as the people and equipment needed to provide adequate assessment and treatment of children with CVI. This limited access was described in both the healthcare system, where lack of available providers led to long wait times and reduced multidisciplinary involvement, and the education system, where collaboration with teachers for the visually impaired was described positively, but not always available. One respondent quoted below described their experience at a multidisciplinary center in Edmonton, suggesting this model could be useful elsewhere in the province. The need for appropriate CVI care as it relates to communication, specifically the use of augmentative and alternative communication, was also identified.
“Many of the kids [seen at rehabilitation centre in Edmonton zone] have a complex multidisciplinary team involved. These children are well-served in my opinion.” (Respondent 22, occupational therapist)
“Time allocation to screening CVI, as most of the patient encounter is taken up by history and other parts of neurologic exam.” (Respondent 21, neurologist)
Theme: Education
Respondents highlighted the current lack of evidence in the literature related to both the assessment and management of CVI. Concerns arose regarding the lack of evidence-based online resources and time required for healthcare providers to find and personalize high-quality resources for treatment and family education purposes.
“Clarity on what interventions are helpful for these children, how they should be implemented.” (Respondent 48, ophthalmologist)
“Access to resources and education for both professionals and parents of these children.” (Respondent 14, physiotherapist)
Theme: The need for a pediatric-specific focus
Many pediatric care providers described the need for a pediatric-specific approach rather than modifications to assessment and treatment practices used in adults. Respondents highlighted a lack of pediatric-focused tools, resources and educational opportunities and the importance of family-centered care. One respondent described the importance of providing children with the tools that they need to advance their own knowledge about their condition, as they will be required to manage it independently in adulthood. AH care providers reflected on the impact of CVI on daily activities such as driving a power wheelchair, school performance and communication.
“Trying to apply adult tools to a pediatric population.” (Respondent 49, occupational therapist)
“Contributing observations [related to] other disability, communication challenges, attentional challenges, behavioral challenges…” (Respondent 23, occupational therapist)
“Many of the families […] have a child with CVI and know that they’re child has CVI [but]don’t understand what CVI means or how this impacts their children’s vision and therefore do not do any of the things recommended by a CVI specialist…This clearly indicates to me that the families receive insufficient information.” (Respondent 9, speech and language pathologist)
Discussion
In this study, we explored multidisciplinary healthcare team members’ perceptions of care provision for children affected by CVI in the public health system in Alberta, Canada. Results focused on health provider confidence in their skills and abilities related to CVI care, systemic processes, communication between professionals and availability of education and resources. Quantitative findings found that physicians (neurologists, ophthalmologists and physiatrists) reported the highest levels of confidence in assessing for visual and perceptual impairments, closely followed by occupational therapists. Rural healthcare providers and those with fewer reported years of experience described decreased confidence in perceptual screening, less familiarity with processes to confirm a CVI diagnosis and decreased access to resources to support children with CVI. These results were echoed in the qualitative findings, where healthcare providers described a lack of knowledge of best practices for CVI assessment and treatment, and lack of clarity related to referral processes.
This study was conducted within the public health system of Alberta, Canada, which has both similarities and differences from other provincial health systems across the country. AHS is structured as a provincial health entity with a central clinical information system, whereas other Canadian provinces may operate regional health authorities for healthcare delivery. This may reduce applicability of study findings regarding referrals and care communication to other provinces. Descriptions of reduced access to resources by respondents in rural and remote locations are likely a Canada-wide issue. Geographic location has been a known challenge for pediatric health care provision across Canada and along with other social determinants affects a disproportionate number of Indigenous children. Reference Sanders, Breen-Reid and Scarisbrick30–Reference Nickel, Lee, Chateau and Paillé32 Addressing these environmental inequities, particularly in a child’s early years, ensures that all children have a fair chance to reach their full potential. Reference Gerlach and McFadden33
Through content analysis of open-ended responses, a lack of CVI-focused educational opportunities and resources for healthcare providers and families was identified. This parallels findings from a National Eye Institute report published in 2021 that reported a lack of health provider awareness and training was a key concern in provision of effective CVI care. 34 Respondents in this study included academics, government officials, healthcare providers, patients and families, who expressed a desire for more access to evidence-informed education and resources to increase their own knowledge and better support families. Families and caregivers have also suggested that more knowledgeable health care teams could help reduce stress in the process of receiving and learning about their child’s diagnosis. Reference Goodenough, Pease and Williams18–Reference Lupón, Armayones and Cardona20
The current body of literature on CVI is growing; however, our respondents highlighted that the gap between scientific knowledge and clinical practice remains a barrier. The Canadian Association of Optometrists’ Canadian practice guidelines (adopted from the American Optometric Association and published in 2018) on pediatric visual assessment identified the need for comprehensive assessment of vision disorders in children with developmental disabilities, yet cited insufficient evidence to support or refute specific recommendations. 35 In CVI treatment, habilitation and visual stimulation are currently the most used rehabilitative strategies, although evidence is insufficient to support the use of any specific interventions. Reference Weden, DeCarlo and Barstow26 This can leave healthcare providers feeling uninformed and lacking confidence, as was described in our findings. Ongoing study of CVI and associated quality of life is essential to meet the needs of families and clients with this condition, Reference Goodenough, Pease and Williams18–Reference Lupón, Armayones and Cardona20 in addition to knowledge mobilization and implementation strategies.
Lastly, systemic challenges such as unclear referral processes, lack of clear communication pathways, inadequate resources and care inequities were described. These challenges may be addressed through a collaborative provincial effort. One solution may be the development and implementation of a provincial interdisciplinary pediatric vision care pathway that outlines team member roles and clear referral criteria. A multi-disciplinary approach is recommended to address CVI care, where ophthalmology plays a key role in ruling out ocular causes of dysfunction, physicians review medical history to support a differential diagnosis and AH care providers can determine the impact on daily function and provide strategies for adaptation and remediation. Reference Chang, Merabet and Borchert1,Reference Boonstra, Bosch, Geldof, Stellingwerf and Porro12 One respondent described the success of a multi-disciplinary approach in an Edmonton center and additional information about this service may be useful in guiding future implementation of a team-based approach in other centers across the province. Working groups may also wish to develop virtual and print resources that can be used throughout the province to educate care providers, patients and families, which could be a cost-effective way to increase knowledge and confidence, and can be updated as the evidence base increases.
Limitations of our study include recruitment of participants based on convenience sampling, which may have reduced the reach of the study or included bias from respondents who have a keen interest in CVI care. The researchers were unable to determine the total number of healthcare providers who received the link and any programs or regions where the survey was not distributed. OTs responded to the survey at double the frequency of any other health profession and it is unclear whether this was secondary to a self-selection bias or whether there were higher levels of survey distribution by AHS OT management. Researcher bias can be a limitation of content analysis, and to mitigate this, a collaborator with qualitative research experience but without CVI and health-systems knowledge was selected for the team-based analysis. There were challenges in the interpretation of open-ended survey responses where written answers lacked tone and emphasis. The ranked priorities section would have also benefited from additional comments to provide background information regarding respondent selections, as these proved difficult to interpret. Lastly, a larger sample size would have increased power for statistical analysis and made possible the testing of additional hypotheses. This study could be replicated in the future following the above proposed changes such as implementation of a pediatric vision care pathway and creation of educational materials for staff and families. Expanding this study to include perspectives of persons with lived experience, families, teachers and educators will contribute to our understanding of how best to support children with CVI in healthcare, home and school settings.
Conclusion
Responses from our survey have increased our understanding of the perspectives of healthcare providers within the pediatric public health context in Alberta, Canada, regarding perceived barriers and facilitators to CVI assessment and management. Findings highlight critical gaps in healthcare provider knowledge and confidence, systemic issues of inter-disciplinary communication and referral processes and perceived inequities in access to care and resources depending on geographic location. Tangible opportunities to improve respondent concerns were identified, including the development of a provincial pediatric CVI care pathway and the development of educational materials for healthcare providers and families. Addressing these gaps through inter-disciplinary collaboration is essential to advancing equitable, high-quality care for children and families living with CVI.

Figure 2. Stacked bar graph showing the percentage of respondents who ranked each item from most to least important.
Supplementary material
The supplementary material for this article can be found at https://doi.org/10.1017/cjn.2026.10564.
Acknowledgements
The authors would like to thank the many healthcare providers who took the time to participate in this study. We would like to thank Dr Ugo Dodd, Patricia O’Krafka and Brittany Jamieson for their contributions towards modifying the survey for the pediatric vision care context. This work was financially supported by the Cumming School of Medicine Vision in Stroke Across the Lifespan Grant.
Author contributions
The project was conceptualized for a pediatric population by MM, AK, MG and KPM. KPM, KD, MG and FC contributed to the development of the original survey and provided background knowledge for the study. DJ and AB contributed to qualitative methods development and data analysis. MM completed methods development, data collection and analysis and authored the final manuscript. All authors interpreted results and approved the final manuscript. The authors declare that they have no competing interests relevant to this manuscript.
Funding statement
Cumming School of Medicine – Vision in Stroke Across the Lifespan Grant.
Competing interests
The authors have no conflicts of interest to disclose.