Refine listing
Actions for selected content:
141953 results in Open Access
The Influence of Nonparental Care on Internalizing and Externalizing Behaviors Across Adolescence: An individual Participant Meta-Analysis
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S139-S140
-
- Article
-
- You have access
- Open access
- Export citation
Watersports Inclusion Games: The Benefits for Participants and the Impact of COVID-19 on Access
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S469
-
- Article
-
- You have access
- Open access
- Export citation
Dismantling task-sharing psychosocial interventions to personalize care for people affected by common mental disorders: developing a taxonomy of active ingredients and ranking their efficacy
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S669
-
- Article
-
- You have access
- Open access
- Export citation
The role of cerebral-cognitive reserve in the birth of a child with Alzheimer’s in late-life individuals
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S627
-
- Article
-
- You have access
- Open access
- Export citation
Attitudes on pharmacotherapy among parents of children with autism spectrum disorders
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S458-S459
-
- Article
-
- You have access
- Open access
- Export citation
Efficacy of Silexan in Patients with a Major Depressive Episode – First Results from a Multi-centre, Double-blind, Randomised, Placebo- and Reference-controlled Phase III Trial
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S224-S225
-
- Article
-
- You have access
- Open access
- Export citation
Systematically Informed Literature Review: What is the Prevalence of Borderline Personality Disorder (BPD) in Adolescents, 13-17, using DSM-5 Criteria?
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S220-S221
-
- Article
-
- You have access
- Open access
- Export citation
Retrospective Assessment of Metabolic Syndrome and Cardiovascular Disease Risk Following Monthly and Three-Month Long-Acting Paliperidone Palmitate Treatment in Schizophrenia
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S214-S215
-
- Article
-
- You have access
- Open access
- Export citation
Crosstalk between Anxiety and Depression and Inflammatory bowel diseases: preliminary data on circulating miRNAs
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S71-S72
-
- Article
-
- You have access
- Open access
- Export citation
Gestational age and sex interaction and risk for autism spectrum disorder in extremely preterm newborns: an 18‑month follow‑up study
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S281
-
- Article
-
- You have access
- Open access
- Export citation
Altered Cortical Gyrification Morphology in Nonsucidal Self-injury
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S618-S619
-
- Article
-
- You have access
- Open access
- Export citation
The impact of hormones on emotional and social development: a study in adolescent daughters of women with polycystic ovary syndrome
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S116
-
- Article
-
- You have access
- Open access
- Export citation
‘De Novo’ Psychosis following anterior temporal lobectomy: A case report
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S742
-
- Article
-
- You have access
- Open access
- Export citation
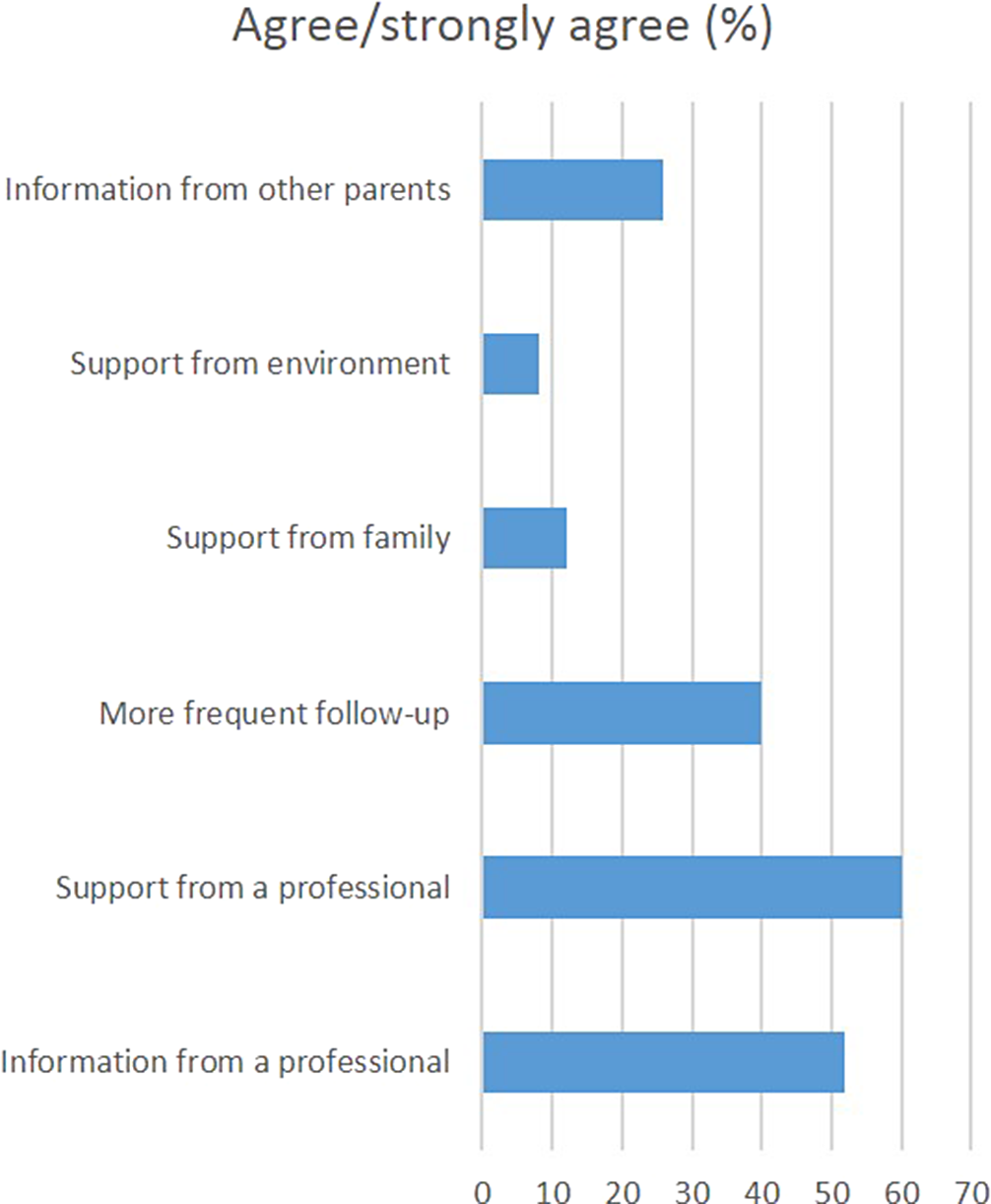
Parents’ psychosocial needs during the child’s hospitalization in pediatric intensive care units (PICU): a systematic review
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S674
-
- Article
-
- You have access
- Open access
- Export citation
Evaluation of daytime sleepiness and insomnia symptoms in OSA patients with a characterization of symptom-defined phenotypes and their involvement in depression comorbidity
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S392
-
- Article
-
- You have access
- Open access
- Export citation
ZNF536 dysfunction enhances spontaneous differentiation of the SH-SY5Y cell line into a neuronal-like phenotype
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S588
-
- Article
-
- You have access
- Open access
- Export citation
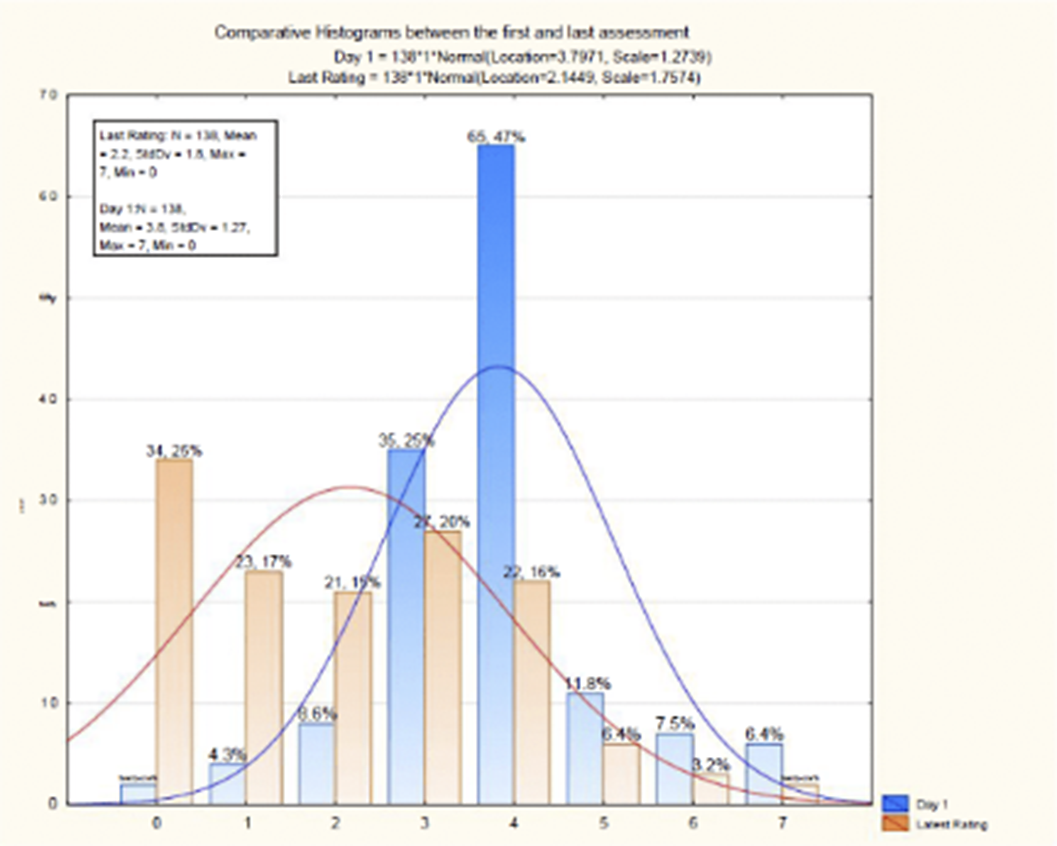
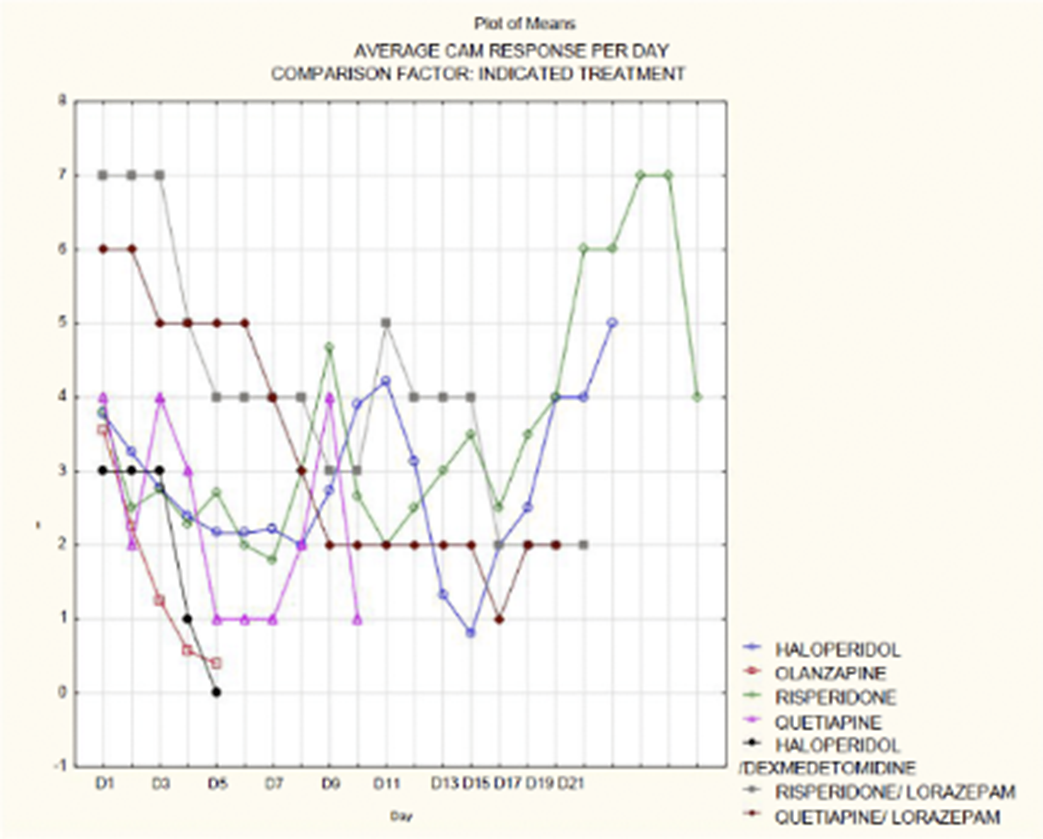
Socio-demographic characteristics and pharmacological treatment options in patients with delirium
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S368-S369
-
- Article
-
- You have access
- Open access
- Export citation
Is bipolar mixed depression associated with a good response to psychotropic augmentation?
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S26-S27
-
- Article
-
- You have access
- Open access
- Export citation
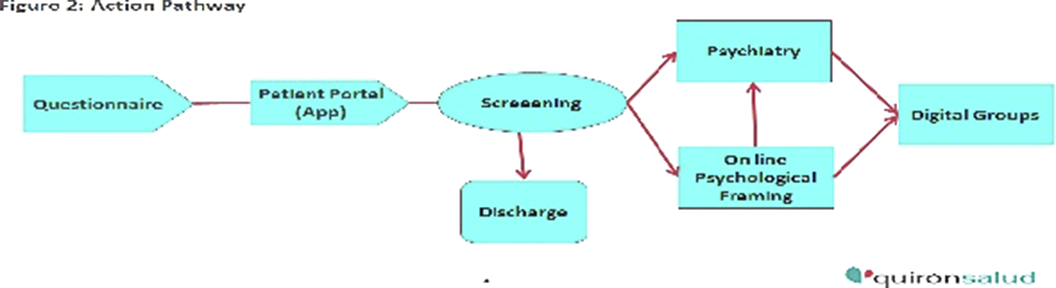
Mental Health and Addictions in Pregnancy: Feasibility and Acceptability of a Computerized Clinical Pathway and Prevalence Rates
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S66-S67
-
- Article
-
- You have access
- Open access
- Export citation
“Ekbom syndrome: delirium engraved on the skin”
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S759-S760
-
- Article
-
- You have access
- Open access
- Export citation