Refine listing
Actions for selected content:
142570 results in Open Access
First episode psychosis in a young person with a diagnosis of Autistic Spectrum Disorder: A Case report
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S456
-
- Article
-
- You have access
- Open access
- Export citation
Exploring Exercise Intervention as a Therapeutic Catalyst within the Mental Health and Addiction Program in Nova Scotia: A Proof-of-Concept Study
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S826
-
- Article
-
- You have access
- Open access
- Export citation
Reactivation of trauma in an inadequately structured person
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S667
-
- Article
-
- You have access
- Open access
- Export citation
Emergence of lobed wakes during the sedimentation of spheres in viscoelastic fluids
-
- Journal:
- Journal of Fluid Mechanics / Volume 992 / 10 August 2024
- Published online by Cambridge University Press:
- 27 August 2024, A14
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
Sociodemographic profile and prescribing pattern of antipsychotic medication in patients with Schizophrenia
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S242
-
- Article
-
- You have access
- Open access
- Export citation
The Most Iniquitous Lobby: The Committee for Constitutional Government and the Shaping of American Politics, 1937–1955
-
- Journal:
- Journal of Policy History / Volume 36 / Issue 3 / July 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. 281-307
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
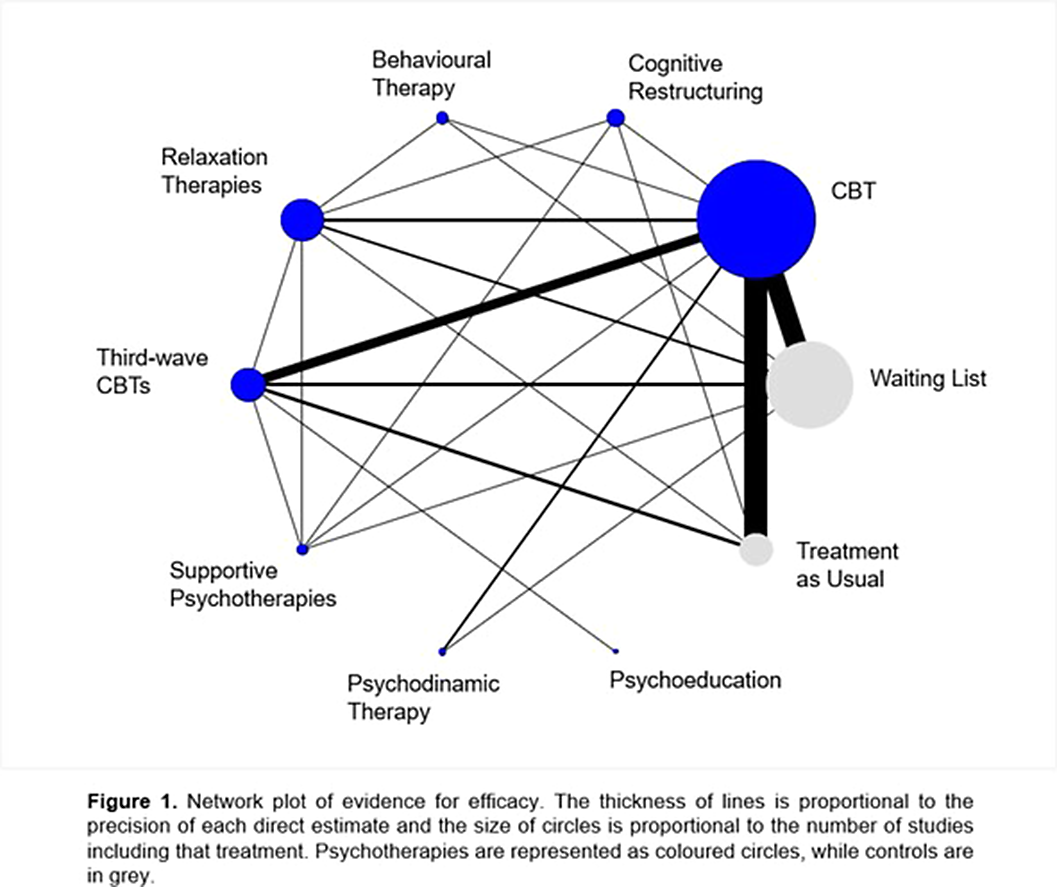
Psychotherapies for generalized anxiety disorder in adults: systematic review and network meta-analysis of randomized-controlled trials
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S50-S51
-
- Article
-
- You have access
- Open access
- Export citation
Cannabis Use and Its Interaction with Anxiety Disorders
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S423-S424
-
- Article
-
- You have access
- Open access
- Export citation
Cariprazine as adjunctive treatment of catatonia in schizoaffective disorder: a case report.
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S238
-
- Article
-
- You have access
- Open access
- Export citation
A Machine Learning Model for Predicting Major Depressive Disorder Using Diffusion-Tensor Imaging Data
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S617-S618
-
- Article
-
- You have access
- Open access
- Export citation
In People who Identify as Gender Minority People the Social Cure Model and in People who Identify as LGBTQ* People the Intragroup Status and Health Model might Explain the Link between Identity Centrality and Body Appreciation
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S557
-
- Article
-
- You have access
- Open access
- Export citation
Prevalence and Risk Factors of Burnout Among Medical Residents in Tunisia: A Cross-Sectional Study
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S830
-
- Article
-
- You have access
- Open access
- Export citation
Guanfacine in the Treatment of a Child Diagnosed with Tourette Syndrome: A Case Report
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S697-S698
-
- Article
-
- You have access
- Open access
- Export citation
Prevalence and predictors of PTSD and resilience among Adolescents and Young Adults: Findings from the MoreGoodDays Support Program in Alberta, Canada
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S306
-
- Article
-
- You have access
- Open access
- Export citation
Dissociative Identity Disorder from a Palestinian Perspective: A Case Report
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S522
-
- Article
-
- You have access
- Open access
- Export citation
Aberrant Functional Connectivity Between Regions Involved in Belief Evaluation and Processing of Bodily Information in Patients with Somatic Delusions
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S644-S645
-
- Article
-
- You have access
- Open access
- Export citation
Protective effect of lithium pyruvate against oxidative damage to peripheral blood mononuclear cells
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S239
-
- Article
-
- You have access
- Open access
- Export citation
Personality Traits in Patients with Depression: Association with Symptoms of Depression and Anxiety
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S257
-
- Article
-
- You have access
- Open access
- Export citation
Ketamine in the treatment of obsessive-compulsive disorder – a case report and literature review
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S631
-
- Article
-
- You have access
- Open access
- Export citation
Psychometric Properties of the Depression, Anxiety, Stress Scales-21 (DASS-21) in a Portuguese Sample during the early stage of the COVID-19 pandemic
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S149
-
- Article
-
- You have access
- Open access
- Export citation