1. Background
The vast majority (96%) of patients with a first-time schizophrenia diagnosis had previously been diagnosed with somatic diseases and a broad range of somatic diseases are associated with an increased risk of schizophrenia [Reference Sorensen, Nielsen, Benros, Pedersen and Mortensen1]. Particularly epilepsy [Reference Sorensen, Nielsen, Benros, Pedersen and Mortensen1], brain injury [Reference Sorensen, Nielsen, Benros, Pedersen and Mortensen1, Reference Orlovska, Pedersen, Benros, Mortensen, Agerbo and Nordentoft2], infections [Reference Benros, Nielsen, Nordentoft, Eaton, Dalton and Mortensen3–Reference Köhler, Petersen, Mors, Mortensen, Yolken and Gasse6] autoimmune diseases [Reference Benros, Nielsen, Nordentoft, Eaton, Dalton and Mortensen3], and asthma [Reference Pedersen, Benros, Agerbo, Borglum and Mortensen7] have been associated with increased risk of schizophrenia.
However, it is important to extend these findings beyond an etiological perspective and investigate whether somatic conditions affect the early clinical course and readmission risk after a schizophrenia diagnosis. Only a few smaller clinical studies among patients with mental disorders have indicated that somatic conditions may result in a longer duration of illness and an increased readmission risk [Reference Manu, Khan, Radhakrishnan, Russ, Kane and Correll8, Reference Sylvia, Shelton, Kemp, Bernstein, Friedman and Brody9], thus indicating that somatic diseases may affect the clinical course of the mental disorder. Nevertheless, these studies were limited by small study populations and by not including schizophrenia specifically or specific somatic diseases nor the timing of the somatic diseases, i.e. whether the somatic diseases occurred before or after the mental disorder diagnosis. Furthermore, it is important to investigate the early clinical course among patients with a first-time schizophrenia diagnosis since this time-frame has been emphasized as highly important for long-term treatment outcomes [Reference Laursen, Munk-Olsen, Agerbo, Gasse and Mortensen10, Reference Nordentoft, Wahlbeck, Hällgren, Westman, Osby and Alinaghizadeh11].
Hence, we hypothesized that somatic diseases diagnosed prior to the incident schizophrenia diagnosis would be associated with an increased risk for schizophrenia relapse during the first five years after the first-time diagnosis. Our associated hypothesis was that the specific somatic diseases that have been associated with subsequent development of schizophrenia as described above1−7 also would be associated with an increased risk for schizophrenia re-hospitalizations.
2. Methods
The present study is a register-based cohort study based on the Danish nationwide registers [Reference Mors, Perto and Mortensen12–Reference Jensen and Rasmussen16]. The unique personal identification number enables individual linkage between all registers. This study has been approved by the Danish Data Protection Agency, the Danish National Board of Health and Statistics Denmark (Danish Data Protection Agency: Journal number: 2015-57-0002 / Journal number: 62908 (Joint Registration for Aarhus University); National Board of Health registration number: FSEID 00000098).
2.1. Study population
The Danish Psychiatric Central Research Register has covered all mental disorders diagnosed within the secondary healthcare system since 1969 [Reference Mors, Perto and Mortensen12] and the Danish National Patient Registry has covered all somatic diseases diagnosed in the secondary healthcare system since 1977 [Reference Lynge, Sandegaard and Rebolj13]. Both registers have included all outpatient contacts for mental disorders and somatic diseases, respectively, since 1995. We conducted a nationwide cohort study covering all individuals born in Denmark after January 1st, 1977 [Reference Pedersen14] to be able to assess life-time somatic diseases and mental disorders. We identified individuals with a first-time schizophrenia diagnosis (International Classification of Diseases, 8th edition (ICD-8): 295. × 9 excluding 295.79; ICD-10: F20.X) between January, 1st 1996 and December 31st, 2015 during admission or an outpatient setting (age≥10 years) [Reference Mors, Perto and Mortensen12]. A total of 12 individuals were excluded due to a diagnosis before the age of 10. We included only individuals diagnosed with a first-time schizophrenia diagnosis after January 1st, 1996, since the Danish National Prescription Registry [Reference Kildemoes, Sorensen and Hallas15] contains nationwide information on all redeemed prescriptions after January 1st, 1995, allowing inclusion of previous somatic medication use and adjustment for previous psychotropic drug use. The validity of the schizophrenia diagnosis in the registers is high with 97.5% of patients with a registered schizophrenia diagnosis fulfilling ICD-10 criteria [Reference Uggerby, Ostergaard, Roge, Correll and Nielsen17].
2.2. Follow-up
The index date was the day of first schizophrenia diagnosis. Among patients diagnosed during an admission, this was the discharge date, and among outpatients this was the day of initiation of the outpatient contact. We followed all individuals from the index date for a maximum of five years until first outcome (see below), death, emigration, or end of the study period on April 10th, 2017.
2.3. Outcome – schizophrenia relapse
We identified the first inpatient hospitalization with schizophrenia (ICD-10: F20.X) between January 15th, 1996 and April 10th, 2017 during the first five years after the incident schizophrenia diagnosis via the Danish Psychiatric Central Research Register [Reference Mors, Perto and Mortensen12]. Hospitalizations for schizophrenia have been evaluated as an adequate proxy for relapse in schizophrenia [Reference Olivares, Sermon, Hemels and Schreiner18]. The hospitalization had to occur at least 14 days after the first-time schizophrenia diagnosis. Thereby, we avoided hospitalizations shortly after or in connection with initiation of an outpatient contact, and discharges lasting only few days.
2.4. Exposure – somatic diseases
To cover all treated somatic diseases, we identified 1) any life-time somatic disease diagnosed in a hospital setting before the first-time schizophrenia diagnosis and 2) any somatic medication use during the year before the first-time schizophrenia diagnosis.
Via the Danish National Patient Registry [Reference Lynge, Sandegaard and Rebolj13], we identified all somatic hospital contacts since birth and prior to first-time schizophrenia diagnosis (ICD-codes supplied in Supplementary Table 1). We included the main diagnoses from hospitalizations, outpatient contacts and emergency room contacts. In addition to the main ICD-categories, we were interested in specific disease entities, which have been associated with an increased risk of subsequent schizophrenia diagnosis: Epilepsy [Reference Sorensen, Nielsen, Benros, Pedersen and Mortensen1], brain injury [Reference Orlovska, Pedersen, Benros, Mortensen, Agerbo and Nordentoft2], autoimmune diseases [Reference Benros, Nielsen, Nordentoft, Eaton, Dalton and Mortensen3], and asthma including other atopic diseases [Reference Pedersen, Benros, Agerbo, Borglum and Mortensen7] (Supplementary Table 1). To evaluate the influence of chronic diseases, we identified diagnoses included in the Charlson comorbidity score [Reference Charlson, Pompei, Ales and MacKenzie19], covering 19 severe chronic conditions (myocardial infarct, congestive heart failure, peripheral vascular disease, cerebrovascular disease, dementia, chronic pulmonary disease, connective tissue disease, ulcer disease, mild liver disease, diabetes, hemiplegia, moderate to severe renal disease, diabetes with end organ damage, any tumor, leukemia, lymphoma, moderate to severe liver disease, metastatic solid tumor, AIDS). These diagnoses were identified from main diagnoses at in- or outpatient contacts to somatic hospitals only. The Charlson score has been validated [Reference Thygesen, Christiansen, Christensen, Lash and Sorensen20] and modified for use with the ICD-10 [Reference Nuttall, van der Meulen and Emberton21].
We excluded individuals who had only received the following diagnostic codes: Symptoms, signs and abnormal clinical and laboratory findings, not elsewhere classified (ICD-8: 780, 782.3, 782.5-791, 793-796; ICD-10: R00-R99), and factors influencing health status and contact with health services (ICD-10: Z00-Z99).
In addition to hospital contacts and as a proxy for contacts with the general practitioner, we used the Danish National Prescription Registry [Reference Kildemoes, Sorensen and Hallas15] to identify all redeemed prescriptions for somatic medications (i.e., except for psychotropic drugs defined as Anatomical Therapeutic Chemical (ATC) codes: N03-N07) within the year before the first-time schizophrenia diagnosis, as prescriptions indicate somatic diseases treated in the primary sector (ATC-codes supplied in Supplementary Table 2). We calculated the amount of prescriptions from different ATC groups.
2.5. Assessment of covariates
We assessed sociodemographic covariates at the date of first-time schizophrenia diagnosis: age, sex [Reference Pedersen14], and educational level (divided into primary school and higher education) [Reference Jensen and Rasmussen16]. Regarding the severity of schizophrenia, we identified whether individuals were in- or outpatients at first-time schizophrenia diagnosis including the length of hospitalization. In addition, the following psychiatric diagnoses prior to incident schizophrenia diagnosis were identified [Reference Mors, Perto and Mortensen12]: Disorders due to use of alcohol or other psychoactive substances, bipolar disorder, depression, and anxiety disorders (codes supplied in Supplementary Table 3). Via the Danish National Prescription Registry [Reference Kildemoes, Sorensen and Hallas15], we included information on any use of psychotropic medication (ATC-code: N03-N07) and specifically use of antipsychotics (N05A), anxiolytics (N05B), hypnotics (N05C) and antidepressants (N06A) within the year prior to first-time schizophrenia diagnosis, since prior treatment may influence both treatment course and the risk of somatic diseases by induction of metabolic disturbances. Furthermore, we identified information on any parental psychiatric diagnosis since 1969 (ICD-8: 290-315; ICD-10: F00-99) [Reference Mors, Perto and Mortensen12] and the highest educational level achieved by the parents16 at the time of first-time schizophrenia diagnosis.
2.6. Statistical analyses
First, to evaluate differences in baseline characteristics between people with and without previous somatic hospital contacts and somatic medication use, we performed logistic regression analyses and report odds ratios (OR) including 95%-confidence intervals (95%-CI). In addition, we calculated the annual prevalence of individuals with a somatic hospital contact during the 10 years prior to the first-time schizophrenia diagnosis.
Second, concerning the association between previous somatic hospital contacts or somatic medication use and hospitalizations with schizophrenia during the subsequent five years, we performed Cox regression analyses and report hazard rate ratios (HRR) and 95%-CI. We studied the association between 1) any life-time somatic hospital contact and 2) any somatic medication use during the year before the first-time schizophrenia diagnosis with the risk of subsequent re-hospitalization with schizophrenia during the first five years after the first-time schizophrenia diagnosis. Furthermore, we performed analyses that included the different categories of somatic hospital contacts and specific somatic disease categories. The latter analyses were adjusted for multiple testing by dividing the p-value of 0.05 with the number of tests performed.
The adjusted analyses were adjusted for age, gender, and year of diagnosis. The fully adjusted analyses were adjusted for age, gender, year of diagnosis, in- or outpatient status at first-time schizophrenia diagnosis, length of index hospitalization, psychiatric diagnoses prior to first-time schizophrenia diagnosis, highest educational level, use of psychotropics within the year prior to first-time diagnosis, parental psychiatric diagnoses and highest parental educational level. All analyses were mutually adjusted, i.e. analyses on somatic hospital contacts were adjusted for previous somatic medication use and vice versa.
Furthermore, we investigated the amount of different prior somatic diseases, which included analyses on the amount of somatic hospital contacts with different somatic diseases and the amount of different somatic medication groups. In addition, since some somatic diseases may have occurred several years before the first schizophrenia diagnosis, and thus not may be relevant for the course of the schizophrenia disorder, we investigated the association between the time since the last somatic hospital contact prior to first-time schizophrenia diagnosis. To investigate on possible linear relationships, we performed Wald´s test and report p-values.
2.7. Post-hoc analysis
First, having observed that somatic hospital contacts during the year before the first-time schizophrenia diagnosis were associated with a significantly increased risk of subsequent hospitalization with schizophrenia, we performed multiplicative interaction analyses between somatic hospital contacts during the year before the first-time schizophrenia diagnosis and somatic medication use during the year before the first-time schizophrenia diagnosis. Second, we analyzed the association between the amount of different somatic hospital contacts during the year before the first-time schizophrenia diagnosis and risk of schizophrenia re-hospitalization. Third, since we found large gender differences regarding baseline characteristics (Table 1), we performed gender interaction analyses.
3. Results
Among 11,856 individuals diagnosed with schizophrenia between 1996 and 2015 (follow-up of 39,033.3 person-years), a total of 11,312 (95.4%) had been hospitalized in a somatic hospital prior to first-time schizophrenia diagnosis and 7243 (61.1%) had redeemed at least one prescription for somatic medications during the previous year. We identified the following baseline characteristics to be associated with somatic hospital contacts prior to first-time schizophrenia diagnosis (Table 1): a later index year, a prior diagnosis with substance abuse, and a maternal mental disorder (all p < 0.05). Somatic medication use during the previous year was associated with female gender, a later index year, and previous psychotropic drug use (all p < 0.05). Fig. 1 shows an increase of individuals with a contact to a somatic hospital during the 10 years prior to the first-time schizophrenia diagnosis.
3.1. Prior somatic hospital contacts and risk of relapse
Among the 11,856 individuals diagnosed with schizophrenia, 5506 (46.4%) were re-hospitalized with schizophrenia during the first five years of follow-up. The occurrence of any somatic hospital contact at any time prior to first-time schizophrenia diagnosis was associated with an increased risk of hospitalization with schizophrenia by a HRR of 1.30 (95%-CI = 1.07; 1.59) during the first five years (Table 2).
Several specific somatic diseases and diagnostic categories were associated with an increased risk for re-hospitalization with schizophrenia, which remained significant after adjustment for multiple testing (Table 2). Concerning chronic diseases, individuals with diagnoses included in the Charlson comorbidity score were associated with an increased risk for re-hospitalization with schizophrenia. However, we found no association between a Charlson comorbidity score of three or more and re-hospitalization (HR = 0.79; 95%-CI = 0.54–1.15).
Table 3 shows a relationship (p < 0.005) between the number of somatic hospital contacts prior to first-time schizophrenia diagnosis and the risk for hospitalization with schizophrenia, with 6 or more prior somatic hospital contacts increasing the risk of hospitalization with schizophrenia by a HR of 1.61 (95%-CI = 1.29; 2.00).
When studying the temporal associations (Table 3), we found that it was only somatic hospital contacts within the year prior to the first-time schizophrenia diagnosis that were associated with an increased HRR of 1.36 (95%-CI = 1.11; 1.66) for re-hospitalization with schizophrenia during the subsequent five years.
3.2. Prior somatic medication use and risk of relapse
When investigating individuals who had redeemed a prescription for any somatic medication during the year prior to first-time schizophrenia diagnosis we observed an inverse relationship, where redeemed prescriptions for any somatic medication during the year prior to first-time schizophrenia diagnosis were associated with a non-significantly slightly decreased risk for 5-year-(re) hospitalization with schizophrenia (HRR of 0.96; 95%-CI = 0.90; 1.02) (Table 2). The risk estimates were significantly decreased among individuals who redeemed two or four different prescriptions (Fig. 2 & Supplementary Table 4).
3.3. Post-hoc analysis
First, interaction analyses between somatic hospital contacts and somatic medication use within the year before the first-time schizophrenia diagnosis showed no significant interaction (p = 0.39). Second, we found that a larger amount of somatic hospital contacts during the year prior to first-time schizophrenia diagnosis was associated with increased 5-year-risks for hospitalization with schizophrenia (p < 0.005) (Fig. 2 & Supplementary Table 4), with 6 or more prior somatic hospital contacts during the year prior increasing the risk by a HRR of 1.66 (95%-CI = 1.50; 1.84). Third, gender interaction analyses did not show a significant interaction in the analyses on previous somatic hospital contacts (p = 0.16) nor previous somatic medication use (p = 0.06).
Baseline characteristics at the time of incident schizophrenia diagnosis among 11,856 patients diagnosed during 1996 and 2015 depending on life-time somatic hospital contacts and somatic medication use during the year before the schizophrenia diagnosis.

Abbreviations: OR=Odds Ratio; 95%-CI=95%-Confidence Interval. Bold values represent significant results.
a The ORs are based on logistic regression analyses and all results are adjusted for all covariates mentioned in Table 1.
b Within the year prior to first schizophrenia diagnosis.
Annual prevalence of individuals with a contact to a somatic hospital during the 10 years prior to first-time schizophrenia diagnosis among 11,856 patients.

The association between somatic hospital contacts and somatic medication use prior to first-time schizophrenia diagnosis and hospitalizations with schizophrenia among 11,856 incident patients with schizophrenia.
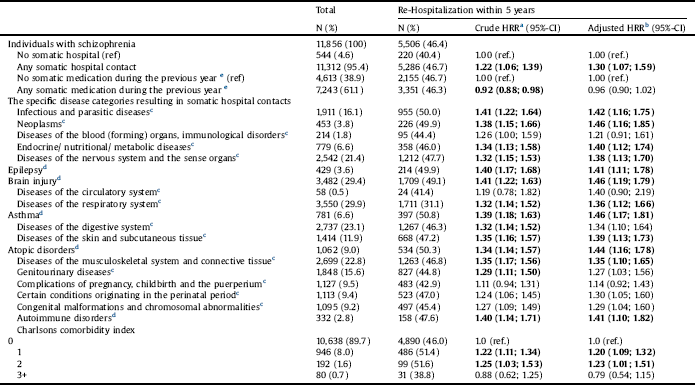
Abbreviations: HRR=Hazard rate ratio; 95%-CI = 95% Confidence Interval; Bold numbers represent significant results even after adjustment for multiple testing.
a The crude analyses are adjusted for age at diagnosis, gender and indexyear.
b The adjusted analyses are adjusted for age at diagnosis, gender, indexyear, in- or outpatient status at incident schizophrenia diagnosis, length of baseline hospitalization, educational level, prior psychiatric diagnoses and use of antipsychotics, parental psychiatric diagnoses and parental educational level. Furthermore, the analyses on somatic hospital contacts were adjusted for somatic medication use during the previous year and vice versa.
c The overall ICD classes were adjusted for multiple testing, i.e. p = 0.05/15 = 0.003.
d The specific diseases were ajusted for multiple testing, i.e. p = 0.05/6 = 0.008.
e Refers to any redeemed medications during the year prior to the first-time schizophrenia diagnosis.
Risk of hospitalization with schizophrenia (i.e. relapse) during the first five years after incident schizophrenia diagnosis depending on the number of different somatic hospital contacts and the time since the last somatic hospital contact.
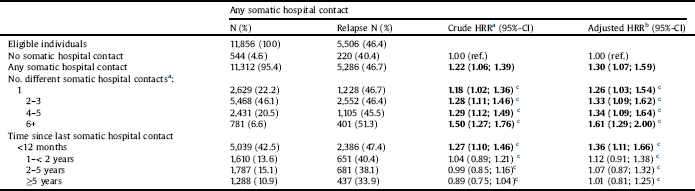
Abbreviations: HRR=Hazard rate ratio; 95%-CI = 95% Confidence Interval; Bold values represent significant results.
a The crude analyses are adjusted for age at diagnosis, gender and indexyear.
b The adjusted analyses are adjusted for age at diagnosis, gender, indexyear, in- or outpatient status at incident schizophrenia diagnosis, length of baseline hospitalization, educational level, prior psychiatric diagnoses and use of antipsychotics, parental psychiatric diagnoses and parental educational level, and any somatic medication use during the previous year.
c The risk of relapse increased with a larger number of somatic hospital contacts (p < 0.005), as tested with the Wald´s test.
Risk and 95% confidence intervals of hospitalization with schizophrenia (i.e. relapse) during the first five years after incident schizophrenia diagnosis depending on the number of different somatic hospital contacts (blue bars) and redeemed somatic medications (red bars) during the year before the incident schizophrenia diagnosis.

4. Discussion
This nationwide study represents the largest investigation of the association between the entire range of somatic diseases prior to first-time schizophrenia diagnosis and the risk of schizophrenia relapse during the first five years. We included 11,856 patients born after 1977 with a first-time schizophrenia diagnosis between 1996 and 2015 and followed the cohort for 39,033 person-years. Somatic hospital contacts within the year prior to the first-time schizophrenia diagnosis were associated with a 36% increased risk of schizophrenia relapse, with the risk increasing with the number of somatic diseases. Hence, our findings indicate that severe somatic diseases within the year prior to the first-time schizophrenia diagnosis may negatively affect early schizophrenia treatment course, and that treatment of the somatic disease (as indicated by redeemed prescriptions) may improve treatment course. The latter may also indicate better compliance and help-seeking behavior. We did not find any specific somatic disease(s) to be associated with greater relapse risk and hence no evidence to support that inflammatory diseases were associated with a greater relapse risk.
4.1. Association between somatic diseases and the early treatment course of schizophrenia
First, our finding that somatic diseases leading to hospital contacts increased schizophrenia relapse risks indicate that severe somatic diseases negatively affect the early treatment course of schizophrenia. To date, a number of studies have focused on the association between somatic diseases and subsequent development of schizophrenia [Reference Sorensen, Nielsen, Benros, Pedersen and Mortensen1, Reference Benros, Nielsen, Nordentoft, Eaton, Dalton and Mortensen3, Reference Nielsen, Benros and Mortensen4] respectively the higher mortality risk among patients with schizophrenia [Reference Laursen, Munk-Olsen, Agerbo, Gasse and Mortensen10, Reference Nordentoft, Wahlbeck, Hällgren, Westman, Osby and Alinaghizadeh11]. Epidemiologic evidence suggests that somatic diseases occur more frequently among patients with schizophrenia compared to non-psychiatric patients [Reference Sorensen, Nielsen, Benros, Pedersen and Mortensen1] and that somatic comorbidity is attributable for more than half of the reduced expected life expectancy [Reference Laursen, Munk-Olsen, Agerbo, Gasse and Mortensen10]. Despite these important associations, to date, only two clinical studies associated higher BMI with an increased readmission risk among 224 psychiatric patients [Reference Manu, Khan, Radhakrishnan, Russ, Kane and Correll8] respectively somatic conditions with more time spent depressed and longer duration of illness among 482 patients with bipolar disorder [Reference Sylvia, Shelton, Kemp, Bernstein, Friedman and Brody9]. An observational study found an association between chronic somatic diseases and an increased 30-day re-hospitalization risk among 3563 patients with schizophrenia [Reference Boaz, Becker, Andel, Van Dorn, Choi and Sikirica22]. One register-based study has shown that prescriptions for non-steroidal anti-inflammatory drugs (NSAIDs) during the early schizophrenia treatment course, indicating the presence of painful somatic conditions, were associated with increased schizophrenia relapse risks [Reference Kohler, Petersen, Benros, Mors and Gasse23]. Finally, another register-based study found that patients with higher inflammatory markers had a higher mortality rate, but that the risk for relapse was not affected [Reference Horsdal, Köhler-Forsberg, Benros and Gasse24]. However, despite studies indicating that somatic diseases among patients with schizophrenia may be undertreated [Reference Laursen, Munk-Olsen and Gasse25], the present study is the first to investigate the overall impact of life-time somatic diseases on treatment course, indicating that previous somatic comorbidity indeed may affect the early schizophrenia treatment course.
Our findings that somatic diseases in schizophrenia predict increased risks of schizophrenia relapse could point to several underlying explanations. First, it is possible that serious co-morbid somatic diseases add complexity to the psychopharmacological treatment. Secondly, the threshold to become readmitted with schizophrenia could be influenced by having a potentially life threatening co-morbid disease. Third, a patient’s compliance with respect to antipsychotic medication could be influenced by the number of co-morbid somatic diseases. Fourth, having a severe somatic disease could also cause somatic anxiety which could affect the psychological well-being as well as help-seeking behavior.
Secondly, we found no associations between redeemed prescriptions for somatic medications and an increased risk for schizophrenia re-hospitalization. Rather, our findings indicate a trend that individuals who had redeemed prescriptions for somatic medications during the year before the first-time schizophrenia diagnosis had a slightly reduced risk for relapse. This indicates that treatment of a somatic disease may improve the treatment course of the mental disorder, in this case schizophrenia. These findings may also indicate that the patients had more help-seeking behavior and better compliance as they were able to see their general practitioner and redeem prescriptions at the pharmacy. Nonetheless, it has been shown in previous studies that sufficient treatment of somatic diseases can significantly reduce the mortality risk [Reference Kugathasan, Horsdal, Aagaard, Jensen, Laursen and Nielsen26, Reference Laursen, Mortensen, MacCabe, Cohen and Gasse27]. Taken together, these results emphasize that diagnosing and treating somatic diseases among individuals with schizophrenia seem to improve the life and the early clinical course of these individuals.
4.2. Strengths and limitations
The strengths of the present study are the nationwide setting and the well-validated Danish registers [12–Reference Jensen and Rasmussen16]. Importantly, the validity of the schizophrenia diagnoses in the registers is high [Reference Uggerby, Ostergaard, Roge, Correll and Nielsen17]. In addition, for the present study, we only included individuals with life-long information on all contacts to somatic and psychiatric hospital settings, yielding life-long information for both exposure and outcomes. Finally, the prescription register gives nationwide information on all redeemed prescriptions.
Limitations include that we had a relatively young study population aged up to a maximum of 39 years to capture life time disease burden. Second, we had no information on whether individuals visited their general practitioner without redeeming prescriptions. It has been shown that general practitioner visits increase prior to the first schizophrenia diagnosis [Reference Nørgaard, Søndergaard Pedersen, Fenger-Grøn, Mors, Nordentoft and Vestergaard28]. Third, we had only information whether patients redeemed prescriptions but no information on actual compliance, both regarding somatic and psychotropic medication. Fourth, we had no information on the severity of the somatic disease nor the schizophrenia disorder.
4.3. Conclusion
The present study found that severe somatic diseases may increase the risk for schizophrenia relapse among patients with a first-time schizophrenia diagnosis, whereas patients who redeemed prescriptions for somatic diseases showed a trend towards slightly lower relapse risks. These findings emphasize the need for a good and broad assessment of somatic diseases among patients with schizophrenia and relevant treatment hereof, as this also may improve the treatment course of the schizophrenia disorder.
Appendix A. Supplementary data
Supplementary material related to this article can be found, in the online version, at doi:https://doi.org/10.1016/j.eurpsy.2019.03.006.







Comments
No Comments have been published for this article.