Defined as ‘a potential consequence of food insecurity that, because of prolonged, involuntary lack of food, results in discomfort, illness, weakness, or pain that goes beyond the usual uneasy sensation’(1,Reference Norwood and Wunderlich2) , hunger affected an estimated 733 million people globally in 2023(1). Among those affected, children are especially vulnerable to hunger(3), with approximately 45 % of all deaths among children under 5 years of age linked to hunger-related concerns(4). Adequate nutrition, particularly in the first 1000 d of life, is thus widely recognised as critical for children’s physical, cognitive and psychological development, as well as long-term health(4–Reference Ooi, Abdul Jalal and Wong7). Children experiencing hunger are at heightened risk of poor health outcomes, including more frequent illnesses and infections, increased rates of hospitalisation(Reference Ooi, Abdul Jalal and Wong7–Reference Kirkpatrick, McIntyre and Potestio11) and higher odds of asthma and other chronic conditions(Reference Kirkpatrick, McIntyre and Potestio11). Moreover, childhood hunger is associated with an increased risk of mental health difficulties during adolescence, including depression and suicidal ideation(Reference McIntyre, Williams and Lavorato12). Beyond individual health consequences, child hunger and undernutrition impose significant economic burdens at the societal level. For example, the estimated annual economic cost of child undernutrition is approximately $600 million in Malawi and $4·7 billion in Ethiopia(Reference McConville13).
Given the profound health and economic consequences of hunger, global efforts have been directed towards its eradication by 2030, as reflected in Sustainable Development Goal (SDG) 2(14). Today, the prevalence of hunger among children varies widely across countries, from as low as 3·0 % in Australia(Reference Baker, Gallegos and MacKenzie6) to as high as 58·4 % in Malawi(Reference Ooi, Abdul Jalal and Wong7). Global crises such as armed conflicts, climate change, economic instability and health pandemics, however, are known to exacerbate food insecurity and its impact on child hunger and malnutrition(Reference Shemyakina15,16) . For example, the current humanitarian crisis in Gaza has underscored the devastating effects of conflict on child nutrition, as nearly 75 % of children in food-insecure households reportedly went to bed hungry in 2024(Reference Horino, Zaqqout and Habash17). The Central African Republic, which has also experienced prolonged conflict and displacement, recorded the highest Global Hunger Index rate in 2023, with one in twenty children reportedly dying before their fifth birthday and 5 % of children suffering from wasting(16). Similarly, Madagascar, which is severely affected by the impacts of climate change, ranked second on the Global Hunger Index, with a child mortality rate of 6·6 in 2023(16). More recently, cuts to funding for humanitarian assistance are expected to further undermine global responses to food insecurity and contribute to rising rates of child hunger in the coming years(Reference Locks, Stewart and Hoffman18). Amid escalating global food insecurity, a clear understanding of how child hunger is conceptualised and addressed is critical to guide the design, implementation and scale-up of effective child nutrition interventions. Existing programmes targeting child hunger adopt varying approaches to its conceptualisation and measurement, with some equating child hunger with malnutrition or food insecurity. While these concepts are closely related(Reference Norwood and Wunderlich2), using them interchangeably can result in misaligned policies and ineffective interventions. Food insecurity, for instance, is a household-level construct which reflects whether a family has consistent access to adequate food and does not necessarily capture the individual experiences of hunger, particularly among children(Reference Norwood and Wunderlich2). Within food-insecure households, for example, parents may try to shield children from hunger by prioritising their child’s food intake. Child hunger may therefore be a separate and more severe indicator of food insecurity(Reference Steyer, Townley-Flores and Sulik19). Failing to distinguish between the two, however, obscures the true extent of child hunger and can result in interventions that fail to target the children most in need.
Aware of this gap, a panel convened by the US Committee on National Statistics (CNSTAT) recommended that child hunger and household food insecurity be measured separately, concluding that for valid measurement of hunger, it is essential to first define and operationalise child hunger(Reference Norwood and Wunderlich2). This clarity in the conceptualisation of child hunger would facilitate more accurate and consistent measurement across contexts and over time, thereby supporting the implementation and evaluation of programmes aimed at reducing child hunger. However, limited research has investigated whether and, if so, how these recommendations have been reflected in child nutrition research over the past two decades. To address this gap, we conducted a review of the literature on ‘child hunger’ to examine how it is most commonly conceptualised and measured. This review was guided by the following research questions: (i) How is child hunger defined and conceptualised? and (ii) which questionnaires are commonly used to measure child hunger?
Methods
Recommended for the production of timely evidence for decision-making(Reference Garritty, Gartlehner and Nussbaumer-Streit20), we conducted a pre-registered rapid review in accordance with the Interim Guidance by the Cochrane Rapid Reviews Methods Group(Reference Garritty, Gartlehner and Nussbaumer-Streit20). Findings are reported in line with the PRISMA guidance for systematic reviews(Reference Page, McKenzie and Bossuyt21), as the PRISMA extension for rapid reviews is currently under development.
Eligibility criteria
We included peer-reviewed articles and grey literature reports that focused on hunger among children aged 0–18 years. To be included, papers had to mention the terms ‘child hunger’ or ‘child’ and ‘hunger’ together or in close proximity. Articles were excluded if they did not provide either a definition of child hunger or a description of the methods used to measure child hunger in the study. The full inclusion and exclusion criteria are shown in Table 1.
Table 1. Inclusion and exclusion criteria

Information sources and search strategy
We searched for peer-reviewed literature published from 2006 onwards across six electronic databases: Web of Science, MEDLINE, Embase, PsycINFO, Social Science Database and ERIC. The search strategy for the review included keywords for the population (children 18 years or younger) and the condition under study (child hunger). The search strategy was developed with the assistance of GS, a subject librarian. The initial search was conducted in January 2024 and subsequently updated in February 2025, with newly identified records imported into the existing Covidence account used for this review. Annex 1 contains an example search strategy formatted for Web of Science.
As per the Cochrane guidelines for rapid reviews, a comprehensive grey literature search is not required for rapid review(Reference Garritty, Gartlehner and Nussbaumer-Streit20). However, given that child hunger is a key priority area for numerous global and non-profit organisations, a targeted grey literature search was considered essential to identify reports specifically addressing the conceptualisation, evaluation or measurement of ‘child hunger’. Accordingly, a systematic grey literature search was conducted on the websites of the following organisations: WHO, UNICEF, Scaling Up Nutrition, GAIN Health, ReliefWeb, World Food Programme, Save the Children, Akshaya Patra, Feeding America, Action Against Hunger, The Hunger Project, Care, Food for the Hungry, Caritas, Mercy Corps, Inter-agency Network for Education in Emergencies, Global Hunger Index, Global Nutrition Report, Core Group, Emergency Nutrition Network and Advancing Nutrition. These organisations were selected in collaboration with non-profit organisations implementing nutrition programmes aimed at addressing child hunger.
Study selection
Search results for peer-reviewed literature retrieved from electronic databases were imported into Covidence, while grey literature identified through organisational websites was recorded in an Excel spreadsheet. Title and abstract screening, as well as full-text screening, were conducted by AM for the initial search conducted in 2024 and by AW for the updated search conducted in 2025. To ensure quality control and resolve any discrepancies, all results were reviewed and discussed with a third author (KH).
Data extraction and synthesis
A data extraction form was developed in Covidence to systematically collect the following information: author(s) and year of publication, country of study, definitions of child hunger, study methodology, measurement tools used to assess child hunger and demographic characteristics of study participants (age range and gender). Relevant data from peer-reviewed literature were extracted in Covidence, while data from grey literature reports were extracted using Excel. AM independently completed all data extraction for studies included from the 2024 search, while AW extracted data from studies identified through the updated search in 2025. A randomly selected subset of five articles was reviewed by KH to promote rigour.
All extracted data were compiled in Excel for analysis. Data pertaining to the definitions of child hunger, measurement methods and studied population groups were analysed using narrative synthesis. Relevant fields were inductively coded and categorised under emerging themes to narratively describe the key patterns within the data.
Quality assessment
Given that this rapid review was focused on mapping concepts and methodologies related to child hunger rather than evaluating the effectiveness of interventions, a quality assessment of the included studies was not conducted. The decision to include studies regardless of quality allowed for a more comprehensive and inclusive assessment of how research studies define and measure child hunger.
Results
We included a total of sixty-seven eligible studies from the initial 2165 reports identified from the electronic databases and other sources. Figure 1 summarises the study selection process.

Figure 1. PRISMA flow chart.
Sample characteristics
Most studies were conducted in the USA (n 19), followed by Malaysia (n 9), Canada (n 8) and South Africa (n 4) (Table 2).
Table 2. Included studies (n 67)

Conceptualisation of child hunger
Out of the sixty-seven studies included in the review, twenty-three provided a specific definition of child hunger (see Table 3). Several key themes emerged from these definitions.
Table 3. Child hunger definitions extracted from included articles (n 23)

The text included in the column to the right is directly quoted from the included article.
Centrality of food insecurity, quantity and quality
A total of twenty studies defined child hunger as being associated with a lack of access to food or food insecurity(Reference Ooi, Abdul Jalal and Wong7,Reference Kirkpatrick, McIntyre and Potestio11,Reference Apodaca22–Reference Zhang, Su and Li39) . Among these, fifteen studies conceptualised child hunger as an outcome of food insecurity(Reference Ooi, Abdul Jalal and Wong7,Reference Kirkpatrick, McIntyre and Potestio11,Reference Apodaca22–Reference Hicks, Nelson and Rhoads25,Reference Kersey, Geppert and Cutts28–Reference Smith, López Sánchez and Tully35,Reference Weffort and Lamounier37) , while five studies equated child hunger directly with food insecurity(Reference Haque, Farzana and Sultana26,Reference Jones, Draper and Bell27,Reference Tam, Findlay and Kohen36,Reference Wong, Moy and Nair38,Reference Zhang, Su and Li39) . This pattern reflects a conceptual model whereby child hunger is both a symptom and an extreme manifestation of inadequate food access.
In addition, eleven studies defined child hunger as inadequate food consumption. Nine of these studies consistently identified reduced or insufficient food intake, often reflected in smaller meal portions or skipped meals, as a core indicator of childhood hunger(Reference Azhar, Ross and Keller23,Reference Haque, Farzana and Sultana26,Reference Jones, Draper and Bell27,Reference McIntyre, Bartoo and Pow30,Reference Naser, Jalil and Muda31,Reference Sharkey, Dean and Nalty33,Reference Weffort and Lamounier37,Reference Li, Guo and Zhang40,Reference Depboylu and Şimşek41) . A subset of these studies also emphasised the role of decreased food quality as a contributing factor to childhood hunger(Reference Jones, Draper and Bell27,Reference Depboylu and Şimşek41) . In these studies, low food quality was characterised in two ways: first, as a lack of dietary variety(Reference Jones, Draper and Bell27), and second, as the consumption of foods deficient in essential nutrients and vitamins, resulting in hidden hunger(Reference Weffort and Lamounier37,Reference Depboylu and Şimşek41) .
Physiological dimensions of child hunger
The underlying physical and psychological aspects of child hunger were highlighted in definitions used in ten studies(Reference Ooi, Abdul Jalal and Wong7,Reference Ecker and Sifers24,Reference Hicks, Nelson and Rhoads25,Reference Kersey, Geppert and Cutts28,Reference Liu, Fu and Zhang29,Reference Romo, Abril-Ulloa and Kelvin32–Reference Smith, López Sánchez and Tully35,Reference Stevenson, Serebro and Mruk42) . Amongst these ten studies, the predominant focus was on physiological framing of hunger(Reference Ecker and Sifers24,Reference Hicks, Nelson and Rhoads25,Reference Romo, Abril-Ulloa and Kelvin32) evidenced by definitions describing hunger as an ‘uneasy or painful sensation’(Reference Ooi, Abdul Jalal and Wong7,Reference Kersey, Geppert and Cutts28,Reference Liu, Fu and Zhang29,Reference Smith, López Sánchez and Tully35) , or a state of ‘discomfort, illness, and weakness, or pain that goes beyond the usual uneasy sensation’(Reference Smith and Richards34). Only one study incorporated the psychological dimensions in the definition of childhood hunger, particularly in relation to mental health consequences stemming from chronic hunger(Reference Sharkey, Dean and Nalty33).
Operationalisation of duration or frequency of hunger
The temporal dimension of hunger was inconsistently addressed across the reviewed definitions. Some studies provided specific time frames, such as ‘more than three months’ or ‘within the past month’(Reference Jones, Draper and Bell27,Reference Romo, Abril-Ulloa and Kelvin32) , which may imply a focus on the chronic nature of hunger. In contrast, other definitions used time frames that referred to more episodic experiences of hunger, describing situations in which children were unable to access food even for ‘short periods’(Reference Haque, Farzana and Sultana26). A few studies used vague descriptors such as ‘recurrent or repeated’(Reference Ooi, Abdul Jalal and Wong7,Reference Kersey, Geppert and Cutts28,Reference Liu, Fu and Zhang29) or ‘long-term’ experiences of hunger(Reference Zhang, Su and Li39) without clarifying the precise duration, frequency or severity of hunger episodes.
Individual-level conceptualisation of child hunger
Only three studies explicitly defined childhood hunger as an individual-level construct that was distinct from the household-level construct of food insecurity(Reference Ecker and Sifers24,Reference Hicks, Nelson and Rhoads25,Reference Romo, Abril-Ulloa and Kelvin32) .
Measurement of child hunger
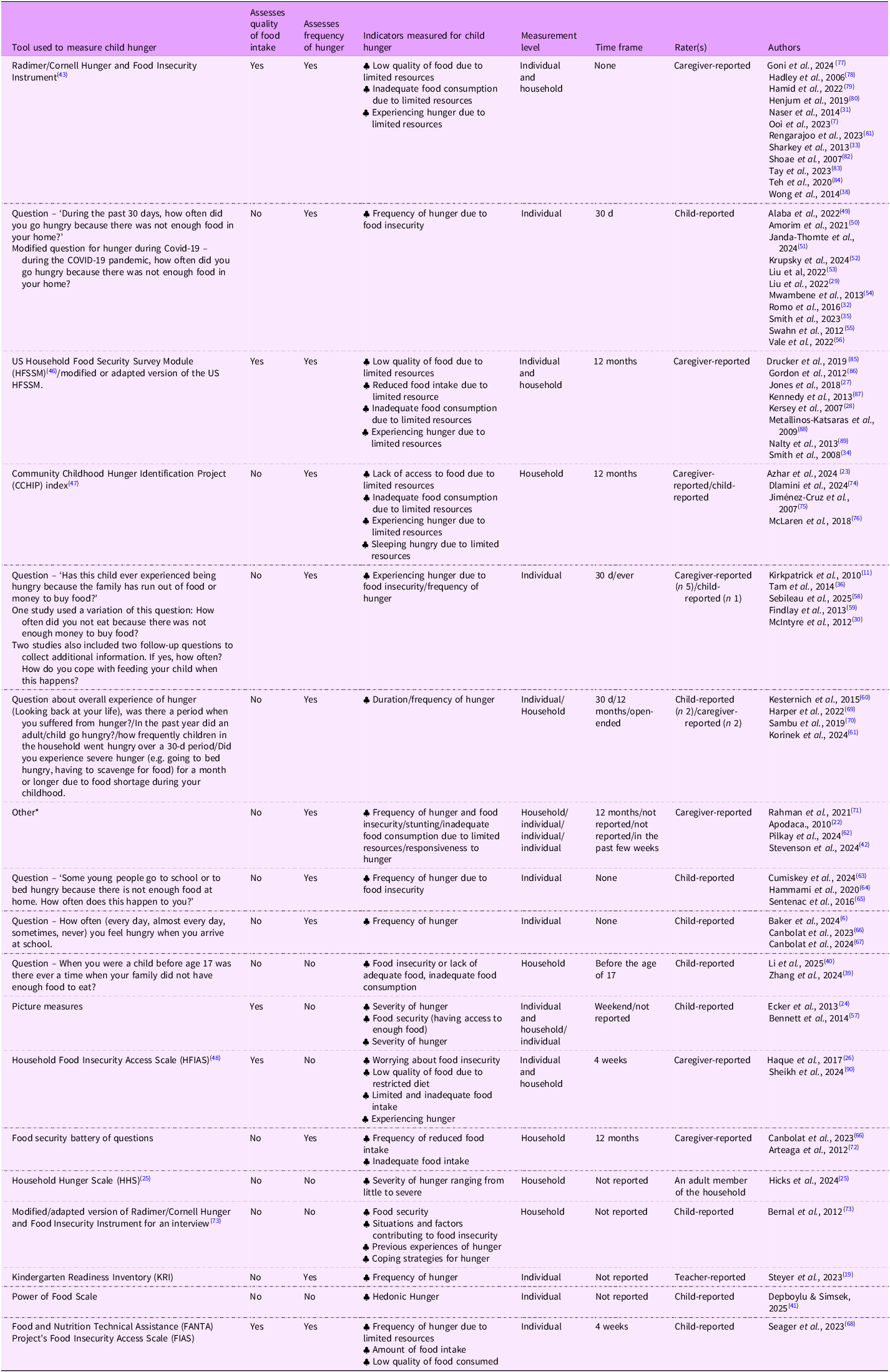
In the included studies, child hunger was assessed using a total of twenty-one measures. These measures are outlined in Table 4.
Table 4. Measures of child hunger

*Rahman et al., 2021 – Structured questionnaire relating to household dietary diversity and household food security was used to collect data from the respondents. The questionnaire was adopted and adapted from various questionnaires based on the study’s objectives. Apodaca et al., 2010 – The prevalence of stunted children under the age of five is used to measure child hunger and malnutrition. Pilkay et al. (2024) asked mothers about the meals missed by children. Stevenson et al. (2024) administered a 25-item measure on caregivers’ attention towards, and response to, their child’s interoceptive hunger and thirst cues.
Overview of the commonly used measures for child hunger
The most frequently used measure in the included studies (n 12) was the Radimer/Cornell Hunger and Food Insecurity Instrument(Reference Radimer, Olson and Campbell43). This instrument includes ten items, with three questions specifically focusing on child hunger: Question 8 relates to the quality of a child’s diet, and questions 9 and 10 focus on the quantity of food intake. Child hunger was assumed if questions 9 and 10 were answered with either ‘sometimes true’ or ‘often true’(Reference Kendall, Olson and Frongillo44,Reference Mohamadpour, Sharif and Keysami45) . Other frequently used and validated survey tools included the US Household Food Security Survey Module (HFSSM)(Reference Gulliford, Nunes and Rocke46) (n 8), the Community Childhood Hunger Identification Project (CCHIP) index(Reference Wehler, Scott and Anderson47) (n 4) and the Household Food Insecurity Access Scale (HFIAS)(Reference Coates, Swindale and Bilinsky48) (n 2). The HFSSM is an eighteen-item questionnaire that measures food security, with ten questions focusing on the quality and quantity of food intake as indicators of child hunger(Reference Gulliford, Nunes and Rocke46). The CCHIP is an eight-item measure that assesses food insecurity and hunger among low-income families with at least one child under the age of 12 years(Reference Wehler, Scott and Anderson47). Four of the CCHIP items are aimed to capture various indicators of child hunger resulting from food insecurity. The HFIAS is a nine-item tool that assesses both food insecurity and the resulting child hunger manifested in the form of reduced food intake, consumption of low-quality food restricted in variety and disrupted eating patterns(Reference Coates, Swindale and Bilinsky48).
Twenty-eight studies assessed child hunger using a single-item measure. The most commonly used one-item measure was: ‘During the past 30 days, how often did you go hungry because there was not enough food in your home?’ (n 11)(Reference Liu, Fu and Zhang29,Reference Romo, Abril-Ulloa and Kelvin32,Reference Smith, López Sánchez and Tully35,Reference Alaba, Hongoro and Thulare49–Reference Vale, Santos and Dantas56) . Possible responses were ‘never’, ‘rarely’, ‘sometimes’, ‘most of the time’ and ‘always’. Two surveys used words and pictures to measure child hunger among school students. Bennett et al. (2014)(Reference Bennett and Blissett57). developed a picture rating scale that consisted of five cartoon bears with different amounts of food in their stomachs, represented by black ovals. The ovals would increase in size in proportion to the amount of food consumed and the bear’s level of satisfaction. Each of the cartoon bears were accompanied by a label to describe the bear’s level of hunger, starting from ‘very hungry’ to ‘not hungry at all’(Reference Bennett and Blissett57). Similarly, Ecker et al. (2013)(Reference Ecker and Sifers24) used a hunger survey that contained words and pictures to make it easier for all participants to understand the survey as some students were English Language Learner students or were unable to read. This study used labelled cartoon faces to depict hunger and satiety from 1 ‘not hungry’, 2 ‘a little hungry’ to 3 ‘very hungry’(Reference Ecker and Sifers24).
Measurement levels and time frames
A total of twelve scales were used across thirty-one studies(Reference Baker, Gallegos and MacKenzie6,Reference Kirkpatrick, McIntyre and Potestio11,Reference Steyer, Townley-Flores and Sulik19,Reference Apodaca22,Reference Liu, Fu and Zhang29,Reference McIntyre, Bartoo and Pow30,Reference Romo, Abril-Ulloa and Kelvin32,Reference Smith, López Sánchez and Tully35,Reference Tam, Findlay and Kohen36,Reference Depboylu and Şimşek41,Reference Stevenson, Serebro and Mruk42,Reference Alaba, Hongoro and Thulare49–Reference Seager, Baird and Kalow68) to measure child hunger at the individual child level. Of these, seven scales used in twenty-two studies were self-rated by children(Reference Baker, Gallegos and MacKenzie6,Reference Liu, Fu and Zhang29,Reference Romo, Abril-Ulloa and Kelvin32,Reference Smith, López Sánchez and Tully35,Reference Depboylu and Şimşek41,Reference Alaba, Hongoro and Thulare49–Reference Bennett and Blissett57,Reference Kesternich, Siflinger and Smith60,Reference Korinek, Zimmer and Teerawichitchainan61,Reference Cumiskey, Patte and Michaelson63–Reference Seager, Baird and Kalow68) , one questionnaire in a single study was rated by teachers(Reference Steyer, Townley-Flores and Sulik19) and three measures used in three studies were completed by caregivers(Reference Apodaca22,Reference Stevenson, Serebro and Mruk42,Reference Pilkay, Nolasco and Nunes62) . One measure was completed by children in one study(Reference Sebileau, Swinburn and De Seymour58) and by caregivers in four studies(Reference Kirkpatrick, McIntyre and Potestio11,Reference McIntyre, Bartoo and Pow30,Reference Tam, Findlay and Kohen36,Reference Findlay, Langlois and Kohen59) . At the household level, seven scales were used to assess food insecurity and child hunger in thirteen studies(Reference Azhar, Ross and Keller23,Reference Hicks, Nelson and Rhoads25,Reference Zhang, Su and Li39,Reference Li, Guo and Zhang40,Reference Canbolat, Rutkowski and Rutkowski66,Reference Harper, Goudge and Chirwa69–Reference McLaren, Steenkamp and Feeley76) . Among these, four questionnaires were rated by caregivers in six studies(Reference Hicks, Nelson and Rhoads25,Reference Canbolat, Rutkowski and Rutkowski66,Reference Harper, Goudge and Chirwa69–Reference Arteaga, Heflin and Gable72) , two measures were child-rated in three studies(Reference Zhang, Su and Li39,Reference Li, Guo and Zhang40,Reference Bernal, Frongillo and Herrera73) , while one tool was completed by either children or caregivers in four studies(Reference Azhar, Ross and Keller23,Reference Dlamini, Mtintsilana and Craig74–Reference McLaren, Steenkamp and Feeley76) .
Twenty-three studies measured food insecurity and child hunger at both the individual and household levels simultaneously(Reference Ooi, Abdul Jalal and Wong7,Reference Ecker and Sifers24,Reference Haque, Farzana and Sultana26–Reference Kersey, Geppert and Cutts28,Reference Naser, Jalil and Muda31,Reference Sharkey, Dean and Nalty33,Reference Smith and Richards34,Reference Wong, Moy and Nair38,Reference Goni, Aroyehun and Razak77–Reference Sheikh, Barolia and Habib90) , using four different questionnaires. Three of these scales were rated by caregivers in twenty-two studies(Reference Ooi, Abdul Jalal and Wong7,Reference Haque, Farzana and Sultana26–Reference Kersey, Geppert and Cutts28,Reference Naser, Jalil and Muda31,Reference Sharkey, Dean and Nalty33,Reference Smith and Richards34,Reference Wong, Moy and Nair38,Reference Goni, Aroyehun and Razak77–Reference Sheikh, Barolia and Habib90) , while one scale was child-rated in a single study(Reference Ecker and Sifers24). The time frames used to measure child hunger varied widely across studies. The most frequently used reference periods were the past 12 months (n 15)(Reference Azhar, Ross and Keller23,Reference Jones, Draper and Bell27,Reference Kersey, Geppert and Cutts28,Reference Smith and Richards34,Reference Harper, Goudge and Chirwa69,Reference Rahman, Seling and Kiyu71,Reference Arteaga, Heflin and Gable72,Reference Dlamini, Mtintsilana and Craig74–Reference McLaren, Steenkamp and Feeley76,Reference Drucker, Liese and Sercy85–Reference Nalty, Sharkey and Dean89) and the past 30 d (n 15)(Reference Haque, Farzana and Sultana26,Reference Liu, Fu and Zhang29,Reference Romo, Abril-Ulloa and Kelvin32,Reference Smith, López Sánchez and Tully35,Reference de Amorim, Junior and Gonçalves50,Reference Krupsky, Sliwa and Seligman52–Reference Vale, Santos and Dantas56,Reference Sebileau, Swinburn and De Seymour58,Reference Korinek, Zimmer and Teerawichitchainan61,Reference Seager, Baird and Kalow68,Reference Sambu and Hall70,Reference Sheikh, Barolia and Habib90) , though other recall periods were also used in studies.
Constructs measured by the child hunger measures
Five key constructs were captured by the scales used in the included studies: food insecurity and hunger (n 11), hunger (n 7), food insecurity (n 2), hedonic hunger (n 1) and stunting (n 1) (Table 4). These five constructs were measured using nine distinct indicators (online Supplementary Table 1). Most of these scales (n 14) claimed to assess the overall experience of hunger among children without defining or operationalising hunger. In nine of these scales, hunger was defined as a consequence of food insecurity or resulting from a lack of resources to acquire food.
Discussion
This rapid review aimed to explore how ‘child hunger’ is currently conceptualised and measured, identifying considerable methodological variation and inconsistencies in the definitions and measurement of child hunger across included studies. First, most studies defined and measured child hunger as a consequence of food insecurity. This is aligned with the results from a previous review examining various measures of food insecurity, where most questionnaires were found to include items on child hunger as an indicator of food insecurity(Reference Taylor, Baker and Gallegos91). A few studies used ‘child hunger’ and ‘food insecurity’ interchangeably in their definitions of child hunger(Reference Haque, Farzana and Sultana26,Reference Jones, Draper and Bell27,Reference Tam, Findlay and Kohen36,Reference Wong, Moy and Nair38,Reference Zhang, Su and Li39) . This conflation is highly contested in the literature, as some studies argue that ‘hunger’ manifests only in cases of very low food security(92), while others, such as Steyer et al. (Reference Steyer, Townley-Flores and Sulik19), contend that children may be shielded from hunger by adults even in households experiencing high food insecurity. The latter perspective aligns with the recommendations of the CNSTAT, which advocated for the distinct conceptualisation and measurement of hunger and food insecurity(Reference Norwood and Wunderlich2). Consistent with this guidance, most scales either assessed hunger (n 7) or food insecurity (n 2) or measured both constructs as related yet distinct concepts (n 11).
CNSTAT further recommended the need to operationalise hunger to enable consistent and valid measurement(Reference Norwood and Wunderlich2). Among the studies that provided an operationalised definition of hunger, most (n 9) focused on quantitative indicators such as number of meals skipped, portion size reductions or the number of days a child lacked adequate food, while the quality of food consumed was rarely discussed(Reference Jones, Draper and Bell27,Reference Depboylu and Şimşek41) . This pattern is similarly reflected in the measurement of child hunger, with most scales assessing the amount of food intake. This disproportionate emphasis on quantity-based indicators of child hunger over the quality of food consumed is consistent with a conceptualisation of hunger that fails to take into account ‘hidden hunger’; adequate access and intake of nutrient-poor foods may shield children from overtly experiencing hunger, yet leaves them vulnerable to stunting, cognitive delays and a weakened immune system(Reference Weffort and Lamounier37). Consequently, micronutrient deficiencies characteristic of hidden hunger are not captured in measurement tools solely focused on food access or quantity of food intake.
Notably, while physiological sensations associated with hunger, such as stomach pain, uneasy feeling or fatigue, were referenced in the definitions provided by ten studies(Reference Ooi, Abdul Jalal and Wong7,Reference Ecker and Sifers24,Reference Hicks, Nelson and Rhoads25,Reference Kersey, Geppert and Cutts28,Reference Liu, Fu and Zhang29,Reference Romo, Abril-Ulloa and Kelvin32–Reference Smith, López Sánchez and Tully35,Reference Stevenson, Serebro and Mruk42) , none of the scales directly measured these experiences. These omissions reflect a lack of regard for children’s subjective experiences of hunger as the physiological, cognitive and emotional aspects of hunger have been reported to be more salient to children themselves(Reference Fram, Frongillo and Jones93). Including child-reported physical and emotional indicators could improve both sensitivity and relevance of child hunger assessments. These methodological gaps in operationalisation and assessment of child hunger across studies underscore the need for more comprehensive and standardised approaches that account for the multidimensional nature of child hunger, including quantity, quality, severity, and physiological and emotional impacts of hunger.
The most common approach to measure child hunger was the use of a single question linking the experience of hunger to insufficient quantities of food in the home. While this approach was frequently used with child respondents for feasibility of administration and minimal participant burden, it has been critiqued for oversimplifying the operationalisation and measurement of hunger(Reference Taylor, Baker and Gallegos91). As discussed above, hunger as a complex construct with a range of indicators uniquely associated with social, physiological and structural dimensions of hunger is not likely captured through the use of single-item measures.
Another key inconsistency was the temporality of hunger across definitions and measurement approaches in the included studies. While some definitions and measures referred to episodic or short-term hunger(Reference Haque, Farzana and Sultana26), most focused on chronic or long-term experiences of hunger among children(Reference Jones, Draper and Bell27,Reference Romo, Abril-Ulloa and Kelvin32,Reference Zhang, Su and Li39) . Similarly, the measures employed a range of reference periods, from short-term intervals (e.g. past weekend, past 7 d or past 30 d)(Reference Azhar, Ross and Keller23,Reference Jones, Draper and Bell27,Reference Kersey, Geppert and Cutts28,Reference Smith and Richards34,Reference Harper, Goudge and Chirwa69,Reference Rahman, Seling and Kiyu71,Reference Arteaga, Heflin and Gable72,Reference Dlamini, Mtintsilana and Craig74–Reference McLaren, Steenkamp and Feeley76,Reference Drucker, Liese and Sercy85–Reference Nalty, Sharkey and Dean89) to longer-term periods (e.g. the past 12 months)(Reference Haque, Farzana and Sultana26,Reference Liu, Fu and Zhang29,Reference Romo, Abril-Ulloa and Kelvin32,Reference Smith, López Sánchez and Tully35,Reference de Amorim, Junior and Gonçalves50,Reference Krupsky, Sliwa and Seligman52–Reference Vale, Santos and Dantas56,Reference Sebileau, Swinburn and De Seymour58,Reference Korinek, Zimmer and Teerawichitchainan61,Reference Seager, Baird and Kalow68,Reference Sambu and Hall70,Reference Sheikh, Barolia and Habib90) . Despite its implications for practice, the importance of clearly defining the temporality of child hunger is often overlooked in the literature. For example, a child who is hungry only during school holidays v. one who is persistently underfed all year would both count as ‘food-insecure’ using a 12-month measure, despite their need for different interventions. To address this, future research should desegregate hunger experiences by duration and frequency, distinguishing between acute, intermittent and chronic hunger. Additionally, studies should assess contextual factors contributing to fluctuations in food access and resulting child hunger (e.g. school closures, seasonal income changes or household shocks) to better target interventions based on the timing and persistence of child hunger.
The level of measurement was rarely conceptualised in the definitions of child hunger, with only three studies explicitly defining it as an individual-level construct(Reference Ecker and Sifers24,Reference Hicks, Nelson and Rhoads25,Reference Romo, Abril-Ulloa and Kelvin32) . However, the administration of child hunger scales varied across studies. Those aiming to assess hunger at the individual child level typically included children as respondents(Reference Baker, Gallegos and MacKenzie6,Reference Liu, Fu and Zhang29,Reference Romo, Abril-Ulloa and Kelvin32,Reference Smith, López Sánchez and Tully35,Reference Depboylu and Şimşek41,Reference Alaba, Hongoro and Thulare49–Reference Bennett and Blissett57,Reference Kesternich, Siflinger and Smith60,Reference Korinek, Zimmer and Teerawichitchainan61,Reference Cumiskey, Patte and Michaelson63–Reference Seager, Baird and Kalow68) , whereas studies examining both food insecurity and hunger at the household level predominantly relied on caregiver-reported measures(Reference Hicks, Nelson and Rhoads25,Reference Canbolat, Rutkowski and Rutkowski66,Reference Harper, Goudge and Chirwa69–Reference Arteaga, Heflin and Gable72) . This finding is consistent with a recent scoping review on food insecurity, which reported that the measurement of child food insecurity has ‘predominantly [been] reported by adult respondents on behalf of children’(Reference Taylor, Baker and Gallegos91). This raises critical questions about whose perspectives are being captured in the assessment of child hunger and food insecurity. Research increasingly shows that children may have distinct experiences of food insecurity that may not be fully known or reported by adults in the household(Reference Taylor, Baker and Gallegos91,Reference Fram, Frongillo and Jones93) . Children, for example, have been found to be acutely aware of household food shortages and may internalise or hide their experiences of hunger and food insecurity to protect their caregivers(Reference Bernal, Frongillo and Herrera73,Reference Fram, Frongillo and Jones93,Reference Frongillo, Fram and Ghattas94) . As such, relying solely on caregiver reports may obscure children’s lived realities(Reference Fram, Frongillo and Jones93) and underestimate the true prevalence of hunger and food insecurity among children(Reference Taylor, Baker and Gallegos91). To address this gap, future research should prioritise the inclusion of both child-and caregiver-reported measures. Using parallel instruments at both the individual and household levels can offer a more comprehensive and reliable understanding of child hunger and food insecurity(Reference Taylor, Baker and Gallegos91).
Beyond measurement challenges, geographic gaps were also observed. Most of the included studies were conducted in the USA, Canada, Malaysia and South Africa. While child hunger is a global challenge, the countries with the highest prevalence of food insecurity in 2023 were Somalia, Afghanistan, Syrian Arab Republic, Haiti, Yemen, Sierra Leone, Nigeria, Liberia, Mauritania, Central African Republic, Lesotho and Vanuatu(95). Countries with the highest prevalence of childhood obesity, on the other hand, include the Cook Islands, Wallis and Futuna, Niue, Tonga, and Samoa, among other countries of Polynesia and Micronesia(96). However, our review did not find any relevant studies conducted in these countries. Future research should be prioritised in countries with high levels of food insecurity and child hunger.
The current review is not without limitations. Only English language studies were included, which could have resulted in the exclusion of potentially relevant studies. Additionally, the inclusion of only a small number of NGO reports (n 3) may reflect the specificity of our narrowly focused inclusion criteria. Lastly, this rapid review used single-reviewer screening and data extraction, with a second reviewer checking a subset of studies, and did not include a formal quality assessment. These choices may limit the comprehensiveness of the study selection process and preclude conclusions regarding the quality of included studies; however, they are unlikely to introduce systematic bias because the review focuses on identifying and describing the range of methods used to measure child hunger, rather than estimating effects or evaluating the comparative performance of different approaches. Furthermore, the use of a pre-registered protocol, systematic searches across multiple databases and standardised study selection process support the validity of the findings. Results should be interpreted in light of these considerations.
Conclusion
This rapid review sought to understand what is meant by ‘child hunger’ and how it is measured through a rapid and systematic investigation of research. Despite recommendations from CNSTAT to clearly define and operationalise child hunger and to differentiate between child hunger and household food insecurity, these principles are inconsistently applied in extant child hunger research. Our review highlights persistent and significant variations in how child hunger is conceptualised and measured across studies, with differences in definitions, reference periods, levels of reporting and the inclusion of key dimensions such as quantity, quality, severity and temporality. Moreover, the dominance of caregiver-reported measures raises concerns about the extent to which children’s unique experiences are accurately captured. To advance research and policy, future work should prioritise child-centred, culturally relevant tools that reflect both the multiple dimensions and lived experience of child hunger.
Supplementary material
For supplementary material accompanying this paper visit https://doi.org/10.1017/S1368980026102195
Acknowledgements
None
Author contributions
A. M.: Data curation, Formal analysis and Writing – Original draft. F. V.: Conceptualisation, Project administration, Methodology and Writing – Review and Editing. G. S.: Data curation, Methodology and Writing – Review and Editing. M. S.: Conceptualisation, Project administration, Methodology and Writing – Review and Editing. S. G.: Conceptualisation, Project administration, Methodology and Writing – Review and Editing. A. G. – Conceptualisation and Writing – Review and Editing. K. H.: Conceptualisation, Project administration, Methodology, Writing – Review and Editing and Supervision. A. W.: Data curation, Formal analysis and Writing – Review and Editing.
Financial support
This work was graciously supported by World Vision Ireland’s NOURISH (Nature-based Opportunities Underpinning Resilient Sustainable Households) project, supported by the Department of Foreign Affairs/Irish Aid under Ireland’s Civil Society Partnership for A Better World 2023–2027. The contents of this document are the responsibility of the author(s) and do not necessarily reflect the views of Irish Aid. Irish Aid had no role in the study design, analysis, manuscript preparation and revision and publication decisions for this article.
Competing interests
There are no conflicts of interest.