Intrathecal morphine (ITM) has been adopted as an adjunct to traditional postoperative analgesia in the fields of obstetric, cardiac, urologic, and orthopedic surgery.Reference Abboud, Dror and Mosaad 1 - Reference Kirson, Goldman and Slover 4 Through a single intrathecal injection of morphine, patients benefit from prolonged postoperative analgesia without the need for indwelling catheters or continuous infusions. The resulting improvement in pain management significantly reduces the need for intravenous opioid analgesia, improves time to mobilization, and shortens length of hospital stay.Reference Rathmell, Lair and Nauman 5 - Reference Ziegeler, Bauer, Mencke, Müller, Soltesz and Silomon 7 Although routine use of ITM has long been implemented in many surgical specialties, it has yet to become standard operative care in the setting of lumbar spine surgery despite multiple reports of the safety and efficacy.Reference Ziegeler, Bauer, Mencke, Müller, Soltesz and Silomon 7 - Reference Yorukoglu, Ates, Temiz, Yamali and Kecik 12
Open lumbar spine surgery provides an opportunity for intrathecal injection under direct visualization of the exposed thecal sac before wound closure with technical ease. A theoretical concern of this procedure particularly relevant to spine surgeons is the risk of an iatrogenic cerebrospinal fluid (CSF) leak with dural puncture. Limited exposure of the thecal sac and the depth of the incision often necessitate the administration of ITM through a needle held nearly perpendicular to the dural sac. As a result, punctures through the dura and arachnoid occur along a contiguous plane, potentially creating a channel through which CSF can flow. Iatrogenic CSF leaks following puncture of the dural sac with the needle held perpendicular to the dural surface have been reported.Reference Ziegeler, Fritsch and Bauer 11
Herein we describe a technique for oblique injection into the dural sac that is feasible in cases where dural sac exposure is limited. Oblique injection has the benefit of offsetting punctures in the dura and arachnoid to minimize CSF leak risk. This technique can be performed easily and quickly with standard surgical equipment. Through use of this technique, patients undergoing spine surgery may benefit from ITM while limiting the theoretical risk of iatrogenic CSF leak.
Injection Technique
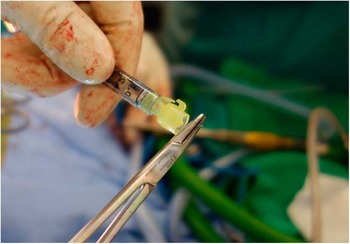
Oblique injection can be accomplished with the use of equipment readily at hand in the operating theatre and without significantly prolonging operative time. A standard 30-gauge needle is used to mitigate trauma to the dural sac while accommodating a 60° bend without compromising the lumen. The bend procedure is performed using a 6-inch Crile Wood Needle Holder. The 30-gauge needle is grasped just distal of the syringe with the needle holder and a moment force is applied toward the direction of the open needle bevel (Figure 1). The needle is bent to a 60° angle (Figure 2).
The needle is prepared for injection by applying a 60° bend towards the open side of the bevel.
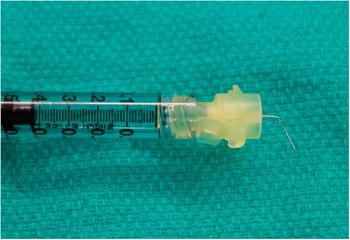
A prepared 30-gauge needle with 60° bend is ready for injection. The lumen is not compromised by the bend procedure.
During injection, the syringe is held perpendicular to the surface of the dural sac. The 60° bend results in the needle approaching the dural surface at a 30° angle. This angle can be reduced or increased as desired to accommodate the depth of the incision or extent of exposure. The needle is passed into the intrathecal space and the injection is performed under direct visualization. The intrathecal injection is performed at the end of the procedure when the dural sac is maximally exposed, and immediately before closure.
Methods
Participating spinal surgeons were provided with brief instructions outlining the injection technique. A total of 0.4 ml of fluid was injected with the oblique intrathecal injection technique during open lumbar spine surgery when the dura was fully exposed before closure. According to the study arm of the randomized controlled trial to which patients were assigned, they were administered either 200 mcg of 500 mcg/ml Epimorph (preservative-free morphine sulphate, total volume 0.4 ml) or 0.4 ml of saline placebo. Assessment of iatrogenic leaks was made through visual inspection of the injection site immediately following injection. Valsalva maneuvers were used only at the discretion of the treating surgeon and were not required by the study protocol. Additionally, patients were monitored postoperatively for signs and symptoms of CSF leak and other complications by a research nurse during a follow-up period lasting the duration of their postoperative stay. Surgical site drains were placed at the discretion of the treating surgeon according to individual practice; they were placed to active suction in the immediate postoperative period in less than one-quarter of patients. Adherence and complications were collected prospectively in the setting of a randomized controlled trial investigating use of ITM.
Results
The oblique injection technique was applied to 104 cases of elective open posterior instrumented fusion between L2 and the sacrum at our institution. Patient, surgical, and follow-up characteristics are shown in Table 1. In two cases (2/104, 1.9%), nonadherence followed preinjection dural tear. In the 102 cases in which oblique injection was performed, there were no instances of postoperative CSF leakage. Three cases (3/102, 2.9%) of transient CSF leakage were observed intraoperatively immediately following intrathecal injection, with no associated sequelae or requirement for postsurgical intervention. In two cases, the observed leak was repaired with fibrin (TISSEEL, Baxter) glue, whereas in a single case the leak was self-limited. There were no cases of postsurgical intervention or complication related to CSF leak during postoperative inpatient follow-up lasting a median of 96 hours with standard deviation of 2 hours.
Patient, surgical, and follow-up characteristics
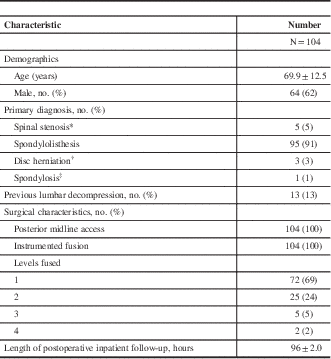
Plus–minus values are medians±standard deviation.
* In the absence of spondylolisthesis.
† In the absence of the spondylolisthesis or spinal stenosis.
‡ In the absence of spondylolisthesis, spinal stenosis, or disc herniation.
Discussion
The potential benefits of offsetting puncture sites in adjacent tissue layers has been established in other medical procedures such as paracentesis, where angular insertion and Z-tract insertion techniques are used to offset epidermal and peritoneal punctures and reduce risk of ascitic fluid leak.Reference Thomsen, Shaffer, White and Setnik 13
An injection angle of 30° relative to the dural surface results in offset between punctures of the dura and arachnoid. Mean lumbar dura thickness ranges from 0.3 to 0.4 mm, whereas arachnoid membrane thickness ranges from 35 to 40 μm.Reference Hong, Suh and Park 14 - Reference Reina, Maches, López and De Andres 16 Injecting through a 0.35-mm thick dura at a 30° angle results in an estimated 0.61 mm offset between entry into the dura and puncture of the arachnoid (Figure 3); this almost entirely eliminates overlap between the dura and arachnoid penetration sites if a 30-gauge needle (0.31 mm outer diameter) is used. Figure 3 illustrates the importance of both needle gauge and injection angle in creating offset between punctures in adjacent layers. Additionally, the oblique needle trajectory is near perpendicular to the expansile CSF pressure within the dural sac, which potentially seals the injection tract.
Injecting at 30° from the dural surface creates nearly complete offset between punctures of the dura and arachnoid. With an estimated dura thickness of 0.35 mm, a 30-gauge needle (0.31 mm outer diameter) creates an initial puncture approximately 0.62 mm wide. The leading lumen wall of the needle travels approximately 0.61 mm horizontally between initial dura penetration and arachnoid penetration. The result is a theoretical overlap of only 10 μm between dura and arachnoid puncture sites. CSF pressure within the dural sac may contribute to sealing the injection lumen.

In our study, this technique was used for open spine surgery only with a traditional posterior midline incision and instrumented fusion. ITM has been used extensively via transcutaneous injection, which approximates oblique injection out of necessity to pass the needle between spinous processes.Reference Abboud, Dror and Mosaad 1 - Reference Kirson, Goldman and Slover 4 This technique could theoretically be applied to minimally invasive surgery with a tubular retractor by using a longer needle with a short distal bent segment; however, we did not specifically assess the applicability or limitations of adapting this technique for minimally invasive surgery.
Although complications with this technique appear to be uncommon, they may be serious and their long-term effects uncertain. The rate of nerve root injury observed in our surgical cases was 3%, which was not meaningfully different from previously published complication rates.Reference Ghogawala, Dziura and Butler 17 , Reference Forsth, Olafsson and Carlsson 18 Neural injury is a theoretical risk of intrathecal injection; however, nerve rootlets and the needle tip can be visualized through the dura. With care, nerve rootlet injury can be avoided; treating surgeons did not observe direct neural injury as a result of intrathecal injection in our study group.
Postoperative meningitis and arachnoiditis were not observed in our study, but are potential complications of any disruption of the meninges. CSF fistula is theoretically potentiated in the setting of CSF leak by use of surgical site drains on active suction. These were placed in less than one-quarter of our patients without observed complication. No dural tears were attributed to intrathecal injection, although this is theoretically possible. It may be reasonable to avoid intrathecal injection in patients with particularly fragile meninges where dural injury may be more likely. Intrathecal catheters for long-term opioid use are associated with formation of granulomas.Reference Kratzsch, Stienen, Reck, Hildebrandt and Hoederath 19 We are not aware of any complications of this nature resulting from a single injection.
Conclusions
Despite demonstrated safety and efficacy of ITM in lumbar spine surgery, the risk of precipitating a CSF leak remains as a barrier to widespread adoption of this analgesic technique.Reference France, Jorgenson, Lowe and Dwyer 8 - Reference Yorukoglu, Ates, Temiz, Yamali and Kecik 12 Introducing a bend to the needle facilitates an oblique approach to intrathecal injection, even in a limited working space. Oblique injection when the dural sac is exposed intraoperatively ensures that punctures of the dura and arachnoid are offset. This theoretically improves puncture sealing and eliminates the direct path for CSF leak that exists when injecting perpendicularly. Oblique intrathecal injection is not associated with increased incidence of postoperative CSF leakage and is therefore a simple and effective way of administering ITM. This technique could be applied to administration of other intrathecal substrates in the future.
Disclosures
The authors do not have anything to disclose.





