Refine listing
Actions for selected content:
142032 results in Open Access
Understanding the Occurrence of Psychiatric Disorders in Epilepsy in Brazil: An Epidemiological Investigation
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S98
-
- Article
-
- You have access
- Open access
- Export citation
Quality of Life Assessment in Patients with Knee Osteoarthritis
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S421
-
- Article
-
- You have access
- Open access
- Export citation
A longitudinal study of child and adolescent psychopathology in conditions of the war in Ukraine
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S74-S75
-
- Article
-
- You have access
- Open access
- Export citation
Major depressive episode in the elderly. Use of maintenance ECT: a case report.
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S641
-
- Article
-
- You have access
- Open access
- Export citation
Comparing the characteristcs of hospitalized patients admitted in involuntary or voluntary treatment after first episode psychosis
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S313
-
- Article
-
- You have access
- Open access
- Export citation
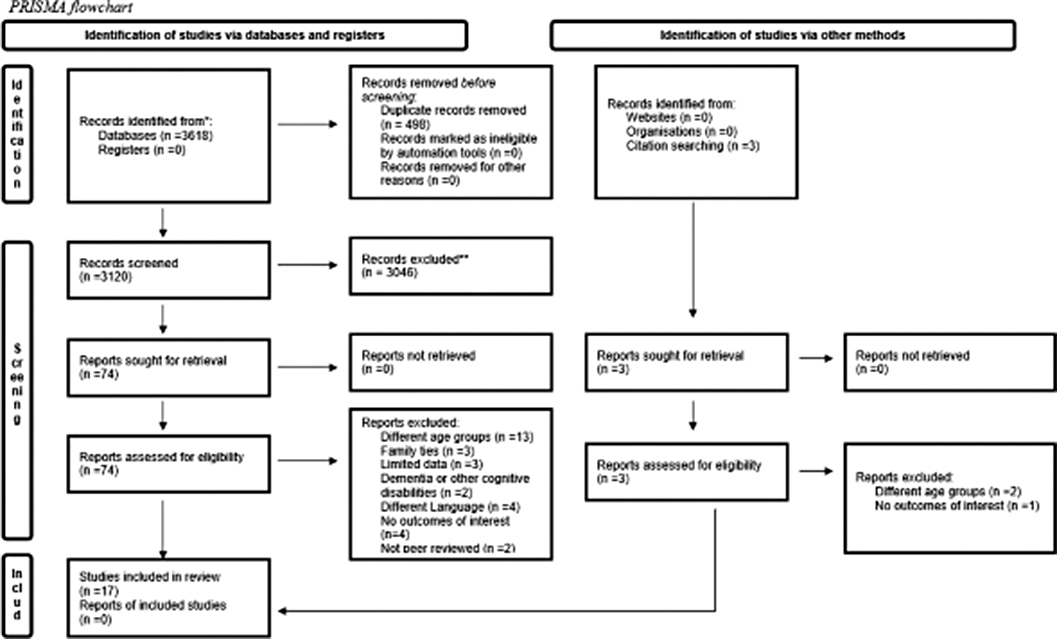
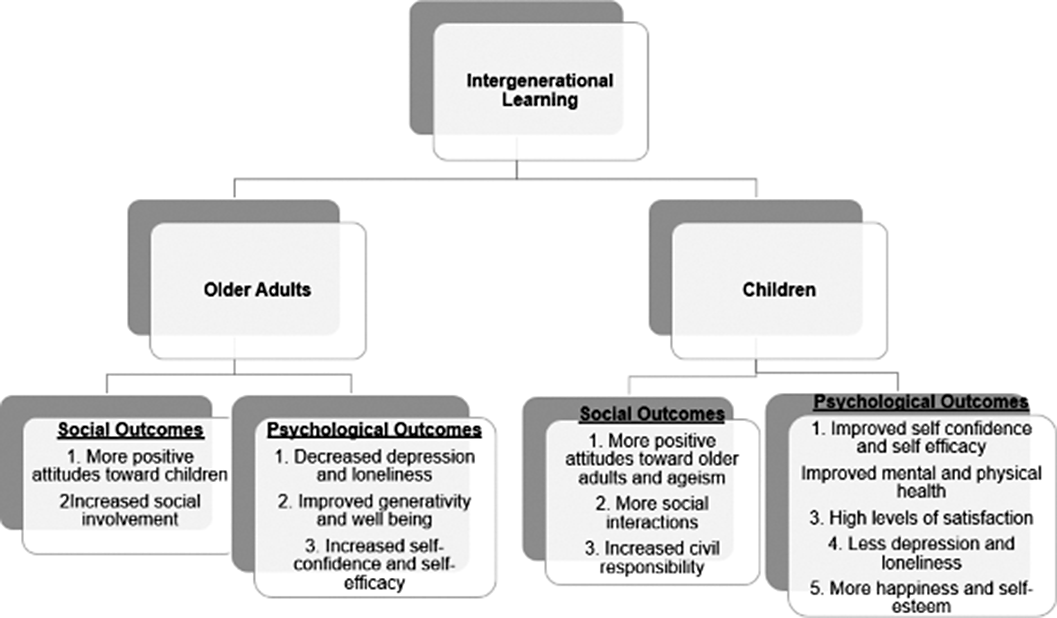
A Systematic Review of the Impact of Intergenerational Learning on the Psychosocial Well-being of Primary School Children and Older Adults.
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S340-S341
-
- Article
-
- You have access
- Open access
- Export citation
Innovation in the treatment, interventions and systems of care for opioid use disorder: opportunities to understand multimorbidities
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S34
-
- Article
-
- You have access
- Open access
- Export citation
An Experiment Measuring Water Consumption in Roman Hydrophobic Mortar (opus signinum)
-
- Journal:
- European Journal of Archaeology / Volume 27 / Issue 4 / November 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. 488-506
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
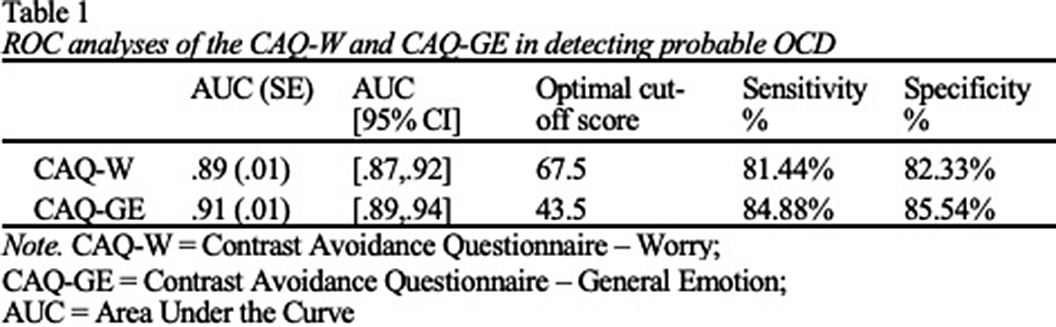
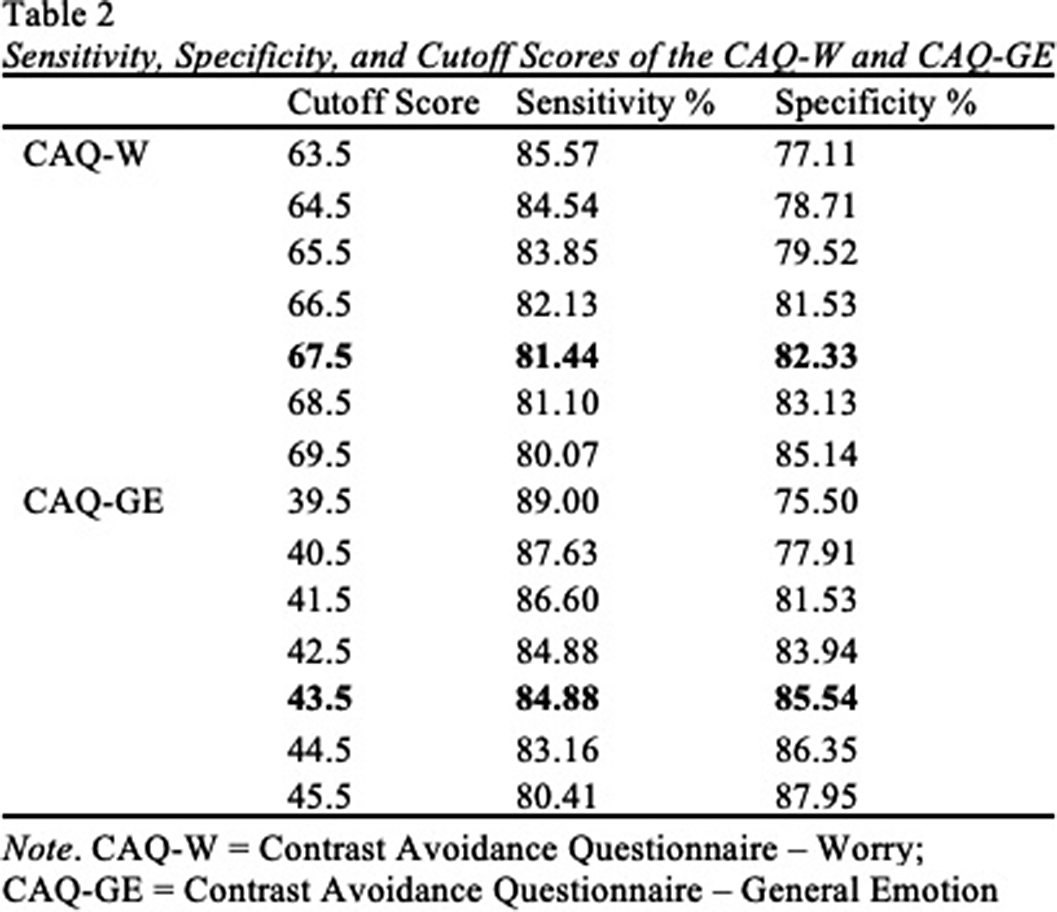
Avoidance of Negative Emotional Contrasts as a Diagnostic Feature of OCD: A Receiver-Operator Characteristic Curve Analysis of the Contrast Avoidance Questionnaires
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S357-S358
-
- Article
-
- You have access
- Open access
- Export citation
How psychopathy is associated with the level and change of impulsivity in correctional treatment
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S154
-
- Article
-
- You have access
- Open access
- Export citation
Mental health of children in ukraine. risks and challenges today
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S253
-
- Article
-
- You have access
- Open access
- Export citation
Psychopharmacological factor in the course of COVID-19 among psychiatric inpatients
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S506
-
- Article
-
- You have access
- Open access
- Export citation
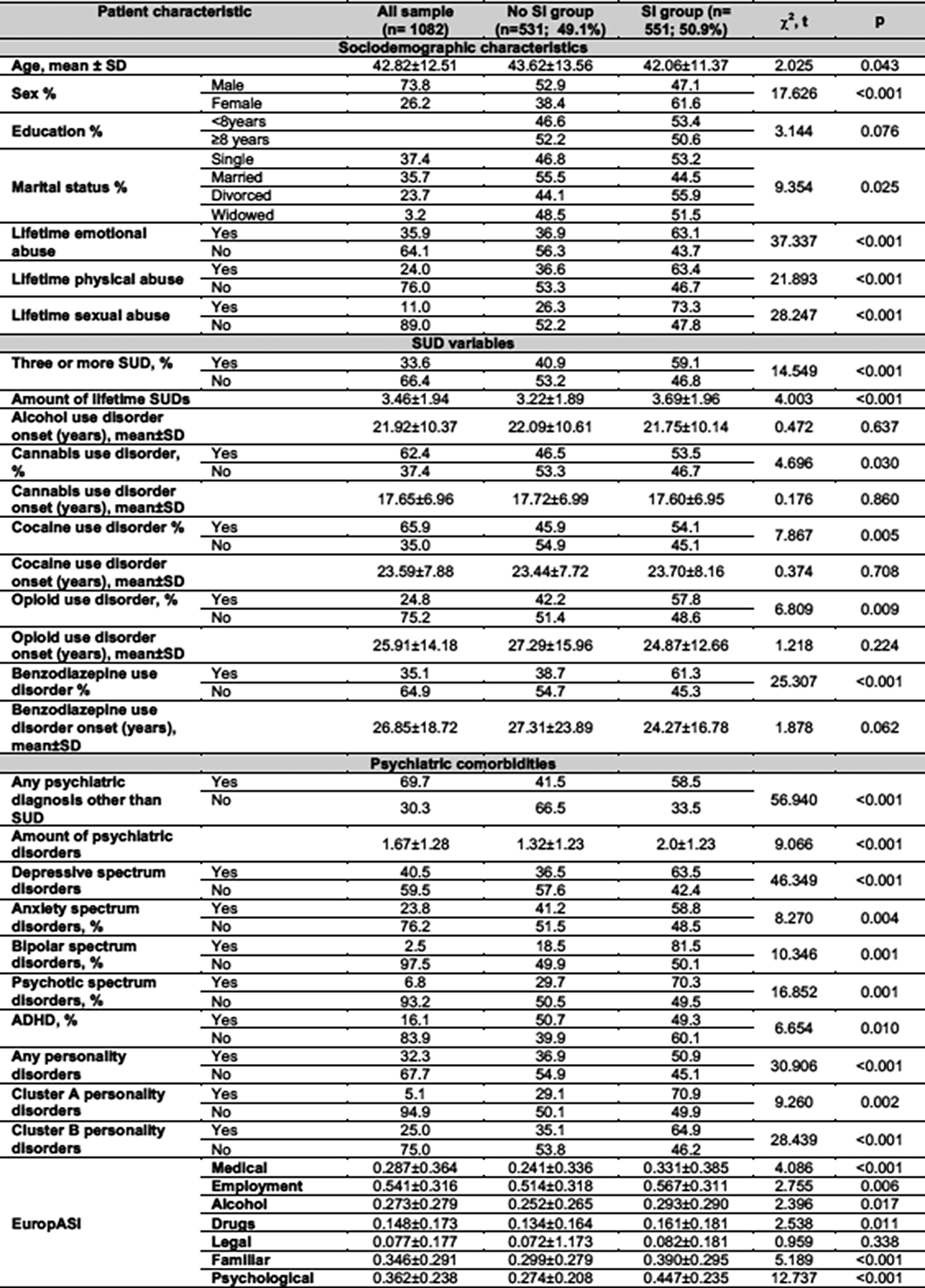
A preliminary analysis of clinical characteristics of patient with alcohol use disorder and suicidal ideation
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S185-S186
-
- Article
-
- You have access
- Open access
- Export citation
The social determinants of depression: social support, loneliness, and the impact of the COVID-19 pandemic
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S193
-
- Article
-
- You have access
- Open access
- Export citation
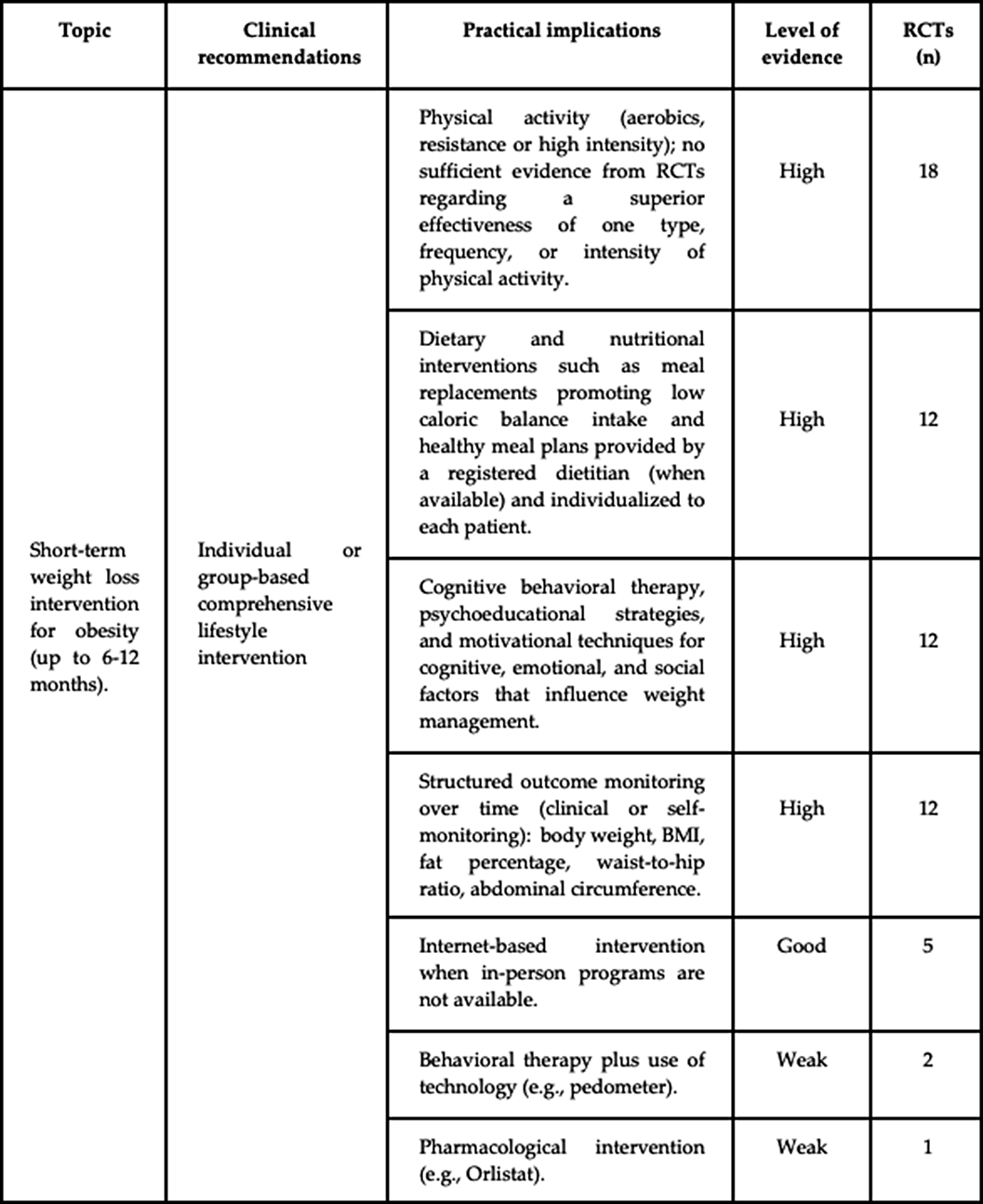
Randomized Controlled Trials to Treat Obesity in Military Populations: A Systematic Review and Meta-Analysis
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S307-S308
-
- Article
-
- You have access
- Open access
- Export citation
Epilepsy and psychiatric pathologies: A study of a case series
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S476-S477
-
- Article
-
- You have access
- Open access
- Export citation
How Many Criteria Should be Required to Define the DSM-5 Mixed Features Specifier in Depressed Patients?
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S298
-
- Article
-
- You have access
- Open access
- Export citation
Reaching Out from Europe to the Globe: The International Journal of Psychiatric Trainees
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S177
-
- Article
-
- You have access
- Open access
- Export citation
Navigating Mental Health Support in Tunisia’s Digital Age: Preferences, Challenges, and Paradoxes-An online survey
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S547
-
- Article
-
- You have access
- Open access
- Export citation
Emergency Department Presentations to the Mental Health Services at Sligo University Hospital during the COVID pandemic
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S150
-
- Article
-
- You have access
- Open access
- Export citation