Refine listing
Actions for selected content:
142466 results in Open Access
The opportunity for e-mental health to overcome stigma and discrimination
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S549-S550
-
- Article
-
- You have access
- Open access
- Export citation
Psychosomatic relationships between the state of mental health and the level of vital threat of dermatological disease
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S370-S371
-
- Article
-
- You have access
- Open access
- Export citation
Cognitive complaints in schizophrenia:relationship with clinical symptoms, stigma and insight
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S757
-
- Article
-
- You have access
- Open access
- Export citation
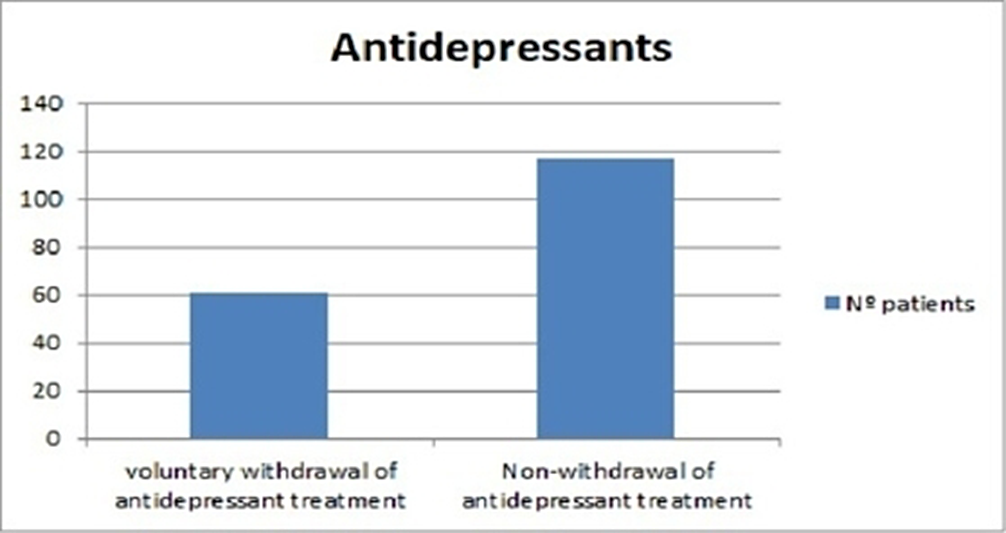
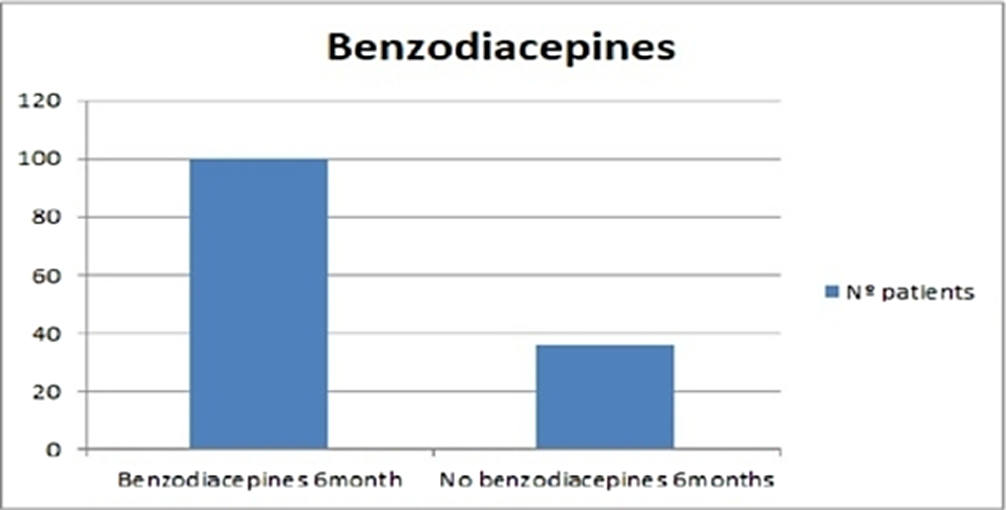
Evaluation of adherence to treatment in patients with anxious-depressive syndrome.
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S674-S675
-
- Article
-
- You have access
- Open access
- Export citation
Experience in the Psychotherapeutic Treatment of Eating Disorders in Children and Adolescents: A Brief Approach and EMDR Outcomes
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S460
-
- Article
-
- You have access
- Open access
- Export citation
Do antidepressants lead to weight-increase? Antidepressant therapy and long-term changes in body mass index, waist circumference and fat mass - A prospective, population-based study
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S24-S25
-
- Article
-
- You have access
- Open access
- Export citation
War and Migration – when Mental Health is left behind
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S614
-
- Article
-
- You have access
- Open access
- Export citation
Case Report and Literature review. Neuropsychiatry Manifestation of Frontal Lobe Neoplasm- Meningioma. Prevalence, Presentation and Pathogenesis
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S646
-
- Article
-
- You have access
- Open access
- Export citation
Effects of light therapy in the anxious-depressive clinic
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S533
-
- Article
-
- You have access
- Open access
- Export citation
Typology of hyperthymic personalities with affective phases
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S656-S657
-
- Article
-
- You have access
- Open access
- Export citation
The future of psychiatry and psychotherapy - An Early Career psychiatrist’s view
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S819
-
- Article
-
- You have access
- Open access
- Export citation
Co-design of a digital violence prevention and management tool for psychiatric inpatient care: focus on supporting integration into electronic health record system
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S59
-
- Article
-
- You have access
- Open access
- Export citation
The activity of platelet enzymes and subpopulation composition of monocytes in schizophrenia
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S688
-
- Article
-
- You have access
- Open access
- Export citation
Social determinants of involuntary psychiatric hospital admissions in Ontario, Canada
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S335
-
- Article
-
- You have access
- Open access
- Export citation
Exploring the connections between psychiatric disorders and climate change
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S472
-
- Article
-
- You have access
- Open access
- Export citation
Childhood socio-economic disadvantages versus adverse care experiences: Mediation and moderation impacts on late-life depressive symptoms
- Part of
-
- Journal:
- European Psychiatry / Volume 67 / Issue 1 / 2024
- Published online by Cambridge University Press:
- 27 August 2024, e47
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Cyber victimisation and depression among adolescents in Tunisia: a case report study and review of literature
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S449-S450
-
- Article
-
- You have access
- Open access
- Export citation
Increased emergency room visits without corresponding rehospitalizations in cannabis users with psychosis
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S388-S389
-
- Article
-
- You have access
- Open access
- Export citation
Short-term memory depends on the level of emotional burnout
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S380
-
- Article
-
- You have access
- Open access
- Export citation
Responses to serious adverse incidents in mental health care settings: a qualitative study of a complex patient safety system
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S610-S611
-
- Article
-
- You have access
- Open access
- Export citation