Gestational diabetes mellitus (GDM) – defined as hyperglycaemia diagnosed in the second or third trimester of pregnancy that was not clearly overt diabetes prior to gestation(1) – is a common obstetric complication, affecting an estimated 16·5 % of pregnancies worldwide(2). In the majority (about 80 %) of cases, GDM is the result of β-cell dysfunction on a background of chronic insulin resistance, leading to glucose intolerance(Reference Buchanan and Xiang3). Risk factors include a family history of diabetes (either type 1, type 2 or gestational diabetes), advanced maternal age and overweight and obesity(Reference Chu, Callaghan and Kim4–Reference Lao, Ho and Chan6). Although GDM usually resolves following delivery, it is associated with a number of short- and long-term health consequences for both the mother and child. The mother is at increased risk of further pregnancy complications, surgical delivery and of developing future type 2 diabetes and CVD(Reference Damm7). The child is at increased risk of being born large for gestational age, experiencing shoulder dystocia and respiratory distress, as well as developing obesity, type 2 diabetes and CVD in later life(Reference Clausen, Mathiesen and Hansen8). This perpetuates an intergenerational cycle of disease that further escalates the obesity epidemic. To break this cycle, it would be beneficial to generate therapies that prevent GDM from developing(Reference Page and Buchanan9). Current treatments include diet and lifestyle interventions, followed by insulin treatment and, in some countries, oral agents such as metformin. Although women are able to maintain adequate glycaemic control using these treatment strategies, they can be difficult to implement and concerns remain regarding the long-term effects of oral agents on the developing fetus. Further, prevention is preferred over treatment because GDM is typically diagnosed after 24 weeks of gestation, when the fetus may have already been exposed to hyperglycaemia. For these reasons, it would be beneficial to develop novel, safe and effective strategies for GDM risk reduction.
A growing body of research suggests that myo-inositol (MI) – a simple carbohydrate produced in the body and available in foods such as fruits and cereals – can facilitate insulin signalling and reduce blood glucose concentrations in individuals with type 2 diabetes and GDM(Reference D’Anna, Scilipoti and Giordano10). This is because MI forms the structural basis of phosphatidylinositol and the phosphatidyl phosphate lipids (PIP2/PIP3), in the insulin signalling pathway(Reference Di Paolo and De Camilli11). Furthermore, probiotic (PB) supplementation has been associated with improved glucose metabolism and reduced risk of GDM(Reference Badehnoosh, Karamali and Zarrati12). While the mechanisms linking PB supplementation to metabolic health are poorly understood, PB are known to modify the intestinal microbiome and stimulate production of SCFA. SCFA affect the expression of a number of proteins that have been demonstrated to decrease gut permeability and increase insulin sensitivity(Reference Taylor, Woodfall and Sheedy13, Reference Tilg and Moschen14). However, the evidence that MI or PB supplementation should be recommended before or during pregnancy to reduce the risk of GDM is limited(Reference Rogozińska, Chamillard and Hitman15, Reference Plows, Reynolds and Vickers16). Further, it is unknown if the combination of MI and PB – which are both easy-to-administer and safe nutritional supplements that appear to affect glucose regulation via different mechanisms – would have additive effects. The purpose of the present study was to assess if MI and PB, both separately and in combination, would improve glucose tolerance and other measures related to GDM – including lipidaemia, hepatic steatosis and intestinal permeability – in a preclinical mouse model.
Experimental methods
All animal procedures were approved by the University of Auckland Animal Ethics Committee in accordance with the New Zealand Animal Welfare Act, 1999. Eighty 7-week-old nulliparous female C57BL/6 mice were acquired from the Vernon Jansen Unit at the University of Auckland, New Zealand, and housed in groups of four within individually ventilated cages with woodchip bedding. Mice were maintained in a 12-h light cycle environment with an ambient temperature of 22oC and 40–45 % humidity. After 1 week of acclimatisation, mice were randomly assigned to receive either control diet (CD) (AIN-93 G, Research Diets Inc.; 20 % energy protein, 63·9 % energy carbohydrate, 15·8 % energy fat; 3·9 kcal/g (16·3 kJ/g)), CD with MI added to the diet (AIN-93 G, Research Diets Inc.; with 2 % added MI (Sigma-Aldrich)), CD with PB mix added to drinking water (Lactobacillus rhamnosus and Bifidobacterium lactis at 6 g/l, for 109 colony-forming units/d) or CD with MI added to the diet and PB mix added to drinking water. MI dosage was based on previous rodent studies(Reference Franke, Klootwijk and Lemmers17) and was below the maximum dose tested and tolerated in human studies (20 g/d)(Reference Lam, McWilliams and LeRiche18), while PB dosage was based on that used previously in humans(Reference Luoto, Laitinen and Nermes19). The period of 5 weeks of exposure to the treatments prior to the onset of high-fat diet (HFD) and throughout mating and gestation (for a total of about 10 weeks of exposure) was chosen in order to maximise the potential preventive effects of the supplements. This duration is beyond the length of exposure in other studies utilising these supplements in pregnant mice and was therefore determined to be sufficient(Reference Ferrari, Facchinetti and Ontiveros20, Reference Treven, Mrak and Bogovič Matijašić21). Because the PB included maltodextrin (DE 12) as a binding agent, the non-PB groups received an equal dose (5 g/l) of the same form of maltodextrin (Glucidex IT12, Axieo Specialties) in their drinking water. Drinking solutions were measured and changed daily. Preventive measures were taken when handling cages and mice to prevent contamination between PB and non-PB groups, including the use of separate equipment as well as changing PB cages and drinking solutions last. Body weight and food intake were measured weekly. After 4 weeks (12 weeks of age), mice were switched onto HFD (D12451, Research Diets Inc., 20 % energy protein, 35 % energy carbohydrate, 45 % energy fat; 4·73 kcal/g (19·8 kJ/g)), with or without adding 2 % MI. One additional group remained on CD and acted as a reference group. The groups were thereby labelled as follows: CD (reference only), HFD, HFD with MI added to the diet (HFMI), HFD with PB added to drinking water (HFPB) and HFMI and PB added to drinking water (HFMIPB). Groups and their definitions are summarised in Fig. 1. Compositional and fatty acid profiles of the diets used in the present study are provided in online Supplementary Tables S1 and S2.
Experimental design. Timeline of the experiment. Probiotic mix contained Lactobacillus rhamnosus and Bifidobacterium lactis at 109 colony-forming units/d. CD, control diet; HFD, high-fat diet; HFMI, HFD with myo-inositol added to the diet; HFPB, HFD with probiotic added to drinking water; HFMIPB, HFMI and probiotic added to drinking water; GD, gestational day; OGTT, oral glucose tolerance test.

Maternal weight gain, energy intake and litter size at gestational day 18·5 (cull)* (Mean values with their standard errors; n 10–13 mice per group)

CD, control diet; HFD, high-fat diet; HFMI, HFD with myo-inositol added to the diet; HFPB, HFD with probiotic added to drinking water; HFMIPB, HFMI and probiotic added to drinking water; MI, myo-inositol.
* Data were analysed by Student’s t test (CD v. HFD) or two-way ANOVA (all HFD groups) followed by Tukey’s post hoc test.
† Significant difference between HFD and CD (reference).
‡ To convert kcal to kJ, multiply by 4·184.
Maternal plasma profile at gestational day 18·5 (cull)* (Mean values with their standard errors; n 10–13 mice per group)

CD, control diet; HFD, high-fat diet; HFMI, HFD with myo-inositol added to the diet; HFPB, HFD with probiotic added to drinking water; HFMIPB, HFMI and probiotic added to drinking water; MI, myo-inositol; PB, probiotics; HOMA-IR, homeostatic model assessment of insulin resistance.
* Data were analysed by Student’s t test (CD v. HFD) and two-way ANOVA (all HFD groups) followed by Tukey’s post hoc test.
† Significant difference between HFD and CD (reference).
After 1 week of HFD exposure, mice were placed with unrelated males for a period of 1 week. They remained on their allocated diet/treatment throughout mating and pregnancy. HFD 1 week prior to and throughout pregnancy has been previously demonstrated to produce an effective mouse model of gestational-specific glucose intolerance(Reference Pennington, van der Walt and Pollock22). Mice were checked daily by inspection of the vagina for a cervical plug. Upon its detection (denoted gestational day 0·5: GD 0·5), female mice were separated from males and were pair-housed with food and water intake monitored throughout pregnancy. If after 1 week a mouse did not become pregnant, it was removed from the study. Although initial groups consisted of sixteen mice, the numbers that became and remained pregnant for the study period are presented as the final numbers per group in Fig. 1.
Oral glucose tolerance test
Glucose tolerance was measured at GD 16·5. At 08.00 hours, food was removed and, following a 6 h fasting period, blood glucose was measured by slicing 1 mm from the tip of the tail, dabbing the first resulting drop on a paper towel and measuring the second drop with a glucometer (FreeStyle Optimum Neo, Abbott Diabetes Care). Mice were then dosed with 2 g/kg glucose solution via oral administration, and blood glucose was measured at 15, 30, 60 and 120 min(Reference Andrikopoulos, Blair and Deluca23). Blood was also collected in heparinised capillary tubes at 0, 15 and 60 min and plasma prepared for later insulin analysis.
Gut permeability procedure
Gut permeability was assessed as it has been associated with the development of metabolic disease(Reference Do, Lee and Oh24) and PB are thought to affect glucose tolerance in part by reducing gut permeability(Reference Rao and Samak25). At GD 18·5, mice were again fasted for 6 h and then dosed with 4000-Da fluorescein isothiocyanate-dextran (Sigma-Aldrich) via oral administration (600 mg/kg body weight), in order to later assess gut permeability, outlined in the plasma analysis section.
Tissue collection
At GD 18·5, following a 6 h fast, mice were anesthetised using isoflurane and about 1 ml blood was acquired via cardiac puncture. Fasting blood glucose was measured from the tail tip as described above. Mice were then culled by cervical dislocation, and the uterine horns with fetuses were removed and placed into ice-cold saline. The maternal pancreas, liver, adipose tissue (retroperitoneal, gonadal, perirenal and mesenteric) and kidneys were removed, weighed and either snap-frozen and stored at –80°C or fixed in 10 % neutral buffered formalin for later histological analysis. In addition, the digestive tract was removed, flushed with saline, cut into sections (oesophagus, stomach, duodenum, jejunum, ileum, caecum, colon, rectum and faecal samples) and snap-frozen. Fetuses and their placentae were sexed, weighed and length measured.
Plasma analysis
Tail and cardiac puncture blood were collected in EDTA-coated tubes and centrifuged at 2500 rpm for 10 min. Plasma was then aliquoted and stored in light-protected tubes at –20°C. Commercially available mouse-specific ELISA were used to measure plasma insulin (Ultrasensitive Mouse Insulin ELISA, Crystal Chem. no. 90080; sensitivity: 50 pg/ml), leptin (Mouse Leptin ELISA, Crystal Chem. no. 90030; sensitivity: 200 pg/ml) and adiponectin (Mouse Adiponectin ELISA, Crystal Chem. no. 80569; sensitivity: 8 pg/ml). Homeostatic model assessment of insulin resistance (HOMA-IR) was calculated as: (fasting glucose (mmol/l) × fasting insulin (mU/l))/14·1(Reference Mather26). Matsuda index was calculated as: 10 000/(√ (fasting glucose (mmol/l) × fasting insulin (mU/l) × mean glucose over oral glucose tolerance test (OGTT) (mmol/l) × mean insulin over OGTT (mU/l)))(Reference Matsuda and DeFronzo27).
A COBAS automated analyser (Roche Diagnostics) was used to measure plasma total cholesterol (Roche 04718917190; sensitivity: 9·7 mg/dl (0·25 mmol/l)), HDL (Roche 05401488190), LDL (Roche 05401682190) and NEFA (Wako WA243491795).
For gut permeability analysis, 25 µl plasma was diluted in 25 µl PBS (pH 7·4). Two standard curves were obtained by serial two-fold dilution of fluorescein isothiocyanate-D stock solution at 10 mg/ml, covering a wide range (first range 800–12·5 µg/ml; second range 50–0·78 µg/ml). Samples, standards and blanks were transferred to a clear 96-well microplate and were protected from light at all times. Fluorescein isothiocyanate-D concentration was detected using an InfiniteF200 fluorescence spectrophotometer (Tecan) and Tecan I-control software (Tecan) at an excitation wavelength of 485 nm and emission wavelength of 528 nm(Reference Cani, Bibiloni and Knauf28).
Histology
Gonadal adipose, liver and placental tissue samples were fixed in 10 % neutral buffered formalin and were paraffin-embedded and sectioned (10 μm) using a Leica RM 2135 rotary microtome (Leica Instruments). Haematoxylin–eosin staining was performed, and sections were mounted using DPX (Sigma-Aldrich). Slides were visualised under a light microscope (Nikon Eclipse E800), and images were captured with NIS Elements-D software by an individual blinded to the study groups. For adipose histology, four representative images were captured per sample at 20× magnification and images were analysed using ImageJ 1.50v software (US National Institutes of Health) to determine adipocyte size. Four sections has been determined sufficiently in previous studies from our group(Reference Segovia, Vickers and Gray29). For placentae, two images were captured under 4× magnification and the width, labyrinth zone, junctional zone and decidua lengths were determined using ImageJ. For liver, sections were examined under 20× magnification and foci of lobular inflammation were counted and graded (small foci = 1, medium foci = 2, large foci = 3). Ten random images per animal at 40× magnification were evaluated for general steatosis (score of 0–3) and microvesicular steatosis (score of 0–2). NAFLD score was calculated as the unweighted sum of general steatosis, microvesicular steatosis and lobular inflammation scores(Reference Kleiner, Brunt and Van Natta30).
Gene expression analysis
Maternal gonadal adipose tissue was studied because it is most directly associated with the development of metabolic disease in mice(Reference van Beek, van Klinken and Pronk31) and generates the largest RNA yield. RNA was extracted using a Trizol reagent (ThermoFisher Scientific) and a bead homogeniser (TissueLyser; Qiagen) according to the manufacturers’ instructions. Minor modifications were made to the protocol to maximise RNA yield, namely: (1) sample was centrifuged and the lipid layer was removed by a pipette following homogenisation, and (2) samples were left with isopropanol for 2 h at –20oC rather than 10 min at room temperature to aid precipitation of RNA. RNA was suspended in nuclease-free water, and concentrations were measured using a NanoPhotometer N60 (Implen). Only RNA samples with a 260:280 nm ratio of about 2·0 and 260:230 nm ratio of 1·7–2·2 were used further. RNA quality was validated by gel electrophoresis(Reference Almeida-Oliveira, Leandro and Ausina32). mRNA was reverse-transcribed using a high-capacity cDNA kit (Applied Biosystems). Taqman Fast Advanced Master Mix (Applied Biosystems) and pre-designed Taqman probes (Applied Biosystems) were pipetted into microplates using an epiMotion automated pipetting robot (Eppendorf), and quantitative PCR was performed using the Applied Biosystems QuantStudio 6 Flex Real-Time PCR System (ThermoFisher). Taqman probes examined are outlined in online Supplementary Table S3. Gene expression was normalised to Atpaf1 (ATP synthase mitochondrial F1 complex assembly factor 1; Mm00619286_g1) and Tbp (TATA-box binding protein; Mm01277042_m1), according to previous optimisation studies and in-house testing(Reference Almeida-Oliveira, Leandro and Ausina32). The 2–ΔΔCT method was used for analysis(Reference Schmittgen and Livak33).
Maternal organ weights at gestational day 18·5 (cull)* (Mean values with their standard errors; n 10–13 mice per group)

CD, control diet; HFD, high-fat diet; HFMI, HFD with myo-inositol added to the diet; HFPB, HFD with probiotic added to drinking water; HFMIPB, HFMI and probiotic added to drinking water; MI, myo-inositol; PB, probiotics; BW, body weight.
* Data were analysed by Student’s t test (CD v. HFD) or two-way ANOVA (all HFD groups) followed by Tukey’s post hoc test.
† Significant difference between HFD and CD (reference).
Statistical analysis
Statistical analysis was performed using SPSS Statistics 24 (IBM), and graphs were generated in Prism 7 (GraphPad). Sample size was based on in-house pilot data of the model and previous studies of the effects of MI and PB(Reference Do, Lee and Oh24, Reference Rao and Samak25) with the primary outcome being the peak of OGTT (delta = 20 % CmaxHFD). With an α = 0·5 and power = 0·80, and taking into account the fertility rate of C57BL/6 mice on HFD (70 %), a recruitment size of n 16 per group was required, in order to generate a final number of at least n 10 per group. For each outcome, CD (reference) and HFD were compared using unpaired Student’s t test, in order to determine the effects of the short-term HFD model. Within-HFD treatment groups were then compared using two-way ANOVA, with repeated measures in the case of growth/food intake curves and OGTT results(34). Box plots, Shapiro–Wilk’s test and Levene’s test were used to assess outliers, normality and homogeneity of variances, respectively. If outliers were determined to be genuine and not the result of input or measurement error, the outlier value was winsorized(Reference Ghosh and Vogt35). Where data failed Shapiro–Wilk’s or Levene’s test, data were appropriately transformed(34). Where both the non-transformed and transformed data yielded the same result (i.e. degrees of significance), non-transformed data are presented for clarity. Where a significant two-way interaction between MI and PB was present, multiple comparison differences were detected using Tukey’s post hoc test. Where there were significant differences between treatment groups, Hedges’ g statistic (the recommended measure for sample sizes < 20) was used to calculate the effect size of these differences(Reference Hedges36). Data are presented as mean values with their standard errors.
Results
Pre-pregnancy measurements
Body weights did not differ amongst the groups until after the commencement of HFD, at which point groups fed HFD weighed more than CD (P = 0·030); no differences were observed across treatment groups (Fig. 2(A)). Similarly, food and energy intake did not differ amongst the groups until after the commencement of HFD, at which point HFD groups had increased energy intake compared with CD, including adjustment for energy intake from fluids (Fig. 2(B–D); P = 0·028). However, again there were no effects of treatment.
Pre-pregnancy measurements. Fluid intake was measured daily, and body weights and food intake were measured weekly. (A) Body weights per mouse per week prior to mating; (B) food intake per mouse per week prior to mating; (C) energy intake from fluid per d per mouse prior to mating; (D) energy intake per week per mouse accounting for fluid energy. Data were analysed by repeated-measures ANOVA and expressed as mean values with their standard errors, where * P < 0·05 all groups compared with CD; n 16 mice per group.  , CD;
, CD;  , HFD;
, HFD;  , HFMI;
, HFMI;  , HFPB;
, HFPB;  , HFMIPB. CD, control diet; HFD, high-fat diet; HFMI, HFD with myo-inositol added to the diet; HFPB, HFD with probiotic added to drinking water; HFMIPB, HFMI and probiotic added to drinking water. † To convert kcal to kJ, multiply by 4·184.
, HFMIPB. CD, control diet; HFD, high-fat diet; HFMI, HFD with myo-inositol added to the diet; HFPB, HFD with probiotic added to drinking water; HFMIPB, HFMI and probiotic added to drinking water. † To convert kcal to kJ, multiply by 4·184.

Pregnancy measurements
There were no differences between CD and HFD in gestational weight gain or litter size. MI was associated with reduced gestational weight gain (g = 1·91, P = 0·013), which was not explained by any difference in litter size (Table 1). While groups fed HFD had reduced food intake over pregnancy compared with CD (P = 0·020), this difference disappeared when expressed as energy intake. No effects of treatment were observed (Table 1).
Oral glucose tolerance test and fasting plasma measurements
HFD 1 week before and throughout pregnancy successfully induced glucose intolerance at GD 16·5, as demonstrated at 30 (P < 0·0001) and 60 (P = 0·003) min of the OGTT, and in the AUC (P = 0·0004; Fig. 3(A) and (B)). However, there was no effect of any of the treatments on oral glucose tolerance (Fig. 3(A)and (B)). There were also no differences between any of the groups in plasma insulin during the OGTT (Fig. 3(C) and (D)).
Glucose tolerance and plasma insulin concentrations at gestational day (GD) 16·5. (A) Oral glucose tolerance test (OGTT) curves following oral administration of 2 g/kg d-glucose at GD 16·5; (B) AUC of OGTT curves at GD 16·5; (C) plasma insulin concentration during OGTT at GD 16·5; (D) insulin AUC at GD 16·5. Data were analysed by two-way repeated-measures, Student’s t test (control diet (CD) v. high-fat diet (HFD)) or two-way ANOVA followed by Tukey’s post hoc test (all HFD groups) and expressed as mean values with their standard errors. ** P < 0·01, *** P < 0·001 and **** P < 0·0001 when HFD is compared with CD group; n 10–13 mice per group. (A and C) 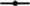 , CD;
, CD; 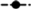 , HFD;
, HFD; 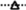 , HFMI;
, HFMI; 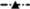 , HFPB;
, HFPB;  , HFMIPB. (B and D)
, HFMIPB. (B and D)  , No myo-inositol (MI);
, No myo-inositol (MI);  , MI. HFMI, HFD with MI added to the diet; HFPB, HFD with probiotic added to drinking water; HFMIPB, HFMI and probiotic added to drinking water; PB, probiotics; Int., interaction.
, MI. HFMI, HFD with MI added to the diet; HFPB, HFD with probiotic added to drinking water; HFMIPB, HFMI and probiotic added to drinking water; PB, probiotics; Int., interaction.

HFD decreased fasting plasma insulin (P = 0·033) and increased fasting plasma LDL at GD 18·5 compared with CD (P = 0·014, Table 2). There were no differences between HFD and CD in fasting blood glucose, plasma leptin, adiponectin, Matsuda index or HOMA-IR at GD 18·5. PB was associated with increased fasting blood glucose (g = 0·64; P = 0·043) and plasma total cholesterol (g = 0·85; P = 0·015) at GD 18·5 (Table 2). Treatments had no effect on fasting plasma insulin, leptin, HOMA-IR, Matsuda index, adiponectin, HDL, LDL or NEFA at GD 18·5 (Table 2).
Gut permeability
There were no significant differences between any of the groups in plasma fluorescein isothiocyanate-D concentration at GD 18·5, indicating no differences in gut permeability (online Supplementary Fig. S1).
Organ weights
HFD increased retroperitoneal (P = 0·011) and gonadal (P = 0·023), but not perirenal and mesenteric adipose deposition, compared with CD (Table 3). HFD also resulted in decreased pancreas weight (P = 0·042), but had no impact on average kidney or liver weight (Table 3). There were no effects of MI or PB on adipose deposition in any depot or on average kidney weight. PB was associated with increased pancreas weight (g = 0·68; P = 0·042, Table 3). Further, an interaction between MI and PB treatment was observed when liver weight was assessed (P = 0·048); mice receiving PB and MI simultaneously showed a slight reduction in relative liver weight when compared with the single treatments (Table 3). There were, however, no significant multiple comparison differences.
Adipocyte histology
HFD increased average adipocyte size (P = 0·036; Fig. 4(A) and (B)) and increased the proportion of adipocytes measured at >15 000 µm compared with CD (P = 0·024; Fig. 4(C)). Neither MI nor PB had any effect on adipocyte histology (Fig. 4).
Adipocyte histology. (A) Representative haematoxylin–eosin stained sections of gonadal adipose tissue. Scale bar = 10 µm. (B) Average adipocyte area per group; (C) percentage of adipocytes per area bracket. Data were analysed by Student’s t test (control diet (CD) v. high-fat diet (HFD)) or two-way ANOVA followed by Tukey’s post hoc test (all HFD groups) and expressed as mean values with their standard errors, where * P < 0·05, HFD v. CD; n 10–13 mice per group. (B)  , No myo-inositol (MI);
, No myo-inositol (MI);  , MI. (C)
, MI. (C)  , CD;
, CD;  , HFD;
, HFD;  , HFMI;
, HFMI;  , HFPB;
, HFPB;  , HFMIPB. HFMI, HFD with MI added to the diet; HFPB, HFD with probiotic added to drinking water; HFMIPB, HFMI and probiotic added to drinking water; PB, probiotics; Int., interaction.
, HFMIPB. HFMI, HFD with MI added to the diet; HFPB, HFD with probiotic added to drinking water; HFMIPB, HFMI and probiotic added to drinking water; PB, probiotics; Int., interaction.

Gonadal adipose tissue gene expression
HFD was associated with reduced gonadal adipose gene expression of Pck1 (P = 0·028) and Pparg (P = 0·0007) compared with CD (Fig. 5(D) and (E)). There were significant MI/PB interactions observed when the expression of Ir (P = 0·002), Irs1 (P = 0·002), Akt2 (P < 0·0001) and Pck1 (P = 0·0012) was analysed. In all of these cases, HFMI and HFPB increased the expression compared with HFD alone, but HFMIPB did not (Fig. 5). There was also a significant increase in Akt2 expression amongst MI groups overall (g = 1·06; P = 0·023; Fig. 5(C)), and a significant increase in Pparg expression amongst PB groups overall (g = 2·04; P = 0·024; Fig. 5(E)). No differences were observed in Slc2a4, Igf1r, Fas, Lepr, Tnf, Mcp1, Il6, Angptl4, Nlrp3, Nfκb, Il1β, Cd11 or Ccr5 (online Supplementary Fig. 2).
Gonadal adipose tissue gene expression. Adipose mRNA expression determined by quantitative PCR. Differences were seen in: (A) Ir; (B) Irs1; (C) Akt2; (D) Pck1; (E) Pparγ. Data were analysed as Student’s t test (control diet (CD) v. high-fat diet (HFD)) or two-way ANOVA followed by Tukey’s post hoc test (all HFD groups) and presented as mean values with their standard errors, where * P < 0·05 and **** P < 0·0001 when HFD is compared with CD. a,b,c Unlike letters denote a significant difference between groups according to Tukey’s post hoc test. n 6–10 mice per group.  , No myo-inositol (MI);
, No myo-inositol (MI);  , MI. HFMI, HFD with MI added to the diet; HFPB, HFD with probiotic added to drinking water; HFMIPB, HFMI and probiotic added to drinking water; PB, probiotics; Int., interaction.
, MI. HFMI, HFD with MI added to the diet; HFPB, HFD with probiotic added to drinking water; HFMIPB, HFMI and probiotic added to drinking water; PB, probiotics; Int., interaction.

Hepatic histology
HFD increased hepatic non-alcoholic steatosis score compared with CD (P = 0·015; Fig. 6(C)). None of the treatments had any effects on hepatic histology (Fig. 6).
Hepatic histology. Haematoxylin–eosin stained sections of liver. Each section was examined under 20× magnification to evaluate lobular inflammation. Ten random 40× magnification fields per animal were evaluated for general steatosis and microvesicular steatosis. (A) Representative micrographs from each experimental group at 20× magnification; (B) representative micrographs from each experimental group at 40× magnification. Scale bars = 10 µm. (C) Non-alcoholic fatty liver disease (NAFLD) activity score (NAS) in table format. Data were analysed by Student’s t test (control diet (CD) v. high-fat diet (HFD)) or two-way ANOVA followed by Tukey’s post hoc test (all HFD groups) and presented as mean values with their standard errors, where * P < 0·05 when HFD is compared with CD; n 10–13 mice per group. HFMI, HFD with myo-inositol added to the diet; HFPB, HFD with probiotic added to drinking water; HFMIPB, HFMI and probiotic added to drinking water; MI, myo-inositol; PB, probiotics.

Fetal measurements
HFD reduced male fetal weight (P = 0·037), female fetal weight (P = 0·0016), male abdominal circumference (P = 0·0043) and female abdominal circumference (P < 0 0001) compared with CD (Table 4). PB was associated with increased male fetal weight (g = 0·68; P = 0·035) and increased female placental weight (g = 0·89; P = 0·021) in HFD-fed animals, making them more similar to those from CD dams (Table 4). An interaction between MI and PB treatment was observed when male abdominal circumference was measured, in which PB tended to increase abdominal circumference in the absence of MI, but tended to decrease it in the presence of MI, although there were no significant multiple comparison differences (Table 4).
Fetal measurements* (Mean values with their standard errors; n 10–13 mice per group)

CD, control diet; HFD, high-fat diet; HFMI, HFD with myo-inositol added to the diet; HFPB, HFD with probiotic added to drinking water; HFMIPB, HFMI and probiotic added to drinking water; MI, myo-inositol; PB, probiotics.
* Data were analysed by Student’s t test (CD v. HFD) or two-way ANOVA (all HFD groups) followed by Tukey’s post hoc test.
† Significant difference between HFD and CD (reference).
Discussion
The aim of the present study was to determine whether MI and PB, taken together or separately before and during pregnancy, would impact the development of HFD-induced glucose intolerance during pregnancy(Reference Pennington, van der Walt and Pollock22). This mouse model allowed a factorial design to determine the interaction of treatments, as well as more thorough examination of potential mechanistic pathways and whole-tissue analysis, which would not be possible in human trials.
Suitability of the mouse model
GDM is a challenging condition to model in small animals, as reviewed by Pasek & Gannon(Reference Pasek and Gannon37). This is as GDM, by definition, only develops after the onset of pregnancy(1). The model used in the present study is an adaptation of a mouse model previously developed by Pennington et al. (Reference Pennington, van der Walt and Pollock22). We chose this model because our original model of choice, the heterozygous LepRdb/+ mouse, did not display glucose intolerance, as discussed in detail in our previous publications(Reference Plows, Budin and Andersson38, Reference Plows, Yu and Broadhurst39). Pennington et al. demonstrated that acute exposure to HFD 1 week prior to and during pregnancy impaired islet cell proliferation, therefore reducing insulin secretion and resulting in gestational glucose intolerance. We similarly demonstrated glucose intolerance compared with CD – our primary outcome. Similar to that of Pennington et al., we also observed reduced plasma fasting insulin. This result is in contrast with most longer-term HFD studies in mice and in women with GDM, where fasting insulin is usually raised due to insulin resistance(Reference Wang and Liao40, Reference Catalano, Kirwan and Haugel-de Mouzon41). We also did not observe leptin resistance in our model – another typical trait in long-term HFD rodent studies and in GDM(Reference Lin, Thomas and Storlien42, Reference Soheilykhah, Mojibian and Rahimi-Saghand43). It is likely that our acute exposure to HFD was insufficient for insulin and leptin resistance to develop and that longer exposure to HFD would have resulted in a more pronounced metabolic phenotype. However, such an extended exposure would have negated the pregnancy-specific aspect of the study. Our model did demonstrate increased body weight, increased adipose tissue deposition, increased LDL-cholesterol, increased adipocyte size and reduced fetal weight compared with CD. Each of these outcomes is associated with GDM with the exception of reduced fetal weight (GDM usually results in macrosomia(Reference Kc, Shakya and Zhang44)). However, reduced fetal weight is commonly observed in pregnant mice-fed HFD(Reference Mark, Sisala and Connor45, Reference Kamimae-Lanning, Krasnow and Goloviznina46), which is one of the limitations of using HFD-induced models of GDM. Overall, our model was effective at inducing our primary outcome (glucose intolerance), but not many of the secondary characteristics of GDM, including insulin resistance, and our results should be viewed in light of these limitations.
Effects of myo-inositol
MI supplementation did not significantly improve glucose tolerance, our primary outcome. However, MI did increase adipose gene expression of key members of the insulin signalling pathway – Ir, Irs1, Akt2 and Pck1. Mice in the HFMI group consumed on average 3 g/d, which extrapolates to approximately 60 mg MI/d, which is beyond the 36 mg/d recently reported to show beneficial effects in pregnant mice(Reference Ferrari, Facchinetti and Ontiveros20). Previous studies have similarly demonstrated beneficial effects of MI at doses ranging from 0·08 to 48 mg/d in mouse models of neural tube defects(Reference Reece, Khandelwal and Wu47, Reference Cogram, Tesh and Tesh48). Therefore, it is unlikely that the lack of effect on glucose tolerance in the present study was due to an insufficient dose of MI. Although the dietary model used in the present study did demonstrate impaired glucose tolerance, the absence of fasting hyperglycaemia or insulin resistance in this present study suggests that it is a very mild model of GDM, which may have prevented us from demonstrating some of the benefits of MI. This is consistent with the results of Ferrari et al., which reported very little effect of MI in HFD-fed pregnant mice, but did see benefit in a mouse model of the metabolic syndrome (HFD + eNOS–/–)(Reference Ferrari, Facchinetti and Ontiveros20). One explanation offered by the authors was that the metabolic syndrome model displayed fasting hyperglycaemia and hyperleptinaemia, while the HFD-only model did not. Also consistent with Ferrari et al., we demonstrated reduced gestational weight in MI-fed mice. This finding is notable, as excessive gestational weight gain is a significant risk factor for poor pregnancy outcomes, including GDM(Reference Durnwald49). However, we saw no effect of MI on adipose deposition (i.e. fat mass) or adipose or liver histology. Increased fat deposition, adipocyte hyperplasia and liver steatosis are all indicators of metabolic disease(Reference Cotillard, Poitou and Torcivia50–Reference Cali, De Oliveira and Kim52). In contrast, Croze et al. reported reduced adipose deposition in HFD-fed male mice supplemented with MI, although they similarly saw no improvement in liver steatosis with MI(Reference Croze, Géloën and Soulage53). These discrepancies may simply represent differences between sexes and during pregnancy. Further, MI did not improve the growth restriction observed in the HFD group in the present study, which aligns with the results of Ferrari et al.Reference Ferrari, Facchinetti and Ontiveros20 and with a previous study from our group(Reference Segovia, Vickers and Gray29, Reference Schmittgen and Livak33). However, it should be noted that GDM is more frequently associated with macrosomia, which is difficult to replicate in rodents. In human trials, MI is associated with reduced rates of fetal macrosomia(Reference D’Anna, Scilipoti and Giordano10, Reference Matarrelli, Vitacolonna and D’Angelo54).
Effects of probiotics
Like MI, PB did not affect glucose tolerance, but did increase adipose gene expression of insulin signalling mediators Ir, Irs1, Akt2 and Pck1 compared with HFD alone. PB was also surprisingly associated with increased fasting blood glucose and plasma total cholesterol concentrations. A recent meta-analysis of thirty-two randomised controlled trials (RCT) of various strains of PB noted a significant reduction in total cholesterol concentration(Reference Wang, Guo and Gao55). However, one RCT investigating the effects of Lactobacillus salivarius in GDM did report an increase in total and LDL-cholesterol during pregnancy(Reference Lindsay, Brennan and Kennelly56). Therefore, it may be the case that PB have unintended consequences for lipid metabolism during pregnancy, and this warrants further investigation. The most recent systematic review/meta-analysis of the use of various PB for the management of GDM found that PB do not decrease fasting glucose or LDL, which is consistent with our results(Reference Taylor, Woodfall and Sheedy13).
PB also had a significant effect on adipose Pparγ expression (Hedges’ g was 2·0, where a Hedges’ g of 0·8 is considered a large effect size(Reference Hedges36, Reference Ellis57)). PB supplementation (Lactobacillus reuteri, Lactobacillus crispatus, Bacillus subtilis (Reference Memarrast, Ghafouri-Fard and Kolivand58) and Lactobacillus casei, B. bacterium longum (Reference Karimi, Jamaluddin and Mohtarrudin59)) has previously been associated with enhanced PPARγ activation in HFD- and STZ-induced rodent models of obesity and diabetes(Reference Memarrast, Ghafouri-Fard and Kolivand58, Reference Karimi, Jamaluddin and Mohtarrudin59). Several studies similarly suggest that the PB compound VSL#3 exerts its beneficial effects through PPARγ-dependent mechanisms(Reference Ewaschuk, Endersby and Thiel60–Reference Mencarelli, Distrutti and Renga62). However, to our knowledge, the PB strains used in the present study (L. rhamnosus and B. lactis) have not been previously linked to PPARγ. Typically, up-regulated Pparγ expression results in improved adipogenic capacity and a reduction in ectopic fat deposition, such as in the liver. However, we did not observe any effects of PB on measures of liver steatosis. Therefore, while our results further support a Pparγ-inducing effect of PB supplementation, we have not confirmed any physiological benefit from this.
PB also increased maternal pancreas weight, male fetal weight and female placental weight. Typically, increased pancreatic mass will be accompanied by reduced blood glucose; however, in the present study, we saw the opposite(Reference Yagihashi63). These data could illustrate a feedback mechanism, whereby pancreatic mass increased to compensate for increased blood glucose. The observed increase in fetal and placental weight following PB treatment could be interpreted as an improvement of HFD-induced growth restriction when compared with the CD group. However, our study was not powered for this outcome, and it should be noted that the available data on PB use in human pregnancy have not reported any meaningful changes in fetal weight or growth(Reference Badehnoosh, Karamali and Zarrati12).
Effects of combined myo-inositol and probiotics
For most outcomes, the combination of MI and PB did not result in an additive, beneficial effect compared with the effects seen when the ingredients were administered separately. Indeed, in some cases, the combination negated beneficial effects of the individual components. This was most pronounced with adipose gene expression: while MI and PB individually enhanced the expression of Ir and Akt2, the HFMIPB group was not different than HFD alone. As ours is the first study to examine MI and PB together, the reasons for this are unknown. However, our data suggest that the combination of MI and PB might not be more effective than the individual components for managing glucose intolerance and associated metabolic outcomes during pregnancy.
Strengths of the present study include the balanced two-way factorial ANOVA design, allowing for pooled analysis of treatments, and the onset of supplementation before pregnancy, allowing an investigation into the preventative effects of MI and PB. As discussed earlier, a limitation of the present study is that the chosen mouse model – short-term HFD feeding – did not result in many of the metabolic dysfunctions that usually accompany glucose intolerance. It is possible that longer exposure to HFD would have resulted in a more severe phenotype (albeit, one not limited to pregnancy) and that in this case we may have seen some effect of MI and/or PB. This is especially true given that both supplements had effects on adipose gene expression. Another limitation of the present study is that we did not examine the supplements in normal control-fed animals during pregnancy. We recognise that supplements such as these may have exhibit different effects in healthy animals. It is also important to note that fathers were exposed to the same diets as the mothers during the mating period (1 week) and that therefore paternal effects may have contributed to the fetal and placental outcomes.
In conclusion, neither MI, PB, nor the combination of the two had an impact on HFD-induced glucose intolerance. The effects of the treatments on other measures of metabolic health during pregnancy were also minimal. MI and PB did separately affect adipose tissue gene expression of insulin signalling mediators (both increased Ir, Irs1, Akt2 and Pck1), but this effect was ameliorated in the combination. PB was also associated with increased fasting glucose and total cholesterol, which are of unknown consequence. It is possible that the lack of some key features of GDM in the model used in the present study (fasting hyperglycaemia, hyperinsulinaemia, hyperleptinaemia and adipose inflammation) may have prevented a full demonstration of the effects of MI and PB.
Acknowledgements
The authors would like to thank Axieo Specialties, who donated the maltodextrin used for control purposes. They would also like to acknowledge Satya Amirapu, who was responsible for histological processing, sectioning and staining, Thashma Ganapathy for assistance with animal experiments, and Michael Pellizzon for formulating the diets used in the present study.
This work was funded by Nestec Ltd. The funders contributed to the design of the study and approved the final version of the manuscript, but did not conduct the study, analyse the data or write the manuscript. The maltodextrin used for control purposes was donated by Axieo Specialties.
J. P. helped to design the study, collected data, analysed data and primarily wrote the manuscript. J. R. N., F. B., K. M. and I. S. Z. helped to design the study. C. R. helped to supervise the study and edit the manuscript. M. V. and P. B. helped to design and supervise the study and edit the manuscript. J. S. helped to design the study, supervised the study, collected data and edited the manuscript.
J. M. R. N., F. B., K. M. and I. S.-Z. are full-time employees of Nestlé Research.
Supplementary material
For supplementary materials referred to in this article, please visit https://doi.org/10.1017/S0007114519003039












