Maple syrup urine disease (MSUD) is due to an autosomal recessive genetic defect in the mitochondrial branched-chain a-ketoacid dehydrogenase complex, causing accumulation of branched-chain amino acids (BCAA) leucine, isoleucine and their alpha-ketoacids.Reference Ha, Kim and Eun1 Much of the literature and experience with MSUD metabolic decompensations to date has been with neonates. Cerebral oedema is a serious complication of MSUD precipitated by worsening biochemical control during intercurrent illnessReference Ha, Kim and Eun1 or from high protein intake from poor dietary compliance.Reference Reddy, Calloni, Vernon, Boltshauser, Huisman and Soares2 Cerebral oedema can be reversible but in severe cases may lead to death.Reference Riviello, Rezvani, DiGeorge and Foley3
We report a rather late presentation of a 17-year-old female who presented with a gradual reduction in vision over a 1-month period and a new worsening generalised headache. MSUD was diagnosed at birth with no prior complications or imaging abnormalities. The most recent neuroimaging, an MRI brain, had been normal 2 years prior. On admission, an ophthalmology assessment revealed bilateral papilloedema, reduced visual fields and acuity with preserved colour vision. There were no signs of infection. Plasma amino acid levels of leucine and isoleucine levels were elevated. MRI brain imaging showed the typical intramyelinic pattern of MSUD oedema caused by a metabolic decompensation. This showed bilateral symmetrical striking white matter T2 hyperintense signal and restricted diffusion in the U fibres, corona radiata, posterior limbs of the internal capsules, thalami, lentiform nuclei, corticospinal tracts, brainstem and cerebellum (Figure 1A-C). Signs of raised intracranial pressure included reduced cerebral sulcal spaces and papilloedema, cerebral tonsils lying just below the foramen magnum and intrasellar arachnoid herniation (Figure 1E, F). Imaging features of papilloedema included dilated optic nerve sheaths and bulging optic nerve heads (Figure 1D, E). The optic chiasm and optic radiations were also involved. Strict dietary control was initiated, plasma amino acid levels decreased and the papilloedema improved. Signal changes persisted but had improved on MRI imaging at 1-month follow-up, and there had been some improvement in vision.
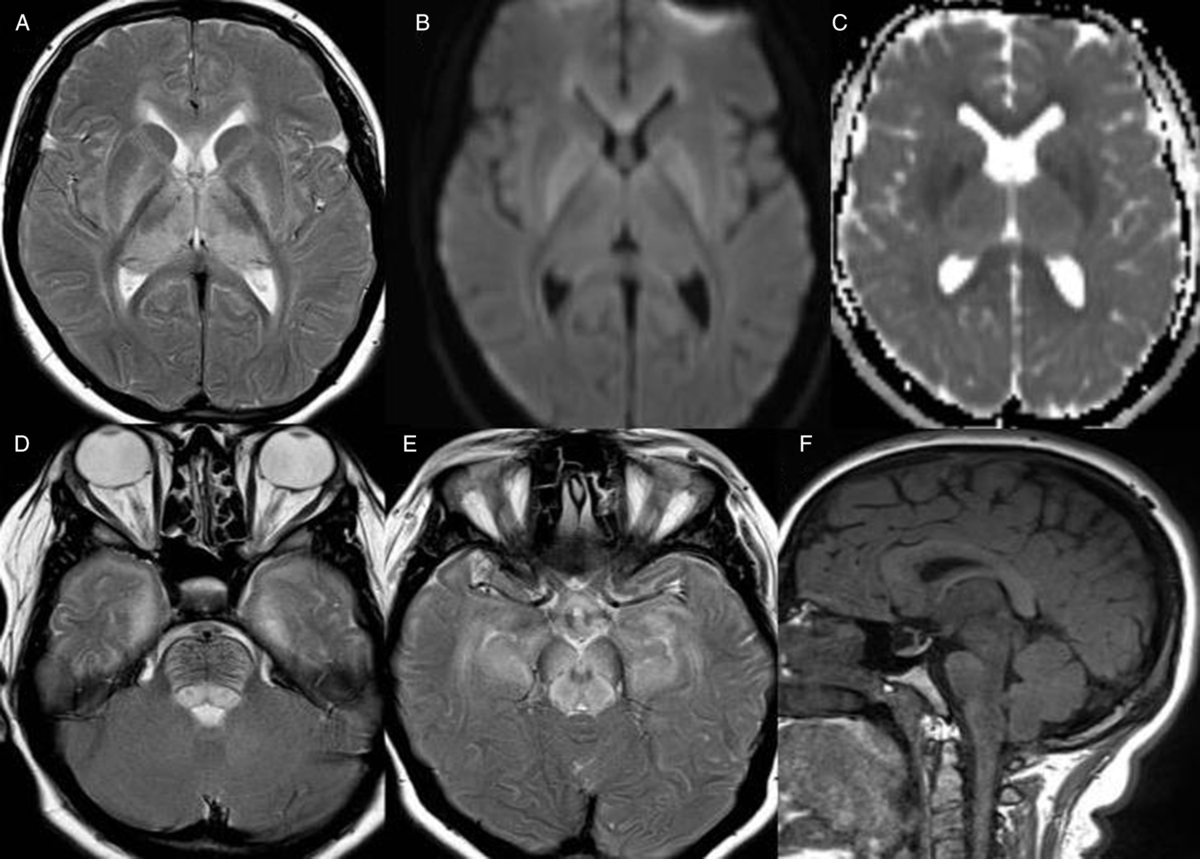
Axial and sagittal MRI brain images showing the intramyelinic oedema and brain swelling. Symmetrical T2 hyperintense signal in the cerebral white matter including the lentiform nuclei and thalami (A) which shows restricted diffusion (B, C). Dilated optic nerve sheaths and bulging of the optic nerve heads (D, E) and intrasellar arachnoid herniation (F) due to raised intracranial pressure.
This clinical presentation with deteriorating vision was due to the raised intracranial pressure from diffuse cerebral oedema and brain swelling caused by a metabolic decompensation. The exact pathogenesis of cerebral oedema remains unclearReference Riviello, Rezvani, DiGeorge and Foley3 but is thought to result from a combination of increased cerebral BCAA, decreased levels of other essential amino acids and neurotransmitters.Reference Myers, Reeves, Wei and Khan4 Ocular complications in untreated MSUD or late diagnosis include optic atrophy, nystagmus, ophthalmoplegia, strabismus and cortical blindness.Reference Burke, O’Keefe, Bowell and Naughten5 This case had a prolonged subacute course presumably as a consequence of poor dietary compliance with long-standing exposure to elevated branched-chain amino acids. It is important to recognise signs of cerebral oedema and raised intracranial pressure in older children and adults with MSUD as brain swelling causes many complications and can even result in cerebral herniation and death.Reference Riviello, Rezvani, DiGeorge and Foley3
Disclosures
The authors have no conflicts of interest to declare.


