Neurosarcoidosis is an uncommon initial manifestation of sarcoidosis, representing only 2%–10% of initial presentations.Reference Westendorp, van de Beek and Brouwer1 Due to both the difficulty of obtaining adequate tissue and the lack of reliable biomarkers, including imaging findings, it is often challenging to diagnose.Reference Westendorp, van de Beek and Brouwer1 Given these diagnostic challenges, the recognition of specific clinical and paraclinical features remains useful in the recognition of this disease entity.
We present a case of a 63-year-old man with three months of progressive, bilateral leg weakness culminating in his inability to ambulate. His examination revealed Medical Research Council grade 3 and 2 strength in right and left hip flexors, respectively, grade 3 strength bilaterally in hip extensors, grade 4 strength bilaterally in knee flexion and extension and grade 5 bilaterally in dorsiflexion and plantarflexion. He was areflexic in the lower extremities with upgoing plantars bilaterally. He had anesthesia to pain and temperature up to the T4 spinal level. No involvement of other organ systems was suspected based on review of systems. CSF total protein was 747 mg/L (normal 150–450), and the white blood cell count was 9 (normal 0–5), all lymphocytes, with an elevated CD4+/CD8+ ratio of 7.6. CSF and serum angiotensin-converting enzyme were negative. MRI spine revealed a longitudinally extensive transverse myelitis from T2 to T9 (Figure 1A), with three consecutive levels of ventral-subpial disc-level enhancement from T4 to T7 (Figure 1B–1C). This enhancement was intermittently full thickness, and where only partial thickness, a reverse trident signReference Jaafari, Newman, Flanagan, Lopez-Chiriboga and Irani2 was noted (Figure 1D–1G). No nerve root enhancement was seen. Electromyography and nerve conduction studies confirmed the presence of lumbosacral polyradiculopathy. Brain MRI was normal. Chest CT revealed hilar lymphadenopathy. Supraclavicular lymph node biopsy confirmed the presence of noncaseating granulomas (Figure 1H). The patient was diagnosed with probable neurosarcoidosis as per the 2018 Neurosarcoidosis Consortium Consensus guidelines.Reference Stern, Royal and Gefland3 He demonstrated rapid clinical response to pulse steroids, regaining his ability to weight bear and his lower limb reflexes within several days. He continues to improve on methotrexate with regular outpatient follow-up and is now ambulating independently. Repeat imaging at three months (Figure 2A–2C) shows marked improvement of edema and reduced enhancement.

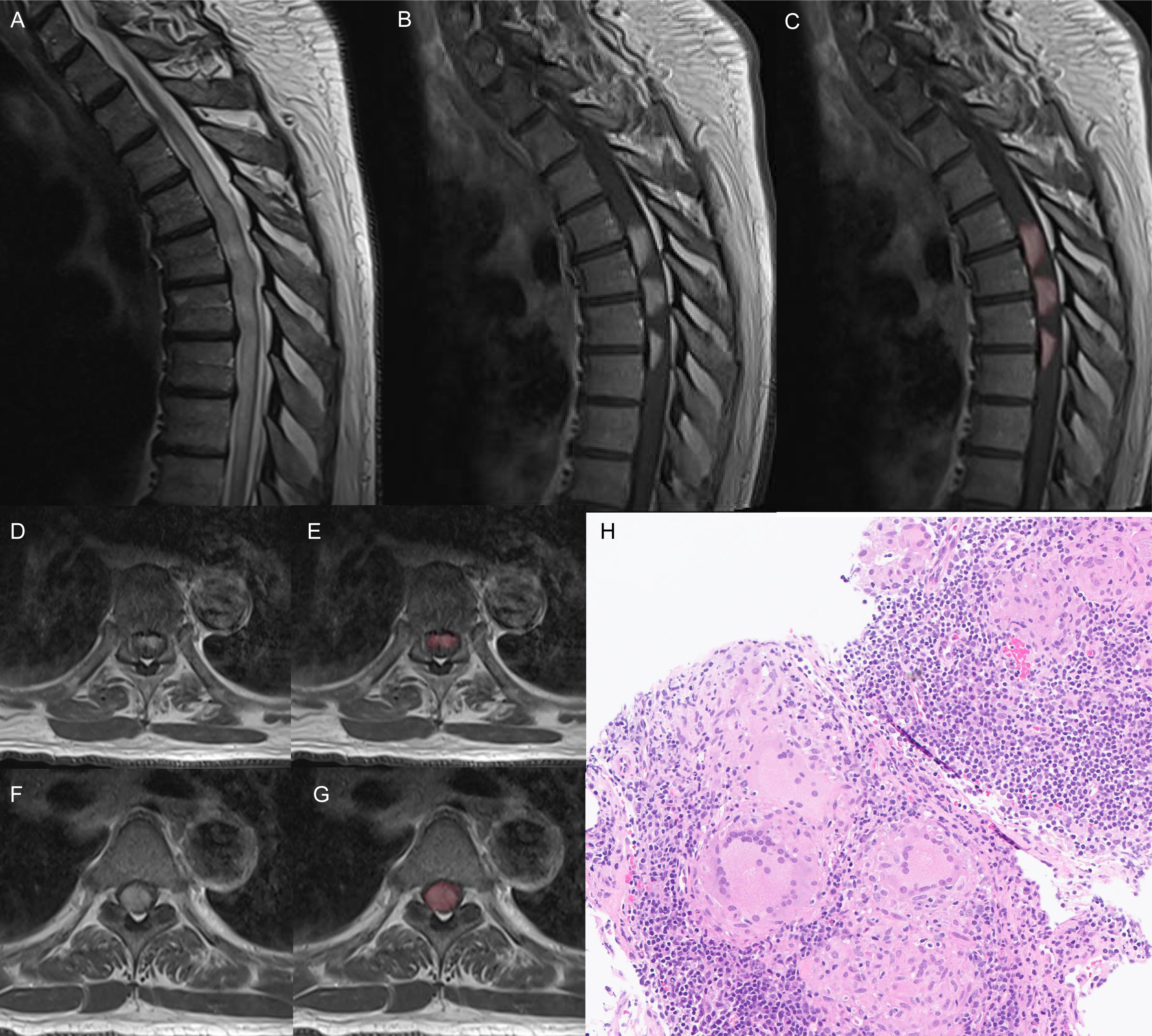
Figure 1. Patient imaging and pathology during initial presentation. (A) Sagittal, T2-weighted sequence: longitudinally extensive transverse myelitis from T2–T9. (B) Sagittal T1-weighted post-contrast sequence: three consecutive levels of ventral-subpial enhancement, centered at the intervertebral disc. (C) Annotation of (B) indicating areas of enhancement. (D) Axial T1-weighted post-contrast sequence: reverse trident sign at the T6–T7 disc level. (E) Annotation of (D) indicating area of enhancement. (F) Axial T1-weighted post-contrast sequence: full-thickness cord involvement at the T5–T6 disc level. (G) Annotation of (F) indicating area of enhancement. (H) Pathology of supraclavicular node biopsy showing noncaseating granulomas.

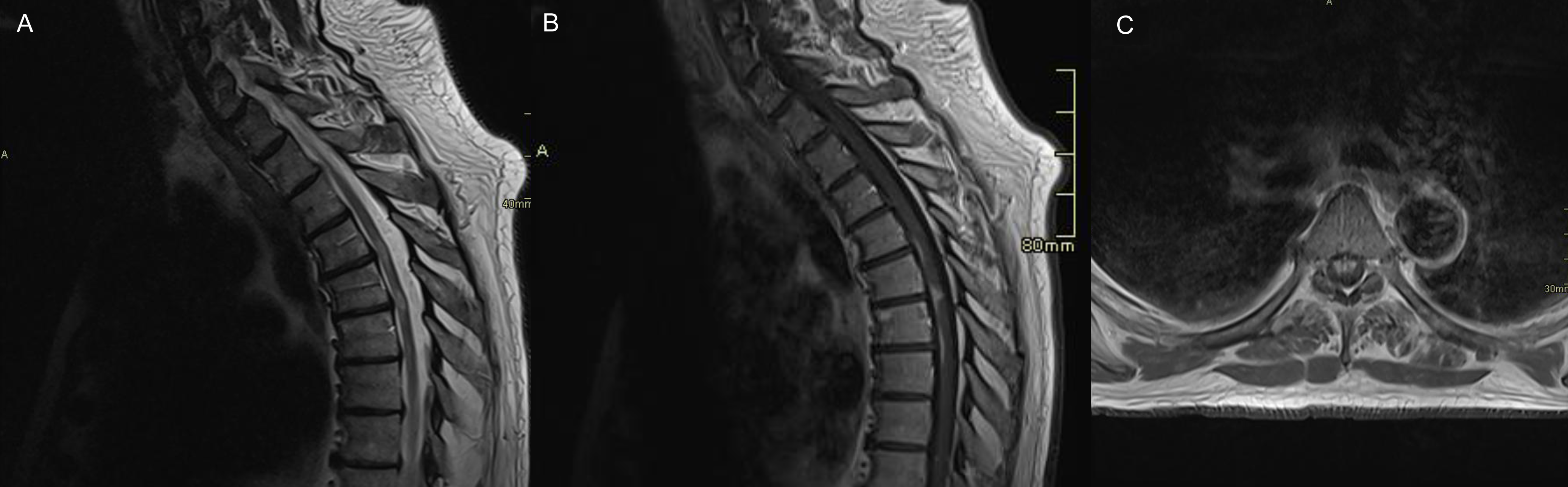
Figure 2. Three-month follow-up MRI findings. (A) Sagittal, T2-weighted sequence showing improvement of the expansile longitudinally extensive transverse myelitis seen in 1A. (B) Sagittal T1-weighted post-contrast sequence showing improvement of the previously noted “stegosaurus sign” in 1B. (C) Residual partial-thickness cord involvement at the T5–T6 level improved from full thickness seen in 1F.
Myeloradiculopathy is a relatively uncommon presentation of neurosarcoidosis, with myelitis accounting for between 5% and 26% of casesReference Bradshaw, Pawate, Koth, Cho and Gefland4 and radiculopathy accounting for about 5%.Reference Westendorp, van de Beek and Brouwer1 The highly variable presentations seen even within specifically neurosarcoid myelitisReference Nolte, ten Dam, van de Beek and Brouwer5 can make diagnosis challenging and make documentation of atypical and novel radiographic presentations particularly important. Ventral partial-thickness and consecutive enhancement have been reported only once and appeared phenotypically different, without a reverse trident or full-thickness enhancement.Reference Boban and Thurnher6 The striking pattern of full-thickness segmental enhancement centered at the levels of consecutive discs, which we have termed the “stegosaurus sign,” is a novel radiographic finding of neurosarcoid myelopathy.
Acknowledgments
We would like to thank the patient involved in this case for permitting us to publish his images and share his clinical course.
Author contributions
All authors were involved in the care of this patient. MB, LL, HK and JM were involved in conceptualization. JM was involved in writing. All authors reviewed and edited the manuscript and provided final approval.
Funding statement
The authors report no funding for this manuscript.
Competing interests
The authors report no disclosures.