The Mediterranean diet is characterised by the high consumption of extra virgin olive oil (EVOO), vegetables, fruits, grains, legumes and nuts; moderate consumption of fish, poultry, eggs, dairy products and red wine; and low consumption of red meat and commercial sweets(Reference Davis, Bryan and Hodgson1). The components of the Mediterranean diet are rich in bioactive nutrients, including MUFA and PUFA, n-3 fatty acids, polyphenols, flavonoids, antioxidants, fibre, and a range of vitamins and minerals.
Cross-sectional and longitudinal studies show that populations following a Mediterranean diet experience better cardiovascular health and lower rates of CVD(Reference Sofi, Macchi and Abbate2). Randomised controlled trials corroborate observational findings, reporting improvements to blood pressure, blood vessel function, lipid profiles, atherosclerosis, insulin sensitivity and risk of CVD following adherence to a Mediterranean diet(Reference Martínez-González, Salas-Salvadó and Estruch3, Reference Davis, Hodgson and Woodman4–Reference Lee, Pase and Pipingas6).
Dietary guidelines in the USA have been revised to include the Mediterranean diet as a healthy dietary pattern while Nutrition Australia have revised their Healthy Eating Pyramid to reflect Mediterranean dietary principles(7). However, few studies have examined the feasibility of implementing a Mediterranean diet in non-Mediterranean populations. Conducted in an older Australian population, the Mediterranean diet for cognitive and cardiovascular health in the elderly (MedLey) study examined cardiovascular and cognitive effects of a Mediterranean diet, as well as dietary adherence and compliance over 6 months. Participants achieved a high level of Mediterranean diet adherence, as measured by a priori adherence scores(Reference Davis, Bryan and Hodgson8). However, participants also reported that adhering to the red meat restrictions was one of the most challenging aspects of following the diet(Reference Davis, Hodgson and Bryan9).
Mediterranean dietary guidelines recommend consuming <2 serves of red meat per week(10, Reference Bach-Faig, Berry and Lairon11). A traditional Mediterranean diet includes 105 g, or 0·5–0·75 standard serves of meat and meat products per d(Reference Davis, Bryan and Hodgson1). This figure is inclusive of all processed and unprocessed red and white meat products. In contrast, Australians over the age of 19 years consume an average of 184 g of meat per d, or 1·7 serves of lean meats and alternates, with red meat contributing the largest proportion of this (38 %)(12). Australians are amongst the highest consumers of meat in the world(13). Therefore, restricting red meat may be difficult. Countries with comparatively high meat intakes, such as the USA and UK, may experience similar challenges(13). As socio-cultural norms and palatability are key determinants of a dietary intervention’s sustainability(Reference Knight, Bryan and Murphy14), non-Mediterranean populations may be more likely to adhere to a diet containing more red meat or meat protein.
Prospective studies indicate that red meat consumption may be linked to poorer health outcomes, including bowel cancer and CVD(Reference Wolk15). However, recent investigations suggest that the presence of other dietary components, including oleic acid, vitamin E and fibre, may attenuate the negative effects of red meat consumption(Reference Van Hecke, Van Camp and De Smet16, Reference Tirosh, Shpaizer and Kanner17, Reference Norat, Bingham and Ferrari18).
In Australia, beef, veal and pork are the most frequently consumed red meats(13). Fresh lean beef and fresh lean pork have similar nutrient profiles. However fresh lean pork contains less saturated fat per 100 g. Therefore, pork may be a suitable addition to the Mediterranean diet, which is typically low in saturated fat and haeme Fe sources(Reference Davis, Bryan and Hodgson1). Substituting beef and chicken with pork also positively affects weight, BMI, percentage body fat, fat mass and abdominal fat(Reference Murphy, Thomson and Coates19). Further, when compared with ruminant meats such as beef, pork production is associated with significantly less agricultural greenhouse gas emissions(Reference Tilman and Clark20).
To our knowledge, no studies have investigated the cardiovascular effects of a Mediterranean diet with an increased intake of lean red meat. Therefore, the present study aimed to evaluate the cardiovascular effects of a Mediterranean diet supplemented with fresh lean pork against a low-fat (LF) diet. An LF control diet was chosen due to its continued recommendation for the clinical management and reduction of cardiovascular risk(21). Further, including an LF control would enable comparisons of our findings with larger studies of the same design, such as the Prevención con Dieta Mediterránea (PREDIMED) trial(Reference Estruch, Ros and Salas-Salvadó22).
Methodology
The study protocol has been described in detail elsewhere(Reference Wade, Davis and Dyer23).
Ethics and registration
This trial was registered with the Australian New Zealand Clinical Trials Registry (ACTRN12616001046493) on August 2016 and was conducted in accordance with the Declaration of Helsinki. All procedures involving human participants were approved by the University of South Australia Human Ethics Committee (no. 35662).
Participants and recruitment
Volunteers aged between 45 and 80 years and at risk of developing CVD were recruited between January and May 2017 via electronic and paper advertisements.
Volunteers were required to have systolic blood pressure (SBP) above 120 mmHg and at least two other risk factors for CVD, including a BMI ≥ 25 kg/m2; elevated fasting total cholesterol (≥5·5 mmol/l), TAG (≥2·0 mmol/l), LDL (≥3·5 mmol/l) or low levels of HDL (≤0·9 mmol/l for men and ≤1·0 mmol/l for women); impaired fasting glucose tolerance (between 6·1 and 7·8 mmol/l); and/or a family history (up to one generation) of CVD or type 2 diabetes mellitus. Exclusion criteria included antihypertensive medication; smoking; current CVD or angina; current or recent (within 6 months) malignancies; respiratory disease; gastrointestinal disease; kidney disease; a current diagnosis of type 2 diabetes mellitus; a current or previous traumatic head or brain injury; a current neurological or psychiatric condition; antidepressant or anxiety medication; a current diagnosis of Alzheimer’s disease or dementia; high adherence to a Mediterranean diet indicated by a score of 10 or more, out of a total possible fifteen points, assessed using a modified Mediterranean diet adherence survey (described below); or supplemental n-3 fatty acids > 1000 mg daily.
Design
A 24-week parallel cross-over design trial compared a Mediterranean diet intervention with 2–3 weekly serves of pork (MedPork) with an LF control intervention. Each participant completed both dietary interventions for 8 weeks and the two intervention phases were separated by an 8-week washout period (see Fig. 1). Using block randomisation and a block size of 4, an independent staff member randomly assigned participants to their first dietary intervention (MedPork or LF), stratified by sex and age. During the washout period, participants returned to their habitual diet. An 8-week intervention period was deemed adequate due to previous research, which indicates that the nutrients contained within the Mediterranean diet can improve both cardiovascular function over similar time periods(Reference Desideri, Kwik-Uribe and Grassi24–Reference Nilsson, Radeborg and Salo26).
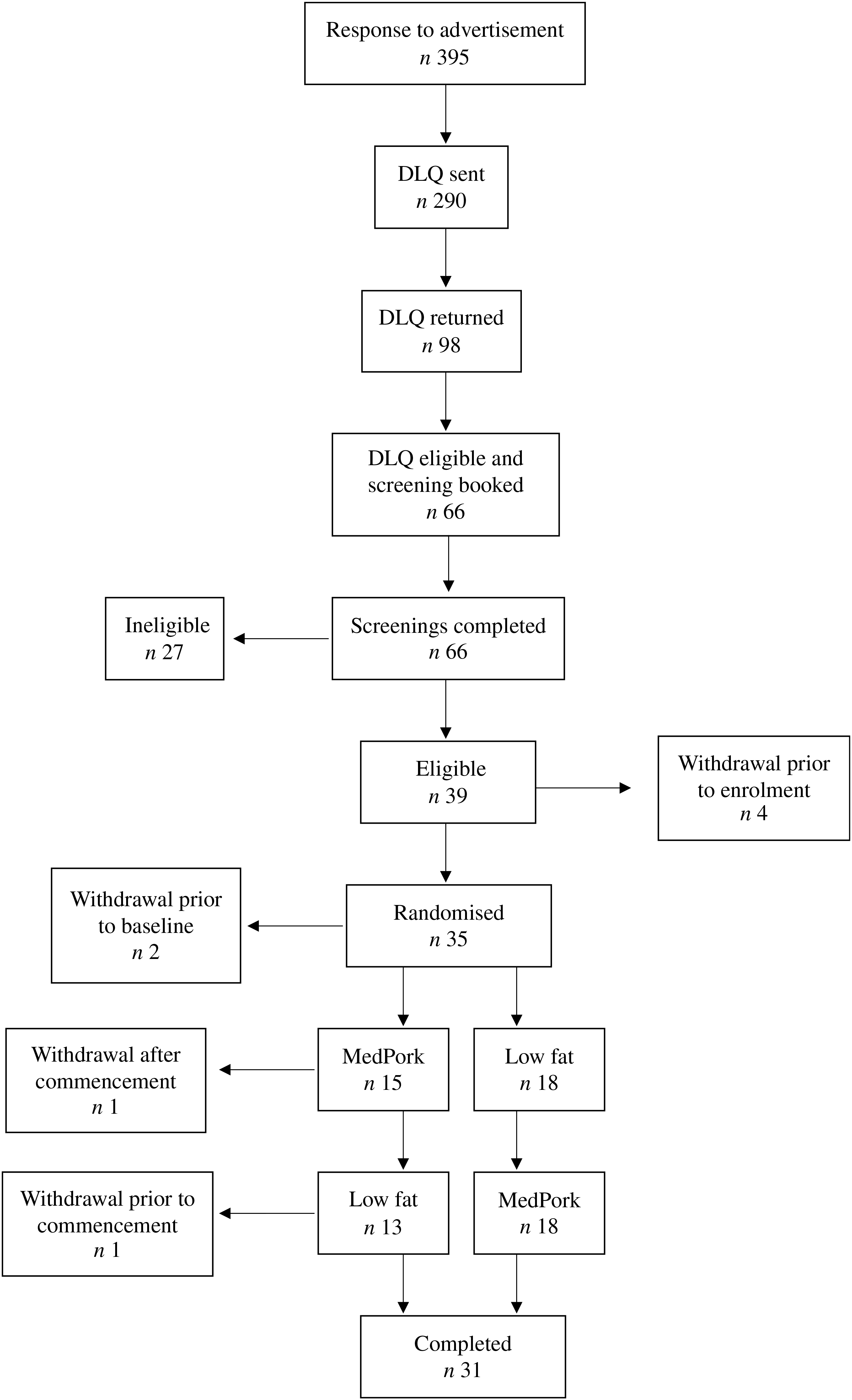
Consolidated Standards of Reporting Trials (CONSORT) diagram illustrating flow of participants from recruitment through to study completion. Intention-to-treat analysis is based on all participants with baseline data (n 33). DLQ, Diet and Lifestyle Questionnaire; MedPork, Mediterranean diet supplemented with pork.
Dietary interventions
Neither diet restricted energy intake. Participants were advised to consume foods ad libitum and self-regulate their food intake according to individual hunger and satiety cues.
Low-fat diet. Guidelines for the LF diet were based on the PREDIMED study(Reference Martínez-González, Corella and Salas-Salvadó27). General guidelines were adapted from the Australian Guide to Healthy Eating and the National Heart Foundation Guidelines (2012)(28, 29). Participants were advised to make adjustments to their habitual diet in order to reduce total fat intake. For example, participants were recommended to replace high-fat foods, including all types of oil, butter, margarine, processed and high-fat meats, nuts, chocolates, cakes, pastry, and high- or full-fat dairy products, with LF alternatives, such as breads and cereals, legumes, rice, fruits and vegetables and LF varieties (e.g. LF dairy products, LF sauces). Daily limits were set for oil (≤20 ml), butter and margarine (≤2 teaspoons), and participants were instructed to remove visible fat and skin from meat and fish before cooking.
Mediterranean diet supplemented with pork. Guidelines for the MedPork intervention were adapted from Estruch et al.(Reference Estruch, Ros and Salas-Salvadó22) for an Australian food supply and to include increased serves of fresh lean pork:
Minimum of one tablespoon (20 ml) of EVOO per d;
≥2–3 daily servings of fresh fruit (1 serve = 150 g fresh, 30 g dried, or one cup canned in natural juice);
≥3 weekly servings of legumes (1 serve = 75 g);
2–3 weekly servings of fresh lean pork (1 serve = 100 g cooked)
≥3 weekly servings of fish and seafood (at least 1 serving of oily fish) (1 serve = 100 g cooked);
≥5 weekly serving of raw or roasted nuts or seeds, without added salt, sugar or chocolate (1 serve = 30 g; 7·5 g hazelnuts, 15 g walnuts, 7·5 g almonds supplied for each serve);
Ad libitum consumption of wholegrain cereal products (bread, pasta, rice, cereal) and dairy products;
Ad libitum consumption of eggs, not to exceed 6 serves per week (1 serve = approximately 70 g or 1 egg);
Select white meats (poultry without skin) instead of red meats or processed meats;
Limit consumption of red and cured meat (remove all visible fat) to ≤1 serve/week (1 serve of red meat/cured ham = 100 g);
Limit consumption of chocolate to ≤1 serve/week (1 serve of chocolate = 50 g);
Use EVOO for cooking and dressing vegetables and salad;
Cook regularly (at least twice a week) with a tomato-based sauce (EVOO, tomato, garlic and onion);
Dress vegetables, pasta, rice and other dishes with EVOO, tomato, garlic and onion sauce;
Eliminate or limit the consumption of cream, butter, margarine, cold meat, pâté, duck, carbonated and/or sugared beverages, pastries, commercial bakery products (cakes, doughnuts, cookies), desserts (puddings), French fries, potato crisps, sweets; and
For usual drinkers, red wine is recommended as the main source of alcohol with a maximum of two standard drinks per d (200 ml = two standard drinks).(30)
Participants were advised to consume pork in place of chicken and red meat and ensure that total meat consumption did not exceed 400 g (four serves) per week.
Notably, recommendations for EVOO differ from the original PREDIMED guidelines, which advised participants to consume ≥60 ml/d. This decision was made to increase acceptability for an Australian population, where EVOO is consumed neither habitually nor in abundance(Reference Davis, Bryan and Hodgson8). Although considerably lower than recommendations from the PREDIMED trial, previous research conducted in Australia has indicated that a Mediterranean diet containing ≥1 tablespoon of EVOO per d is capable of improving cardiovascular outcomes(Reference Davis, Hodgson and Woodman4).
To assist with adherence, the following foods were provided each week: 375 ml EVOO (donated by Cobram Estate); 250 g of fresh lean pork; 150 g raw, unsalted almonds (donated by Almond Board of Australia), walnuts and hazelnuts; 225 g (net weight) of canned chickpeas, red kidney beans, four-bean mix and lentils (donated by Simplot Australia Pty Ltd); 95 g of canned tuna; and 95 g of canned salmon (donated by Simplot Australia Pty Ltd).
Dietetic counselling. For the Mediterranean diet and LF diets, participants were provided with a set of dietary resources as described by Wade et al.(Reference Wade, Davis and Dyer23). Throughout each intervention phase, participants attended fortnightly dietetic visits to discuss progress, food intake, challenges and any adverse effects. Dietetic visits also included weight measurement to determine body mass, weight loss or weight gain.
Outcome measures
Home blood pressure. Home-measured SBP was the primary outcome measure. Participants received training on self-administered blood pressure measurement and were provided with a clinically validated A&D Company Ltd digital blood pressure monitor (model UA-767). Participants were instructed to take three blood pressure measurements, with a 1-min rest period in between each reading, every morning, afternoon and evening for a period of 6 d.
Secondary outcome measures. Over the four assessment time points, home-measured diastolic blood pressure (DBP) and heart rate, clinic blood pressure and heart rate, BMI, waist:hip ratio, body composition, fasting blood lipids, C-reactive protein, fasting plasma glucose, fasting serum insulin, dietary adherence and nutrient intake were secondary outcomes.
Dietary adherence. A fiteen-item MedPork adherence survey and a nine-item LF diet adherence survey were administered to participants fortnightly to capture generalised patterns of food consumption during each of the intervention phases. Surveys were adapted from the Mediterranean diet and LF questionnaires used in the PREDIMED study(Reference Martínez-González, Corella and Salas-Salvadó27). The scoring of the Mediterranean diet survey was modified to reflect our MedPork guidelines developed for an Australian population as outlined above. Specifically, consumption of ≥1 tablespoon of EVOO was awarded 1 point in the present study, as compared with the necessary ≥4 tablespoons in the PREDIMED design. An item relating to fresh pork consumption was also included to reflect the MedPork intervention. See Supplementary material S1 for surveys and scoring. During the MedPork intervention, participants also completed a semi-quantitative weekly checklist (described above). In line with the study protocol, participants required to achieve a minimum of 75 % adherence on the MedPork and LF surveys each fortnight.
Adherence to the Mediterranean diet was also calculated using the Mediterranean diet score (MDS), developed by Trichopoulou et al.(Reference Trichopoulou, Costacou and Bamia31). The MDS was applied to dietary data from 3-d weighed food records completed by participants before and at the end of each intervention phase.
Procedure
Participants attended a prebaseline appointment at the Sansom Institute for Health Research Clinical Trial Facility (SIHR CTF) where the study was explained, and informed consent was obtained by study personnel. Instructions and equipment were given for the collection of home measures, including blood pressure and weighed food records. Participants then returned 1 week later for week 0 assessments.
Clinic assessment visits took place at baseline of the first diet (week 0), at the end of the first diet (week 8), at baseline of the second diet, after the 8-week washout period (week 16) and at the end of the second diet (week 24). Data for home measures were collected by participants in the week prior to each of these visits.
Volunteers were instructed to continue any habitual exercise and medications for the duration of the trial. Changes to exercise and medications were monitored and recorded at fortnightly dietetic visits and clinic assessment visits by the investigators.
Statistical analysis
Statistical analyses were conducted using SPSS for Windows, version 21.0 (SPSS Inc.) and Stata (version 14.2, StataCorp). Weighed food records were entered into Foodworks Professional software (version 9.0, Xyris Software) to calculate food group and nutrient values. Serve sizes are based on recommendations from the Australian Guide to Healthy Eating(28).
Data are presented as means and standard deviations or standard errors for descriptive statistics and as means and 95 % CI for estimated effects. All tests are two-tailed with P < 0·05 deemed statistically significant. Residuals were screened for normality and variables were transformed if necessary.
Based on power calculations, a sample size of thirty-one volunteers was required to detect a clinically relevant difference of 2·5 mmHg in home blood pressure, the primary outcome measure, with power of 90 %. This calculation assumes a total of fifty-four blood pressure readings (three readings taken three times per d for 6 d) at each time point, a within-group SD of 14 mmHg, a within-subject repeated measures correlation of r 0·6 and a between-phase within-subject correlation of ρ = 0·5. The correlation (ρ) and use of a cross-over design reduce the number of required participants required for a parallel group design by a factor of 1/(1 − ρ)/2 = 4(Reference Hsieh, Lavori and Cohen32), that is, from approximately 124 subjects for a parallel group design using ANCOVA with adjustment for baseline (n 62 per group) to thirty-one subjects in total.
Linear mixed-effects models were used to compare the effects of the two treatments. The period of intervention (first v. second), the order in which dietary interventions were given (LF first v. MedPork first), the visit (baseline v. week 8) and an interaction term for treatment × visit were included in the model as fixed effects, while subjects were included as random effects. Differences in effects between treatments were assessed using the estimated marginal mean differences in week-8 values between treatments and the associated P values. We also investigated possible period effects and carryover effects using treatment × visit × period and visit × period interaction terms, respectively. Where significant these terms were also included in the model. As change in weight might potentially influence the treatment effects, weight at each time point was included as a covariate for all cardiometabolic outcomes, excluding measures of body composition and adiposity. Intention to treat analyses was performed by including all participants with baseline data (n 33). Missing data were estimated by relying on the best linear unbiased predictions in each mixed model. Difference in change between interventions (i.e. the difference between week 0 and week 8 following the MedPork intervention v. the difference between week 0 and week 8 following the LF intervention) is presented as the ‘estimated mean difference between interventions (MedPork v. LF)’. Positive values indicate an increase following the MedPork intervention and negative values indicate a decrease following the MedPork intervention. For log-transformed data, the difference between interventions is presented as the rate ratio change in the geometric mean.
Since obesity leads to increaseds blood pressure and a subsequent risk of the metabolic syndrome and CVD(Reference Dong, Ma and Song33), we conducted post hoc sub-group analyses for home-measured blood pressure and cardiometabolic outcomes, grouping participants into overweight (BMI ≥25–<30 kg/m2; n 17) and obese (BMI ≥ 30 kg/m2; n 14) categories. Participants with a BMI < 25 kg/m2 (n 2) were excluded from this analysis.
Previous studies have indicated that blood pressure readings taken on the first day of home blood pressure measurement may be higher than subsequent days. Daily averages were computed for each of the 6 d of home-measured SBP at week 0 (baseline) for each period. Paired samples t tests were conducted to compare day 1 with all other days. No significant differences were detected at P < 0·05 and therefore day 1 of SBP readings were retained in the analysis. Averages were also computed for the first, second and third readings of each day at week 0. Paired sampled t tests revealed significant differences for first readings as compared with second and third readings. The first reading for each day was therefore excluded from the analysis.
Results
A total of thirty-five participants were randomised. Baseline data were collected for thirty-three participants, who formed the modified intention-to-treat population. A total of thirty-one participants completed the two dietary interventions.
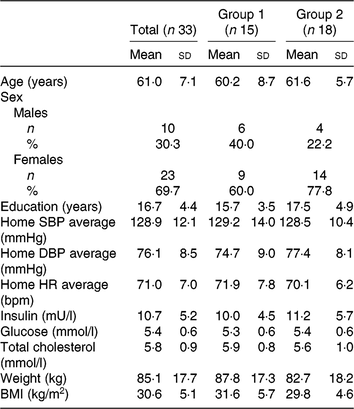
Results are based on the modified intention to treat population (n 33). Participants were randomly allocated to their starting dietary intervention. Group 1 (n 15) completed the MedPork intervention in period 1 and the LF intervention in period 2; group 2 (n 18) completed the LF intervention in period 1 and the MedPork intervention in period 2. Baseline characteristics of each group are presented in Table 1. No significant differences were detected between groups for demographic or cardiometabolic outcomes.
Demographic and clinical characteristics of the study sample at baseline, according to first dietary intervention*
(Mean values and standard deviations; numbers and percentages)
SBP, systolic blood pressure; DBP, diastolic blood pressure; HR, heart rate; bpm, beats per min; MedPork, Mediterranean diet supplemented with pork.
* Group 1 received the MedPork intervention first; group 2 received the low-fat intervention first.
Fig. 1 illustrates the consort flow of the study, indicating time of withdrawals. Of the thirty-three subjects, one participant withdrew during the MedPork intervention in the first period and one participant withdrew during the washout period, prior to commencing the LF intervention. Reasons for withdrawal included competing commitments (n 1) and illness preventing adherence to dietary intervention (n 1).
Period and carryover effects
A period effect for treatment (significant treatment × visit × period interaction) was detected for home-measured morning DBP, total cholesterol and HDL. Possible carryover effects (significant visit × period interaction) were detected for clinic DBP and LDL.
Dietary adherence and nutrient intake
Throughout both dietary interventions, all participants met the minimum requirement of 75 % dietary adherence. No participants were excluded from the study for failure to meet MedPork dietary guidelines.
The average LF adherence score achieved across the four fortnights of the LF intervention was 8·4 ± 1·1 out of a maximum of 9 points (93·3 % compliance).
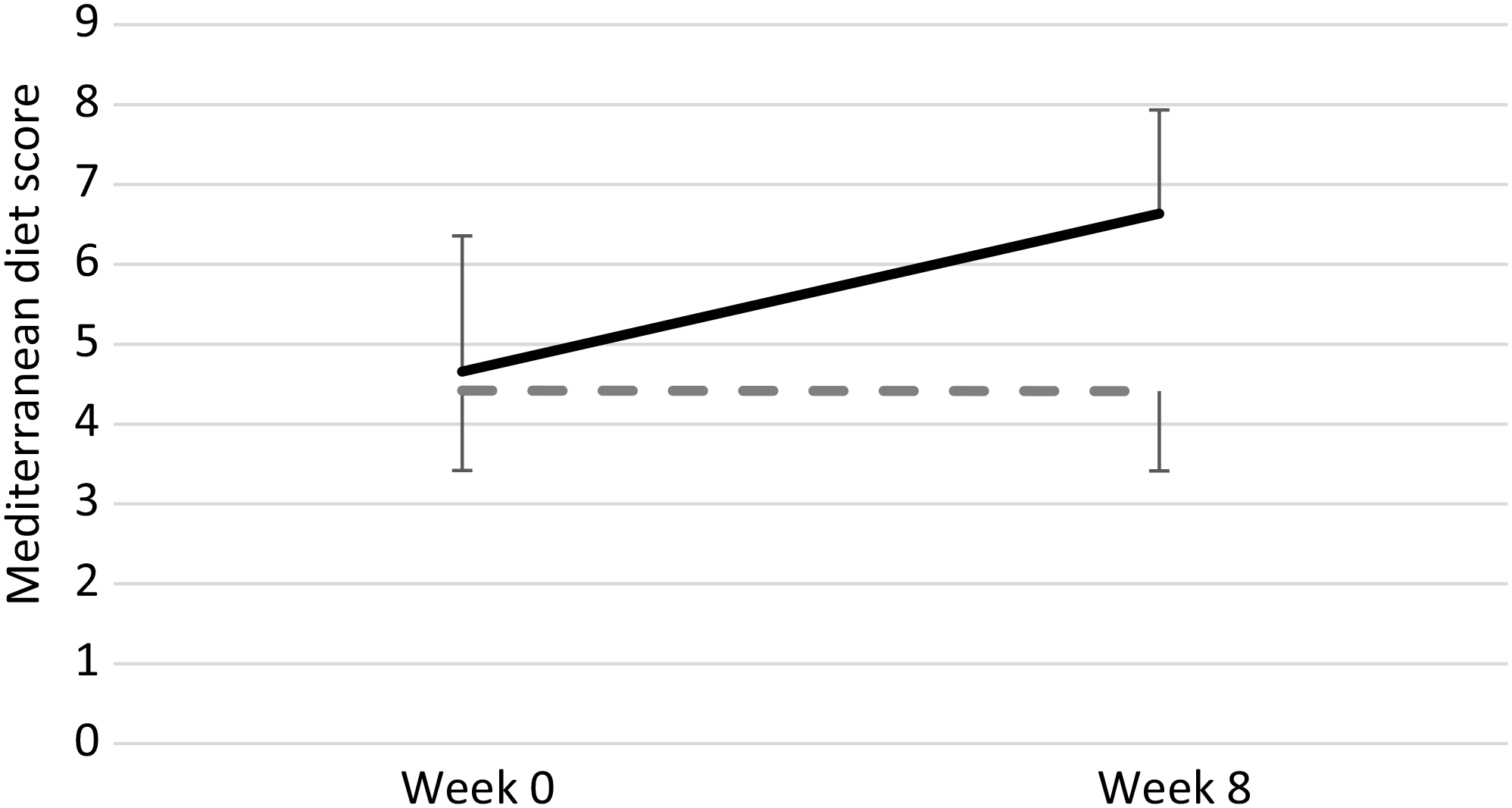
The average MedPork adherence score during the MedPork intervention was 13·5 ± 1·7 out of 15 (90 % compliance), representing an increase of 7·5 points from screening. According to the Trichopoulou et al. MDS(Reference Trichopoulou, Costacou and Bamia31) mean Mediterranean diet adherence increased from 4·7 (sd 1·8) to 6·6 (sd 1·3) out of 9 during the MedPork intervention and remained at 4·4 (sd 1·7) during the LF intervention (Fig. 2).
Adherence to the Mediterranean diet before and during the MedPork (---) and low-fat (LF; -- --) interventions, according to the Mediterranean diet score developed by Trichopoulou et al.(Reference Trichopoulou, Costacou and Bamia31). Mediterranean diet adherence increased from 4·7 to 6·6 by the end of the MedPork intervention and remained at 4·4 throughout the LF intervention. Data are means, with standard deviations represented by vertical bars.
Nutrient and food group intakes across both intervention periods are presented in Table 2. According to weighed food records and fortnightly checklists, mean fresh pork intake increased from 0·09 (se 0·1) serves per d to 0·44 (se 0·1) serves per d (approximately 3 serves per week) during the MedPork intervention and decreased from 0·16 (se 0·3) serves per d to 0·13 (se 0·2) serves per d during the LF intervention (P ≤ 0·001) (Table 2).
Energy and nutrient intakes at baseline and week 8, including between-group differences
(Mean values with their standard errors; mean differences and 95 % confidence intervals)
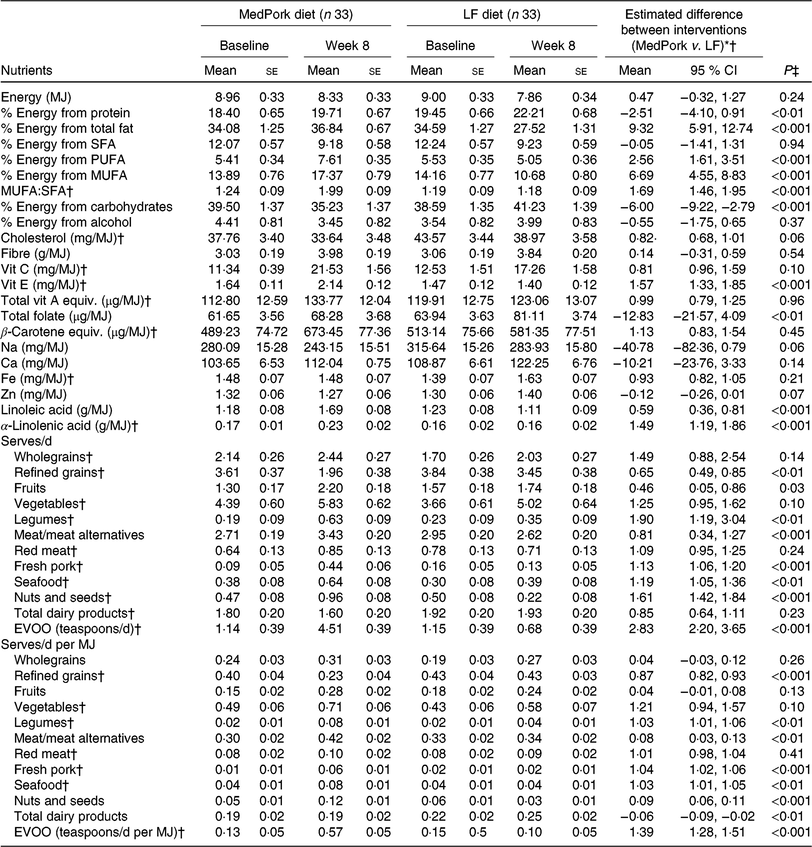
MedPork, Mediterranean diet supplemented with pork; LF, low-fat; vit, vitamin; equiv., equivalents.
* Estimated marginal mean difference from linear mixed-effects models. Differences between interventions were analysed by linear mixed-effects models, including fixed-effect terms for group, visit, group × visit, period, order and weight (excluding weight-related variables).
† Transformed variable: observed mean and standard error are presented together with rate ratio change in the geometric mean and associated P value.
‡ Adjusted for differences between treatments.
After 8 weeks, compared with the LF intervention, the MedPork intervention led to a significantly higher intake of % energy from fat (P < 0·001), % energy from MUFA (P < 0·001), % energy from PUFA (P < 0·001) and MUFA:SFA (P < 0·001). The LF intervention led to significantly higher intake of % energy from protein (P < 0·01) and carbohydrates (P < 0·001). The MedPork intervention led to significantly lower consumption of refined grains (P < 0·01), and higher consumption of legumes (P < 0·01), seafood (P < 0·01), nuts and seeds (P < 0·001), EVOO (P < 0·001), meat and meat alternatives (P < 0·001), but not red meat (P = 0·27).
The MedPork intervention led to significantly higher consumption of vitamin E (P < 0·001), linoleic acid (P < 0·001) and α--linolenic acid (P < 0·001). The LF intervention led to significantly higher intake of total folate (P ≤ 0·01). No other significant differences were observed across nutrients.
Home-measured blood pressure
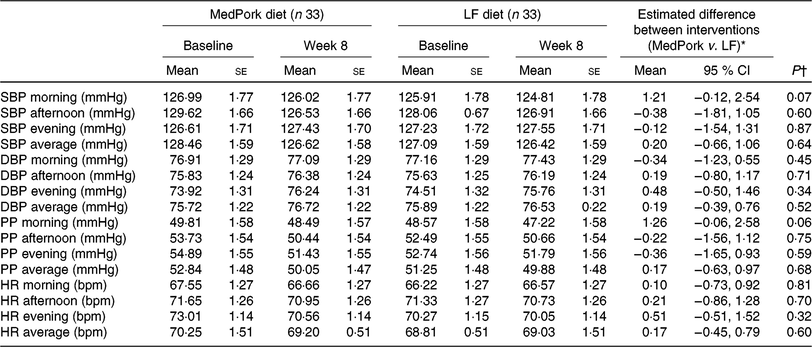
Results for home-measured blood pressure are presented in Table 3. For participants who completed blood pressure measurements at all time points (n 31), an average of 49/54 measures were taken, indicating 90 % compliance with instruction.
Home blood pressure at baseline and week 8, including between-group differences
(Mean values with their standard errors; mean differences and 95 % confidence intervals)
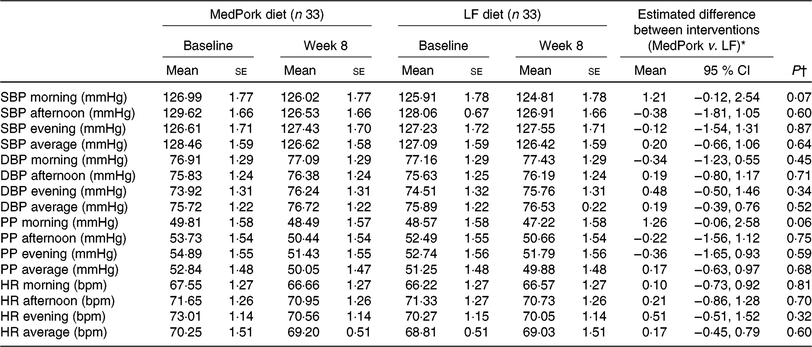
MedPork, Mediterranean diet supplemented with pork; LF, low-fat; SBP, systolic blood pressure; DBP, diastolic blood pressure; PP, pulse pressure; HR, heart rate; bpm, beats per min.
* Estimated marginal mean difference from linear mixed-effects models. Differences between interventions were analysed by linear mixed-effects models, including fixed-effect terms for group, visit, group × visit, period, order and weight.
† Adjusted for differences between treatments.
There was no difference in the changes to home SBP or DBP between the MedPork and LF diets for morning, afternoon, evening and average blood pressure (mmHg) or heart rate (beats per min) measurements. Similar trends were observed for SBP (mmHg) for both the MedPork and LF intervention, where morning, afternoon and average blood pressure decreased between baseline and week 8.
Secondary outcomes
Results for secondary cardiometabolic outcomes are presented in Table 4. The LF intervention led to significantly greater reductions in weight (kg) (P = 0·04), BMI (kg/m2) (P = 0·01), waist circumference (cm) (P ≤ 0·01) and fat mass (kg) (P = 0·04) compared with MedPork. No significant differences between diets were observed for clinic measures of SBP, DBP (mmHg) or heart rate (beats per min), insulin, glucose, C-reactive protein, total cholesterol, total TAG, HDL, LDL (mmol/l) or total cholesterol:HDL.
Clinic measures at baseline and week 8, including between-group differences
(Mean values with their standard errors; mean differences and 95 % confidence intervals)
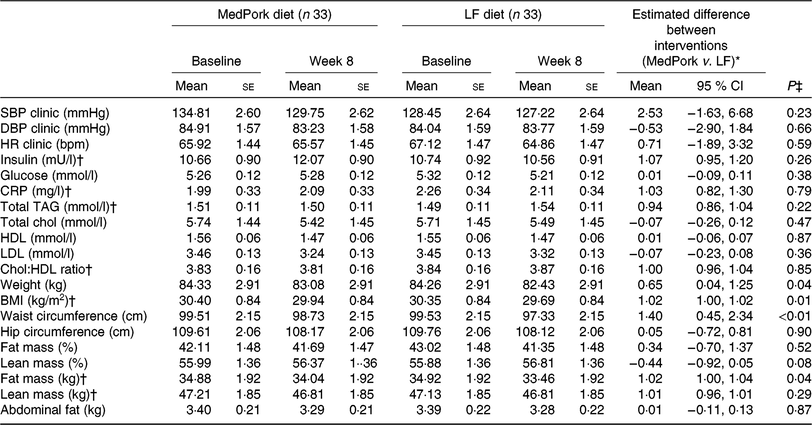
MedPork, Mediterranean diet supplemented with pork; LF, low-fat, SBP, systolic blood pressure; DBP, diastolic blood pressure; HR, heart rate; CRP, C-reactive protein; chol, cholesterol.
* Estimated marginal mean difference from linear mixed-effects models. Differences between interventions were analysed by linear mixed-effects models, including fixed-effect terms for group, visit, group × visit, period, order and weight (excluding weight-related variables).
† Transformed variable: observed mean and standard error are presented together with rate ratio change in the geometric mean and associated P value.
‡ Adjusted for differences between treatments.
Sub-group analyses
Sub-group analyses are presented in Table 5. In the overweight group, average home SBP (mmHg) was reduced more in the MedPork intervention compared with the LF intervention (P = 0·01). In contrast, in the obese group, average home SBP (mmHg) was reduced more in the LF intervention compared with the MedPork intervention (P < 0·001).
Subgroup analysis: average systolic blood pressure (SBP), diastolic blood pressure (DBP) and pulse pressure at baseline and week 8, including between-group differences, in overweight (BMI < 30 kg/m2) and obese (BMI ≥ 30 kg/m2) participants
(Mean values with their standard errors; mean differences and 95 % confidence intervals)
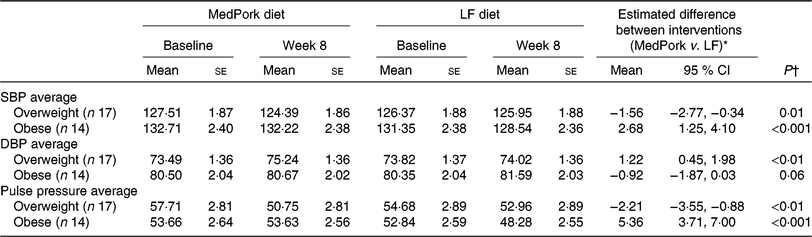
MedPork, Mediterranean diet supplemented with pork; LF, low-fat.
* Estimated marginal mean difference from linear mixed-effects models. Differences between interventions were analysed by linear mixed-effects models, including fixed-effect terms for group, visit, group × visit, period, order and weight.
† Adjusted for differences between treatments.
The MedPork intervention increased average home DBP (mmHg) more than the LF intervention in the overweight group (P < 0·01). There was no difference between interventions for average home DBP in the obese group.
Consistent with the changes in home SBP and home DBP, the MedPork led to a greater reduction in pulse pressure in the overweight group (P ≤ 0·01), while the LF intervention led to a greater reduction in pulse pressure (mmHg) in the obese group (P ≤ 0·001).
Discussion
The present study examined the cardiovascular effects of including 2–3 serves per week of fresh lean pork as a part of a Mediterranean dietary pattern for use in Australia. During the MedPork intervention, participants achieved a high level of adherence to MedPork dietary guidelines. The LF intervention led to greater reductions in weight, waist circumference and fat mass. Reductions were observed in morning, afternoon and average SBP following both the MedPork and LF interventions. However, no significant differences were detected between the MedPork and LF interventions for measures of cardiometabolic health, including home and clinic blood pressures, cholesterol, C-reactive protein, insulin and glucose.
Our cardiovascular findings differ from previous studies comparing the Mediterranean diet with the LF diet. A recent meta-analysis reported that Mediterranean diet interventions of at least 1-year duration effectively reduce both SBP and DBP(Reference Nissensohn, Román-Viñas and Sánchez-Villegas34). Notably, pooled analysis across six studies revealed a relatively small effect size. It is possible that the addition of pork to the Mediterranean diet displaced other bioactive ingredients and diluted these effects. Alternatively, the 8-week MedPork intervention may not have been long enough to elicit significant changes in blood pressure. Similarly, an 8-week intervention may have limited our capacity to observe significant improvements in secondary markers of cardiometabolic health, such as cholesterol, glucose and insulin, as seen in longer intervention trials(Reference Martínez-González, Salas-Salvadó and Estruch3).
The comparable changes in blood pressure may be partly explained by improvements to overall diet quality. Both the MedPork and LF intervention led to increased consumption of wholegrains, vegetables, fruit and fibre, and reduced intake of saturated fat. Notably, recent systematic reviews have reported that replacing SFA with MUFA, PUFA or high-quality carbohydrates has similarly beneficial effects on blood pressure and risk of cardiovascular events(Reference Clifton and Keogh35, Reference Jovanovski, de Castro Ruiz Marques and Li36). The LF intervention also led to significant improvements in measures of body composition. This is likely due to significant reductions in fat intake. However, reductions in weight, BMI, waist circumference and fat mass did not translate to improvements across other markers of cardiovascular health. While changes may have been observed over a longer intervention, previous research, including the PREDIMED trial, indicates that the LF diet is unsustainable and difficult to follow over extended periods of time(Reference Martínez-González, Corella and Salas-Salvadó27).
Our sub-group analyses revealed a significant effect of the MedPork intervention for average home SBP in overweight participants. In contrast, the LF intervention led to a decrease in average home SBP in obese participants. Corresponding with these reductions in SBP were increased DBP: the MedPork intervention led to an increase in DBP in the overweight group, while the LF intervention led to an increased DBP in the obese group. By reducing the difference between SBP and DBP, the MedPork diet led to significant improvements in pulse pressure for overweight participants. Likewise, the LF intervention led to significant improvements in pulse pressure for obese participants. These findings indicate that the MedPork intervention may improve vascular haemodynamics in overweight individuals, while obese individuals may require further dietetic intervention, such as energy restriction with targeted weight loss, to achieve similar results. However, these findings should be interpreted with caution due to the small sample size of overweight and obese individuals included in the analysis.
It is important to acknowledge the following limitations. As mentioned above, the present study was limited in duration, comparing two 8-week interventions. Although similar nutritional interventions have elicited cardiovascular change over comparable time periods, a longer intervention may have led to stronger results. Our selection criteria were developed to identify individuals at risk of CVD. This included individuals with a minimum SBP of 120 mmHg. However, higher blood pressure values may have been more responsive to our intervention. It is also important to note modifications made to the Mediterranean diet, which may have influenced our results. Firstly, the addition of pork increased red meat consumption. Although the change was not significant, higher red meat intake is not characteristic of a traditional Mediterranean diet(Reference Davis, Bryan and Hodgson1). Fresh lean pork was included to assist with compliance and to provide an alternative meat source to beef, Australia’s main source of red meat. This choice was also supported by a study conducted by our research group, which found that replacing chicken with pork has positive cardiometabolic outcomes(Reference Murphy, Thomson and Coates19). Notwithstanding, the MedPork intervention aimed to reduce total meat intake and promote consumption of meat alternatives. In Australia, average meat consumption is 800 g/week(12). During the MedPork intervention, participants were advised to consume no more than 400 g/week. Participants were also monitored to ensure they consistently consumed legumes, seafood, and nuts and seeds, along with other traditional components of the diet. The present study also modified EVOO recommendations to suit an Australian population. Although our guidelines were lower than traditional values, participants increased their EVOO consumption (teaspoons/MJ) 5-fold between baseline and week 8. Consistent with the adoption of Mediterranean dietary principles, participants significantly increased MUFA intake and improved MUFA:SFA ratio. Further, at week 8 of the MedPork intervention, macronutrient ratios were consistent with that of a Mediterranean diet (approximately 40 % energy from fat, approximately 40 % energy from carbohydrates and approximately 20 % energy from protein). The shift in dietary intake was captured by the MDS and MedPork adherence score. Interestingly, the MDS increased by 2 points between baseline and week 8, while the MedPork adherence score increased by 7·5 points. This difference is probably due to the information captured by each score: the MDS is based on actual dietary intake, measured in grams, while the MedPork adherence score assesses overall adherence to dietary principles. Further, the MDS penalises meat consumption, while the MedPork adherence score was tailored to accommodate the inclusion of pork.
With regard to study design, the provision of study foods during the MedPork intervention probably contributed to the level of adherence to the intervention and may limit generalisability. The design of the LF intervention may not reflect current LF dietary recommendations in Australia. Since the study’s conceptions, dietary guidelines for heart health have been updated and now include advice to consume healthy fats from nuts, seeds, fish and olive oil(37). In light of these limitations, future investigations should consider clinical populations, higher consumption of EVOO, longer time periods, feasibility of adherence without the provision of food supplies and a control that is reflective of current dietary habits in Australia.
To reduce the burden of CVD, health and lifestyle interventions with the potential to mitigate multiple risk factors have been recommended above reactive, costly treatments(Reference Mendis, Puska and Norrving38, Reference Norton, Matthews and Barnes39). Interventions like the Mediterranean diet may be effective in reducing incidence and prevalence of CVD. However, it is necessary to ensure that such interventions are suitable for the target population. The present study employed a rigorous design to evaluate the cardiovascular effects of a modified Mediterranean diet developed for an Australian population.
Both the MedPork and LF interventions led to similar improvements across blood pressure measures. This indicates that the MedPork intervention has a similar cardiovascular risk profile to an LF diet and can be adhered to by an Australian population at risk of CVD. These findings are relevant at both an individual and policy level and provide insight regarding future dietary recommendations for individuals in the general community. Longer intervention trials with larger sample sizes are now required to demonstrate the longer-term feasibility and clinical effectiveness of the MedPork intervention in a population with elevated blood pressure.
Acknowledgements
The authors would like to thank Louise Massie for clinical trials support. We would also like to acknowledge the following organisations for their generous contributions: Almond Board of Australia for the donation of almonds; Cobram Estate for the donation of Australian EVOO; and Simplot Australia Pty Ltd for the donation of legumes, tuna and salmon.
The present study was funded by the Pork Cooperative Research Centre (no. 3B-113). The Pork CRC had no role in the study design, implementation, analysis or interpretation of data. A. T. W. was supported by an Australian Government Research Training Program (RTP) Scholarship. J. M. H. was supported by a National Health and Medical Research Council Senior Research Fellowship and a Royal Perth Hospital Medical Research Foundation Fellowship.
K. J. M., J. M. H., A. T. W. and C. R. D. designed the project. K. J. M. and C. R. D. developed the dietary interventions. K. J. M., A. T. W., J. M. H. and C. R. D. developed the cardiovascular measures. R. J. W. contributed to the study design and developed the statistical approach. K. A. D. contributed to the study design. K. J. M., A. T. W., K. A. D. and C. R. D. conducted the trial and collected study data. A. T. W. prepared the manuscript. All authors reviewed manuscript drafts and approved the final version.
None of the authors has any conflicts of interest to declare.
Supplementary material
For supplementary material/s referred to in this article, please visit https://doi.org/10.1017/S0007114519001168