Introduction
Postpartum depression (PPD) affects up to 20% of birthing parents and negatively affects them and their infants (Gavin et al., Reference Gavin, Gaynes, Lohr, Meltzer-Brody, Gartlehner and Swinson2005; Letourneau et al., Reference Letourneau, Stewart, Dennis, Hegadoren, Duffett-Leger and Watson2011; Racine et al., Reference Racine, Hetherington, McArthur, McDonald, Edwards, Tough and Madigan2021). It is also associated with less optimal parenting practices (Slomian et al., Reference Slomian, Honvo, Emonts, Reginster and Bruyère2019)and more cognitive, emotional, and behavioral problems in offspring (Grace et al., Reference Grace, Evindar and Stewart2003; Liu et al., Reference Liu, Kaaya, Chai, McCoy, Surkan, Black, Sutter-Dallay, Verdoux and Smith-Fawzi2017). Indeed, up to two-thirds of the costs associated with PPD are due to its effects on infants and children (Bauer et al., Reference Bauer, Knapp and Parsonage2016).
Evidence-based psychotherapies like cognitive-behavioral therapy (CBT) are first-line treatments for PPD and are favored by many birthing parents over antidepressant medication (Goodman, Reference Goodman2009; MacQueen et al., Reference MacQueen, Frey, Ismail, Jaworska, Steiner, Lieshout, Kennedy, Lam, Milev, Parikh and Ravindran2016). While CBT is an effective treatment for PPD in birthing parents, much less attention has been paid to infant outcomes following maternal treatment, with existing studies yielding inconsistent results (e.g., Ammerman et al., Reference Ammerman, Peugh, Putnam and van Ginkel2012; Cicchetti et al., Reference Cicchetti, Rogosch and Toth2000; Cohen et al., Reference Cohen, Lojkasek, Muir, Muir and Parker2002; Cooper et al., Reference Cooper, Murray, Wilson and Romaniuk2003).The majority of extant studies have relied solely on maternal reports of infant outcomes which may not fully capture the subtle yet important changes that occur in preverbal infants after maternal PPD treatment.
Mixed findings in the literature on infant outcomes following maternal PPD treatment may reflect variability in how infants respond to changes in the caregiving environment, an idea supported by developmental frameworks like the differential susceptibility model, which emphasize that individual traits shape sensitivity to environmental influences (Belsky & Pluess, Reference Belsky and Pluess2009; Pluess & Belsky, Reference Pluess and Belsky2011). Indeed, studies on the impact of PPD treatment on offspring have largely overlooked the role of infant traits in their adapting to the shifting dynamics of maternal caregiving post-treatment. Since treatment for maternal PPD can modify a parent’s emotions and caregiving behaviors (Liu et al., Reference Liu, Kaaya, Chai, McCoy, Surkan, Black, Sutter-Dallay, Verdoux and Smith-Fawzi2017), identifying traits that influence the putative changes infants undergo when their birthing parent with PPD is treated can help birthing parents, their families, and healthcare providers recognize which infants and parent-infant pairs may need additional support beyond maternal care alone.
Decades of research suggest that temperamental fear in infancy is a trait that has been associated with a range of long-term socioemotional and behavioral outcomes (Fox & Henderson, Reference Fox and Henderson1999; Tang et al., Reference Tang, Crawford, Morales, Degnan, Pine and Fox2020; Van Hulle et al., Reference Van Hulle, Moore, Lemery-Chalfant, Goldsmith and Brooker2017), with fearful infants demonstrating unique patterns of interaction with their parents (Kochanska et al., Reference Kochanska, Murray and Coy1997; Volling & Feagans, Reference Volling and Feagans1995). Infants identified as fearful have been found to show greater anxiety by middle childhood (Van Hulle et al., Reference Van Hulle, Moore, Lemery-Chalfant, Goldsmith and Brooker2017), increased risk for social anxiety disorder in adolescence (Chronis-Tuscano et al., Reference Chronis-Tuscano, Degnan, Pine, Perez-Edgar, Henderson, Diaz, Raggi and Fox2009), and by adulthood, higher levels of introversion along with more social and mental health difficulties (Tang et al., Reference Tang, Crawford, Morales, Degnan, Pine and Fox2020). Other work emphasizes the potentially adaptive nature of fear. For instance, Graham et al. (Reference Graham, Buss, Rasmussen, Rudolph, Demeter, Gilmore, Styner, Entringer, Wadhwa and Fair2016) found that amygdala connectivity to the ventral anterior cingulate cortex predicted a phenotype of high fear and advanced cognitive skills, suggesting higher fear may be adaptive when paired with cognitive maturity. Similarly, other studies have shown that early fearfulness can be linked to the development of prosocial emotions (Kochanska et al., Reference Kochanska, Murray and Harlan2000), and lower levels of aggression in early childhood (Rothbart & Bates, Reference Rothbart and Bates1998). Taken together, these findings suggest that fear is a developmentally important trait whose implications vary by context, a core feature of the differential susceptibility model.
Temperamental fear appears to have a strong physiological basis, involving both the central nervous system, through the amygdala-prefrontal cortex pathway, and the peripheral nervous system, particularly the autonomic nervous system (ANS), which regulates bodily responses to fear (Porges & Furman, Reference Porges and Furman2011; Tottenham, Reference Tottenham2020). When fear is triggered, the sympathetic nervous system (SNS), a branch of the ANS, activates the ‘fight or flight’ response, preparing the body for action. The parasympathetic nervous system (PSNS) counterbalances the SNS, promoting relaxation once the fear-inducing stimuli have subsided (Porges & Furman, Reference Porges and Furman2011; Thayer et al., Reference Thayer, Mather and Koenig2021).
Heart rate variability (HRV), which represents the variability in the beat-to-beat intervals of the heart due to the interplay between the SNS and PSNS, is thought to reflect infant’s ability to adapt to changing emotional or environmental demands (Field & Diego, Reference Field and Diego2008). High-frequency HRV (HF-HRV) in particular, often measured as Respiratory Sinus Arrhythmia, more specifically indexes PSNS activity and there is evidence that resting levels of HF-HRV are associated with an individual’s sensitivity to their environment. Both low (e.g. Obradović, Reference Obradović2012) and high (e.g. Eisenberg et al., Reference Eisenberg, Sulik, Spinrad, Edwards, Eggum, Liew, Sallquist, Popp, Smith and Hart2012) resting HF-HRV have been linked to greater susceptibility to environmental influences. Studies have found that HF-HRV may itself be altered by environmental adversities, particularly PPD exposure, with a significant body of literature linking higher HF-HRV to better emotion regulation and adaptability to environmental changes (Field et al., Reference Field, Diego, Dieter, Hernandez-Reif, Schanberg, Kuhn, Yando and Bendell2001, Reference Field, Diego, Hernandez-Reif, Schanberg and Kuhn2003; Hernandez-Reif et al., Reference Hernandez-Reif, Diego and Field2006; Sevenster et al., Reference Sevenster, Hamm, Beckers and Kindt2015)with Somers et al. (Reference Somers, Luecken, Spinrad and Crnic2019) reporting that infants with low resting state HF-HRV appear to be at greater risk for adverse outcomes relative to those with greater HF-HRV. Moreover, the HF-HRV isdecreased in infants of birthing parents with depression (Amani et al., Reference Amani, Krzeczkowski, Savoy, Schmidt and Van Lieshout2023; Gentzler et al., Reference Gentzler, Rottenberg, Kovacs, George and Morey2012)and can also reflect states of fear and startle (Sevenster et al., Reference Sevenster, Hamm, Beckers and Kindt2015). Moreover, infants with low resting state HF-HRV appear to be at greater risk for adverse outcomes relative to those with greater HF-HRV.
Frontal brain regions are also crucial for higher executive functioning and modulation of responses during fearful situations (Graham et al., Reference Graham, Buss, Rasmussen, Rudolph, Demeter, Gilmore, Styner, Entringer, Wadhwa and Fair2016). Frontal alpha asymmetry (FAA), which reflects hemispheric differences in frontal brain activity, typically presents as higher right FAA at rest in infants of depressed birthing parents and is linked to poorer emotion regulation FAA can also reflect individual differences in fear processing (Liu et al., Reference Liu, Snidman, Kagan and Tronick2020).
To date, it remains unclear if infant fear, a developmentally important trait, impedes potential adaptive changes in infant emotion regulatory capacity following maternal receipt of PPD treatment. In the present study, we examine whether infants’ temperamental fear predicts the extent of their physiological improvement (measured through HF-HRV and FAA) following maternal receipt of group cognitive-behavioral therapy for PPD. Assessing fear in the context of PPD treatment could reveal infants who may be at risk for suboptimal outcomes following maternal treatment for PPD and could enable interventions to be optimized for the benefit of both these offspring and their birthing parents.
Methods
Participants
The study sample was comprised of 80 infants and their birthing parents recruited from Hamilton, Ontario, Canada, and nearby municipalities between March 2016 and July 2019. Participants were divided into two groups: case (PPD) dyads and control dyads. The case group was comprised of 40 birthing parents with major depressive disorder (MDD) diagnosed within the first year of delivery, along with their infants. These birthing parents were patients of the Women’s Health Concerns Clinic, a specialty perinatal mental health clinic located at St Joseph’s Healthcare Hamilton in Ontario, Canada. Individuals with MDD and attending the clinic were given the option to receive a 9-week group CBT for PPD intervention and participants were invited to participate in the current study during the first CBT session. To be eligible, birthing parents had to have a primary diagnosis of MDD, but not bipolar disorder, a schizophrenia spectrum disorder, and/or a substance use disorder. Psychiatric diagnoses (DSM-5) were made by mental health clinicians (e.g., nurses, and social workers) using a semi-structured interview format and were confirmed by a psychiatrist. Individuals who had co-morbid psychiatric conditions were eligible. Additionally, those with other physical health problems were eligible, though none were present in the sample. Individuals who were not fluent in English or whose infants were older than 12 months were also not eligible to participate. Fourteen participants (35%) received a diagnosis of MDD before childbirth, while twenty-six (65%) were diagnosed during the postpartum period.
Control infants (n = 40), born to birthing parents without PPD, were matched 1:1 with case infants on age, sex, and familial socioeconomic status (SES; total household income [Canadian Dollars {CAD}]). This group was recruited to attempt to reduce the likelihood that any observed changes or associations following maternal PPD treatment in case infants were due to developmental factors (e.g., occurring with age), sex, or other early experiences. Birthing parents in the healthy control group did not receive any intervention. These control dyads were recruited from the Infant Database of the Department of Psychology at McMaster University, which recruited from a similar catchment area to case dyads. Birthing parents who were not fluent in English, screened positive on the major depressive episode (current) module of the Mini International Neuropsychiatric Interview (Lecrubier et al., Reference Lecrubier, Sheehan, Weiller, Amorim, Bonora, Sheehan, Janavs and Dunbar1997), were taking psychotropic medications, and/or had infants older than 12 months were excluded.
PPD intervention group (Case dyads)
Cases (birthing parents with PPD) received a nine-week group CBT for PPD intervention (Van Lieshout et al., Reference Van Lieshout, Yang, Haber and Ferro2017), delivered weekly by a pair of psychotherapists. Each session lasted two hours, the first half of which covered core CBT content, while the second half involved discussions on relevant topics co-led by both patients and therapists. We used the Edinburgh Postnatal Depression Scale (EPDS) to assess birthing parents’ improvement in depressive symptoms following the intervention. The EPDS is a gold-standard measure of PPD symptoms which consists of 10 self-reported items that assess depressive symptoms experienced in the previous week (Cox et al., Reference Cox, Holden and Sagovsky1987). Birthing parents also completed the Postpartum Bonding Questionnaire (PBQ), which is scored on a 6-point scale (0–5) (Brockington et al., Reference Brockington, Oates, George, Turner, Vostanis, Sullivan, Loh and Murdoch2001). The PBQ assesses the quality of the mother-infant bond after childbirth, detects potential problems within the relationship. This study focused on the impaired bonding subscale given its high sensitivity and ability to reflect bonding quality between birthing parents and their offspring (Brockington et al., Reference Brockington, Oates, George, Turner, Vostanis, Sullivan, Loh and Murdoch2001). The impaired bonding subscale (Cronbach’s α = 0.69) has 12 questions and higher impaired bonding scores indicate poorer bonding.
Study design
Data on the effectiveness of CBT in this sample of birthing parents was published previously (Krzeczkowski et al., Reference Krzeczkowski, Schmidt and Van Lieshout2021) and so are not the focus of the current study. However, briefly: 80 mother-infant dyads participated, 40 with PPD who received the 9-week group CBT intervention, and 40 matched healthy controls who did not require CBT. At baseline, birthing parents with PPD reported significantly higher depressive symptoms on the EPDS compared to controls. Those who received treatment showed a statistically significant reduction in depressive symptoms (mean EPDS decrease = 4.1 points, p = .001, Cohen’s d = 0.75).
In the present study, we report data gathered at three time points. For case dyads, Visit 1 (T1), occurred after the first CBT session, Visit 2 (T2) took place immediately after treatment completion, and Visit 3 (T3) occurred three months after the CBT group had concluded. Control dyads had data collected during a baseline session (T1), 9 weeks later (T2), and three months after that (T3). All assessments were conducted at the Child Emotion Laboratory at McMaster University. The study received approval from the Hamilton Integrated Research Ethics Board (Study Number 0912), and all participants provided their informed consent before participating. This study’s hypotheses were not pre-registered.
Measures
Infant temperament
Infant temperament was assessed using the Infant Behavior Questionnaire-Revised Short-Form (IBQ-R SF) and was completed by birthing parents at all three study time points. It consists of 91 questions, each of which is rated on a 7-point scale (1–7) (Putnam et al., Reference Putnam, Helbig, Gartstein, Rothbart and Leerkes2014).
Most research on infant temperament and PPD focuses on broader temperament aspects like negative emotionality (e.g.,Roubinov et al., Reference Roubinov, Epel, Adler, Laraia and Bush2022; Takács et al., Reference Takács, Smolík, Kaźmierczak and Putnam2020)While this perspective can expand our understanding of infant temperament within dyadic interactions, there is a need to delve into specific temperament domains to identify nuances within mother-infant interactions (Kousha et al., Reference Kousha, Krzeczkowski and Van Lieshout2025). In this study, we selected the fear subscale of the IBQ-R SF as the primary temperament dimension of interest, a priori. Fear has a well-established genetic basis, emphasizing innate infant traits and their potential influence on treatment outcomes. By focusing on fear, we also leverage its unique position as a temperament dimension with both behavioral significance and a strong physiological basis, rooted in well-defined neural systems such as the amygdala, prefrontal cortex, and the autonomic nervous system, systems that are also assessedby our physiological measurements (HRV and FAA). This dual relevance makes fear particularly suitable for exploring outcomes in preverbal infants within the context of our study.
The fear subscale of IBQ-R SF measures the infant’s reaction of startle or distress to sudden changes in stimulation, novel physical objects, or social stimuli (Putnam et al., Reference Putnam, Helbig, Gartstein, Rothbart and Leerkes2014). Higher scores on the fear subscale (6 questions) indicate greater infant temperamental fear. This subscale showed high internal reliability in our sample (Cronbach’s α of 0.89 in the case group and 0.83 in the control group).
High-frequency heart rate variability
Two infant electrocardiogram (ECG) electrodes were positioned on the infants’ backs, and data were wirelessly collected through Biolab software (v 3.2.3; Mindware Ltd). Mindware HRV software (v 3.3.2) was employed to examine data for artifacts and analyze it in the frequency domain. Mindware Software automatically identifies R-peaks using the Shannon’s Entropy Envelope technique, which accurately identifies peaks even in the in traces with elevated motion artifacts (Manikandan & Soman, Reference Manikandan and Soman2012). The software also identifies artifacts using the minimum artifact deviation/maximum expected deviation (MAD/MED) artifact detection algorithm (Berntson et al., Reference Berntson, Quigley, Jang and Boysen1990). Identified artifacts were manually corrected by a research assistant trained by Mindware Scientists. In keeping with Mindware protocols, data were discarded from analysis if greater than 5% of the trace required manual R-Peak correction. One trained research assistant conducted the processing for all participants.
Calculation of HF-HRV was performed automatically by the software. Power within the infant high-frequency band (0.24–1.04Hz; Laborde et al., Reference Laborde, Mosley and Thayer2017) was recorded. In the case group, HRV data were unanalyzable for n = 1 infant at T1, and n = 4 at T3 did not meet criteria for analysis due to excessive noise from infant motion and/or poor ECG sticker adherence. In the control group, n = 1 did not meet criteria for analyses at T1. At T3, n = 5 infants did not meet criteria for analyses and another 3 infants refused the ECG protocol.
Frontal EEG asymmetry
Electroencephalography (EEG) data were recorded using Netstation (v.4.4.1) with 128-electrode HydroCel sensor nets at a sampling rate of 250 Hz and referenced to the vertex (EGI Inc.). The offline analysis was performed in EEGlab. Data were re-referenced to the average and then segmented into two-second epochs with a 50% overlap. Each epoch underwent a 100% Hanning window, and a Fourier transform was utilized to extract power within the “infant” alpha (α) band (6–9Hz; Ann Bell, Reference Ann Bell2013). Frontal alpha asymmetry was computed by subtracting the natural log-transformed alpha power at the left frontal hemisphere (at site F3 [channel 24]) from the right frontal hemisphere (at F4 [channel 124]) [i.e., FAA = ln(F4) – ln(F3)].
At T1, n = 6 case infants and n = 2 control infants had unanalyzable data due to excessive noise in the EEG recording. At T2, EEG data were unanalyzable for n = 4case infants at n = 2 control infants due to excessive noise. At T3, four case infants refused the cap, one birthing parent did not wish to complete the EEG protocol, and three had excessive noise in the recording. For V3 controls, four refused the cap, and four had excessive noise in the EEG recording.
Testing procedure
During study visits, standard infant protocols (Lusby et al., Reference Lusby, Goodman, Bell and Newport2014)were followed to collect four minutes of resting-state physiological data. To account for potential influences on HF-RV and FAA measures, we collected information on factors that could impact infant physiological state before each measurement session at all 3 time points. Specifically, birthing parents provided information on their offspring’s sleep patterns (morning wake time, and last sleep episode), feeding history (time of last feeding and type: breastfeeding, formula, or solid food). Infants were positioned on the birthing parents’ laps facing forward, and a research assistant, seated at the infant’s eye level, interacted with a toy placed 50 cm in front of the infant’s face. Birthing parents were given instructions not to communicate with their infants during this period. All data collection sessions occurred between 9 AM and 3 PM.
Statistical analyses
Descriptive statistics (mean, standard deviation, percentage) summarizing study participant characteristics data were summarized for continuous variables and frequencies for dichotomous variables. Differences between case and control groups were assessed using χ2 and independent samples t-tests to investigate whether the groups differed from each other on demographic characteristics.
To examine longitudinal changes in infant physiology (HF-HRV and FAA), maternal depressive symptoms (EPDS), and infant temperament (fear), we employed repeated measures analysis of variance (ANOVA). Given that the meaning of time varied across the study phases, due to the intervention occurring only between Visit 1 (baseline) and Visit 2 (post-treatment) for the CBT group, and no corresponding time-locked event for controls, we structured the analysis to reflect these differences. Specifically, we conducted two separate repeated measures ANOVAs for each outcome: one for the treatment phase (Visit 1 to Visit 2) and one for the follow-up phase (Visit 2 to Visit 3). This approach allowed us to model time-dependent changes within each phase while accommodating variation in the definition of time across groups, helping us circumvent violations of sphericity assumptions by maintaining conceptual and statistical consistency. Each model included group (intervention vs. control) as a between-subjects factor, time (visit) as a within-subjects factor. Baseline infant fear was included as a covariate in relevant analyses. To better understand the direction and timing of significant changes identified in the repeated measure ANOVAs, we conducted paired samples t-tests comparing scores between paired time points (T1–T2 or T2–T3) within each group.
In parallel, we used linear regression models (i.e., bivariate regressions) to investigate associations between baseline (T1) infant fear, change in HRV (difference in HRV scores for T1–T2 and T1–T3), and change in FAA (difference in FAA scores for T1–T2 and T1–T3)to preserve statistical power and probe specific directional hypotheses related to infant fearfulness. Moreover, we used linear regression to assess whether baseline maternal depression or bonding correlated with baseline infant fearfulness. These regressions complement the repeated measure approach by offering greater interpretability and statistical sensitivity to detect associations within groups.
After completing our primary analyses, we conducted exploratory models testing all 14 IBQ-R SF subdomains (in addition to fear) as moderators of physiological outcomes over time. These analyses are reported in the Supplementary Materials to provide a more comprehensive look at temperament in the context of this study.
Statistically significant results were defined as p <.05 (two-tailed) and all statistical analyses were performed using the sjstats package (v0.18.2; Lüdecke Reference Lüdecke2022) and rstatix package (v0.7.2; Kassambara 2023) in RStudio.
Results
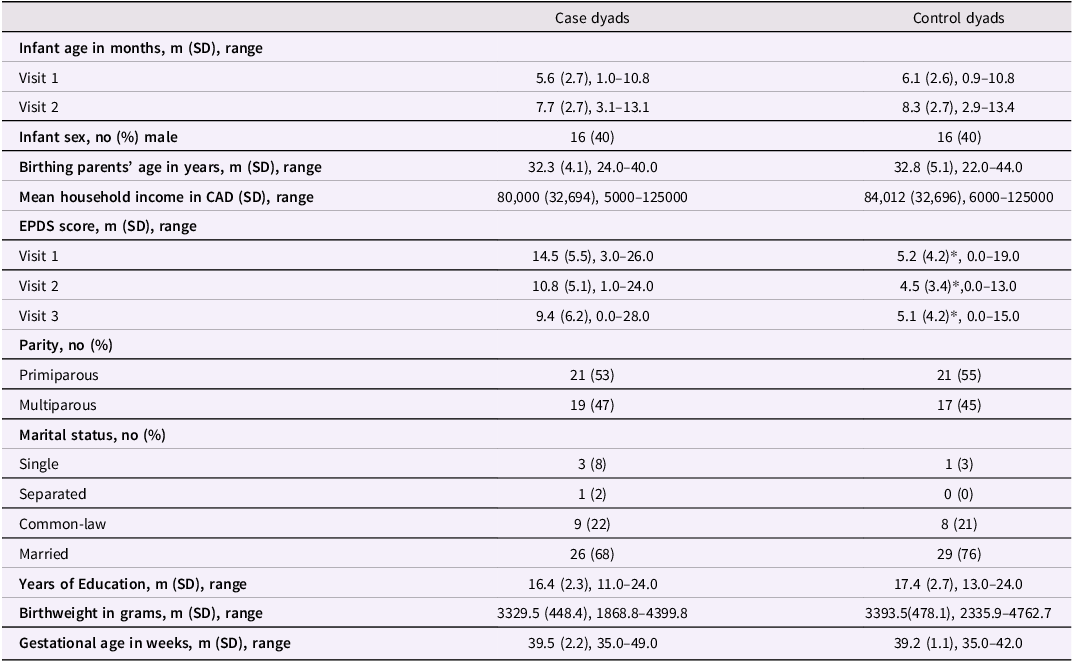
The characteristics of the sample are summarized in Table 1. We obtained data from a total of 40 birthing parents with PPD and their infants at T1, with 35 dyads providing data at T2 and T3. We also obtained data from 40 healthy control dyads at T1, with 33 dyads providing data at T2 and T3.
Sample characteristics for case and control dyads

CAD = Canadian dollars.
* denotes a statistically significant difference (p< 0.05) compared to the case group.
For the case group, the average age of birthing parents at T1 was 32.3 years (SD = 4.1), and the average age of infants was 5.6 months (SD = 2.7).Their mean before-tax household income was on average $80,000/year (Canadian dollars), and 92.1% were married or living common-law. The control dyads did not show statistically significantly different demographic characteristics compared to case groups.
In the case group, sixteen participants (40%) were diagnosed with a co-morbid psychiatric condition, most commonly generalized anxiety disorder. Fifty-five percent (22 individuals) of case birthing parents were taking antidepressant medication. Two had a medication change, and six had a dosage increase during the 9-week CBT treatment. Sixty-three percent completed all nine CBT sessions, six (15%) completed eight sessions, five (13%) completed seven sessions, and four (10%) completed six sessions. Household income, education, or marital status were not correlated with the number of CBT sessions attended. No individual participated in any other psychosocial treatments during the 9-week group. For the treatment phase (Visit 1 to Visit 2), there was a significant Time × Group interaction, F(1,70) = 8.98, p = .004). A paired samples t-test showed that EPDS scores significantly decreased in the intervention group following CBT, t(33) = 3.75, p < .001, with a moderate effect size (Cohen’s d = 0.644). In contrast, the control group showed no significant change in EPDS scores over the same period, t(37) = 1.41, p = .167.
In the follow-up phase (Visit 2 to Visit 3), which assessed the stability of effects three months post-treatment, the Time × Group interaction was not significant, F (1,55) = 4.08, p = 0.05.
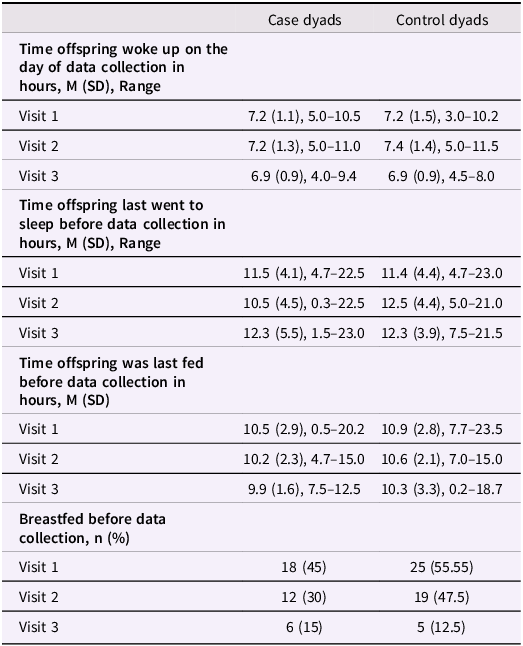
Offspring’s sleep patterns before data collection (morning wake time, and last sleep episode), feeding history (time of last feeding and type: breastfeeding, formula, or solid food) did not significantly differ between the two groups (Table 2). We found no significant correlations between these variables and HF-HRV or FAA at any of the data collection time points. Additionally, ANOVA revealed no significant differences in HF-HRV or FAA based on feeding type.
Offspring sleep and feeding times on the day of data collection

Times are in decimal hours since midnight (e.g., 2:30 PM = 14.5).
Figure 1 shows the trajectory of IBQ-R SF fear, HF-HRV, and FAA across all the visits. For fear scores, the Time × Group interaction was not statistically significant during either the treatment phase (Visit 1 to Visit 2), F (1,77) = 2.88, p = .09, or the follow-up phase (Visit 2 to Visit 3), F(1,59) = 0.05, p = 0.82. Exploratory analyses revealed that infant fearfulness at baseline did not significantly predict maternal impaired bonding scores at any time point.
Birthing parent and infant outcomes across three study visits. Values represent group means with their standard error. EPDS score significantly decreased in the case group at visit 2 (post-treatment) and visit 3 (three months later) compared to visit 1 (baseline). Control infants showed a significant increase in fear at visit 3 compared to visit 1. High-frequency HRV and frontal alpha asymmetry significantly increased in the case group at T2 and T3 compared to T1.

A repeated measures ANOVA was conducted to assess changes in infant HF-HRV from Visit 1 (baseline) to Visit 2 (post-treatment), with baseline fear scores included as a covariate. The Time × Group interaction was statistically significant, F(1,73) = 4.82, p = 0.03. Paired sample t-tests indicated that in the intervention group, HF-HRV significantly increased over time, t(38) = −3.16, p = 0.003, with a medium effect size (Cohen’s d = 0.51). In contrast, the control group showed no significant change in HF-HRV across the same period, t(37) = −0.35, p = 0.73, with a negligible effect size (Cohen’s d = 0.06).
During the follow-up phase (Visit 2 to Visit 3), the Time × Group interaction was not statistically significant, F(1,52) = 1.69, p = 0.19.
We found no significant group × visit × fear interaction during the treatment phase (F(1,72) = 0.31, p = 0.58) or the follow-up phase (F(1,51) = 0.26, p = 0.61). However, during treatment phase (V1-V2) there was a significant Time × Fear interaction (F(1,73) = 4.14, p = 0.04). There was no significant Time × Fear interaction from Visit 2 to Visit 3 (F(1,52) = 0.19, p = 0.66).To assess the specificity of fear as a moderator in the treatment phase, we tested visit × temperament subdomain interactions for all IBQ-R SF subdomains. Out of the 14 subdomains, fear remained the only subdomain that moderated how HF-HRV changes during treatment phase (Table S1). This suggested that fear may have a moderating effect, but our limited statistical power with the repeated measure might have prevented us from detecting specific moderating effects within each group.
As such, we complemented our repeated measure approach by using regression analysis that offers greater interpretability and statistical sensitivity to detect associations within groups with power estimated at ∼ 0.82.We measured changes in values of HF-HRV (ΔHF-HRV) at T2 ([HF-HRV at T1] subtracted from [HF-HRV at T2]) and T3 ([HF-HRV at T1] subtracted from [HF-HRV at T3]).In case infants, greater levels of fear at baseline (T1) were associated with less increase in HF-HRV scores (smaller ΔHF-HRV) immediately after their birthing parents completed the group CBT intervention (Correlation coefficient (R) = −0.37, p = 0.03). Three months after CBT treatment (T3), the negative correlation between baseline infant fear and ΔHF-HRV scores persisted (R = −0.47, p = 0.01). Results remained significant after controlling for infant age and sex. Baseline fear did not correlate with ΔHF-HRV scores among control infants at T2 (R = 0.04, p = 0.82) or T3 (R = −0.24, p = 0.24). When we ran similar regression analyses for all subdomains of IBQ-R SF, fear was the only subdomain at T2 and one of three subdomains at T3 (other two being low intensity pleasure and perceptual sensitivity) that maintained significant associations with ΔHF-HRV in the case group (Tables S2–S3).
A repeated measures ANOVA was conducted to examine changes in infant FAA from Visit 1 to Visit 2, with baseline fear scores included as a covariate. The Time × Group interaction was significant, F(1,64) = 8.28, p< 0.01. However, neither the Time × Fear interaction, F(1,64) = 0.03, p = 0.85, nor the three-way interaction between Time × Group × Fear, F(1,63) = 0.01, p = 0.92, reached statistical significance from Visit 1 to Visit 2. During the follow-up phase (Visit 2 to Visi 3), Time × Group interaction (F(1,45) = 1.14, p = 0.29, the Time × Fear interaction (F(1,45) = 0.23, p = 0.64), and the three-way interaction between Time × Group × Fear (F(1,44) = 0.35, p = 0.56) did not reach statistical significance. Moreover, only activity level of all the 14 subdomains of IBQ-R SF from Visit 1 to Visit 2, and none of the subdomains from Visit 2 to Visit 3 moderated how FAA changes across visits (Table S1).
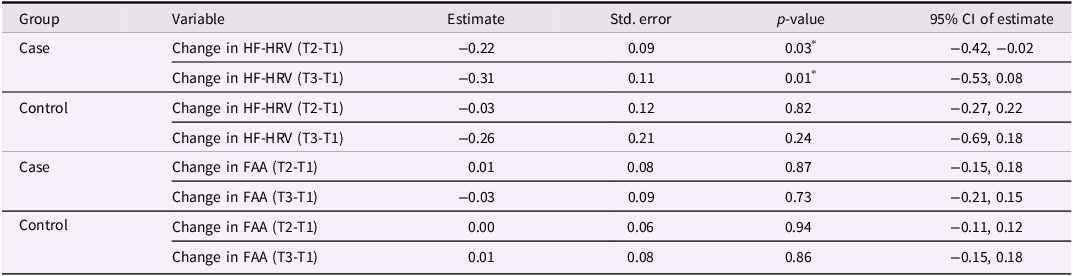
Changes in values of FAA (ΔFAA) at T2 ([FAA at T1] subtracted from [FAA at T2]) and at T3 ([FAA at T1] subtracted from [FAA at T3]) were also assessed. Infant fear at baseline was not correlated with the amount of ΔFAA from T1 to T2 (R = 0.03, p = 0.87), and T1 to T3 (R = −0.07, p = 0.73) in case infants. Moreover, baseline fear did not correlate with ΔFAA scores of healthy control infants at T2 (R = 0.01, p = 0.94) and T3 (R = 0.04, p = 0.86).None of the 14 subdomains of IBQ-R SF significantly predicted FAA changes at T2 or T3 in the case group (Tables S4–S5). Table 3 reports the regression results for the analyses between baseline fear and change in HF-HRV or FAA.
Regression results between infant fear and change in baseline HRV and FAA scores compared to T2 and T3

HF-HRV = high-frequency heart rate variability; FAA = frontal alpha asymmetry.
*denotes statistically significant difference (p< 0.05).
Discussion
In this study, the infants of birthing parents with PPD who received group CBT for PPD showed an increase in HF-HRV and a shift from right to left FAA that endured even 3 months following the cessation of group CBT, suggestive of improved emotion regulatory capacity. Fear moderated changes in HF-HRV over time, and when we increased statistical power through follow-up regression analyses, we found that infant temperamental fear was associated with smaller improvements in HF-HRV scores in the intervention group (but not the controls), both immediately post-treatment and three months later. This suggests that infant fear may limit the physiological benefits of maternal PPD treatment. To our knowledge, this is the first study to explore how infant temperament (i.e., infants’ biologically based dispositional characteristics (Shiner et al., Reference Shiner, Buss, Mcclowry, Putnam, Saudino and Zentner2012))affects infant physiological emotion regulatory outcomes following maternal receipt of PPD treatment. Indeed, the results of this study suggest that infants with greater temperamental fear were less sensitive to the beneficial effects of PPD treatment.
Prior studies in those with PPD (Field et al., Reference Field, Diego, Dieter, Hernandez-Reif, Schanberg, Kuhn, Yando and Bendell2001, Reference Field, Diego, Hernandez-Reif, Vera, Gil, Schanberg, Kuhn and Gonzalez-Garcia2004)showed that their infants exhibited lower vagal tone than those born to individuals who were not depressed, highlighting the physiological impact of maternal depression on infant autonomic functioning. Building on these results, Amani and colleagues (Reference Amani, Krzeczkowski, Savoy, Schmidt and Van Lieshout2023) observed that treating PPD with group CBT leads to improvements in infant HF-HRV that were greater than the infants of birthing parents with PPD who had not received treatment. In the present study, we replicated these findings by showing that maternal PPD treatment with CBT is associated with improvements in infant HF-HRV up to three months post-treatment, evidence of treatment’s potential adaptive influence on infants’ physiological outcomes.
Our findings also suggest that these treatment-related benefits were not uniform across all infant traits. Indeed, fear’s association with HF-HRV stood out relative to the other 13 IBQ-R SF subdomains; fear was the only subdomain to moderate HF-HRV change over time in repeated measures analyses and one of just a few to show significant associations in regression analyses. Specifically, we found that temperamental fearfulness moderated the degree of physiological improvement, such that infants with more fear who had been born to depressed birthing parents (but not healthy control infants) showed smaller increases in HF-HRV following maternal CBT.This, along with the lack of correlation between infant fearfulness and maternal depression before treatment suggests that more fearful infants might align with what frameworks like differential susceptibility describe as “fixed individuals” (Pluess & Belsky, Reference Pluess and Belsky2011). That is, they may be less influenced by environmental changes, whether adverse (maternal PPD) or positive (improved maternal mood post-treatment).
Behavioral dynamics between birthing parents and fearful infants could contribute to why these infants appear less affected by improvements in their rearing environment indexed by decreased maternal depressive symptoms. Infants higher in fearfulness exhibit more reactive and aversive behaviors, while those lower in fearfulness tend to be calmer (Rothbart, Reference Rothbart1981). Moreover, prior research has shown that infant fear may negatively influence how bonded birthing parents feel to their infants (Nolvi et al., Reference Nolvi, Karlsson, Bridgett, Pajulo, Tolvanen and Karlsson2016; Roubinov et al., Reference Roubinov, Epel, Adler, Laraia and Bush2022; Takács et al., Reference Takács, Smolík, Kaźmierczak and Putnam2020), potentially reducing the frequency or quality of parent-infant interactions. While we did not observe a significant association between infant fearfulness and maternal-reported bonding in our sample, we relied on self-report measures that may be less sensitive to subtle or behaviorally based disruptions in the parent-infant relationship. Thus, the possibility remains that reduced co-regulatory engagement, particularly in dyads with more temperamentally fearful infants, may limit infants’ ability to fully benefit from the positive effects of CBT, including improvements in maternal mood. Future work using observational methods may help clarify this potential mechanism.
Alternatively, there may be unobservable inherent factors in fearful infants that make them less responsive to the benefits of maternal PPD treatment. From an evolutionary perspective, ancestral parents, like today’s parents, could not predict which rearing methods would best ensure their children’s survival. Therefore, to maximize survival chances, evolution could have led parents to have children with different levels of adaptability to environmental change. If certain parenting methods were then unsuccessful, less malleable or “fixed” children would not suffer as much, preserving their ability to pass on their genes (Boyce & Ellis, Reference Boyce and Ellis2005). Indeed, infants with parents who are more responsive to their needs have smaller amygdala volumes (Rifkin-Graboi et al., Reference Rifkin-Graboi, Kong, Sim, Sanmugam, Broekman, Chen, Wong, Kwek, Saw, Chong, Gluckman, Fortier, Pederson, Meaney and Qiu2015)and reduced attentional avoidance toward fear-inducing threats (Thrasher et al., Reference Thrasher, Krol and Grossmann2021). This aligns with the idea that supportive caregivers help infants “outsource” their emotion regulation, while infants with less responsive parenting (as in cases of PPD), may become more self-reliant for emotional regulation (Coan & Sbarra, Reference Coan and Sbarra2015; Porges & Furman, Reference Porges and Furman2011; Tottenham, Reference Tottenham2020). Indeed, offspring exposed to higher prenatal depressive symptoms (Qiu et al., Reference Qiu, Anh, Li, Chen, Rifkin-Graboi, Broekman, Kwek, Saw, Chong, Gluckman, Fortier and Meaney2015)or less responsive parents (Thijssen et al., Reference Thijssen, Muetzel, Bakermans-Kranenburg, Jaddoe, Tiemeier, Verhulst, White and Van Ijzendoorn2017)often show accelerated development or stronger connectivity in fear-related brain circuits, like the amygdala-prefrontal cortex pathway (Tottenham, Reference Tottenham2020).These infants’ brain circuitry may have equipped them to depend less on caregivers for emotion regulation, potentially making them less likely to benefit from their parents’ improved mood and increased responsiveness after CBT treatment.
While our findings suggest that in the context of maternal PPD, higher infant fear was associated with reduced physiological improvement following maternal treatment, we caution against interpreting temperamental fear as universally maladaptive or that this trait is fixed in infants. In our high-risk, treatment-seeking sample where infant fearfulness did not correlate with baseline maternal depression but did predict reduced physiological gains post-treatment, fear may have reflected an adaptive form of environmental vigilance. However, other studies suggest that fear can signal increased plasticity and cognitive benefit in supportive conditions (Graham et al., Reference Graham, Buss, Rasmussen, Rudolph, Demeter, Gilmore, Styner, Entringer, Wadhwa and Fair2016), in alignment with the differential susceptibility model (Belsky & Pluess, Reference Belsky and Pluess2009). Thus, the pattern we observed may reflect a context-specific expression of fear as a short-term protective strategy rather than a globally stable trait. Future research should examine whether fear operates differently in lower-risk or more stable caregiving environments.
Prior studies in depressed birthing parents (Dawson et al., Reference Dawson, Frey, Self, Panagiotides, Hessl, Yamada and Rinaldi1999; Diego et al., Reference Diego, Field, Jones, Hernandez-Reif, Cullen, Schanberg and Kuhn2004, Reference Diego, Field, Jones and Hernandez-Reif2006)reported greater right frontal alpha activity on EEG in their infants, suggestive of altered brain symmetry linked to maternal depression. Building on this, Amani et al., (Reference Amani, Krzeczkowski, Savoy, Schmidt and Van Lieshout2023) showed that maternal PPD treatment can shift brain asymmetry toward greater left frontal alpha activity. In the present study we also found a left-shift FAA in the infants of depressed birthing parents after treatment. However, we found that temperamental fear as an infant trait did not correlate with infant FAA outcomes. Frontal cortical functioning indexed using FAA, relies on coordinated brain activity from multiple regions(Davidson, Reference Davidson2004; Thayer & Lane, Reference Thayer and Lane2000), with limited top-down modulation of subcortical regions during the early stages of life (Gao et al., Reference Gao, Alcauter, Elton, Hernandez-Castillo, Smith, Ramirez and Lin2015; Price et al., Reference Price, Kennedy, Dehay, Zhou, Mercier, Jossin, Goffinet, Tissir, Blakey and Molnár2006). Thus, the association between the FAA and regulation of fear might take longer to become evident (Tottenham, Reference Tottenham2020). This contrasts with brain systems underlying HRV which rapidly develop starting in the third trimester to help infants regulate bodily functions (Porges & Furman, Reference Porges and Furman2011). Moreover, our small sample size might have contributed to us not finding an association. Additionally, collecting FAA while infants were at rest might have introduced variance for each subject (Coan et al., Reference Coan, Allen and McKnight2006; Stewart et al., Reference Stewart, Coan, Towers and Allen2014), and so further investigation into task-related FAA, which better eliminates subject variance, with larger sample sizes could provide additional insights into the effects of infants’ fear on FAA.
This study also contains limitations that require acknowledgement. We relied on parental reports to assess maternal psychiatric symptoms and infant temperament. While these measures are widely used and often align with clinical interviews and lab assessments (Goldsmith & Rothbart, Reference Goldsmith and Rothbart1991; Kochanska et al., Reference Kochanska, Murray and Coy1997), they rely on maternal recall and may be prone to bias. For instance, parent perceptions of infant temperament, though arguably more relevant to understanding mother-infant dynamics, can still be influenced by subjective factors (Rothbart & Bates, Reference Rothbart and Bates1998; Rothbart & Goldsmith, Reference Rothbart and Goldsmith1985). Future research should consider adding laboratory-based assessments to complement parent-reported data. Additionally, the birthing parents in this study were primarily White, socioeconomically comfortable, and married, and lived in Canada with access to universal healthcare. The case dyads also consisted of birthing parents diagnosed with MDD and treated in a specialty mental health clinic, and so had syndrome-level MDD and were treatment-seeking. As a result, the results of this work may not be generalizable to all birthing parents with PPD. Also, HRV data were processed by a single rater without formal assessment of interrater reliability; future work would benefit from double-processing to strengthen the robustness of peak detection and artifact rejection. Greater HF-HRV in infancy appears to reflect an elevated potential for the infant to alter psychophysiology resources in the context of stress/demands. However, whether/how this potential consistently gives rise to regulation of emotions (adaptive) or potentially elevated emotional reactivity to stressors (maladaptive) is unclear. Indeed, this process likely depends on a hoist of additional neurophysiological factors and the environmental context. Future studies should investigate HF-HRV at rest and in response to a range of ER challenges both in infancy and longitudinally. Moreover, our study employed an observational design, hindering our ability to establish causality between the investigated variables. As a result, the observed changes could be due to CBT or other elements, including the passage of time, or be contributed to by medication effects (our sample did include individuals taking antidepressants). Finally, this study was not pre-registered, as it was designed as an exploratory investigation of infant neurophysiological outcomes in a context where no prior data existed to our knowledge. As the field advances, future work should incorporate a priori sample size determinations alongside pre-registration of analytic strategies and hypotheses to support transparency.
Nevertheless, this study contributes novel evidence regarding the role of infant fear in influencing their outcomes following maternal PPD treatment. The fact that fear stood out compared to other temperament traits across both analytic approaches and showed associations specific to HF-HRV but not FAA, supports its potential distinct role in moderating infant physiological outcomes following maternal PPD treatment. This convergence increases our confidence that we may be identifying a meaningful, trait-based moderator of infants’ responses to changes in the caregiving environment, warranting further investigation in larger and more diverse samples in more robust study designs (including randomized control trials). While our findings suggest that highly fearful infants maybe less likely to respond to maternal PPD treatment up to three months post-treatment, it is possible that their brains may need more time to adapt to the modified caregiving environment. Moreover, while no studies to date have examined the impact of specific elements of psychotherapy on infant emotion regulation and/or directly compared the effectiveness of psychotherapy for birthing parents alone to mother-infant psychotherapies, such work in the future could help us better understand how to optimize outcomes for offspring in addition to birthing parents. Future research should also employ high spatial resolution methods, such as Functional Magnetic Resonance Imaging (fMRI) or Functional Near-Infrared Spectroscopy (fNIRS) imaging, to investigate connectivity and its correlation with the regulation of fear in relation to parameters like HF-HRV in combination with other cardiac indices for a more comprehensive assessment of the nervous system’s contribution to cardiovascular autonomic balance.
Conclusion
In this study, infant fear, a developmentally important trait, appeared to influence infants’ response to birthing parent PPD treatment. While infants may experience physiological improvement from their parent’s participation in CBT, fearful infants may benefit less. By identifying infant fearfulness as a factor that may limit the impact of PPD treatment, this study highlights the need to integrate infant-focused approaches into existing interventions. For example, incorporating strategies that address infant temperament, such as parent-infant interaction training (Horowitz et al., Reference Horowitz, Posmontier, Chiarello and Geller2019), could enhance outcomes for both birthing parents and their infants. Future research should further explore how specific infant traits interact with PPD interventions to refine and optimize treatment protocols, ensuring that interventions support diverse parent-infant dyads in achieving the best possible developmental trajectories.
Supplementary material
The supplementary material for this article can be found at https://doi.org/10.1017/S0954579425100527.
Data availability statement
This research was not preregistered. We note that the data and materials from this study are not publicly available due to the terms outlined in the participant consent form approved by the Hamilton Integrated Research Ethics Board (HiREB; study number 0912). Specifically, the form states: “This information will be kept in a locked office on University property and will only be available to research team members.” In accordance with this protocol, the dataset is not shared publicly.
Acknowledgments
We thank all participants for their contributions to this study.
Funding statement
This work was supported by Funding-Brain and Behavior Research Foundation: Grant #23595. KYK was funded by the CIHR’s Canada Graduate Scholarship. JEK was funded by the Government of Canada’s Vanier Graduate Program.
Competing interests
The authors declare none.