1. Introduction
Involuntary admission (IA) fundamentally compromises a person’s right to autonomy and self-determination. In patients, it can cause self-stigma [Reference Ruesch, Mueller, Lay, Corrigan, Zahn and Schoenenberger1] and avoidance of psychiatry [Reference Swartz, Swanson and Hannon2]. IA is also challenging for the clinicians who execute it, as well as for those who are responsible for the ensuing inpatient treatment: Especially the latter have to offer treatment options [Reference Zinkler and Priebe3, Reference Lay, Salize, Dressing, Ruesch, Schoenenberger and Buehlmann4] and establish a sound therapeutic relationship [Reference McCabe and Priebe5].
As it restricts patients` freedom, IA is legally regulated in most countries [Reference Salize and Dressing6, Reference Dressing and Salize7]. In Switzerland, a federal republic of 26 cantons (states), IA is regulated at the national and cantonal level by the federal civil code [8]. In 2013, the legislation was revised with the aim to comply with international objectives to reduce coercive measures in psychiatry and to enhance patient autonomy [Reference Swanson, Swartz, Elbogen, Van Dorn, Wagner and Moser9, Reference Curran10]. Despite these international efforts to strengthen patient autonomy, several countries have reported increasing numbers of IA and other coercive measures [Reference Gilhooley and Kelly11], forensic placements and supported housing [Reference Priebe, Badesconyi, Fioritti, Hansson, Kilian and Torres-Gonzales12] over the last years. As factors explaining this development, the reduction of psychiatric beds, selective media coverage of tragic incidents caused by people with a mental disorder, and an increased desire for security in society have been discussed [Reference Gilhooley and Kelly11, Reference Schomerus, Stolzenburg, Bauch, Speerforck, Janowitz and Angermeyer13, Reference Von Heydendorff, Meyer-Lindenberg and Dressing14].
Importantly, there are not only differences in the rates of IA between countries [Reference Salize and Dressing6, Reference Riecher-Roessler and Roessler15], but also between regions of the same country or state i.e. between regions with comparable legal regulations. This finding underlines that besides clinical parameters [16–Reference Lay, Nordt and Roessler18], non-medical factors like cultural beliefs, attitudes, and societal values have an important impact on the decision-making process for or against the execution of IA [19–Reference Steinert, Lepping, Bernhardsgruetter, Conca, Hatling and Janssen22].
With a view to explaining these differences and ultimately to reduce coercion, previous studies have aimed to characterize risk factors for IA. From a clinical perspective, psychotic disorders [Reference Salize and Dressing6, Reference Lay, Nordt and Roessler18, 23–Reference Silva, Golay and Morandi27], organic mental disorders or mental retardation [Reference Lay, Nordt and Roessler18, Reference Silva, Golay and Morandi27], personality disorders [Reference Lay, Nordt and Roessler18], substance use disorders [Reference Lay, Nordt and Roessler18], manic disorders [Reference Silva, Golay and Morandi27], suicidal behavior [Reference Balducci, Bernardini, Pauselli, Tortorella and Compton23], danger to others [Reference Salize and Dressing6, Reference Hustoft, Larsen, Auestad, Joa, Johannessen and Ruud28, Reference Gou, Zhou, Xiang, Zhu, Correll and Ungvari29], impulsive behavior [Reference Balducci, Bernardini, Pauselli, Tortorella and Compton23, Reference Silva, Golay and Morandi27] and poor so called insight into illness [Reference Gou, Zhou, Xiang, Zhu, Correll and Ungvari29] were found to be risk factors for IA. Also socio-demographic factors like higher age [Reference Silva, Golay and Morandi27], male gender [Reference Curley, Agada, Emechebe, Anamdi, Ng and Duffy17, Reference Riecher, Roessler, Loeffler and Faetkenheuer25, Reference Hustoft, Larsen, Auestad, Joa, Johannessen and Ruud28], but also female gender [Reference Eytan, Chatton, Safran and Khazaal26, Reference Gou, Zhou, Xiang, Zhu, Correll and Ungvari29, Reference Chang, Ferreira, Ferreira and Hirata30], not living in an own house [Reference Lay, Nordt and Roessler18, Reference Riecher, Roessler, Loeffler and Faetkenheuer25, Reference Hustoft, Larsen, Auestad, Joa, Johannessen and Ruud28] and being a foreign national [Reference Curley, Agada, Emechebe, Anamdi, Ng and Duffy17, Reference Lay, Nordt and Roessler18, Reference Hustoft, Larsen, Auestad, Joa, Johannessen and Ruud28] have been found to increase the risk for IA. Regarding procedural aspects, no medication prior to admission [Reference Balducci, Bernardini, Pauselli, Tortorella and Compton23], previous IA [Reference Silva, Golay and Morandi27, Reference Montemagni, Bada, Castagna, Frieri, Rocca and Scalese31, Reference Van der Post, Peen, Visch, Mulder, Beekman and Dekker32] and dissatisfaction with previous mental health care [Reference Van der Post, Peen, Visch, Mulder, Beekman and Dekker32] have been described as risk factors. Furthermore, "area-level" factors, such as socio-economic deprivation [Reference Bindman, Tighe, Thornicroft and Leese33] and urban settings [Reference Keown, McBride, Twigg, Crepaz-Keay, Cyhlarova and Parsons34] were positively associated with IA. One study found that the characteristics of involuntarily admitted patients differed over time in some regions [Reference Mulder, Uitenbroek, Broer, Lendemeijer and Van Veldhuizen35].
Based on these - partly inconsistent - findings, it is not possible to generalize the risk factors for IA. In Switzerland specifically, to our knowledge, only one study analyzed patients` risk factors for IA after revision of the legislation in 2013 [Reference Silva, Golay and Morandi27] and no study so far has examined the revision`s effect on the risk for being involuntarily admitted.
This study therefore aimed to identify clinical and socio-demographic patient characteristics associated with IA in Switzerland. Furthermore, we aimed to analyze if the new legislation had an effect on the risk to being involuntarily admitted.
2. Methods
2.1. Setting
The study was set at the University Hospital of Psychiatry Zurich, Switzerland. The hospital has a public service obligation and provides mental health services for a large variety of psychiatric patients.
2.2. Legislation in Switzerland before and after 2013
In Switzerland, the execution of IA has been legally regulated since 1912. Minor revisions to the legislation were made in 1981 [Reference Schweizerische Eidgenossenschaft36]. This legislation stipulated that a person suffering from a state of weakness (e.g. mental disorder, alcoholism) and the risk of self-harm could be involuntarily admitted to an appropriate institution by a physician or the guardianship authorities [Reference Schweizerische Eidgenossenschaft36].
On January 1 st 2013, the new Swiss civil code was implemented [8]. Whilst aiming to reduce stigmatization and increase patient autonomy, the new legislation stipulates that “a person suffering from a mental disorder or mental disability or serious neglect (…) may be committed to an appropriate institution if the required treatment or care cannot be provided otherwise.” (Art. 426) [8]. Similar to the old legislation, it is stipulated that “the burden the patient places on family members and third parties and their protection must be taken into account” (Art. 426), and that the patient has the right to appeal for discharge at any time. The new legislation also explicitly mentions that the patient has to be informed about this right, as well as about the process following the IA and the possibility to inform/include a next of kin (Art. 430) [8].
Like the old legislation, the new legislation is executed on a regional level and procedural aspects differ between the 26 cantons (states) of Switzerland (Art.429). In Zurich, the child and adult protection services, as well as physicians holding a license to practice independently and those who work under their supervision, are allowed to execute IAs. The maximum duration of an IA is 42 days [Reference Kantonsrat Zuerich37].
2.3. Study sample
We screened a comprehensive cohort of all patients admitted for inpatient treatment between 2008 and 2016. We included all patients aged between 18 and 65 years. Persons with an organic mental disorder were excluded due to their specific needs in psychiatric care and organizational structures. To avoid a selection bias of outliers, those with > 10 admissions were excluded. The population in the catchment area grew constantly during 2008 (n = 380’499) to 2016 (n = 415’682) with a balanced distribution of sex and a growing proportion of foreign nationals; 30.9% before, 31.9% after 2013. The number of beds served in the canton Zurich remained unchanged during the study period.
2.4. Data collection
Data of this study are based on anonymized routine documentation including documentation about the admission circumstances (voluntary vs. involuntary), prescribed medication, the application of additive individual or group psychotherapy combined with the standard therapeutic interventions on the wards, and the ICD-10 diagnosis at discharge. We also included socio-demographic parameters like gender, age, education level, disability benefits or Nationality in the analysis.
2.5. Statistical methods
For the longitudinal analysis of repeated measures of hospital admissions we fitted a series of Generalized Estimating Equations (GEE) [Reference Zeger, Liang and Albert38, Reference Gibbons, Hedeker and DuToit39], where we included hospitalizations, coded as voluntary vs. involuntary, as the dependent variable. We applied GEE models to fit regression analyses that account for within-subject correlation, which is an inherent part of longitudinal studies that rely on repeated outcome measures. The GEE approach uses weighted combinations between a predictor variable and repeated outcomes that account for varying observations, e.g. voluntary vs. involuntary admission, within a person across time. We applied a binomial distribution with logit link-function. We specified the within-subject covariance with the “unstructured” correlation type to avoid having any constraints on the covariance structure. To reduce the effects of outliers and influential observations we used a robust sandwich estimator. We included predictor variables in a step-wise procedure. All analyses were conducted with SPSS version 24 for Windows (IBM Corp. Released 2016. IBM SPSS Statistics for Windows, Version 24.0. Armonk, NY: IBM Corp.).
3. Results
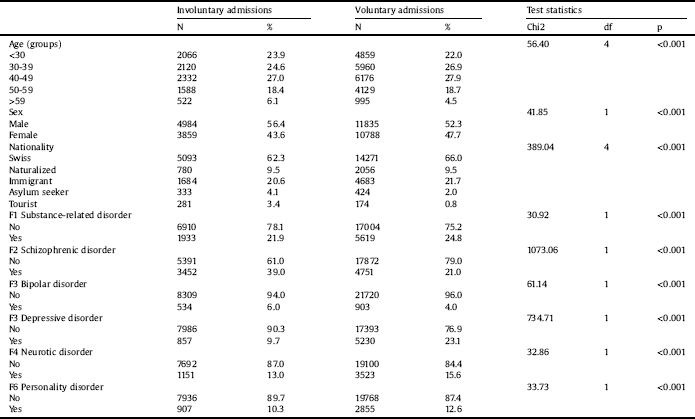
A total of n = 15’125 patients accounted for a total of n = 31’508 admission between the years 2008 and 2016. The number of admissions per patient ranged from 1 to 10, with a median of 2 and an interquartile range from 1 to 3. In detail, altogether n = 15’125 (48.0%) had one admission, n = 5’895 (18.7%) two, n = 3’356 (10.7%) three, n = 2’151 (6.8%) four, n = 1’456 (4.6%) five, n = 1’082 (3.4%) six, n = 827 (2.6%) seven, n = 675 (2.1%) eight, n = 527 (1.7%) nine, and n = 414 (1.3%) had ten admissions. A total of n = 4’560 (30.1%) of all patients experienced at least one IA. Between 2008–2012, n = 5178 (31.6%) and between 2013–2016 n = 3665 (24.2%) admissions were involuntary. In total, between 2008 and 2016, n = 8’843 (28.1%) of all admissions were involuntary. A comparison of the involuntary and voluntary admitted patients is shown in Table 1.
We tested for associations between socio-demographics and IA. In the following we will mainly focus on substantial effect sizes significant at α = 0.1%. The new legislation on child and adult protection, sex, education level, and nationality were significantly related to IA (test of model effects: all p < 0.001). The parameter estimates are shown in Table 2. The results show that women, compared to men, are less susceptible to IA. A high and intermediate education level, compared to a low education level, was also a protective factor. The period after implementation of the new legislation in January 2013 was significantly related with lower risk for IA. As regards nationality, tourists and asylum seekers, compared to Swiss-born people, were at increased risk of IA. Overall, with the exception of being a tourist (OR = 4.73) or an asylum seeker (OR = 1.99), all effect sizes for socio-demographics were small.
Next, we added diagnostic variables to the socio-demographics detailed above. Among the newly included variables, ICD-10 F2 schizophrenic disorder, F3 bipolar disorder and depressive disorder revealed statistically highly significant model effects (all p < 0.001). The parameter estimates are shown in Table 3. The most important predictors of IA were being a tourist (OR = 3.65) or an asylum seeker (OR = 2.20) and having a F2 schizophrenic disorder (OR = 2.27) or a F3 bipolar disorder (OR = 1.95). Noteworthy, having a F3 depressive disorder was related to a considerably lower likelihood of IA (OR = 0.57).
In the final model, we included the following treatment variables into the model: prescription of additive individual or group psychotherapy, prescription of neuroleptics, and prescription of antidepressants. All three variables made statistically highly significant contributions to the full model (test of model effects: all p < 0.001). The parameter estimates of the model are shown in Table 4. As before, the most important predictors were being a tourist (OR = 3.45) or an asylum seeker (OR = 2.29) and having a F2 schizophrenic disorder (OR = 2.04), or a F3 bipolar disorder (OR = 1.86). Having a F3 depressive disorder (OR = 0.65), prescription of antidepressants (OR = 0.66), receipt of psychotherapy (OR = 0.85) and the new legislation (OR = 0.71) were weak protective factors.
In addition to the predictors of involuntary admission detailed above, we compared patients with a Swiss nationality to tourists and asylum seekers. Patients with a Swiss nationality had a higher risk to be hospitalized with an ICD-10 F1 substance-related disorder than tourists and asylum seekers (26.0% vs 12.7% and 12.3%; X2 = 109.75, df = 2, p < 0.001). In contrast, tourists had a higher risk to be hospitalized with an ICD-10 F2 schizophrenic disorder (54.9%) or an ICD-10 F3 bipolar disorder (7.7%) and a lower probability to be hospitalized with an ICD-10 F3 depressive disorder (6.6%) than Swiss people (corresponding rates: 25.5%, 5.3%, and 17.4%; all X2>36.0, df = 2, p < 0.001). Compared to patients with a Swiss nationality, asylum seekers had a higher probability to be hospitalized with an ICD-10 F4 stress related disorders (40.9% vs. 12.6%), whereas the rate did not considerably differ from tourists (13.6%); X2 = 492.61, df = 2, p < 0.001. Finally, asylum seekers (69.8%) and tourists (62.4%) were more often male than patients with a Swiss nationality (51.9%); X2 = 110.62, df = 2, p < 0.001. Asylum seekers (34.0 years) were also significantly younger than patients with a Swiss nationality (40.2 years) or tourists (38.9 years); F = 97.19, df = 2, p < 0.001.
Socio-demographic and clinical characteristics in admissions for inpatient treatment, comparison of subgroups.
Repeated associations of socio-demographic variables with involuntary admissions from 2008 to 2016.

The Generalized Estimating Equations (GEE) reveal the odds ratio for being involuntarily admitted. The new legislation was implemented on 1st January 2013.
4. Discussion
4.1. Key findings
In this study, we could show that being a tourist or an asylum seeker as well as having a schizophrenic disorder or a bipolar disorder, were factors positively associated with IA in a comprehensive cohort of 15’125 patients admitted for inpatient treatment between 2008 and 2016 in Zurich. Male gender and higher age, were also risk factors for IA.
4.2. Involuntary admission in Zurich
The new legislation, implemented in 2013, aimed to strengthen patient autonomy. We could show that it is indeed associated with a lower risk for IA. To our knowledge, no relevant changes in mental health care which could have contributed to the differences in the risk for IA before and after implementation of the new law took place in this catchment area.
Despite this positive effect, the rate of IA in the study population is still high compared to other countries [Reference Salize and Dressing6, Reference Schuler, Tuch and Peter40]. This may seem contradictory as Switzerland has a highly developed health care system and invests a relatively high amount of its Gross Domestic Product (GDP) into health care [41]. The number of psychiatric inpatient beds and psychiatrists in private practice per citizen in Switzerland is among the highest in the world [42, 43]. Patients can choose between a variety of treatment options ranging from treatment in private practices, day hospitals, home treatment, acute crisis intervention to psychiatric inpatient treatment [44]. Against this background, the high rates of IA in the canton of Zurich cannot be explained by insufficient provision of psychiatric treatment. It therefore rather seems likely that it is due to cultural aspects and the legal requirements for IA laid down in the respective legislation [Reference Salize and Dressing6, 8]. In this respect, the range of professionals who are entitled to issue IAs - psychiatrists, public health officers, physicians without a psychiatric specialization and/or non-medical authorities - [Reference Salize and Dressing6, Reference Schuler, Tuch and Peter40] might be worth considering: In a previous study, we found that physicians with different specializations and professional backgrounds differ in the quality of their commitment documents and the patients` clinical course after admission [45–Reference Hotzy, Kieber-Ospelt, Schneeberger, Jaeger and Olbrich47]. Comparable differences regarding the referring authorities have also been found in other countries [48–Reference Cutler, Smith, Wand, Green, Dinh and Gribble51].
:Repeated associations of socio-demographic and diagnostic variables with involuntary admissions between 2008 and 2016.

The Generalized Estimating Equations (GEE) reveal the odds ratio for being involuntarily admitted. The new legislation was implemented on 1st January 2013.
Associations of socio-demographic, diagnostic, and treatment variables with involuntary admissions between 2008 and 2016.

The Generalized Estimating Equations (GEE) reveal the odds ratio for being involuntarily admitted. The new legislation was implemented on 1st January 2013.
Furthermore, the extent to which persons who demonstrate unusual social behavior are perceived as a burden depend on cultural norms and values. Therefore, the “burden criterion” in the Swiss legislation particularly might affect the decision-making process regarding IAs. This effect could be even more pronounced when the physician feels pressurized by third parties (e.g. relatives or authorities) [Reference Rotvold and Wynn52].
Future studies should evaluate the effect of the legal regulation on the rates of IA in more detail. Furthermore, associations between societal attitudes towards psychiatry and coercion and rates of IA should be assessed.
4.3. Associations of patients’ characteristics and involuntary admission
Like in other studies [Reference Salize and Dressing6, Reference Lay, Nordt and Roessler18, 23–Reference Eytan, Chatton, Safran and Khazaal26], we found that patients with schizophrenic disorders were significantly more likely to be involuntarily admitted. Paranoid ideations, hallucinations and anxiety (some of the main symptoms in these disorders) [53] might go hand in hand with an increased stress-level and reduced coping-strategies. They might lead to behavior that is experienced as burdensome or even threatening by others or that is endangering to the patients themselves. Also, the symptomatology of manic exacerbations might lead to distress in the environment. Comparable to patients with psychotic disorders, a lack of awareness [Reference Pini, Cassano, Dell’Osso and Amador54] in patients with a manic episode might lead to refusal of treatment on a voluntary basis and thereby make the decision for an IA more likely in this group of patients.
Besides clinical factors, male gender was significantly associated with IA. Whilst this finding is congruent with several previous studies [Reference Curley, Agada, Emechebe, Anamdi, Ng and Duffy17, Reference Riecher, Roessler, Loeffler and Faetkenheuer25, Reference Hustoft, Larsen, Auestad, Joa, Johannessen and Ruud28], another set of studies have shown a higher risk in female gender [Reference Eytan, Chatton, Safran and Khazaal26, Reference Gou, Zhou, Xiang, Zhu, Correll and Ungvari29, Reference Chang, Ferreira, Ferreira and Hirata30]. Societal attitudes and differences in treatment culture might lead to different help-seeking behavior in males and females. Furthermore, the availability of gender specific treatment programs might play a role in these inconsistencies. Further research should assess which factors are associated with a risk for coercion in male and female persons.
In line with previous results [Reference Curley, Agada, Emechebe, Anamdi, Ng and Duffy17, Reference Lay, Nordt and Roessler18, Reference Hustoft, Larsen, Auestad, Joa, Johannessen and Ruud28], we found that a foreign nationality was significantly associated with IA. More precisely, compared to clinical and other factors analyzed in our models, being a tourist or an asylum seeker had the biggest effect size in the contribution to IA.
Staying or even living in a foreign country, with a different culture and language, can be a stressful situation and might increase the vulnerability for psychiatric disorders. Besides the higher probability for IA, asylum seekers differed from patients with Swiss nationality regarding age and a higher frequency of stress related disorders. Asylum seekers might have experienced violence and lost family members. Therefore, this groups is more vulnerable to suffer from stress related disorders like PTSD [Reference Fazel, Wheeler and Danesh55].
Tourists, suffering more often from a schizophrenic or a bipolar disorder in our study, might sometimes be driven by psychopathological symptoms (e.g. delusional symptoms) which urge them to leave their home country and search freedom in another country. Nevertheless, the lack of a supporting environment, insufficient knowledge about the organizational structures of mental health care in a foreign country, language barriers and cultural differences might hinder patients to get adequate treatment at an early stage. For the referring physicians, the lack of support by next of kin and/or a familiar place might be an important limitation in the search for alternatives (e.g. outpatient crisis intervention or home treatment) to (involuntary) inpatient treatment. Therefore, in some situations, the referral to a psychiatric institution might seem to be the only way to manage the situation. Pressure from third parties involved might also foster the decision for an IA [Reference Rotvold and Wynn52]. The increased risk for IA in tourists and asylum seekers emphasizes the importance to provide easily accessible treatment and widespread information about its availability to prevent a crisis in which IA has to be used and might, in the worst case, lead to re-traumatization instead of relief [Reference Seed, Fox and Berry56].
The diverse clinical and socio-demographic characteristics associated with IA underline that there is not one type of patient who is at risk to be involuntarily admitted. Alternative treatment strategies to IA have to cover different psychiatric diagnoses and socio-demographic aspects.
Also, besides efforts to reduce the numbers of IA, it is important to keep in mind that IA is still part of psychiatric practice and that the establishment of a good therapeutic relationship in involuntarily admitted patients is challenging [57–Reference Theodoridou, Schlatter, Ajdacic, Roessler and Jaeger60]. Therefore, strategies should be used to keep the perceived coercion during involuntary treatment as low as possible. The referring agents and hospital physicians should be transparent and include patients and their next of kin when they make treatment plans [8]. The use of advance directives might also be helpful [Reference Fiorillo, De Rosa, Del Vecchio, Jurjanz and Schnall61]. Psychotherapeutic approaches - associated with a decreased risk for IA in our study - should be emphasized in patients at risk for IA and coercion [Reference Steinert, Weissenau and Hirsch62, 63].
4.4. Limitations
The analysis is based on retrospective analysis. It was not possible to assess the subjective perspectives of patients, nor was it possible to assess the psychopathology/symptom level of the patients during their treatment course.
Data were assessed only in one state of Switzerland. Nevertheless, some of the findings are in line with previous studies from different countries and therefore, might not only be culturally bound. Future studies should focus on the role of patients’ clinical aspects, treatment culture, legal and socio-cultural backgrounds during the decision-making-process for IA.
The duration of the analyzed period (8 years) and the large number of the included patients are strengths of this study and may outweigh some of the limitations.
4.5. Conclusion
We found that some clinical characteristics of patients are associated with a higher risk for IA. Interestingly, non-clinical factors like being a tourist, or an asylum seeker had the highest contributions in our models. This indicates that a variety of aspects shape the decision for an IA. Although the rates of IA remain high in the catchment area assessed in this study [Reference Schuler, Tuch and Peter40], the new legislation resulted in lower risk for IA. This finding can be considered as a success of the new law aiming to strengthen the patients` autonomy. Future studies should focus on treatment strategies to reduce the number of IA in patients at risk. Furthermore, efforts should be made to increase the knowledge about different treatment options in the society and especially, in those who are authorized to decide whether IA is necessary or not.
Authors' contributions
Study conceptualization and data collection: FH, MH, AT
Analysis and interpretation of data: FH, MH, AT
Drafting the article and revising it critically for important intellectual content: FH, MH, PH, MJ, AT
Final approval of the version to be published: FH, MH, PH, MJ, AT.
Funding
This study was conducted without any specific funding.
Conflict of Interest
All authors declare that there are no conflicts of interest in relation to the subject of this study.
Compliance with ethical standards
The study was approved by the Cantonal Ethics Commission of Zurich, Switzerland (Reference Number EK: Req-2017-00592).
This study has been performed in accordance with the ethical standards laid down in the 1964 Declaration of Helsinki and its later amendments. All data analyzed in this study were anonymized data. An identification of the patients was not possible at any time of the study.
This article does not contain any studies with animals performed by any of the authors.






Comments
No Comments have been published for this article.