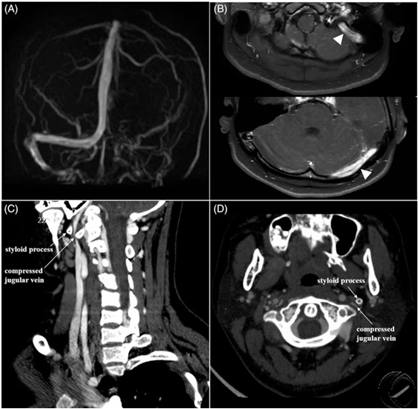
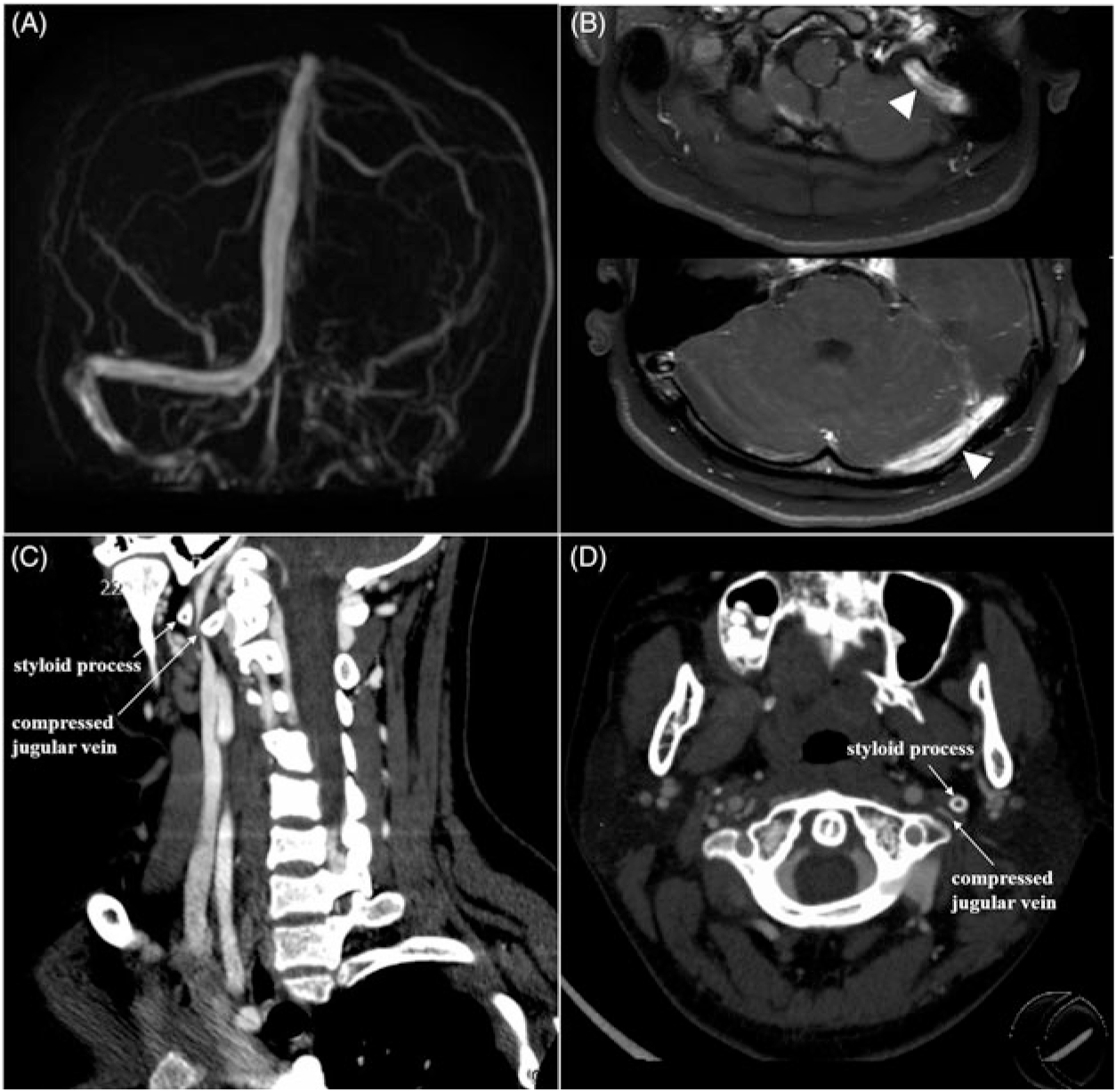
A 15-year-old teenager presented with a 2-month history of headache. Neurological examination was normal except for papilledema. Further lumbar puncture indicated intracranial hypertension (330 mm H2O). Brain magnetic resonance imaging (MRI) was normal but phase contrast-magnetic resonance venography (PC-MRV) (Figure 1(A)) suggested possible left transverse-sigmoid sinus thrombosis; subsequent contrast-enhanced 3D fat-saturated T1 volumetric isotropic turbo spin echo acquisition (VISTA) MRI (Figure 1(B)) confirmed the pathology. Hyper-coagulable panel results (including six steroid sex hormones, antithrombin III, protein C, protein S, lupus anticoagulant, and anticardiolipin antibodies) were all within normal range. In further examination, computed tomography (CT) venography images (Figure 1(C) and (D)) showed that the left jugular vein was compressed by the styloid process, consistent with Eagle syndrome.Reference Badhey, Jategaonkar and Anglin Kovacs1 The patient who refused the recommended surgical treatment, however, chose anticoagulant therapy consisting of low-molecular weight heparin subcutaneous injection in addition to new oral anticoagulant. At 18-month follow-up, the patient reported no symptoms remained.
Neurological imaging examinations of the patient. PC-MRV (A) showed absent signal in the left transverse-sigmoid sinuses. Contrast-enhanced 3D fat-saturated T1 VISTA MRI (B; white arrowheads) demonstrated gadolinium enhancement of the left transverse-sigmoid sinuses, indicating chronic venous sinus thrombosis. The curved planar reformation (CPR) and axial source images from CT venography images (C and D; white arrow) showed styloid process compressing the left jugular vein.
Eagle syndrome, also known as styloid syndrome, was initially described by Watt Weems Eagle in 1937; it often presented with cervical pain on the side of the elongated styloid process, foreign-body sensation in the throat, and dysphagia.Reference Eagle2 In addition, it can cause transient ischemic attacks or stroke due to cervical internal carotid artery compression.Reference Badhey, Jategaonkar and Anglin Kovacs1 However, cases of Eagle syndrome causing cerebral venous sinus thrombosis were seldom reported.Reference Aydin, Quliyev, Cinar, Bozkaya and Oran3 In our report, we want to remind the neurologists that Eagle syndrome should be taken into account when dealing with cases of cerebral venous sinus thrombosis of unknown origin, and CT venography may be a useful diagnostic tool.
Statement of Authorship
Study concept and design: Yang; acquisition of data: Zhang, Zhou, and Guo; image analysis: Zhou; drafting of the manuscript: Zhang, Zhou; critical revision of the manuscript for important intellectual content: Yang; obtained funding: Yang.
Acknowledgements
This research was supported by the National Key R&D Program of China (2016YFC1301600), JLUSTIRT (2017TD-12), and Jilin the Fundamental Research Funds for the Central Universities to YY.
Disclosures
The authors declare no conflicts of interest.