Obsessive–compulsive disorder (OCD) is characterised by the presence of unwanted, intrusive obsessions (unpleasant thoughts, images or urges) and compulsions (repetitive behaviours which may be covert, e.g. mental counting). OCD in childhood and adolescence has benefitted from an explosion in research since the 1980s. Studies in the USA and the UK have demonstrated that OCD in young people can be managed with medication and, more recently, that cognitive–behavioural therapy (CBT) should be the first-choice treatment.
Epidemiology
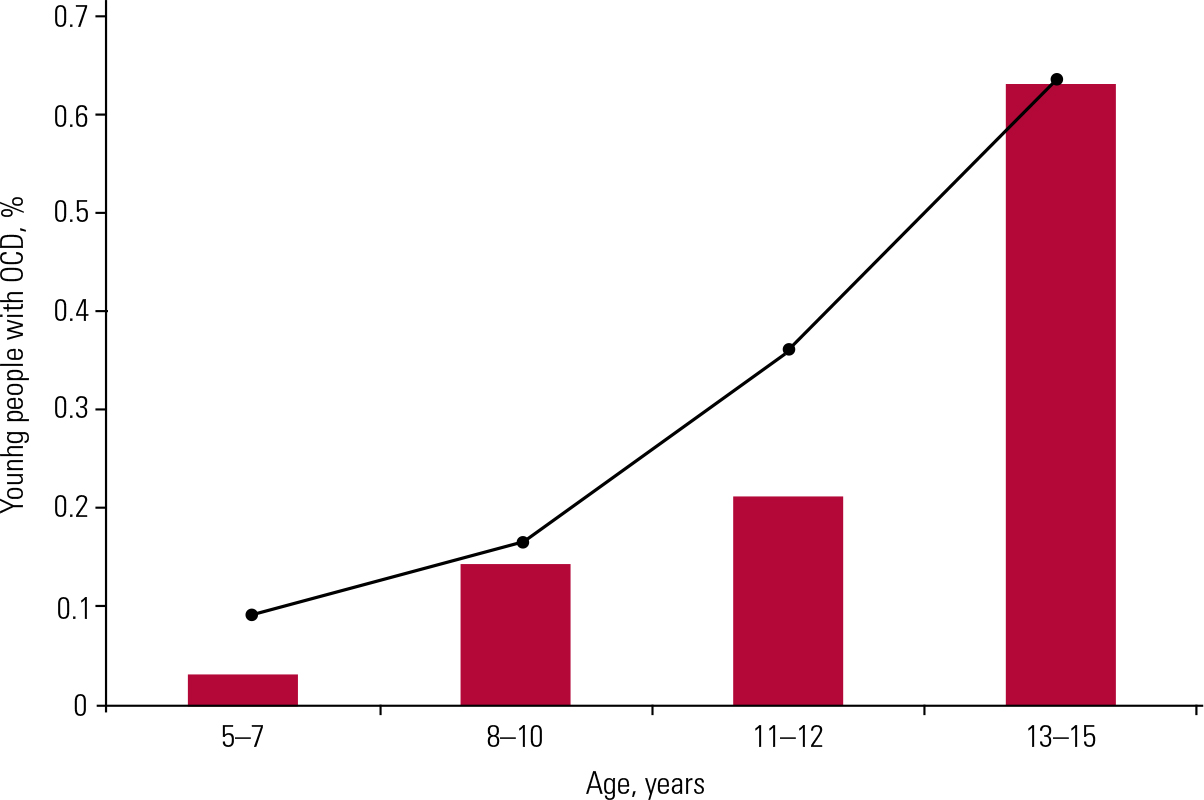
Reference Flessner, Freeman and SapytaFlament et al (1988) showed that about 1% of teen agers could be diagnosed as having OCD and that many young people were not being diagnosed because they did not seek help. Subsequent estimates found that OCD affects between 0.3 and 5.6% of 5- to 18-year-olds. The highest estimate was found in Israel among young armed forces recruits (Zohar 1992) and the lowest estimate in a representative sample of the UK population (Reference Keeley, Storch and MerloHeyman 2001). Reference Keeley, Storch and MerloHeyman et al (2001) also found that the prevalence varied with age (Fig. 1), increasing exponentially to the teenage years.
Estimated prevalence of obsessive–compulsive disorder (OCD) in young people at varying ages, together with best-fit exponential curve (after Reference Keeley, Storch and MerloHeyman 2001, with permission).
OCD in DSM-5
DSM-5 no longer subsumes OCD under the anxiety disorders category, but groups it with body dysmorphic disorder, trichotillomania, hoarding disorder, excoriation (skin-picking) disorder and other disorders (American Psychiatric Association 2013). This change was based on evidence that these disorders share some aspects of phenomenology, such as being motivated by escape from unpleasant feelings through repetitive behaviour. The category now requires a judgement about the degree of insight that the person shows: good/fair, poor or delusional/absent. Children and young people are not required to show egodystonicity, which is a difficult construct to convey to this age group. It is also important to note that it is possible to have either obsessions alone or compulsions alone, although in children pure obsessions are rare (Reference Turner, Mataix-Cols and LovellSwedo 1989). Clinicians should be aware that patients presenting with no overt compulsions may be using mental rituals to control their distressing feelings. Pure compulsions appear more common, perhaps because many children find it hard to identify the obsessions clearly.
In clinical practice it can be particularly hard to distinguish OCD from generalised anxiety disorder (GAD) (Reference Coughtrey, Shafran and LeeComer 2004). Examining the young person’s beliefs about the personal significance or meaning of their intrusive thoughts has been suggested as a useful strategy to help distinguish between these two diagnoses. In young people with autism spectrum disorder, it can also sometimes be challenging to differentiate the compulsions that characterise OCD from the repetitive behaviours of autism, which may be motivated by pleasure. Only careful enquiry and observation will show whether the repetitive behaviours are driven primarily by anxiety/distress or by enjoyment/pleasure.
Interventions and guidelines
The National Institute for Health and Care Excellence (NICE) guidance on the treatment of OCD explicitly includes young people (Reference O'Leary, Barrett and FjermestadNICE 2005). It recommends a stepped-care approach, starting with self-help materials and guidance provided by primary care professionals, progressing if necessary to CBT and then to medication. If a young person does not benefit from a single course of CBT, a selective serotonin reuptake inhibitor (SSRI), alternative SRRI or clomipramine can be considered in conjunction with CBT. A final stage involves various options for in-patient care, specialised living arrangements or adding clomipramine or an alternative SSRI to CBT.
In their guideline watch, an update on the 2007 American Psychiatric Association guidelines, Reference Lebowitz, Scharfstein and JonesKoran & Blair Simpson (2013) recommend that treatment should take place in the least restrictive setting for providing either CBT or medication (SSRIs). Combined treatment should be offered only when either treatment alone has proven ineffective. However, the guideline watch has no specific section on the treatment of children. The American Academy of Child and Adolescent Psychiatry (AACAP) does not make such clear recommendations in its Facts for Families series, stating only that: ‘Most children with OCD can be treated effectively with a combination of psychotherapy (especially cognitive and behavioral techniques) and certain medications for example, serotonin reuptake inhibitors (SSRI’s)’ (AACAP 2013).
Psychological therapies
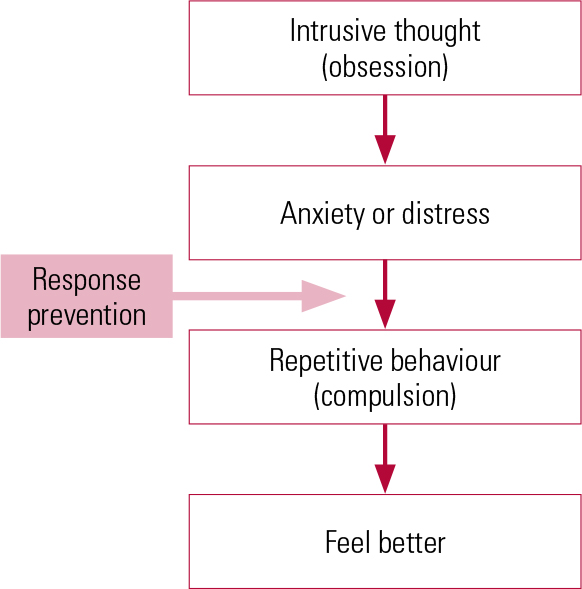
The most effective psychological therapies for OCD are based on learning theory. The idea behind their first use was straightforward: the rituals were being driven and reinforced by a reduction in discomfort caused by the obsession. Often, the obsession is expressed in the form of some type of physical harm coming to a person close to the patient, but it can be more nebulous, and some children are unable to articulate the discomfiting idea clearly. The behavioural treatment therefore consisted of trying to break the link between the reduction of discomfort and the compulsion by allowing the self to experience the anxiety and not perform the compulsion (Fig. 2). The procedure was therefore described as exposure and response prevention (ERP). Reference AbramowitzAbramovitz (1997) concluded that ERP was an effective intervention for adults, but until recently (Reference Storch, Geffken and MerloSkarphedinsson 2015) there was less evidence for its use in children.
Behavioural treatment of obsessive–compulsive disorder: response prevention aims to break the link between the emotional changes and the compulsions.
Cognitive–behavioural therapies
In the early 1980s, it became clear that many people with OCD were unable to use the techniques of ERP because they found them too unpleasant. In retrospect, this is unsurprising since a strict implementation of ERP requires the patient to put themselves in situations that they find aversive. At the same time, the cognitive bases of depression and panic disorder were identified by Reference Bolton and PerrinBeck (1979) and Reference Comer, Kendall and FranklinClark (1988) respectively. Emotions came to be seen as a consequence not of the event but of the interpretation of the event and its personal meaning. In panic attacks, normal physical symptoms that accompany anxiety were interpreted catastrophically, for example as indicating that a heart attack was imminent. For OCD, it had been demonstrated that unwanted intrusive thoughts were experienced widely (Reference RachmanRachman 1978) and cognitive theorists suggested that the interpretation of normal unwanted intrusive thoughts transformed them into obsessions (Reference SalkovskisSalkovskis 1985). In particular, it was proposed that the interpretation of such thoughts as indicating personal responsibility for harm was pivotal in causing and maintaining OCD. Personal responsibility is defined as ‘the belief that one has power which is pivotal to bring about or prevent subjectively crucial negative outcomes’ (Reference Sánchez-Meca, Rosa-Alcázar and Iniesta-SepúlvedaSalkovskis 1996: p. 111). Experimental data support the link with OCD. Reference Skarphedinsson, Hanssen-Bauer and Korn⊘rShafran (1997) showed that the presence of an experimenter could decrease the feeling of responsibility and hence the urges to neutralise it in adults with OCD. In a younger population, Reference Reynolds, Wilson and AustinReeves et al (2010) demonstrated that increasing responsibility led children without OCD to check their actions more, in a way that appeared similar to checking in OCD. Over time, cognitive theories have suggested that intrusive thoughts are transformed into obsessions when they are interpreted as having personal significance, particularly in terms of the person thinking that they are ‘mad, bad or dangerous’ (Reference RachmanRachman 1997).
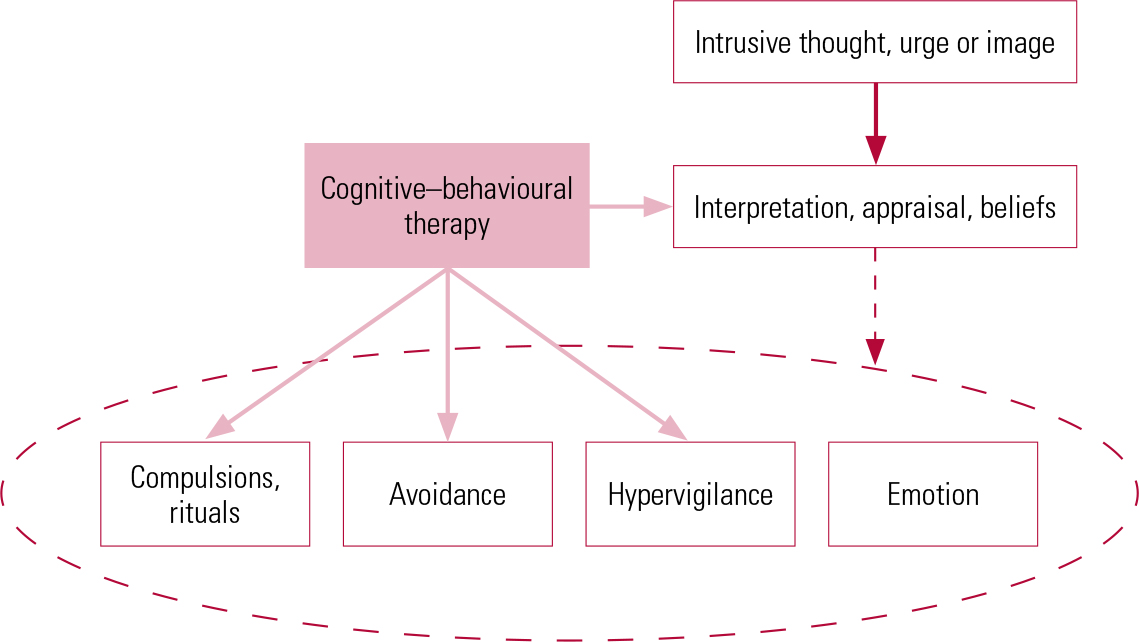
The cognitive model of OCD led to cognitive–behavioural interventions based on the premise that it is important to change both the patient’s misinterpretation of the meaning of their intrusive thoughts and the behavioural cycle in which compulsions and avoidance maintained anxiety and beliefs about danger (Fig. 3). The precise manner in which this is done varies. In the USA, a treatment manual for children described a CBT that used a narrative, externalising context and concentrated on behaviour change (Reference March, Foa and GammonMarch 1998), whereas in the UK, CBT has tended to concentrate on changing the appraisals of cognitions through behavioural experiments to test out beliefs (Reference Clark, Rachman and MaserBolton 2011; Reference Riddle, Scahill and KingReynolds 2013). Here we will focus on a cognitive approach to OCD, as this is an exciting area of development.
How cognitive–behavioural therapy affects obsessive–compulsive disorder. Note that, unlike exposure and response prevention, the treatment affects the cognitive aspects as well as the behaviour.
A cognitive approach
CBT depends on a thorough understanding of the patient’s experiences and thinking which may require the adoption of patients’ own vocabulary to describe the difficulties that they face. Young people with OCD will often not recognise the terms used by mental health professionals and instead of talking about anxiety or fear will describe horrible feelings, distress or discomfort. They may also be unable to access clear cognitions that drive the OCD, but accept the terminology ‘urge’ or ‘nasty feeling’. It is important that the therapist accepts the young person’s own words and uses them in subsequent sessions.
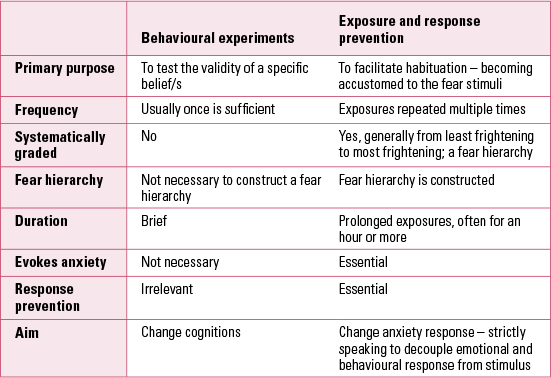
The term CBT has been used to describe a number of different protocols in OCD. They all seek to address the cognitive biases of the disorder, but they differ in the emphasis placed on cognitive techniques as compared with behavioural ones (primarily ERP). Table 1 outlines the differences between behavioural experiments as used in CBT and ERP. Guidelines often obscure the issue by describing a recommended treatment as cognitive therapy with exposure and response prevention, for example ‘CBT (including ERP)’ (Reference O'Leary, Barrett and FjermestadNICE 2005: p. 42). Most published treatment protocols also fail to distinguish between cognitive methods and ERP. Since there are no published trials involving young people that directly compare CBT with ERP, it is not possible to make clear recommendations, although a recent review on the efficacy of psychological treatments in adults addresses this issue (Reference Rachman and De SilvaPonniah 2013). Most published trials have adopted cognitive techniques often in conjunction with ERP, and we therefore focus on those here.
Differences between behavioural experiments and exposure and response prevention
The elements of CBT
The foundation for CBT is collaboration between the therapist as an expert in OCD and the patient as the expert in their own thinking and behaviour (Box 1). The therapist and patient may bring in other family members as and when their involvement in the maintenance cycles becomes apparent.
Key components of CBT
-
Initial formulation
-
Psychoeducation
-
Experiments to:
-
test beliefs
-
test emotional reactions
-
identify obstacles to change
-
Behavioural change
-
Generalisation
-
Relapse prevention – including stress inoculation and problem-solving
First, the therapist and the patient develop an initial formulation which evolves and forms the basis for the activities of treatment.
The next element is often educational, including informing patients about the prevalence of OCD in their age group and helping them to understand that OCD is not a form of psychosis (patients often say that they are afraid that they are ‘going mad’), explaining the nature of human thinking and that unwanted intrusive thoughts are almost universal. Each session is followed by between-session work (the term ‘homework’ can be used, but some young people find it unhelpful). Such work may include conducting surveys to find out the types of thinking experienced by siblings or peers who do not have OCD to establish the universal nature of unwanted intrusive thoughts.
The next stage is the use of behavioural experiments that examine the validity of the young person’s beliefs in such a way that they are able to realise that their feared event is unlikely to happen. Such a realisation enables them to let go of their compulsions and changes the interpretation of their obsessions. This contrasts with ERP, where the same ends are served by systematic graded exposure of the young person to a frightening event and not letting them carry out any compulsive activities.
The formulation
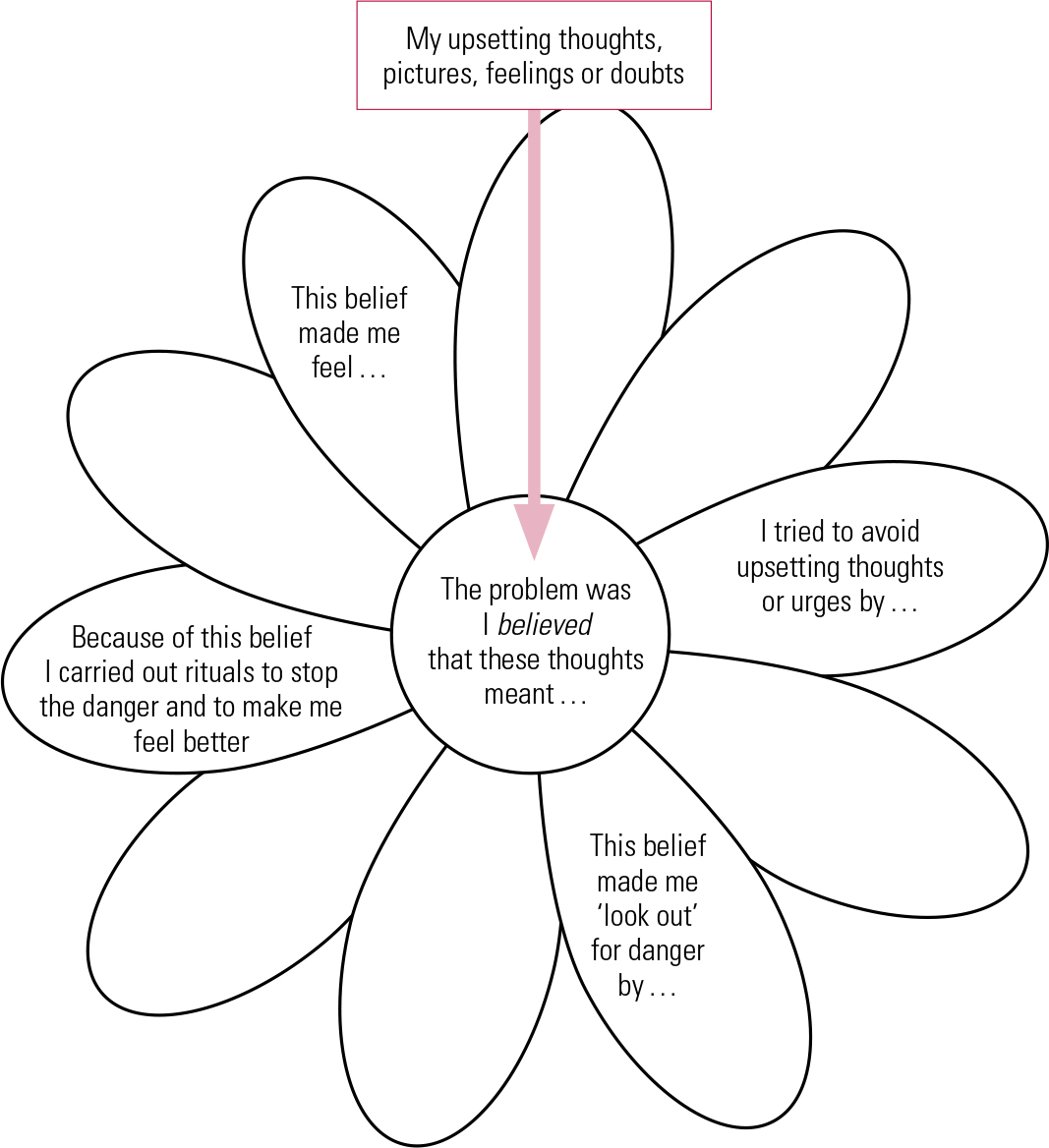
The formulation incorporates both historical information about the development of OCD and where it may have come from and the maintenance cycles. In our work we have used a diagram called the ‘vicious flower’ to illustrate maintenance cycles (Fig. 4).
Vicious flower to help in building a formulation. Each petal represents a cycle that maintains the problem. The arrow shows the connection between the intrusive thought and its interpretation or appraisal.
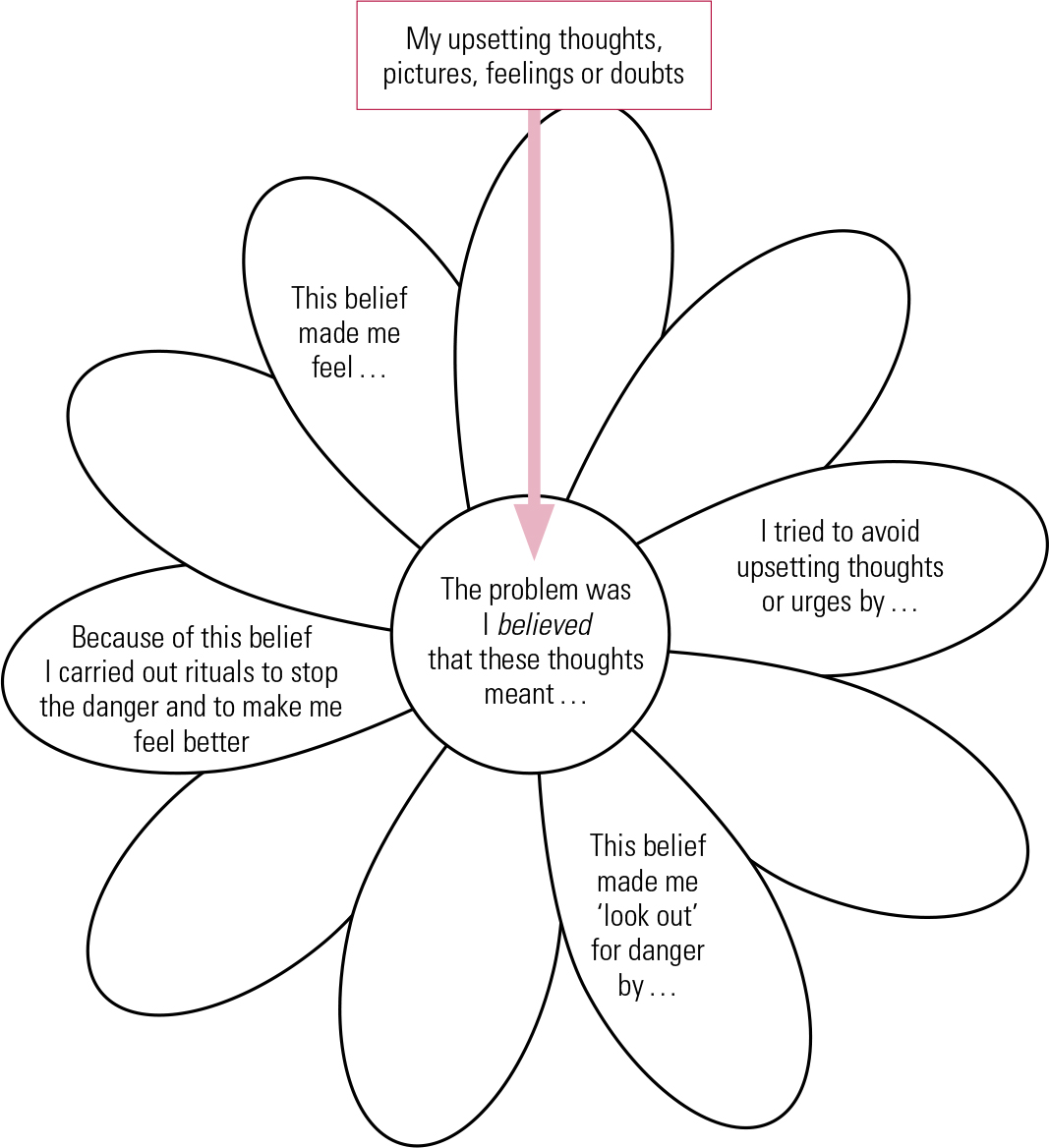
In general, we identify four maintenance cycles:
-
hypervigilance for threatening information
-
counterproductive repetitive behaviours that manage anxiety/distress but maintain preoccupation
-
emotional changes
-
avoidance.
CBT aims to identify all four and enable the patient to break the cycles by learning in a safe way that they are not needed. For this reason, the cognitive distortions seen in the formulation need to be altered so that the patient can change what they do and think.
Psychoeducation
Education about thinking is important because patients often do not understand that the brain is always producing thoughts, even those that are uncalled for (‘intrusive thoughts’), and that struggling against those thoughts is unhelpful. Nearly everyone has intrusive thoughts, which can be illustrated by the case of ‘earworms’ or catchy tunes that we cannot forget. Earworms are interesting intrusive thoughts since they are rarely troublesome (Reference BeckBeaman 2010). As a result, nearly every patient can tell the therapist what they do about earworms and how successful they are. It is also helpful to demonstrate failures of thought control. Understandably, people try to suppress intrusive thoughts, but these efforts are rarely met with success. This can be demonstrated in the therapy session by trying to suppress an image, for example a pink giraffe. The therapist may then explore with the patient the frequency of occurrence of obsessions through the day, thus demonstrating that the individual experiences fewer obsessions when they are busy, because their mind is occupied with other things. Conversely, when they are less occupied, for instance at bedtime, the OCD recurs more often.
The next phase is to help the patient understand anxiety and how it works. This involves understanding the short-lived nature of the surge in fear that results from a single frightening event (e.g. a balloon bursting unexpectedly). The rapid decline in anxiety following a single event is common to most people, so they are aware that they do not remain anxious indefinitely. Psychoeducation includes describing and drawing an anxiety curve, demonstrating that anxiety peaks after provocation, but has a natural course of decline consistent with adrenaline surges following a fear-inducing event. This is contrasted with the compulsions, which reduce the anxiety rapidly, thus reinforcing their use. At the same time it is helpful to get the patient to understand that they might interpret events differently depending on where they are. So, a bang in the night at home could be a burglar breaking in or it could be the cat knocking something over in the kitchen again. The matter of interpretation is important, because the theory makes clear that a major part of the problem in OCD is how the obsessive thoughts are interpreted.
Behavioural experiments
Each behavioural experiment should be accompanied by hypotheses or predictions about what might happen and why. In general we contrast two hypotheses: the OCD hypothesis and a non-OCD hypothesis. For instance, if the young person is concerned with contamination and the experiment is to eat a biscuit without washing their hands, the OCD hypothesis would be that they will become ill after eating the biscuit. The non-OCD hypothesis would be that they will initially be worried about becoming ill, but that the worry would decline.
Behavioural experiments in practice: cognitive error remediation
In this section we describe a few experiments that challenge thinking patterns that are common in OCD. For more experiments see, for example, Reference Williams, Salkovskis and ForresterWaite & Williams (2009) and Reference Fineberg and BrownDerisley et al (2008).
Thought–action fusion
One thinking error that occurs commonly is thought–action fusion. This has two components, one of which is the belief that thinking about a bad event happening to another person makes it more likely to happen. This is a particular form of magical thinking that is common in young people with OCD. It is often amenable to testing. For example, the young person can be asked to perform an experiment: to think about their mother having a minor accident (e.g. twisting her ankle) within a particular time period (e.g. before the next session) and seeing whether or not it happens. The subsequent experiment would build on this, with the young person thinking about a slightly more serious mishap occurring to their loved one and again seeing whether it happens. Ultimately, the experiments provide personally relevant information that the young person cannot cause harm to a loved one simply by thinking about it.
Responsibility
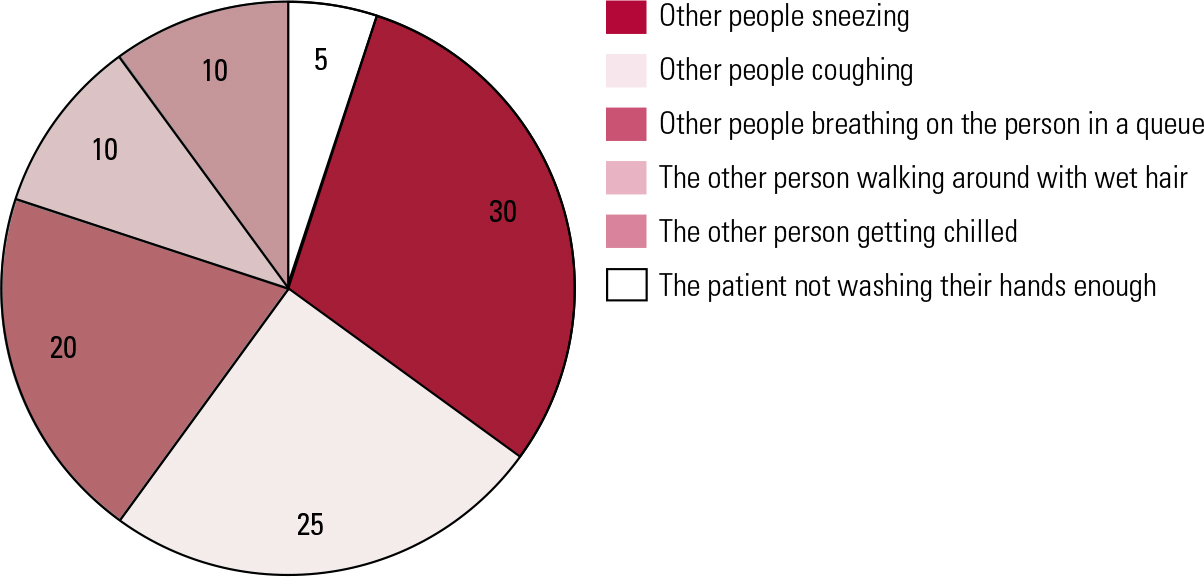
Another thinking error common in people with OCD is the belief that they alone are responsible for the prevention of harm. The method generally used to challenge this belief is the responsibility pie chart. The therapist uses a recent occasion when some type of harm has occurred, e.g. catching a cold. A person with OCD may believe that they failed to prevent someone they know from catching a cold. The therapist runs through the most likely ways the person caught their cold, starting with the most probable, such as exposure to the sneezes and coughs of others with colds, and estimates the likelihood of each cause being responsible (Fig. 5).
Responsibility pie chart showing that the patient’s hand-washing compulsion has a minor effect on the chances of another person catching a cold.
Black and white thinking
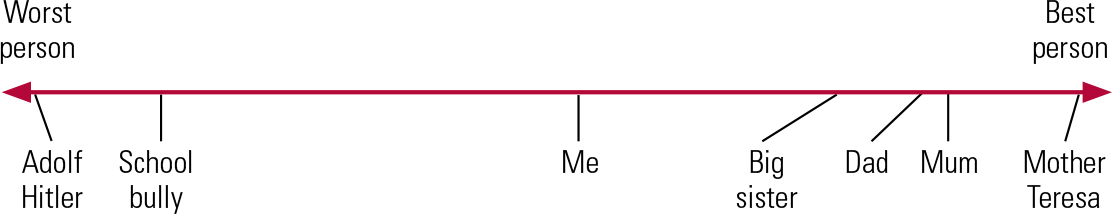
Sometimes people with OCD have particularly ‘black and white’ or ‘all-or-nothing’ thinking. For example, a young man might believe that he is a good person only if he has completely pure thoughts all the time. Any bad thoughts would mean that he was a bad person. So if he had unwanted sexual thoughts, he interpreted it to mean that he was a bad person. The therapist might explore this belief using a continuum diagram (Fig. 6), examining the types of thoughts that someone like Mother Teresa (an extremely good person) would have at one end, and the thoughts that characterised Hitler (an extremely bad person). Other people, such as the young man’s parents, sister and the school bully, can also be placed along the continuum and the sorts of thoughts they might have can be discussed. This can shift the young man’s belief that occasional sexual thoughts make him as bad a person as Hitler.
Continuum diagram illustrating how reference to end points can make self-evaluation more realistic.
Perfectionism and uncertainty
Often young people with OCD believe that they must do things perfectly to avoid disasters. A typical example would be the need for homework to have no crossings out in it. The obvious experiment is to submit to the teacher a piece of homework with a deliberate crossing out in it. It is important to consider predictions from both an OCD view and non-OCD view. For this example, the OCD prediction might be that the homework will be returned to the young person for her to do it again and again until it is perfect. The alternative (non-OCD) prediction would be that the teacher is unlikely to notice anything, but that the young person would be very anxious for a while after handing the work in and anxious again on its return. A cooperative youngster might even complete a record of her feelings every 10 minutes following the handing in.
Encouraging the patient’s participation
Part of the art of the expert CBT therapist is to enable the young person to see that change is possible by helping them do the experiments. One way of making this easier is for the therapist to demonstrate the experiment themselves before asking the patient to do it too. This might be eating a biscuit without first washing your hands. It is important that the difficulty of the experiment is agreed together with the patient, so that it can be achieved and also provide meaningful information about the validity of the patient’s fears.
Generalisation and relapse prevention
CBT will always include homework to be done between sessions. It is conventional for parents to be asked to ensure that this is completed. Certainly, if the parents have knowledge of the techniques of CBT they are better placed to ensure that behavioural experiments are carried out. In one trial, there were explicit instructions for the therapist to ensure that the young person took ownership of their own treatment by working through stages: therapist-generated experiments on which the child reported; child-generated experiments on which the child reported; child-generated experiments with no reporting (Reference Clark, Rachman and MaserBolton 2011). At the end, if the child is successfully engaged in treatment, they will have learned enough techniques to manage their own OCD without recourse to the therapist’s advice.
A number of techniques can be used for relapse prevention. For example, reminders to use the hand-outs and diaries from the active phase of therapy can be written on sticky notes that the young person keeps in their bedroom or can be stored electronically somewhere secure (e.g. using cloud computing). The choice of techniques will be driven by the young person and their parents.
Evidence for cognitive and behavioural therapies
The first randomised controlled trial of behavioural therapy for OCD in young people was that of Reference Derisley, Heyman and Robinsonde Haan et al (1998), who compared it with drug treatment (clomipramine). They concluded that the approach ‘produced stronger therapeutic changes than clomipramine’. Subsequently, evidence has accumulated that CBT or behavioural therapy reduces symptom severity in OCD more than being on a treatment waiting list (Reference March and MulleManassis 2010), although comparisons with pharmacological treatments have proved less easy to interpret. The difficulties may result from site effects such as the site-specific variations in treatment outcome reported by Reference March, Klee and KremerMarch et al (2004) in the Pediatric Obsessive–Compulsive Disorder Treatment Study (POTS), further confounded by different nation-specific referral patterns. The limited long-term evidence suggests that patients successfully treated with CBT remain diagnosis free for at least 7 years (O’Leary 2009).
In the UK, two pilot trials established the efficacy of CBT for young people in out-patient settings (Reference Bolton, Williams and PerrinBolton 2008; Reference Zohar, Ratzoni and PaulsWilliams 2010). More recently, a study compared a short form of CBT (an average of 5 sessions) with the standard 12-session form and found them to be equally effective (Reference Clark, Rachman and MaserBolton 2011). Two further trials have established that the benefits of CBT do not depend on delivery method (telephone v. face to face) (Reference Volz and HeymanTurner 2014) or presence/absence of parent during treatment (Reference Riddle, Scahill and KingReynolds 2013). The latter finding is somewhat surprising considering the role that parents are considered to play in childhood anxiety disorders. Finally, the utility of CBT has recently been shown with children as young as 4 years of age (Reference Heyman, Fombonne and SimmonsFreeman 2014), thus extending the age range.
Pharmacological therapies
Reference Fitzgerald, Stewart and TawileFineberg & Brown (2011) reviewed the literature on pharmacotherapies for young people with OCD. In brief, treatment with clomipramine seems to be an effective option, but its side-effects mean that it is poorly tolerated (Reference Manassis, Russell and NewtonLeonard 1989). SSRIs such as fluvoxamine (Reference SalkovskisRiddle 2001), fluoxetine (Reference Riddle, Reeve and Yaryura-TobiasRiddle 1992) and sertraline (Reference March, Klee and KremerMarch 2004) have all shown promise in randomised controlled trials. March et al (2006) suggested that sertraline showed the best profile. However, as mentioned earlier, the results showed a remarkable variability in effect sizes between sites, which suggests that the utility of sertraline may be overstated. The British National Formulary for Children (Reference Ponniah, Magiati and HollonPaediatric Formulary Committee 2014)) recommends only two SSRIs for OCD, fluvoxamine and sertraline. In the UK, the Medicines and Healthcare Products Regulatory Agency (2014) has advised that ‘Information from clinical trials has shown an increased risk of suicidal behaviour in adults aged less than 25 years with psychiatric conditions who were treated with an antidepressant’.
Other drugs, such as atypical antipsychotics, have been proposed as useful adjuncts to SSRIs (Reference Flament, Whitaker and RapoportFitzgerald 1999). In addition, D-cycloserine has been trialled, with promising preliminary results (Reference Swedo, Rapoport and RapoportStorch 2010).
Future prospects
Although CBT often substantially reduces the level of symptoms in OCD, a significant proportion of patients – as many as one-third (Reference Clark, Rachman and MaserBolton 2011) – do not show return of OCD symptoms to a nonclinical level. The benefits of medication are often lost when it is discontinued. This suggests that the understanding of how best to treat OCD is still limited. In the past few years, a number of promising lines of research have developed that give hope that outcomes will improve.
Research findings in two key areas are driving change in treatment methods. First, there is evidence that parental anxiety may adversely affect treatment response, as Reference Koran and Blair SimpsonKeeley et al (2008) found in relation to family interactions to OCD symptoms. Similarly, Reference Freeman, Sapyta and GarciaFlessner et al (2011) showed that parental anxiety is associated with more accommodation to rituals and more reassurance-seeking. Second is further understanding of how families manage or accommodate the symptoms of OCD. Reference Leonard, Swedo and RapoportLebowitz et al (2014) identified two types of family accommodation to OCD in young people: direct and indirect. Direct accommodation is when family members complete aspects of the child’s rituals. Indirect accommodation is when they try to avoid provoking compulsions or obsessions. Family accommodation may reduce the effectiveness of CBT by preventing the child from engaging in experiments at home to test beliefs (Reference Storch, Murphy and GoodmanStorch 2007).
Family-based CBT
The evidence for the benefits of family involvement in CBT itself are equivocal. Reference Barrett, Healy-Farrell and MarchBarrett et al (2004) found that treating OCD with family-based CBT was effective, possibly more than individual CBT, but Reference Riddle, Scahill and KingReynolds et al (2013) found that the presence of a parent in sessions had no effect. Although surprising, it is the Barrett trial that is the outlier in terms of effect size in both OCD and in other anxiety disorder trials for young people (Reference Reynolds, Clark and SmithReynolds 2012).
Bias-specific CBT
Contamination obsessions
Improving CBT requires better understanding of the cognitive biases in OCD, particularly those associated with different types of OCD. Reference Radomsky, Shafran and CoughtreyRachman (2004) has suggested that contamination fears may require a specific approach. Contamination itself may also be subdivided by phenomenology into mental and physical. Physical or ‘contact’ contamination can be driven by fear of disease, harmful substances or dirt. ‘Mental contamination’ occurs in the absence of physical contact, but leaves the person feeling dirty and polluted. Often the source of the contamination in mental contamination is human (e.g. the person’s own thoughts) and, unlike contact contamination, the person is uniquely vulnerable to the contaminant. This form of contamination includes ‘morphing’ or ‘transformation obsessions’, in which the young person fears that they may assume the undesirable characteristics of another person (Reference Waite and WilliamsVolz 2007).
Recent research (e.g. Reference de Haan, Hoogduin and BuitelaarCoughtrey 2014) has shown that people who are fearful of contamination are much more likely to report contamination by remote connections (distant contact). For example, one young person was afraid that they might lose their intelligence if they walked past a homeless person begging in the street, so she would cross the road and want to wash her hands to prevent this happening. Reference Coughtrey, Shafran and RachmanCoughtrey et al (2013) have suggested that CBT for mental contamination should include gathering information about perceived sources of contamination, obtaining a detailed history of events leading to the development of contamination obsession, considering physical and psychological betrayals, identifying beliefs about mental contamination and its spread, and detailing any mental imagery that might cause the patient to feel contaminated. This enables therapist and patient to build up a personalised formulation of the problems before embarking on a treatment protocol that varies from the standard CBT by including an emphasis on psychoeducation about the mental contamination and correctly labelling mood states.
Obsessive checking
If contamination fears require specific tailoring of CBT protocols, then it may be that other types of OCD, such as checking, also require a tailored approach. For instance, it is possible that checking is driven by an inappropriate over-monitoring of memory, resulting in memory distrust (Reference Reeves, Reynolds and CokerRadomsky 2010). The finding that repeated checking causes memory distrust is robust in adults, but has not been studied in young people. Nevertheless, it may be useful to bear in mind the recommendation by Radomsky and colleagues that therapy should include a behavioural experiment in which patients receive personalised information about the impact of repeated checking on memory confidence.
Scrupulosity
Reference Abramowitz and JacobyAbramovitz & Jacoby (2014) have described a formulation for scrupulosity (religious obsessions and ritual-focused OCD) that suggests that intolerance of uncertainty plays a central role. They propose that treatment should include experiments to demonstrate that it is possible to tolerate uncertainty rather than expending significant amounts of effort in ensuring certainty. This is not the same as learning that anxiety or distress will subside if one ignores an obsessive thought.
Conclusions
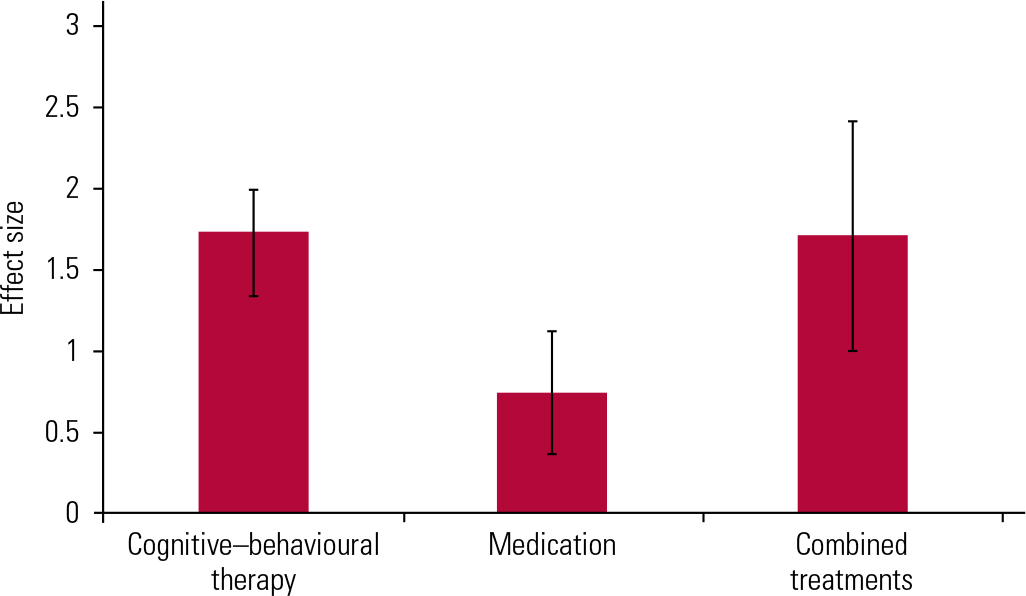
In young people, psychological treatments for OCD, in particular CBT, are arguably more effective than pharmacological treatments (Fig. 7) (Reference ShafranSánchez-Meca 2014). Interventions include learning about the nature of intrusive thoughts, exposure to worrying or disturbing thoughts (obsessions) and finding out how the cycles of behaviour and emotions cause the repetitive behaviours (compulsions) to persist. Experimenting with different ways of reacting to the obsessions enables patients to find alternative ways of managing distressing ideas. Young people taking part in cognitive–behavioural interventions find that this knowledge enables them to overcome their OCD to a large extent.
Effect sizes of different treatment options for obsessive–compulsive disorder in children (data from Reference ShafranSànchez-Meca 2014).
Developments in psychological treatment are likely to come from greater understanding of the particular aspects of cognition that are involved in different types of compulsive behaviour. There are already indications that washing and its associated contamination fears are linked to unusual understanding of how contamination spreads. Similarly, checking may be linked to problems satisfactorily monitoring one’s own behaviour, and religion-focused OCD (scrupulosity) may be motivated by an intolerance of uncertainty. In its turn, greater understanding of particular cognitive errors leads to improved psychological treatment. Developments in drug treatment should similarly arise from greater understanding of brain pathways that are changed by OCD. However, the greater challenge is to find a pharmacological intervention that has an enduring effect instead of requiring ongoing medication.
MCQs
Select the single best option for each question stem
-
1 DSM-5 classifies OCD as a type of:
-
a anxiety disorder
-
b psychotic disorder
-
c emotional disorder
-
d repetitive behaviour disorder
-
e impulse control disorder.
-
-
2 The initial treatment for OCD in young people recommended by NICE:
-
a relaxation
-
b psychodynamic psychotherapy
-
c self-help
-
d medication
-
e cognitive–behavioural therapy.
-
-
3 In CBT for OCD:
-
a the therapist listens to what the young person says and interprets it in terms of relationships
-
b the therapist instructs the young person on how to overcome their OCD
-
c the therapist and the young person discuss strategies for living with OCD
-
d the young person and the therapist work together to discover how the OCD works
-
e none of the above.
-
-
4 During the course of CBT, the young person:
-
a is encouraged to face up to their fears and not back down, no matter how difficult it is
-
b learns that their intrusive thoughts do not reflect reality (predict the future)
-
c does experiments to discover how their OCD works
-
d discusses the reasons why they have developed OCD
-
e expresses their feelings repeatedly.
-
-
5 Experiments are used in CBT to:
-
a change behavior
-
b change thinking patterns
-
c find out how the world works, so as to change thinking patterns and behavior
-
d test scientific hypotheses
-
e achieve all of the above.
-
MCQ answers
| 1 | d | 2 | c | 3 | d | 4 | c | 5 | c |









eLetters
No eLetters have been published for this article.