Refine listing
Actions for selected content:
142351 results in Open Access
Teaching Antimicrobial Decision-Making in Medical Education: A Qualitative Study
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, pp. s42-s43
-
- Article
-
- You have access
- Open access
- Export citation
Infection prevention making a difference on statewide standardized infection ratios for device-associated HAIs from 2015-2022
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, pp. s28-s29
-
- Article
-
- You have access
- Open access
- Export citation
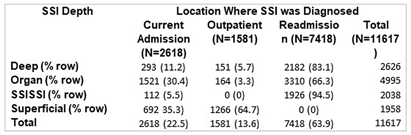
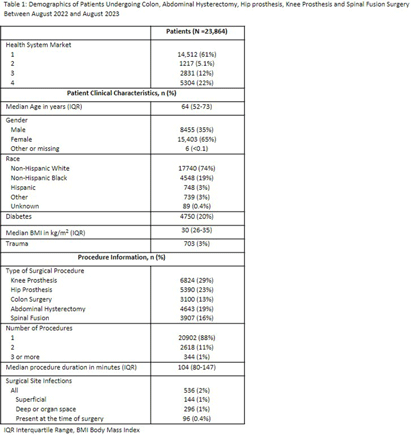
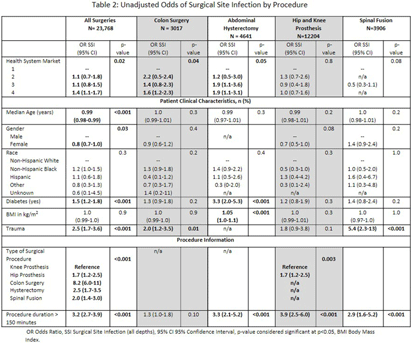
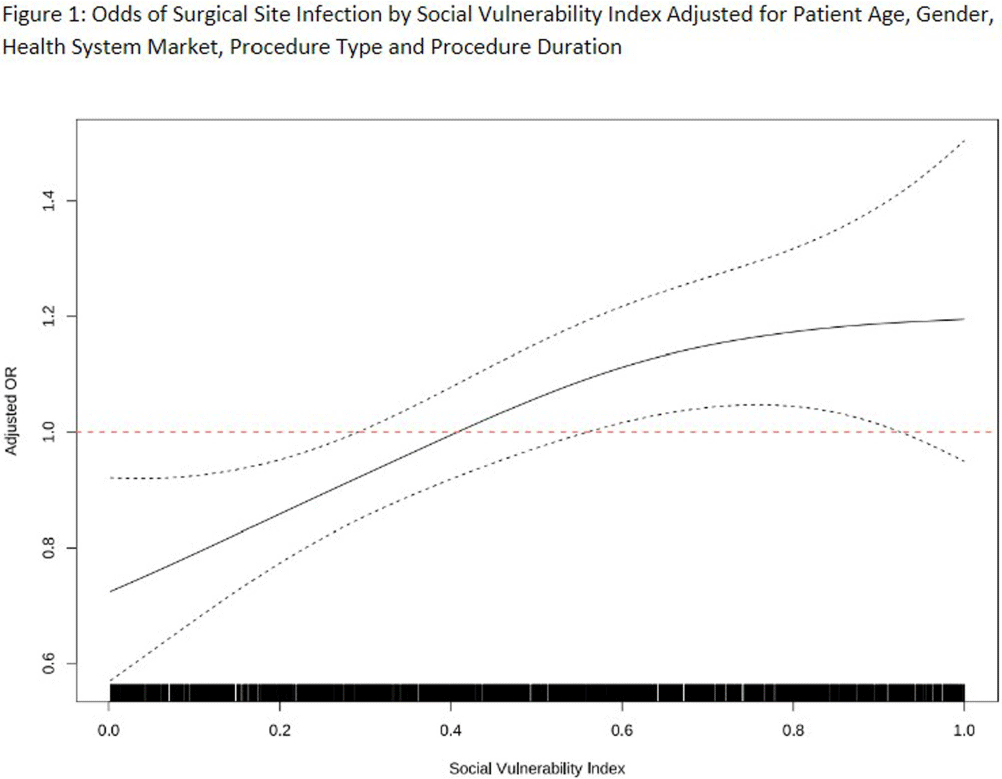
Exploring Socioeconomic Disparities in Surgical Site Infections
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, pp. s2-s3
-
- Article
-
- You have access
- Open access
- Export citation
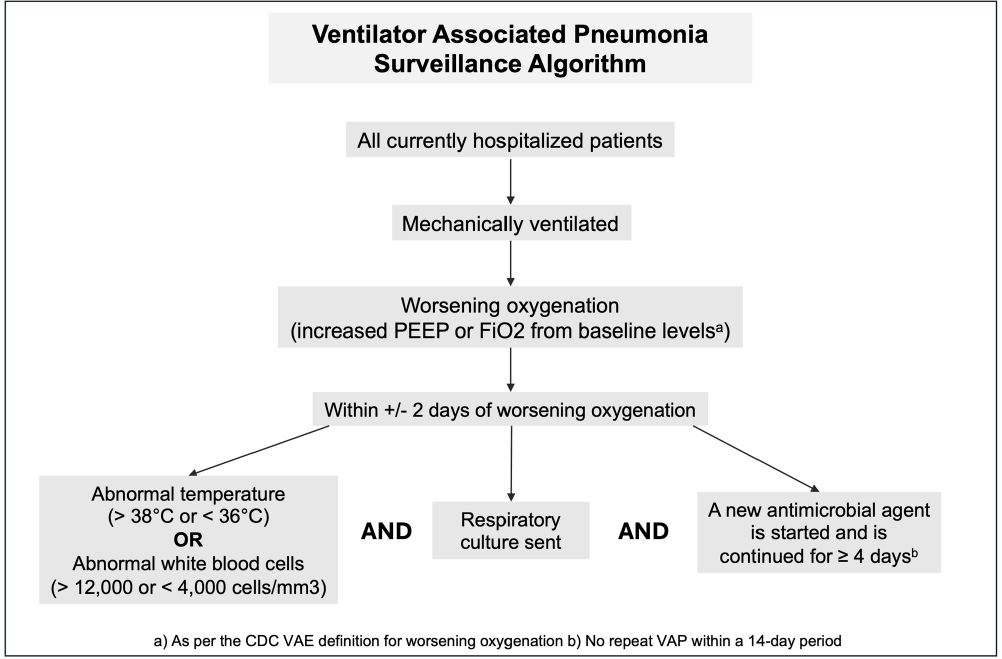
An Improved Algorithm for the Detection of Ventilator Associated Pneumonia
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, pp. s151-s152
-
- Article
-
- You have access
- Open access
- Export citation
Excavating ancient pilgrimage at Nessana, Negev
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Guideline-unjustified inpatient therapy for non-ICU patients with community-acquired pneumonia (CAP) at 105 Veterans Affairs
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, pp. s40-s41
-
- Article
-
- You have access
- Open access
- Export citation
MDRO Colonization Among Nursing Homes Patients: A Risk Classification Tool for Early Identification
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, pp. s118-s119
-
- Article
-
- You have access
- Open access
- Export citation
Twenty-four hour urinary sodium and potassium excretion in adult population of Slovenia: results of the Manjsoli.si/2022 study
-
- Journal:
- Public Health Nutrition / Volume 27 / Issue 1 / 2024
- Published online by Cambridge University Press:
- 16 September 2024, e163
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Differential viral load of surgical masks worn by patients infected with respiratory viruses
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, p. s141
-
- Article
-
- You have access
- Open access
- Export citation
Does Urinary Catheter Replacement Prior To Obtaining Urine for Culture Make a Difference?
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, pp. s69-s70
-
- Article
-
- You have access
- Open access
- Export citation
A Comparison of Variable Input Strategies used for Risk-adjustment Models of Antimicrobial Use
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, pp. s30-s31
-
- Article
-
- You have access
- Open access
- Export citation
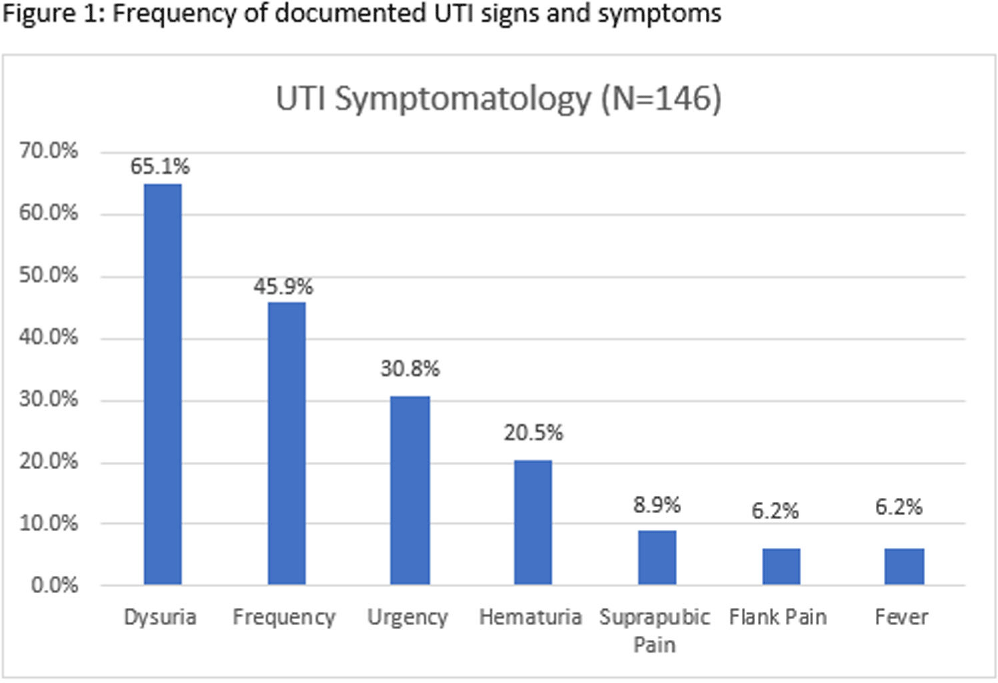
UTI Symptomatology and Antibiotic Prescribing among US Veterans Seen in Outpatient Clinics
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, p. s80
-
- Article
-
- You have access
- Open access
- Export citation
Does Serial Procalcitonin Monitoring predict Clinical Outcomes in Children with Sepsis? A diagnostic stewardship study
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, p. s82
-
- Article
-
- You have access
- Open access
- Export citation
Situations Predisposing Primary Care Patients to Use Antibiotics Without a Prescription in the United States
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, p. s22
-
- Article
-
- You have access
- Open access
- Export citation
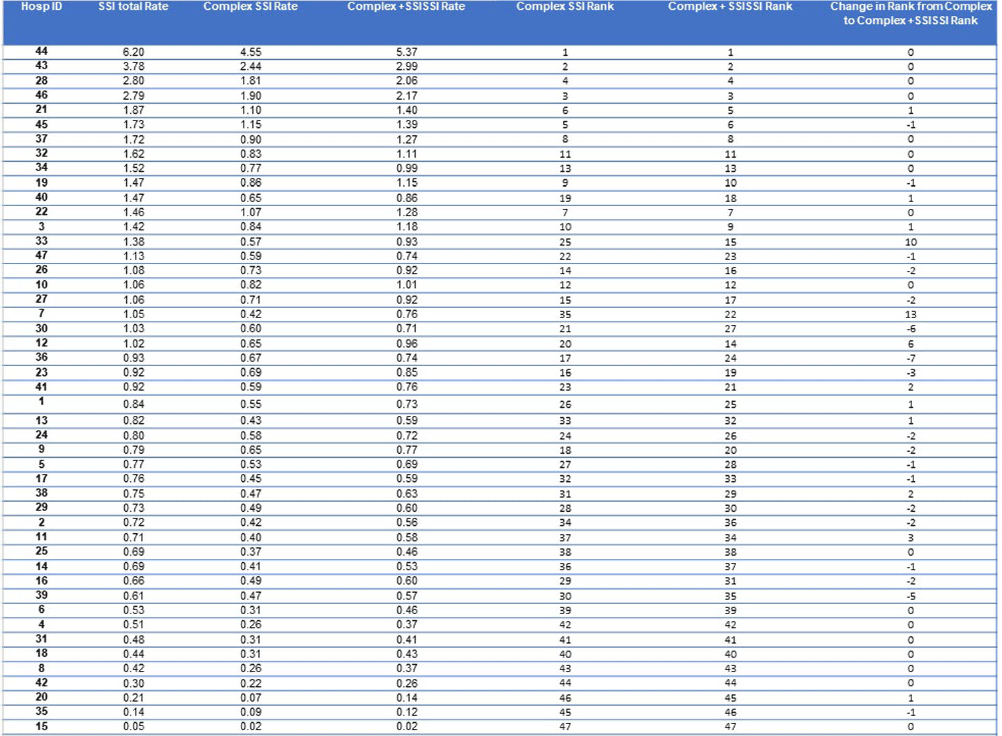
A Deeper Look at Proposed Surveillance of Superficial Incision Surgical Site Infections (SSISSIs)
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, p. s142
-
- Article
-
- You have access
- Open access
- Export citation
Efficacy of Empiric Contact Precautions for Patients from High Risk Facilities
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, p. s150
-
- Article
-
- You have access
- Open access
- Export citation
CAPILLARY LEVELLING OF THIN LIQUID FILMS OF POWER-LAW RHEOLOGY
- Part of
-
- Journal:
- The ANZIAM Journal / Volume 66 / Issue 1 / January 2024
- Published online by Cambridge University Press:
- 16 September 2024, pp. 62-76
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Impact of Universal Masking by Healthcare Personnel on Non-SARS-CoV-2 Healthcare-Associated Viral Respiratory Infections
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, p. s141
-
- Article
-
- You have access
- Open access
- Export citation
Improving Data Quality from a Hematology Unit Hand Hygiene Observation Program
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, pp. s99-s100
-
- Article
-
- You have access
- Open access
- Export citation
Carbapenemase-Producing Enterobacteriaceae detected in a Large Canadian Tertiary Care Hospital: Five-year retrospective study
-
- Journal:
- Antimicrobial Stewardship & Healthcare Epidemiology / Volume 4 / Issue S1 / July 2024
- Published online by Cambridge University Press:
- 16 September 2024, p. s157
-
- Article
-
- You have access
- Open access
- Export citation