Refine listing
Actions for selected content:
142351 results in Open Access
Exhalation
-
- Journal:
- Palliative & Supportive Care / Volume 22 / Issue 5 / October 2024
- Published online by Cambridge University Press:
- 16 September 2024, p. 1533
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Community-associated Carbapenem-Resistant Organism Case Investigations in New York City, December 2020-May 2023
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, p. s147
-
- Article
-
- You have access
- Open access
- Export citation
Assessing chlorhexidine resistance in MRSA isolates from hospitals in Cleveland, OH and Detroit, MI
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, p. s114
-
- Article
-
- You have access
- Open access
- Export citation
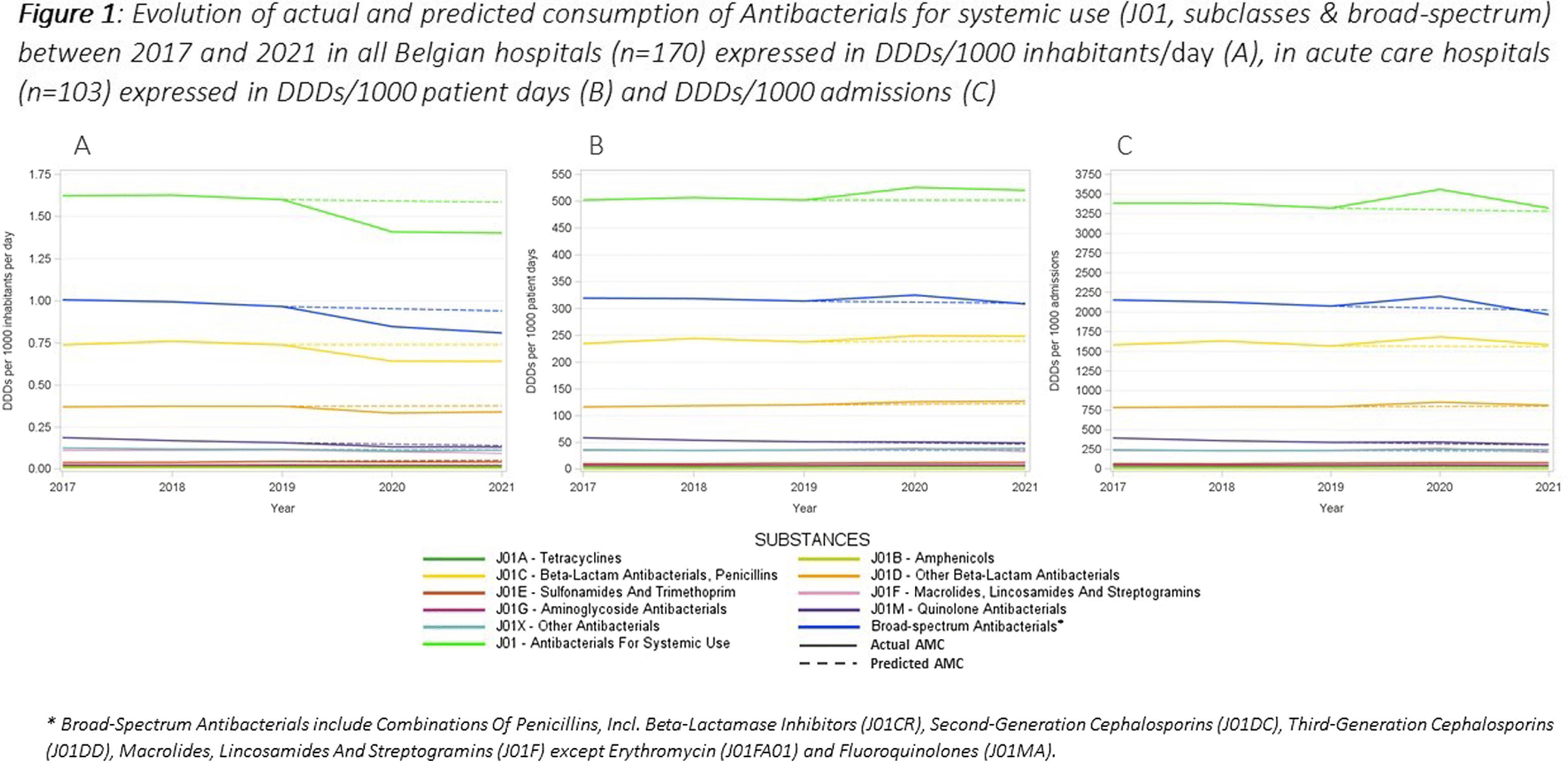
Trends in Hospital Antibacterial Consumption in Belgium (2017-2021): Evaluating the Impact of the COVID-19 Pandemic
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, pp. s149-s150
-
- Article
-
- You have access
- Open access
- Export citation
Assessing the quality of Hand Hygiene data produced by Alberta Health Services using a time-in-motion study
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, p. s100
-
- Article
-
- You have access
- Open access
- Export citation
Underlying Conditions in Community-associated Clostridioides difficile Infections in Davidson County, Tennessee
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, p. s65
-
- Article
-
- You have access
- Open access
- Export citation
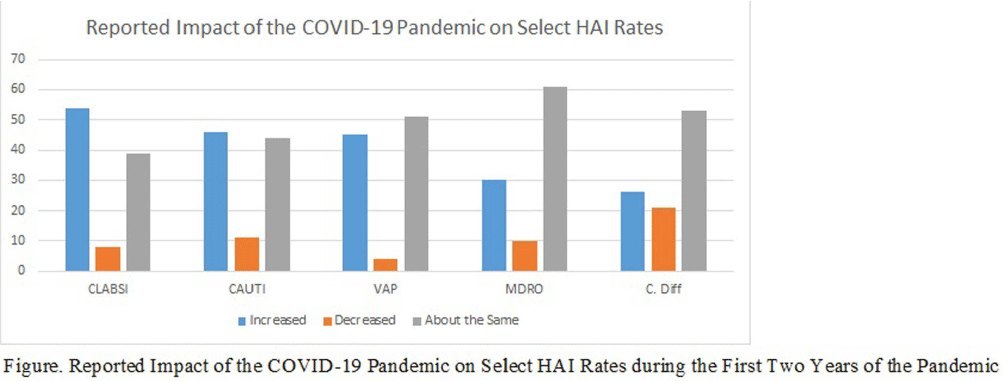
The Impact of COVID-19 on Healthcare-Associated Infections: A Survey of Acute Care Hospitals
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, pp. s11-s12
-
- Article
-
- You have access
- Open access
- Export citation
The Next Target for Readmission Reporting? Exploring Readmission Rates of Patients with CLABSI
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, p. s71
-
- Article
-
- You have access
- Open access
- Export citation
Epidemiology of Extrapulmonary Nontuberculous Mycobacterial Disease – 4 Emerging Infection Program Sites, 2021
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, pp. s90-s91
-
- Article
-
- You have access
- Open access
- Export citation
Quantity versus Quality: Chlorhexidine Bathing Adequacy Assessments in 3 High-Risk Units
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, p. s30
-
- Article
-
- You have access
- Open access
- Export citation
Investigation of Healthcare-Associated Infection Risks from Ice: Summary of CDC Consultations 2016-2023
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, p. s29
-
- Article
-
- You have access
- Open access
- Export citation
Antibiotic Prescribing Practices on Hospital Discharge for Management of Urinary Tract Infections: A Single Center Study
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, pp. s36-s37
-
- Article
-
- You have access
- Open access
- Export citation
The Difference We Make at Home: Impact of Infection Prevention and Control in Pediatric Homecare Tracheitis Reduction
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, p. s130
-
- Article
-
- You have access
- Open access
- Export citation
Antimicrobial use among under-five hospitalized children in Bangladesh: Findings from a Point Prevalence Survey
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, p. s50
-
- Article
-
- You have access
- Open access
- Export citation
Mitigating SSIs: focus on physical operation rooms environmental factors
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, pp. s96-s97
-
- Article
-
- You have access
- Open access
- Export citation
Intervention Targets to Optimize Antibiotic Prescribing on Discharge from the Hospital to Nursing Homes
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, p. s23
-
- Article
-
- You have access
- Open access
- Export citation
Nevertheless
-
- Journal:
- Palliative & Supportive Care / Volume 22 / Issue 6 / December 2024
- Published online by Cambridge University Press:
- 16 September 2024, p. 2247
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Inpatient clinicians’ approach to diagnosis of urinary tract infections in older adults using the COM-B model: a qualitative assessment
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue 1 / 2024
- Published online by Cambridge University Press:
- 16 September 2024, e134
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Mentoring up: How mentorship training influences mentee intent to change behavior
-
- Journal:
- Journal of Clinical and Translational Science / Volume 8 / Issue 1 / 2024
- Published online by Cambridge University Press:
- 16 September 2024, e119
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
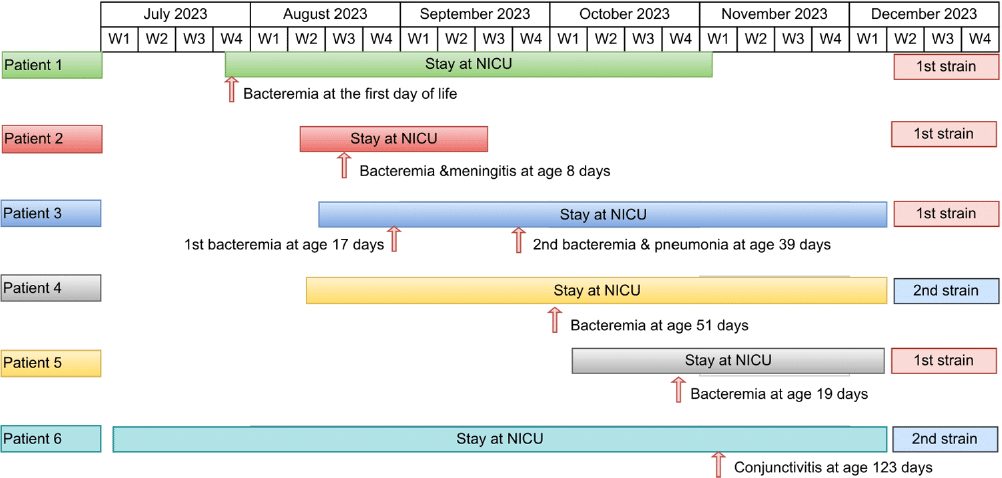
Whole Genome Sequencing for the Identification of a Streptococcus agalactiae Outbreak in Neonatal Intensive Care Unit
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, pp. s124-s125
-
- Article
-
- You have access
- Open access
- Export citation