Introduction
Stroke is a common neurological disease resulting from a sudden loss of brain function by a brain blood vessel blockage or rupture that leads to neuronal cell death. Reference Campbell and Khatri1 This disease is the third leading cause of death in Canada and a leading cause of disability. 2,Reference Krueger, Koot, Hall, O’Callaghan, Bayley and Corbett3 Access to timely and appropriate care, treatment, and rehabilitation is crucial for optimal recovery, as more than two thirds of stroke survivors develop poststroke sequelae, including spasticity that imposes a substantial burden on people living with poststroke spasticity (PSS) and their caregivers. Reference Wissel, Manack and Brainin4–Reference Francisco, Wissel, Platz, Li and Platz6 As defined by Li et al. (2021), “spasticity is manifested as velocity- and muscle length-dependent increase in resistance to externally imposed muscle stretch. It results from hyperexcitable descending excitatory brainstem pathways and from the resultant exaggerated stretch reflex responses. Other related motor impairments, including abnormal synergies, inappropriate muscle activation, and anomalous muscle coactivation, coexist with spasticity and share similar pathophysiological origins.” Reference Li, Francisco and Rymer7 Reports indicate that 25 to 40% of stroke survivors may develop PSS, with 2 to 13% experiencing disabling spasticity (defined as imposing a negative impact on well-being) where there is a need for intervention. Reference Wissel, Manack and Brainin4,Reference Zeng, Chen, Guo and Tan8 While the timing of PSS development varies widely, a recent systematic review and meta-analysis found that the incidence of PSS was highest in the first month after a stroke (32%), and changed little after 3 months (26% in 3–6 months, 24% beyond 6 months) Reference Zeng, Chen, Guo and Tan8 ; development of spasticity at 12 months is considered infrequent. Reference Kong, Lee and Chua9
Early recognition of PSS that may be facilitated by the identification of risk factors such as moderate-to-severe paresis and sensory disorder, Reference Zeng, Chen, Guo and Tan8 and timely management may reduce the risk of secondary maladaptation and impairment (e.g., restricted joint mobility, stiffness and pain), with potential improvements in function, long-term health, and quality of life. Reference Francisco, Wissel, Platz, Li and Platz6,Reference Bavikatte, Subramanian, Ashford, Allison and Hicklin10 Although not all persons with spasticity require treatment, it is widely acknowledged that treatment of disabling or problematic PSS is beneficial. Reference Francisco, Wissel, Platz, Li and Platz6 Various strategies for the management of PSS include rehabilitation by a specialized interdisciplinary team (e.g., physiatrists, nurses, physical therapists and occupational therapists), pharmacological management (baclofen, tizanidine, dantrolene, focal chemo-denervation) and surgical intervention. Reference Teasell, Salbach and Foley11,Reference Kuo and Hu12 However, limited evidence exists on health care system pathways of care experienced by stroke survivors who subsequently do or do not receive spasticity treatment.
The objective of this study was to describe the care pathways for stroke survivors who subsequently did and did not receive treatment for PSS in Alberta, Canada using high quality population based data; time to PSS treatment initiation and the setting where treatment was initiated were also described. Subgroup analysis was performed based on time to initiation of spasticity treatment classified according to defined timepoints after stroke (e.g., <3 months, 3–6 months, 6–12 months, >12 months). Reference Bernhardt, Hayward and Kwakkel13
Methods
The institutional review board at the University of Alberta approved this study (Pro00093914), which used retrospective administrative data without any direct intervention or personal identifiable information; informed consent was waived. This study is reported according to the Strengthening the Reporting of Observational Studies in Epidemiology guidelines. Reference von Elm, Altman and Egger14
Study design
A retrospective, observational, population based cohort study was conducted using administrative health data from Alberta between April 1, 2002 and March 31, 2020 that included adults who experienced a stroke in the community and sought acute care between April 1, 2012 and March 31, 2017 (inclusion period), a 3-year poststroke follow-up period, and a look-back period as far back as April 1, 2002.
Data source
Canadian provinces provide publicly funded health care for all residents. In Alberta, the fourth most populous Canadian province (3.9 to 4.2 million people [2012 to 2017]), health care is administered under the Alberta Health Care Insurance Plan (AHCIP), of which over 99% of Albertans participate. Reference Jin, Elleho, Sanderson, Malo, Haan and Odynak15 Each participant is assigned a unique person-level identifier (Personal Health Number); this was used to link individuals across datasets. Data from the Discharge Abstract Database (DAD), National Ambulatory Care Reporting System (NACRS), National Rehabilitation Reporting System (NRS), Alberta Continuing Care Information System (ACCIS), Millennium Scheduler, Virtual Address eXention (VAX), Practitioner Claims, Pharmaceutical Information Network (PIN), and Vital Statistics were linked to the Population Registry that contains demographic information for all Albertans with AHCIP coverage. DAD and NACRS include data on patients discharged from hospitals and facility-based ambulatory care settings including emergency departments (ED), respectively; a most responsible diagnosis code and secondary codes are included. NRS contains data from adult inpatient rehabilitation facilities; while submission of data is not required in Alberta, all major stroke rehabilitation units within the province submit data as part of the Alberta Health Services pathway for stroke care. Long-term care information was accessed from ACCIS. At the time of this study, there were two specialized spasticity tertiary clinics in Alberta, one located in Calgary (visit information captured in Millennium Scheduler) and one located in Edmonton (visit information captured in VAX). Practitioner Claims includes information on fee-for-service, alternative payment plan billing, and shadow billing. PIN contains information on dispensed prescription medications from all community pharmacies. Information on deaths was obtained from Vital Statistics.
Cohort selection
Adults (≥18-years) who experienced a stroke in the community and sought acute care (ED or hospital) between April 1, 2012 and March 31, 2017 (inclusion period) were considered for inclusion in the study; those who had AHCIP coverage ≥2-years before, and coverage ≥3-years after the index stroke event (first stroke within the inclusion period) or until death, whichever occurred first, were included in the overall cohort. Stroke was defined as an International Classification of Diseases, Tenth Revision – Canadian Enhancement (ICD-10-CA) G08, I60, I61, I62.9, I63, I64, I67.6 or H34.1 code occurring within the most responsible diagnostic field. 16 Transient ischemic attacks were not included; strokes that occurred during the acute care episode were also not included as individuals with a complication of stroke occurring in-hospital have different characteristics from those experiencing stroke in the community. 16–Reference Fluck, Fry and Rankin18
Those who initiated treatment for PSS (first outpatient pharmacy dispensation of an anti-spastic medication [baclofen, tizanidine or dantrolene], first focal chemo-denervation [botulinum toxin] injection [inpatient or outpatient], or first of ≥2 spasticity tertiary clinic visits after the index stroke event, with none of these treatments occurring during the 2-years before) up to March 31, 2019 were included in the PSS treatment group; see Supplementary Table 1 for details. Subgroups included those who initiated spasticity treatment during defined timepoints after the index stroke event that included acute (<3 months; 3–6 months) and chronic (6–12 months; 12–36 months; >36 months) phases. Reference Bernhardt, Hayward and Kwakkel13 Those who did not receive treatment for spasticity after the stroke event were included in the non-PSS treatment group. To our knowledge, there is currently no validated case-finding algorithm to identify spasticity within administrative health data. Therefore, individuals in the non-PSS treatment group encompassed those who did not develop spasticity, along with those who developed spasticity but did not require intervention, or developed disabling spasticity and did not receive any intervention or received treatment that could not be identified within administrative health data (e.g., non-publicly funded community-based rehabilitation).
Study measures
Characteristics were presented for the overall cohort and by PSS treatment status, as well as by time to initiation of PSS treatment. Baseline characteristics determined on the stroke index date included age, sex, urban or rural residence, Reference du Plessis, Beshiri, Bollman and Clemenson19 and stroke type. The Charlson Comorbidity Index score was determined during the 2-year pre-index period that included 17 different specific medical conditions weighted according to their potential for influencing mortality Reference Lix, Smith and Pitz20 ; see Supplementary Table 2. Those who experienced a previous stroke as far back as April 1, 2002 were also reported. After the index stroke event, those who experienced a subsequent stroke were reported, as well as those who died up to March 31, 2020. For those in the PSS treatment group who initiated treatment ≥12 months after the index stroke, additional conditions that are known to cause spasticity (traumatic brain injury, spinal cord injury, myelopathy, multiple sclerosis and transverse myelitis) were identified between the index stroke event and the date of PSS treatment initiation (see Supplementary Table 3 for details). Reference Chen and Colantonio21–Reference Gerber, Cowling, Chen, Yeung, Duquette and Haddad23
Pathways of stroke care within the health care system were determined during the 3-year period after the index stroke event or until death, whichever occurred first. Each pathway began within the health care setting where the index stroke was diagnosed and continued within and across the ED, acute inpatient care, inpatient rehabilitation, and/or long-term care. A pathway of care ended when a patient was discharged home, died or within the setting they were residing other than home at the end of the 3-year period, whichever occurred first. Admission to acute inpatient care, inpatient rehabilitation or long-term care within 3-days after discharge from the ED were considered a continuation in the pathway. 17 Also, if a patient was discharged from acute inpatient care and then (re)admitted (to acute inpatient care, inpatient rehabilitation or long-term care) within 28-days, this was considered a continuation in the pathway. 17,24
The pathway of care setting where PSS treatment was initiated, and timing (number of days) from the index stroke event until treatment initiation were reported. As dispensations for baclofen, tizanidine and dantrolene could only be determined in the outpatient setting, the number of individuals who initiated these medications ≤30-days after discharge from an inpatient setting within their pathway of stroke care was reported to estimate the number of individuals who may have initiated treatment earlier than identified after their index stroke, potentially within an inpatient setting.
Statistical analysis
Descriptive statistics were reported as counts and percentages, and means and standard deviations (SD) or medians and interquartile ranges (IQR), where appropriate. Analyses were performed using SAS 9.4 software. In accordance with data custodian privacy standards, outcomes with one to nine individuals were reported as <10, and associated results censored (e.g., presented as a range) so that the number of individuals (e.g., one to nine) could not be calculated.
Results
Subject selection
Among the 26,505 adults who had a stroke during the inclusion period, 24,307 met criteria for the stroke cohort (Figure 1). Within this cohort, 22,922 were included in the non-PSS treatment group, and of the 1,164 individuals who initiated spasticity treatment after the index stroke event, 1,079 were included in the PSS treatment group (Figure 1). Spasticity treatment was initiated within 3 months for 19%, 3–6 months for 18%, 6–12 months for 20%, 12–36 months for 29% and >36 months for 14% of individuals in the PSS treatment group (Figure 1). Of the 469 individuals who initiated spasticity treatment ≥12 months after the index stoke event, 6% (n = 28) were identified as having an additional condition other than stroke (between the index stroke event and initiation of spasticity treatment) that may cause spasticity (see Supplementary Table 3).
Cohort selection. Abbreviations: AHCIP = Alberta Health Care Insurance Plan; ED = emergency department; HOS = hospitalization; PSS = poststroke spasticity.

Characteristics
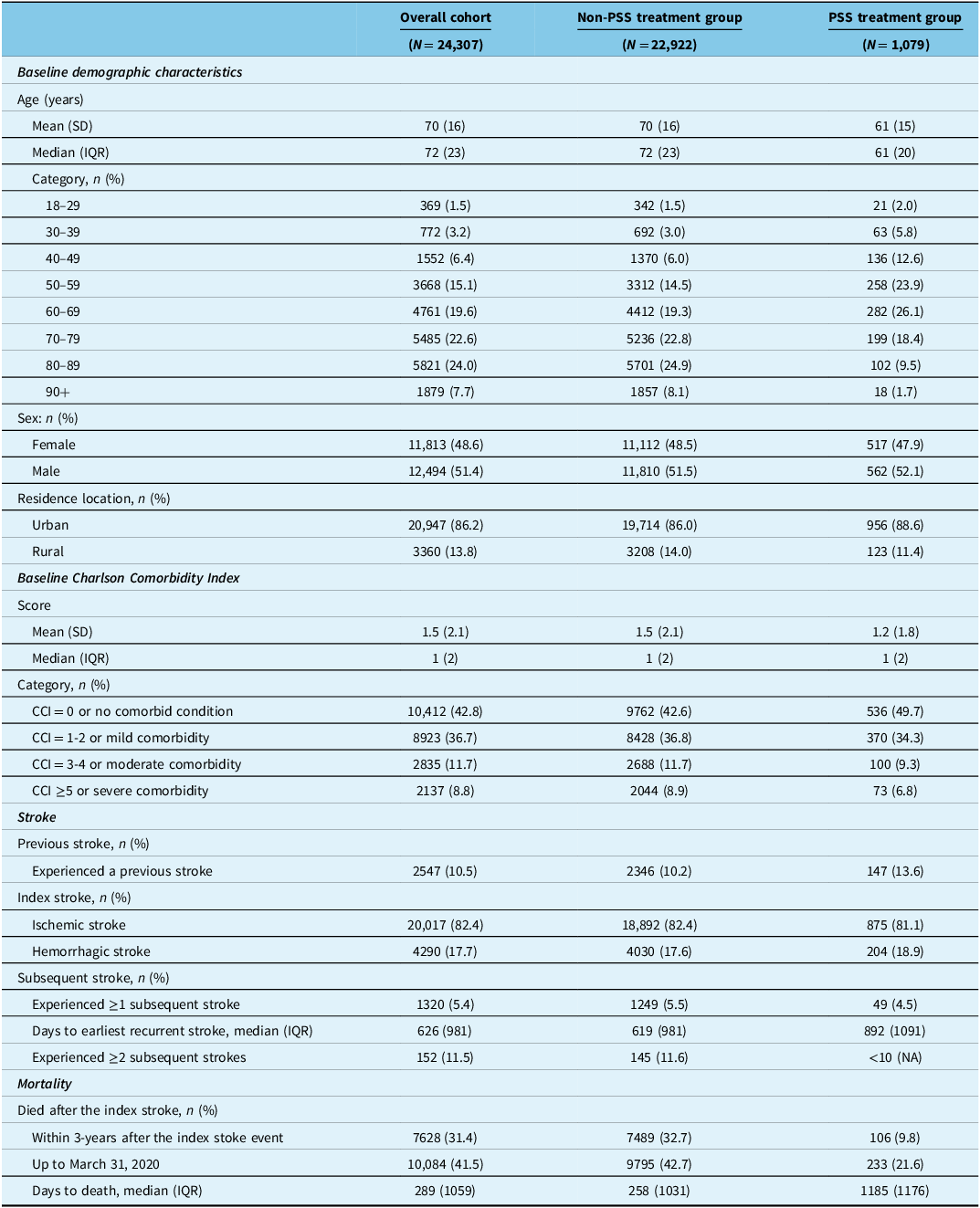
Overall, on the date of the index stroke event (ischemic stroke: 82%; hemorrhagic stroke: 18%), the mean age of the total cohort was 70 (SD 16) years (non-PSS treatment group was 70 [SD 16] years; PSS treatment group was 61 [SD 15] years), 49% were females and 51% were males, a majority lived in urban areas (86%), and the mean Charlson Comorbidity Index score was 1.5 (SD 2.1) (Table 1). Mortality at 3-years after the index stroke event was 10% in the PSS treatment group and 33% in the non-PSS treatment group. Characteristics of the PSS treatment subgroups are presented in Supplementary Table 4.
Characteristics of the cohort

Note: CCI = Charlson Comorbidity Index; IQR = interquartile range; NA = not applicable; PSS = poststroke spasticity; SD = standard deviation.
Pathways of stroke care
Overall, 84% (n = 20,419) of patients who experienced a stroke in the community started their care pathway in the ED and 16% (n = 3,888) started in acute inpatient care (see Supplementary Figure 1). The vast majority of those who started their pathway in acute inpatient care (where stroke was first listed in the most responsible diagnostic field) were admitted through the ED (92%; n = 3,574).
The most common health care settings within the pathways of stroke care that the non-PSS treatment group encountered were the ED (84%), followed by acute inpatient care (69%), long-term care (13%) and inpatient rehabilitation (12%) (Supplementary Figure 2). Regarding specific pathways of stroke care, many different combinations and sequences of pathways existed (Supplementary Figure 2). Outlined in Figure 2, the five most common pathways of care experienced by 74% of the non-PSS treatment group included: 1) ED to acute inpatient care (32%, n = 7,453), 2) ED only (19%, n = 4,272), 3) acute inpatient care only (10%, n = 2,344), 4) ED to acute inpatient care to acute inpatient rehabilitation (∼8%, n = 1,817 to 1,835), and 5) ED to acute inpatient care to long-term care (5%, n = 1,073). The remaining 26% of care pathways included a number of ‘other’ pathways (different and often complicated pathways that had very few individuals within each; 20%, n = 4,643), those that began in acute inpatient care and then either moved through inpatient rehabilitation (2%, n = 367) or to/through long-term care (2%, n = 406), and those that began in the ED and moved to/through long-term care (2%, n = 519 to 537) (Figure 2; detailed in Supplementary Figure 2).
Poststroke care pathways of the non-PSS treatment group. Solid lines show the most common care pathways, and dotted lines show the less common care pathways. Other dispositions were discharges other than to home or deaths such as non-acute care or correctional facilities. Other pathways included a number of different and often complicated pathways that had very few episodes within each pathway; these included those who were still in the care setting at the end of observation period, continued their pathway with another stoke episode, experienced a pathway other than those listed, or was unknown. Abbreviations: ED = emergency department; PSS = poststroke spasticity.

Within the PSS treatment group, the most common health care settings that patients encountered within the pathways of stroke care were the ED (86%), acute inpatient care (80%), inpatient rehabilitation (40%) and long-term care (19%) (Supplementary Figure 3). Outlined in Figure 3, the six most common pathways of care experienced by 74% of the PSS treatment group included: 1) ED to acute inpatient care to inpatient rehabilitation (27%, n = 288), 2) ED to acute inpatient care (∼16%, n = 166 to 182), 3) ED only (15%, n = 167), 4) ED to acute inpatient care to long-term care (∼6%, n = 55 to 73), 5) acute inpatient care only (5%, n = 55 to 65), and 6) acute inpatient care to inpatient rehabilitation (5%, n = 52). The remaining 26% of stroke pathways included a number of “other” pathways (∼22%, n = 235 to 251), and those that began in either the ED or acute inpatient care and ended with a transition to long-term care (2% each) (Figure 3; detailed in Supplementary Figure 3).
Poststroke care pathways of the PSS treatment group. Solid lines show the most common care pathways, and dotted lines show the less common care pathways. Other dispositions were discharges other than to home or deaths such as non-acute care or correctional facilities. Other pathways included a number of different and often complicated pathways that had very few episodes within each pathway; these included those who were still in the care setting at the end of observation period, continued their pathway with another stoke episode, experienced a pathway other than those listed, or was unknown. Abbreviations: ED = emergency department; PSS = poststroke spasticity.

Spasticity treatment
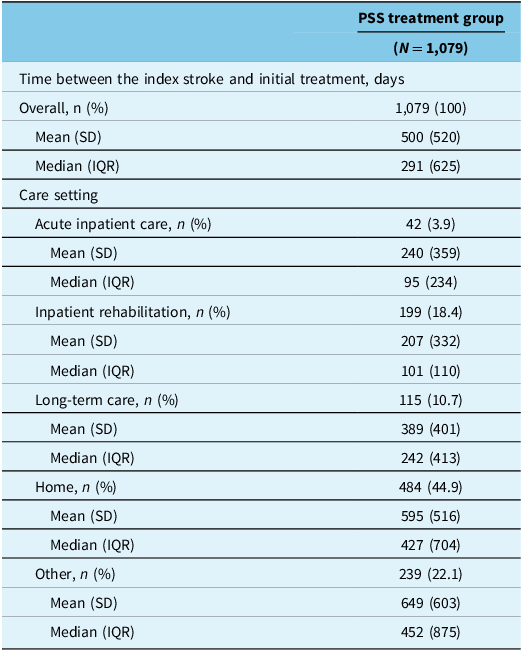
Spasticity treatment was most commonly initiated in the community setting (45% of the PSS treatment group started when residing at home; Table 2), particularly in the chronic phases of stroke recovery (>6-months poststroke; Supplemental Table 3). Treatment during the acute phases of stroke recovery (<6-months poststroke) was most often initiated within the inpatient rehabilitation setting (41% at<3-months poststroke and 35% at 3–6 months poststroke; Supplementary Table 5).
Initial poststroke spasticity treatment

Note: IQR = interquartile range; SD = standard deviation.
Overall, spasticity treatment was initiated a median of 9.5 months (291 [IQR 625] days) after the index stroke event, and ranged from a median of 3 months (95 [IQR 234] days) (acute inpatient care) to 15 months (452 [IQR 875] days) (“other” care setting) across the different health care settings (Table 2). Among the specific pathways of stroke care, those individuals who were discharged home after care in the ED only (n = 93) or acute inpatient care only (n = 52) initiated spasticity treatment the longest after the index stroke event (between 18 and 23 months; median 555 [IQR 902] days to 691 [IQR 1,061] days) (Supplementary Figure 3); 8% (n = 12) of these individuals were identified as having an additional condition other than stroke (between the index stroke event and initiation of spasticity treatment) that could cause spasticity (see Supplementary Table 3).
Less than 4% (n = 41) of individuals within the PSS treatment group initiated baclofen, tizanidine or dantrolene ≤30-days after discharge from an inpatient setting within their pathway of stroke care.
Discussion
In this retrospective, observational, population based, cohort study that included 24,307 adults in Alberta who had a stroke in the community and sought acute care between 2012 and 2017, pathways of stroke care within the health care system were determined overall, and for those who initiated PSS treatment and those who did not. Among those who underwent PSS treatment, the time from the stroke event to treatment initiation and the setting where treatment was initiated were also reported. It was found that the majority of adults who did not receive PSS treatment moved through five main pathways of stroke care, and those who received PSS treatment moved through six. Among those who underwent PSS treatment, most initiated treatment 9.5 months after the index stroke event, while residing in the community setting.
Disabling or problematic spasticity after stroke can impose a significant burden on an individual, negatively impacting function and health-related quality of life. Reference Zorowitz, Gillard and Brainin5,Reference Francisco, Wissel, Platz, Li and Platz6,Reference Gillard, Sucharew and Kleindorfer25 However, studies investigating the incidence of disabling PSS where there is a need for intervention are scarce. Reference Zeng, Chen, Guo and Tan8 Lundström et al. (2010) evaluated 49 adults with a first-ever stroke and found that disabling PSS was present in 2% of patients at 1-month and 13% at 6 months. Reference Lundström, Smits, Terént and Borg26 In the current study, 5% of people who experienced a stroke subsequently initiated pharmacotherapy or visited a specialized clinic for the treatment of spasticityFootnote 1 ; this may under-represent the number of individuals who initiated PSS treatment, as non-publicly funded community-based rehabilitation (e.g., physical therapy, occupational therapy) was not available for measurement in this study.
Pathways of care for stroke survivors have been previously reported in Canada. Among those who experienced a stroke between 2006 and 2010 in Ontario, the most common pathways of care were similar to those found for the overall cohort in the current study. 17 Among those who initiated PSS treatment in this study, the most common pathways of stroke care included inpatient rehabilitation, of which 40% experienced this health care setting, and where PSS treatment was most often initiated during the acute phases of stroke recovery (<6-months poststroke). The 2019 Canadian best practice recommendations for stoke advise that inpatient rehabilitation is indicated for patients with moderate-to-severe stroke. Reference Teasell, Salbach and Foley11 A recent systematic review and meta-analysis found that one of the most significant risk factors for the development of PSS is moderate-to-severe paresis, and Katoozian et al. (2018) reported that PSS is more common in persons with lower functional abilities. Reference Zeng, Chen, Guo and Tan8,Reference Katoozian, Tahan, Zoghi and Bakhshayesh27 Therefore, it is plausible that a number of stroke survivors who developed PSS in this study had moderate-to-severe stroke sequelae and were managed according to best practice; however, this cannot be confirmed without clinical evaluative data.
Early identification and timely management of disabling or problematic spasticity has been suggested, which may provide better motor and functional outcomes, as spasticity has been implicated in secondary maladaptation and impairment such as restricted joint mobility, stiffness and pain. Reference Francisco, Wissel, Platz, Li and Platz6,Reference Bavikatte, Subramanian, Ashford, Allison and Hicklin10 Although the incidence of PSS has been shown to be highest in the first month, there is currently no consensus on the timeframe that defines early treatment for spasticity. Reference Teasell, Salbach and Foley11,Reference Patel, Ward, Geis, Jost, Liu and Dimitrova28,Reference Wissel, Ri and Kivi29 The 2019 Canadian best practice recommendations for stroke define therapies delivered within 6-months post stroke as early interventions, and define those delivered more than 6-months post stroke as late interventions. Reference Teasell, Salbach and Foley11 In the current study, 37% of individuals who received spasticity treatment started within the first 6-months after the stroke event, and 63% started more than 6-months post stroke. Those who initiated spasticity treatment a median of greater than 6-months post stroke moved through the ED (84%), acute inpatient care (81%), inpatient rehabilitation (36%), and/or long-term care (9%) before starting treatment while residing at home (58%), “other” care settings or pathways (24%) or long-term care (19%). As the majority of individuals initiated spasticity treatment more than 6-months post stroke and moved through various acute health care settings before starting treatment in this study, earlier identification and treatment of PSS may be beneficial; this may include strategies such as instituting a post stroke screening assessment for spasticity into stages of care. A number of screening assessments have been developed for PSS Reference Bavikatte, Subramanian, Ashford, Allison and Hicklin10,Reference Zorowitz, Wein and Dunning30,Reference Christofi, Bch and Ashford31 ; evaluation of the implementation of these tools across the continuum of acute care is needed to ensure they are useful and optimize management and outcomes.
Care pathways of stroke for individuals who initiated PSS treatment the longest after their index stroke event included the ED only (spasticity treatment initiated a median of 18 months after stroke in 93 individuals) or acute inpatient care only (spasticity treatment initiated a median of 23 months after stroke in 52 individuals) before being discharged home. A clinical review conducted by Chang et al. (2018) and the 2019 Canadian best practice recommendations for stroke indicate that discharge from the ED may be a safe and effective strategy for some forms of mild stroke without disabling deficits (after careful evaluation and screening for rehabilitation requirements and the appropriate setting for rehabilitation), and early-supported discharge from acute inpatient care is beneficial for some patients with mild impairments. Reference Teasell, Salbach and Foley11,Reference Chang, Rostanski, Willey, Kummer, Miller and Elkind32 Although not reported as a common risk factor for the development of spasticity, it is possible that these individuals experienced a mild stroke, did not have significant deficits at the outset, and were managed appropriately in the acute care setting. Considering the lengthy period of time these individuals were residing at home before PSS treatment was initiated, it is likely that a delay in the identification and/or management of PSS occurred within the community setting. It is also possible that disabling spasticity did not develop until the chronic phase of stroke recovery and was treated within a timely manner; however, this is less likely as development of spasticity at 12 months poststroke is considered infrequent. Reference Kong, Lee and Chua9
There may be a number of potential opportunities to improve earlier identification and/or management of PSS within the outpatient setting. Results from a survey of primary care physicians across Canada found that only 32% felt adequately trained to recognize spasticity, and the vast majority were unable to identify evidence-based best practice recommendations for the management of spasticity. Reference Goldstein, Phadke, Ismail and Boulias33 Additionally, wait times for access to spasticity tertiary clinics in Alberta are approximately 4 months. 34 Therefore, PSS education and training are needed in primary care, as well as investment to improve timely access to spasticity tertiary clinics with fully resourced specialized interdisciplinary teams. Recognizing the strain on primary care in the current Canadian healthcare system, Reference Flood, Thomas and McGibbon35 another option that may help improve identification of PSS are patient-facing educational resources for self-recognition of spasticity. Also, many individuals will have follow-up with outpatient stroke prevention clinics in the months after their stroke, so educating healthcare providers who work in this setting on the recognition of spasticity and potential interventions may be useful in promoting earlier treatment. Similarly, education of clinicians working in long-term care may be beneficial, as 19% of those who initiated spasticity treatment a median of greater than 6-months post stroke were residing in long-term care when treatment was initiated in this study. Lastly, as many individuals receive a prescribed medication regimen to prevent recurrent stroke and adverse outcomes, training pharmacists to inquire about whether an individual has received assessment for spasticity may support earlier identification of PSS. All in all, this study points to the fact that there are considerable opportunities for education of individuals and many care providers about spasticity. Assessment of these strategies is necessary to confirm their utility in the outpatient setting.
This study has several important strengths, including the large size and population based design. However, this study is also subject to limitations that should be taken into consideration when interpreting results. While retrospective administrative claims-based studies use administrative data as opposed to medical records, creating potential for misclassification of study cohorts or outcomes, an established case definition was used to identify the study cohort, and pathways of care were found to be similar to others. 16,17 However, Hall et al. (2016) found that the accuracy of administrative data for the identification of stroke was greater in inpatient data (sensitivity: 82%; positive predictive value [PPV]: 69%) than ED data (sensitivity: 57%; PPV: 59%) (36); therefore, it is likely that some individuals in the non-PSS treatment group who only visited the ED in this study (10% of the total cohort; n = 2,344) may have had a condition that mimicked stroke symptoms. Although all major stroke rehabilitation units in Alberta report data to the NRS, it is possible that some individuals from smaller inpatient rehabilitation units were not reported to the NRS, and therefore may have only been identified as being within acute inpatient care (identified through mandatory reporting in the DAD) in the study. Non-publicly funded community-based rehabilitation was not captured within provincial administrative data, and therefore not included; as a result, the number of individuals who initiated PSS treatment may be somewhat greater than reported. Information on hospital-based pharmacy dispensations were not available at the time of this study. This data limitation potentially impacted up to 4% of the PSS treatment group; a few may have initiated baclofen, tizanidine or dantrolene earlier after their index stroke within an inpatient setting (as opposed to the community setting). PIN only provides information on prescription medication dispensations from community pharmacies, and therefore may not represent actual medication uptake by individuals.
Conclusions
To our knowledge, this is the first population based cohort study describing health system pathways of care among adults with stroke who sought acute care and subsequently did or did not initiate spasticity treatment. Findings indicate that strategies to increase earlier identification and management of spasticity across the continuum of care for stroke survivors merit further study, and may include spasticity screening assessments, patient-facing educational resources for self-recognition of spasticity, education and training for health care providers (e.g., primary care, stroke prevention clinics, long-term care, pharmacists) and timely access to fully resourced interdisciplinary spasticity tertiary clinics teams. With that said, the identification of barriers to the early identification and management of PSS is required prior to advocating for any given strategy or intervention.
Supplementary material
The supplementary material for this article can be found at https://doi.org/10.1017/cjn.2024.42.
Data availability
The datasets analyzed during the current study are not publicly available because the data custodians, Alberta Health Services and Alberta Health do not allow users of the data to publish the data. Please contact the corresponding author for requests related to the data used in this study.
Acknowledgements
We thank the participants of this study. This study is based in part on anonymized raw data from Alberta Health and Alberta Health Services that was provided by the Alberta Strategy for Patient Oriented Research Unit housed within Alberta Health Services. The interpretation and conclusions contained herein are those of the researchers and do not necessarily represent the views of the Government of Alberta or Alberta Health Services. Neither the Government of Alberta/Alberta Health nor Alberta Health Services express any opinion in relation to this study. SK was supported by the Kidney Health Research Chair and the Division of Nephrology at the University of Alberta.
Author contribution
LS, HL, KM, KV and SK contributed to the study concept and design; HL, KV and PUN conducted the analyses; KM prepared the initial manuscript. All authors contributed to the interpretation of the data and critical revision of the manuscript for important intellectual content, as well as approved the final version to be published and agreed to be accountable for all aspects of the work ensuring that questions related to the accuracy of integrity of any part of the work are appropriately investigated and resolved. SK provided study supervision.
Funding statement
Funding for the study was provided by Allergan Inc. to LR. The funder had no role in the study design, analysis, interpretation of the data, drafting of the manuscript or in the decision to submit for publication. The funders had the right to comment on the protocol and the manuscript prior to submission, but final decisions remained with LR and SK.
Competing interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship and/or publication of this article: HL, KM, KV, PUN, LR, TW and SK are members of the Alberta Real World Evidence Consortium, an academic entity that conducts research including investigator-initiated industry-funded studies. Payment received for consultancy, participation on an advisory board and/or honoraria were reported for AbbVie (LS, SD, JY), Ipsen (LS, SD), and Merz (LS, SD, JY) outside of the submitted work within the past three years. No other conflict of interest was declared. All authors of this study had complete autonomy over the content and submission of the manuscript, as well as the design and execution of the study.