Diet is an important factor in the prevention of CVD as demonstrated in the Nurses' Health Study, a large prospective study on 121 700 initially healthy nurses(Reference Hu, Stampfer and Manson1), in which high intakes of SFA, trans-fatty acids and carbohydrates with a high glycaemic index (GI) were associated with increased CVD risk(Reference Hu, Stampfer and Manson1, Reference Liu, Willett and Stampfer2), and high intakes of MUFA and PUFA were associated with reduced CVD risk(Reference Hu, Stampfer and Manson1).
An alternative dietary pyramid has been introduced in the USA by Willett(Reference Willett3), one of the Nurses' Health study investigators. The main difference between Willett's new pyramid and the US Department of Agriculture (USDA) 2004 Food Pyramid(4) is that the new pyramid has no restrictions on fat as long as it is of vegetable origin, and carbohydrates should have a high content of whole grains. Such a diet is assumed to have a more cardioprotective effect than a diet following the USDA 2004 Food Pyramid. Although the Nurses' Health Study is a very large and well-designed study, the study conclusions should not alone be used to change the established dietary recommendations without also having results from long-term controlled comparisons with existing dietary recommendations. Because a controlled randomised dietary study in healthy individuals with CVD as the end point will be practically infeasible, CVD risk markers can be studied as an alternative.
Inflammation and endothelial dysfunction are key factors in CVD as illustrated by the association between plasma variables and the risk of CVD in prospective studies. Associations have been observed for C-reactive protein (CRP)(Reference Danesh, Collins and Appleby5), IL-6(Reference Danesh, Kaptoge and Mann6), intercellular adhesion molecule (ICAM-1)(Reference Ridker7), von Willebrand factor (vWF)(Reference Martinelli8, Reference Morange, Simon and Alessi9) and tissue factor pathway inhibitor (TFPI)(Reference Morange, Simon and Alessi9). Intervention studies have reported an effect of specific dietary components on these CVD risk markers, e.g. effects of specific fatty acids on CRP and IL-6(Reference Baer, Judd and Clevidence10–Reference Rallidis, Paschos and Liakos12), and intervention studies based on dietary advice have observed long-term effects of complex dietary changes on CRP(Reference Esposito, Marfella and Ciotola13–Reference Wolever, Gibbs and Mehling15).
The aim of the present study was to compare the long-term effect on markers of inflammation and endothelial cell function of three different ad libitum diets in a 6-month strictly controlled dietary intervention in healthy obese subjects after weight loss. The diets compared were Willett's new Healthy Eating Pyramid (high in MUFA and low in GI), the Official Nordic Dietary Guidelines (low in fat and medium in GI) and the average Danish diet (high in SFA and high in GI). We hypothesise that inflammation and endothelial cell function will be improved most favourably by the diet high in MUFA and low in GI.
Experimental methods
Study population
The dietary intervention, Mono Unsaturated Fatty acids in Obesity (MUFObes), was conducted at the Department of Human Nutrition, Faculty of Life Sciences, University of Copenhagen (Frederiksberg, Denmark), and has been described in detail elsewhere(Reference Due, Larsen and Mu16, Reference Rasmussen, Larsen and Mortensen17). Briefly, 131 obese individuals were randomly assigned to one of three diets. The inclusion criteria were age 18–35 years, BMI 28–36 kg/m2, body-weight fluctuations of < 3 kg over the previous 2 months and a non-smoking status. Subjects were healthy and took no regular medicine other than contraceptive pills. All subjects gave oral and written informed consent, and the Ethics Committee of the Municipalities of Copenhagen and Frederiksberg approved the study according to the Declaration of Helsinki. The trial was registered at clinicaltrials.gov as NCT00274729.
The population characteristics at study entry are described in Table 1. For various reasons, twenty-five participants dropped out during the intervention period, leaving thirty-nine participants in the MUFA group, forty-three participants in the LF group and twenty-four participants in the control group(Reference Due, Larsen and Mu16).
(Mean values and standard deviations)
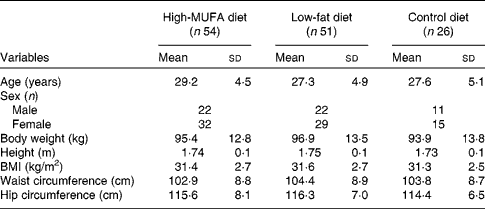
* Measurements were made at screening before weight loss. Mean values for the three diets were compared with an ANOVA. Sex was compared using the χ2 test. No significant differences existed between the groups at study entry.
Study design
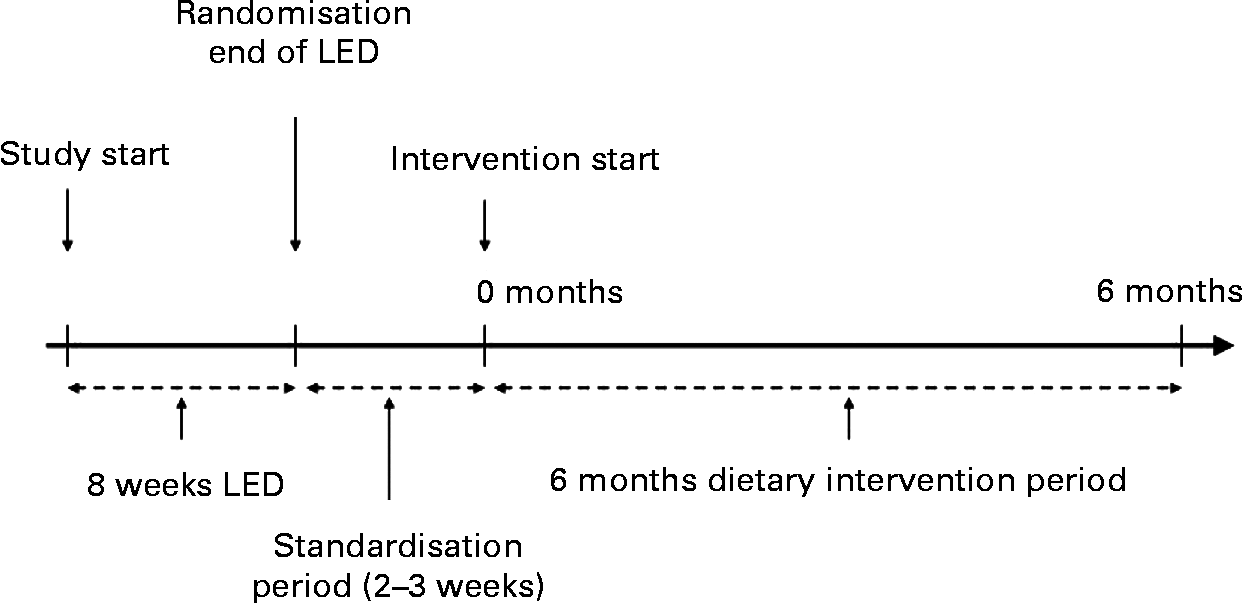
The study was a parallel intervention trial comparing the effect of three diets on body weight and cardiovascular risk after 6 months of intervention. The study design is presented in Fig. 1 and has been described in detail previously(Reference Skov, Toubro and Raben18). After an initial 8-week low-energy diet, only subjects who lost >8 % of their body weight were randomised to one of the experimental diets. After randomisation, the participants completed a 3-week standardisation period (weight stabilisation and adaptation to the supermarket model) eating a diet resembling the average Danish diet, corresponding to the control diet. The 6-month intervention study started in May 2004 and ended in November 2004.
Design of the Mono Unsaturated Fatty acids in Obesity study. LED, low-energy diet.
The experimental diets
The 6-month dietary intervention was based on an ad libitum design in order to mimic free-living conditions and to test the real appetite regulation of the diets. The three prescribed diets were as follows: (1) the MUFA diet designed to be moderate in fat (35–45 % of energy), high in MUFA (>20 % of energy) and moderate in low-GI carbohydrates (40–50 % of energy), with a high content of vegetable oils, whole-grain food, nuts and legumes); (2) the LF diet low in fat (20–30 % of energy) and high in mixed-GI carbohydrates (55–65 % of energy); (3) the control diet corresponding to the average Danish diet moderate in fat (30–40 % of energy), high in SFA (>15 % of energy), moderate in high-GI carbohydrates (45–55 % of energy) and low in fibre ( < 3 % of energy). All three diets were moderate in protein (10–20 % of energy). Foods recommended for the three dietary groups have previously been described(Reference Due, Larsen and Mu16). The actual dietary composition (Table 2) was in accordance with the prescribed dietary composition, and the biopsy content of fatty acids (assessment of compliance) was in accordance with the prescribed diets(Reference Due, Larsen and Mu16).
(Mean values and 95 % confidence intervals)
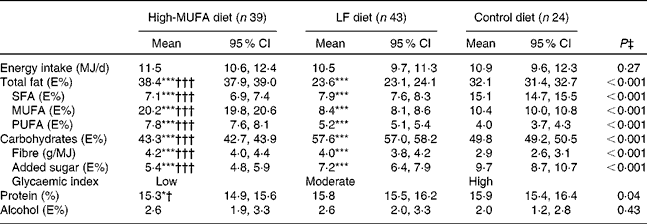
LF, low fat; E%, percentage of energy.
Mean value was significantly different from that for control: *P < 0·05, ***P < 0·001 (pairwise analyses).
Mean value was significantly different from that for LF: † P < 0·05, ††† P < 0·001 (pairwise analyses).
‡ Mean values for the three diets were compared with an ANOVA.
Supermarket foods, the computer program and shopping sessions
To provide the subjects with all necessary foods and to accomplish a total recording of the food consumed, a validated supermarket model(Reference Skov, Toubro and Raben18) was established at the department. The supermarket foods, the computer program and the shopping sessions have been described extensively elsewhere(Reference Due, Larsen and Mu16, Reference Rasmussen, Larsen and Mortensen17, Reference Due, Larsen and Hermansen19). Throughout the 6 months of intervention, the subjects obtained all foods and beverages at the study supermarket, free of charge, and they were instructed to consume only these foods.
Blood sampling
Venous blood samples were drawn after lying in a supine position for 10 min after at least 10 h fasting, and 24 h abstention from alcohol and strenuous physical activity.
Blood samples were collected with minimal stasis using siliconised vacutainers and 21 gauge needles in citrated tubes at room temperature for analyses of CRP, IL-6, ICAM, vWF, TFPI, TAG and total cholesterol.
Tubes were centrifuged at 20°C for 20 min at 2000 g. Plasma was pipetted into plastic vials and stored at − 70°C.
Blood analyses
Plasma samples were rapidly thawed in a water-bath at 37°C and analysed in one series for each subject. Cholesterol, HDL-cholesterol and TAG were determined enzymatically with a COBAS INTEGRA (Roche, Mannheim, Germany). LDL concentration was calculated as follows: LDL = total cholesterol − HDL − (TAG/2·2). Concentrations of CRP (mg/l) were determined by the Latex method (Roche). Commercial ELISA were used to measure concentrations of IL-6 (pg/ml) (R&D Systems, Abingdon, Oxon, UK), ICAM (ng/ml) (R&D Systems), vWF (%) (Liatest®VWF:Ag; Diagnostica Stago, Asnières, France) and total TFPI (ng/ml) (Asserachrom®Total TFPI; Diagnostica Stago). ELISA used were highly sensitive, and no results were below the detection limits. The inter-assay CV were < 6 % for CRP, < 7 % for IL-6, < 7 % for ICAM, < 3 % for vWF and < 8 % for TFPI.
Statistics
Statistical analyses were done on completers only and performed using the SPSS program (version 16; SPSS, Inc., Chicago, IL, USA). The distribution of the results for TAG, CRP and IL-6 was skewed, and values were logarithmically transformed before analysis. Fasting values were compared between the three diets at the start of the intervention (0 months) and at the end of the intervention (6 months) using an ANOVA. When significant between-diet effects were observed, post hoc analyses were performed for pairwise analyses and adjusted for multiple comparisons by the Bonferroni test.
For test for differences within groups, fasting values at 6 months were compared with fasting values at 0 months for each of the three diets separately using a paired t test. Furthermore, differences between the diet groups in changes from months 0 to 6 for all variables were analysed by a univariate ANOVA using dietary group as a fixed factor and baseline values, changes in BMI (or waist:hip ratio), and changes in total cholesterol and TAG as covariates in order to adjust for possible confounders. In the case of significance in the ANOVA, pairwise analyses were performed.
All results are presented as means or geometric means. A P value of less than 0·05 was considered statistically significant.
Results
Of the study participants, seven were excluded from the statistical calculations due to concentrations of CRP>10 mg/l (n 6), indicating an inflammatory condition, or very high concentrations of ICAM (1434 ng/ml, n 1), signifying pronounced endothelial cell dysfunction. These seven participants were distributed as follows: three participants in the MUFA group; three participants in the LF group; one participant in the control group (four participants at 0 months and three participants at 6 months).
There were no significant differences in baseline values (month 0) between the three experimental diets except for significant difference in BMI between the MUFA diet and the LF diet (Table 3). This difference persisted after 6 months (P < 0·01) with significant differences also between the MUFA diet and the control diet (P < 0·05). No other significant differences were observed after 6 months between the three diets (Table 3).
(Mean values and standard deviations)
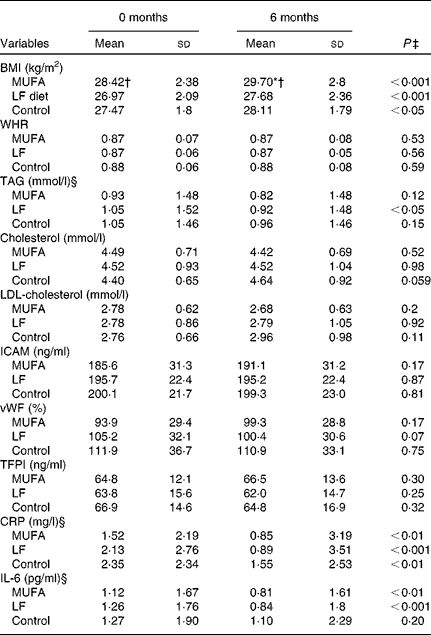
WHR, waist:hip ratio; ICAM, intercellular adhesion molecule; vWF, von Willebrand factor; TFPI, tissue factor pathway inhibitor; CRP, C-reactive protein.
* Mean value was significantly different from that for control (P < 0·05).
† Mean value was significantly different from that for LF (P < 0·05).
‡ Mean values at 0 and 6 months were compared using a paired t test within the diet groups. Between-diet comparisons at 0 and 6 months were performed using an ANOVA. When significant between-diet effects were observed, pairwise comparisons were performed using the Bonferroni test.
§ TAG, CRP and IL-6 were logarithmically transformed before analysis (geometric means and standard deviations).
When the effects of 6 months of intervention were analysed within each dietary group, all three diets resulted in a significant increase in BMI (MUFA, 1·28 (sd 1·45) kg/m2; LF, 0·71 (sd 1·12) kg/m2; control, 0·64 (sd 1·34) kg/m2) and a significant decrease in CRP (MUFA, 0·48 (sd 1·93) mg/l; LF, 1·46 (sd 2·89) mg/l; control, 1·20 (sd 1·97) mg/l). Concentrations of IL-6 were reduced on the MUFA diet (0·37 (sd 0·74) pg/ml) and the LF diet (0·47 (sd 0·69) pg/ml). The LF diet also resulted in a significant decrease in TAG (0·16 (sd 0·37) mmol/l) and a tendency to a decrease in vWF (4·78 (sd 16·44) %), P = 0·07). Concentrations of cholesterol were increased on the control diet (0·21 (sd 0·50) mmol/l; Table 3). No significant changes were observed in waist:hip ratio, LDL-cholesterol, ICAM and TFPI (Table 3).
Changes in vWF concentrations from months 0 to 6 tended to differ between the diet groups (P = 0·07). This was due to significantly different vWF changes during 6 months (mo) between the MUFA diet (ΔvWF 0 → 6 moMUFA = 5·60 (sd 23·8) %) and the LF diet (ΔvWF 0 → 6 moLF = − 4·78 (sd 16·4) %) (P = 0·022), with a reduction on the LF diet and an increase on the MUFA diet. However, this difference was no longer significant (P = 0·21) after adjustment for covariates due to a significant effect of baseline values and changes in TAG. No differences between the diet groups in changes from months 0 to 6 were observed for the other variables measured.
Discussion
In the present weight-loss maintenance study, CRP concentration was significantly lowered irrespective of the experimental diet, and the concentration of IL-6 was lowered by the MUFA diet and the LF diet (Table 3). We observed a tendency to reductions in vWF concentrations on the LF diet (P = 0·07) and not on the MUFA diet. Changes in vWF concentrations during 6 months differed significantly between the LF and MUFA diet groups (P = 0·022), but this difference disappeared after adjustment for covariates. No other significant differences were observed between changes induced by the different diets.
The observed effects on vWF may suggest a less favourable effect on the endothelium of the MUFA diet compared with the LF diet, but this cannot be confirmed by others. In one study, vWF concentrations decreased after 4 weeks on a high-MUFA diet compared with a low-fat diet(Reference Perez-Jimenez, Castro and Lopez-Miranda20). Others found no difference in effects on vWF, when comparing a MUFA diet with either a PUFA diet(Reference Turpeinen and Mutanen21) or a low-fat diet(Reference Thomsen, Rasmussen and Christiansen22). The significant between-diet effect (MUFA v. LF) observed in the present study seems to be due to (non-significant) differences in vWF baseline values. Also, we cannot exclude that the significantly higher body weight in the MUFA group may partly explain the less favourable vWF effect of the MUFA diet.
The two other markers of endothelial function, TFPI and ICAM, were not affected during 6 months by any of the three diets. Only a few dietary studies have measured TFPI, with either a decrease in TFPI concentrations after 4 weeks on a high-MUFA diet compared with a low-fat diet(Reference Perez-Jimenez, Castro and Lopez-Miranda20) or an increase in TFPI after 6 weeks on a diet high in marine n-3 fat v. a diet high in vegetable n-3 fat(Reference Goyens and Mensink23). A cross-sectional study observed an association between high adherence to a Mediterranean diet and lower concentrations of ICAM(Reference Fung, McCullough and Newby24). Concentrations of ICAM are not affected by α-linolenic acid compared with linoleic acid in dyslipaemic men(Reference Bemelmans, Lefrandt and Feskens11).
The most investigated inflammatory marker in dietary studies is CRP, which can be affected by various dietary components. In cross-sectional studies, low concentrations of CRP are associated with ingestion of a Mediterranean diet(Reference Fung, McCullough and Newby24–Reference Pitsavos, Panagiotakos and Tzima26), nuts and whole-grain food(Reference Jiang, Jacobs and Mayer-Davis27), and low-GI diets(Reference Liu, Manson and Buring28). In intervention studies based on dietary advice, CRP is lowered by a Mediterranean diet compared with a prudent diet in subjects with the metabolic syndrome(Reference Esposito, Marfella and Ciotola13), a low-GI diet v. a high-GI diet in patients with type 2 diabetes(Reference Wolever, Gibbs and Mehling15), a high-carbohydrate/low-fat diet compared with a low-carbohydrate/high-fat diet in overweight people(Reference Rankin and Turpyn29) and a low-carbohydrate/high-MUFA diet compared with a low-carbohydrate/high-protein diet in overweight people(Reference Keogh, Luscombe-Marsh and Noakes14). Randomised controlled trials have demonstrated that concentrations of CRP are lowered by almond-enriched high-MUFA diets compared with a healthy diet without nuts(Reference Rajaram, Connell and Sabate30), and by α-linolenic acid compared with linoleic acid in dyslipaemic men(Reference Bemelmans, Lefrandt and Feskens11–Reference Rallidis, Paschos and Liakos12). Thus, many studies have suggested that a high-MUFA diet has a favourable effect on CRP. In the present study, CRP was lowered by all three dietary regimens. Most probably, this indicates that the controlled study in itself had a healthy effect on the study participants, and that all three experimental diets were healthier than the habitual diets eaten by the overweight study participants. Alternatively, the reduction in CRP might be due to an acute-phase reaction in the beginning of the study caused by a stress situation (substantial negative energy balance in the low-energy diet period, getting used to the experimental design and diets, etc.). However, the participants completed a 3-week standardisation period (weight stabilisation on the control diet and adaptation to the supermarket model) before the start of the study. A decrease over time can also be caused by a seasonal variation, but there seems to be no variation in CRP concentrations(Reference Kelly31, Reference Rudnicka, Rumley and Lowe32). Whatever the reason for the decrease in CRP during the study period, the minor increase in body weight cannot counteract this effect, and there was no association between changes in BMI and changes in CRP (r 0·021, P = 0·85) in the present study and in another study(Reference Belza, Toubro and Stender33).
The dietary effect on CRP can be a direct effect of the experimental diets and/or reinforced by the observed reduction in IL-6, which can affect the hepatic synthesis of CRP(Reference Robson, Shephard and Kirsch34). In cross-sectional studies, low concentrations of IL-6 are associated with ingestion of a Mediterranean diet(Reference Fung, McCullough and Newby24, Reference Panagiotakos, Dimakopoulou and Katsouyanni25) and nuts and whole-grain food(Reference Jiang, Jacobs and Mayer-Davis27). Randomised controlled trials demonstrate that concentrations of IL-6 are lowered by high-MUFA oleic acid compared with tran-fatty acid or stearic acid in healthy men(Reference Baer, Judd and Clevidence10), and α-linolenic acid compared with linoleic acid in dyslipaemic men may either lower IL-6 concentrations(Reference Rallidis, Paschos and Liakos12) or has no effect on IL-6(Reference Bemelmans, Lefrandt and Feskens11). Also, concentrations of IL-6 are not affected by almond-enriched high-MUFA diets compared with a healthy diet without nuts(Reference Rajaram, Connell and Sabate30).
Thus, there seems to be no substantial difference between the three experimental diets (MUFA, LF and control) on the long-term effect on inflammation and endothelial cell function. Results from the same study showed that also several haemostatic variables (d-dimer, prothrombin fragment 1+2, factor VII coagulant activity and plasminogen activator inhibitor) were not affected by the three diets except for fibrinogen, which was significantly lowered by the LF diet and not by the MUFA diet, and this change over time was significantly different between the diet groups(Reference Bladbjerg, Larsen and Due35). In contrast, the MUFA diet had a more favourable effect on glucose homeostasis than the two other diets(Reference Due, Larsen and Hermansen19).
Important strengths of the present study include the randomised design, the long-term observation, the number of subjects and the highly controlled supermarket model providing complex ad libitum diets for free-living individuals. It is extremely difficult to standardise dietary studies and to completely control what people are eating, and only a few long-term controlled dietary studies exist. The present study therefore adds important information to our present knowledge. The selected risk markers were not among the primary effect variables in the power calculation (which was based on changes in body weight)(Reference Due, Larsen and Hermansen19), but highly significant differences were observed for CRP and IL-6, and there was not even a trend towards differences in ICAM and TFPI. We cannot exclude that we were unable to detect a true vWF difference between the MUFA diet and the LF diet due to a type 2 error, or due to the significantly higher body weight in the MUFA group. A limitation of the study is the minor weight regain in all three dietary groups, which makes comparison with isoenergetic dietary studies more difficult. However, the aim of the study was to compare the long-term effect of three dietary regimens on inflammation and endothelial cell function during weight maintenance in relatively young subjects. An older (and more atherosclerotic or insulin resistant) study population might have caused a greater difference in risk markers within and between the diets.
In conclusion, the MUFA diet was not superior to the LF diet with respect to long-term effects on inflammation and endothelial cell function in overweight subjects after weight loss. Only the LF diet tended to lower plasma vWF, but this did not result in significant different vWF changes between the diets. The MUFA diet and the LF diet had similar favourable long-term effects on IL-6, and all three diets lowered CRP. The reduction in CRP on the average Danish diet also indicates that following a controlled study in itself has a beneficial effect.
Acknowledgements
The authors wish to thank the project staff of the Department of Human Nutrition. The technicians Kathrine Overgaard and Anette Larsen are kindly thanked for analysing the blood samples. Also, special thanks to Professor Walter Willett, Department of Epidemiology and Nutrition, Harvard School of Public Health, Boston, MA, USA and David Ludwig MD, PhD, Department of Medicine, Children's Hospital, Boston, MA, USA for participating in the design of the project. The work was supported by the HA Foundation, the Danish Heart Association, the Danish Diabetes Association, Centre for Advanced Food Research, the State Research Councils, and the Danish Pork Council foundations, associations and research councils: www.mufobes.dk/?show = sponsorer. Foods in the supermarket and low-energy diets were sponsored by Nutrillett, the HA Foundation, KGT/DEG, the Danish Pork Council, Danisco FDB, Arla Foods, the Danish Heart Association, and LMC Rådighedsfond. Food sponsors were as follows: 3-Stjernet, Aarhus United, Allara, Ardo/Frigodan, Beauvais, Bæchs Conditori, Bähncke, Cadiso, Cerealia, Daloon, Danisco, FDB, Flensted, Frisko, G-kartofler, Gamba Food, Jan Import, Kellogg's, Kims, Kraft Foods, Kryta, Københavns Engros Grønttorv, Kødbranchens Fællesråd, LCH catering, Lykkeberg, Malaco Leaf, Nutana, Nutrillett, Odense Marcipan, Polar Is, Puratos, Rose Poultry, Rynkeby, Saeby, Santa Maria, Schulstad, Svansø, Sønderjysk Kål, Tholstrup Cheese, Toms, Tulip, Unilever, Urtekram and Wasa. Analyses of blood samples were supported by the Faculty of Health Sciences, the University of Southern Denmark. The authors' contributions were as follows: A. A., T. M. L. and A. D. were involved in the study concept and design; A. D. and T. M. L. were involved in the collection of the data; E.-M. B., J. J. and S. S. were involved in the blood analyses; E.-M. B. performed the statistical analysis; E.-M. B. and J. J. were involved in the interpretation of the data; E.-M. B. performed the drafting of the manuscript; E.-M. B., A. D., T. M. L., J. J., S. S. and A. A. contributed to the critical revision of the manuscript for important intellectual content; A. A., T. M. L. and A. D. were involved in the obtained funding; A. D., T. M. L., E.-M. B., J. J., S. S. and A. A. were involved in the administrative, technical or material support; A. A. was involved in the study supervision. No sponsor participated in the analysis or interpretation of the data, manuscript preparation, review or approval, or the decision to publish. The authors declare no conflicts of interest.





