Refine listing
Actions for selected content:
142351 results in Open Access
Retreat of the Greenland Ice Sheet leads to divergent patterns of reconfiguration at its freshwater and tidewater margins
-
- Journal:
- Journal of Glaciology / Volume 70 / 2024
- Published online by Cambridge University Press:
- 16 September 2024, e65
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Survey of VA Laboratory Practices for Carbapenem-resistant Acinetobacter baumannii and Pseudomonas aeruginosa
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, p. s79
-
- Article
-
- You have access
- Open access
- Export citation
Pilot of a Bowel Habit Assessment Tool to Enable Early Identification of C. diff Infection
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, p. s63
-
- Article
-
- You have access
- Open access
- Export citation
A One-year Hospital System Review of Plasma Next-Generation Sequencing in a Mixed Population
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, p. s84
-
- Article
-
- You have access
- Open access
- Export citation
System infection prevention in hospital networks – a SHEA research network survey
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, p. s108
-
- Article
-
- You have access
- Open access
- Export citation
Real-time Whole Genome Sequencing Surveillance as an Effective Outbreak Detection and Mitigation Tool
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, pp. s113-s114
-
- Article
-
- You have access
- Open access
- Export citation
“AWECoP has made my teaching experience so much better!” – Creating community and improving teaching practice through an Animal Welfare Education Community of Practice (AWECoP)
-
- Journal:
- Animal Welfare / Volume 33 / 2024
- Published online by Cambridge University Press:
- 16 September 2024, e35
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Automated Discontinuation of Isolation Precautions with the Use of Electronic Health Record Tools
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, p. s135
-
- Article
-
- You have access
- Open access
- Export citation
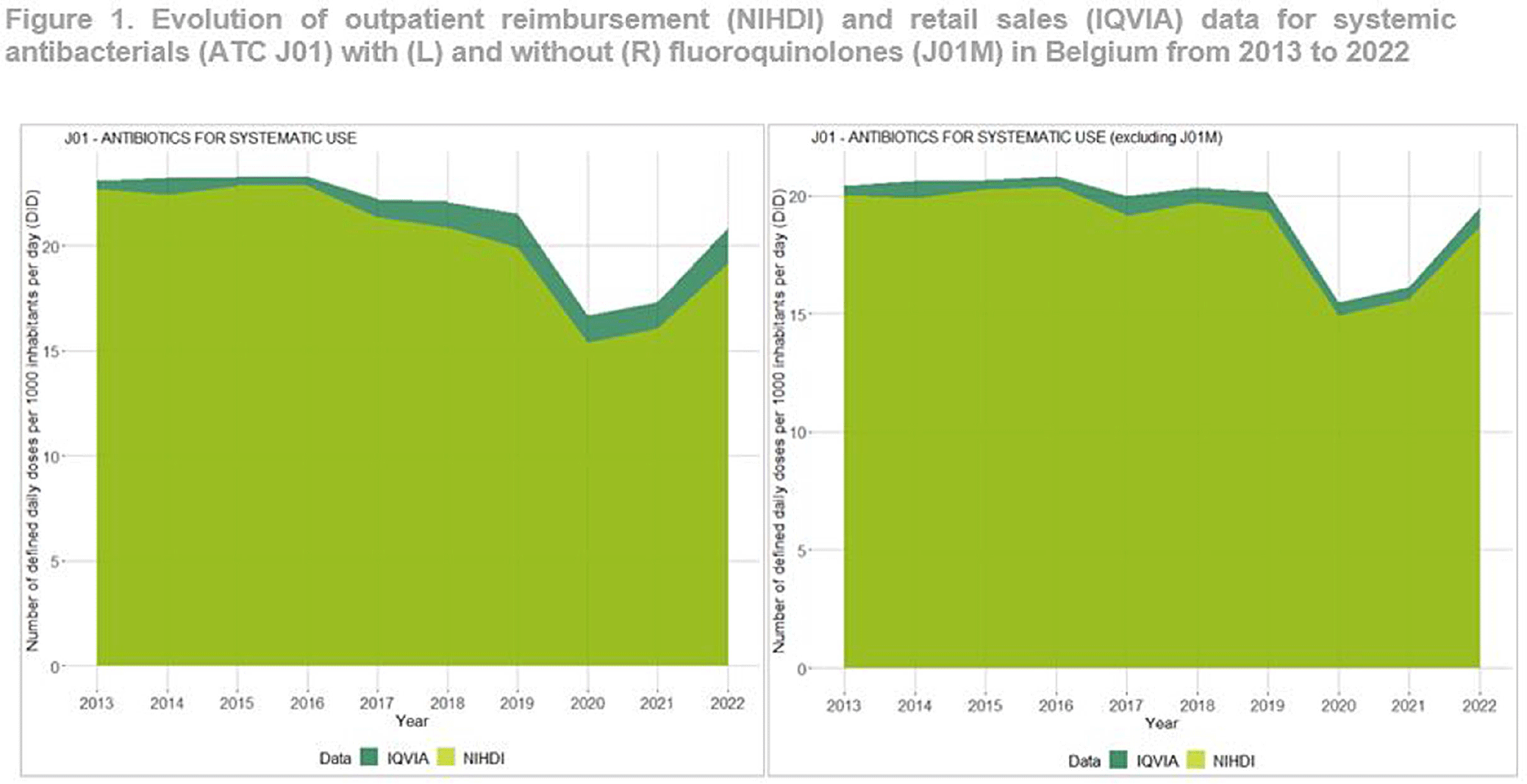
Outpatient Antibiotic Consumption Trends in Belgium: A Comparative Analysis of Reimbursement and Sales Data, 2013-2022
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, pp. s152-s153
-
- Article
-
- You have access
- Open access
- Export citation
Changes in Antibiotic Use and Disruptions to Antimicrobial Resistance Detection in South Africa and Uganda, 2019 – 2020
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, p. s132
-
- Article
-
- You have access
- Open access
- Export citation
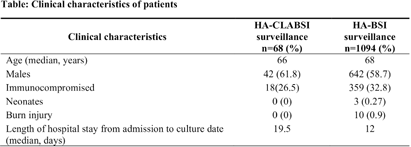
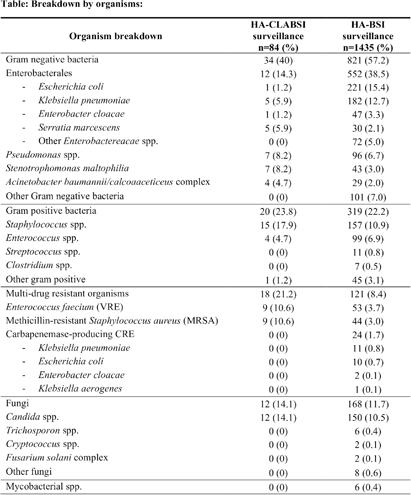
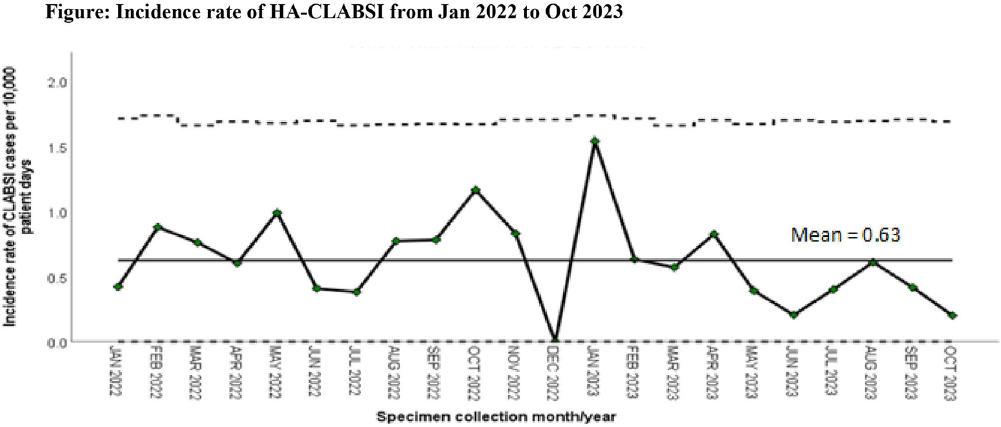
Comparative Analysis of Healthcare-associated Bloodstream Infections & CLABSI Surveillance in A Singaporean tertiary Hospital
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, pp. s154-s155
-
- Article
-
- You have access
- Open access
- Export citation
Factors associated with clinician willingness to adopt HPV self-sampling and self-testing for cervical cancer screening
-
- Journal:
- Journal of Clinical and Translational Science / Volume 8 / Issue 1 / 2024
- Published online by Cambridge University Press:
- 16 September 2024, e118
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Health Equity Factors and Healthcare-Associated Infections in Louisiana Facilities, 2022
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, p. s17
-
- Article
-
- You have access
- Open access
- Export citation
Impact of Stewardship Pharmacist Driven MRSA Nasal Surveillance and De-escalation of Anti-MRSA Therapy
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, p. s44
-
- Article
-
- You have access
- Open access
- Export citation
Implications of high-resolution velocity and strain rate observations for modelling of Greenlandic tidewater glaciers
-
- Journal:
- Journal of Glaciology / Volume 70 / 2024
- Published online by Cambridge University Press:
- 16 September 2024, e17
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
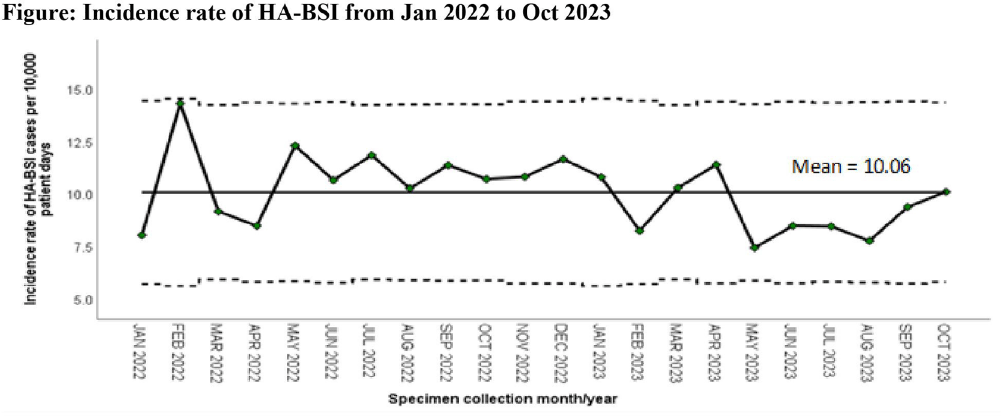
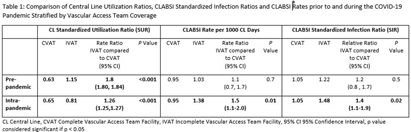
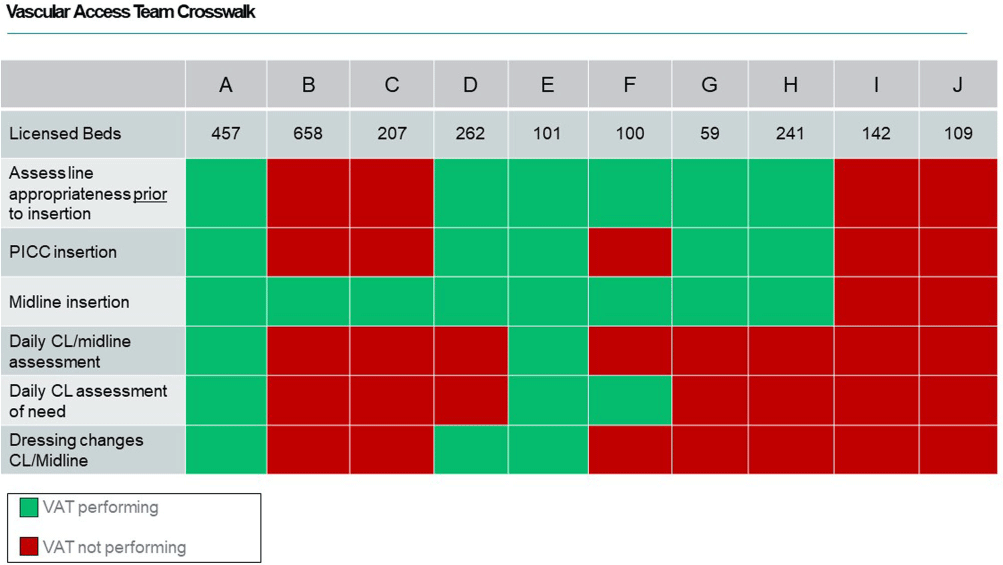
Impact of Vascular Access Teams on Central Line Associated Bloodstream Infections
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, p. s11
-
- Article
-
- You have access
- Open access
- Export citation
An Examination of Racial/Ethnic Differences in the Antibiotic Treatment of Community Acquired Pneumonia
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, p. s23
-
- Article
-
- You have access
- Open access
- Export citation
S. aureus Surveillance and Decolonization Associated with Decreased MRSA, but not MSSA, Infections in the Neonatal ICU
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, pp. s117-s118
-
- Article
-
- You have access
- Open access
- Export citation
Inter-rater agreement of CAUTI (catheter-associated urinary tract infections) diagnosis among Infectious disease physicians
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, pp. s70-s71
-
- Article
-
- You have access
- Open access
- Export citation
It Takes a Village: Leveraging a Multidisciplinary Team and Technology for Urine Culturing Stewardship
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, pp. s82-s83
-
- Article
-
- You have access
- Open access
- Export citation