Refine listing
Actions for selected content:
141953 results in Open Access
Exploring the associations between involuntary treatment and gender in a portuguese acute psychiatric unit
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S309-S310
-
- Article
-
- You have access
- Open access
- Export citation
An educational program, «Women victims of domestic violence: Detection, clinic, help»: Working with the complexity of teaching and Interpreting practice through research
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S805
-
- Article
-
- You have access
- Open access
- Export citation
Kambó as a drug that can induce psychotic or manic symptoms. A case report
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S419
-
- Article
-
- You have access
- Open access
- Export citation
Perceived parental bonding and cortisol awakening response in people with eating disorders
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S65
-
- Article
-
- You have access
- Open access
- Export citation
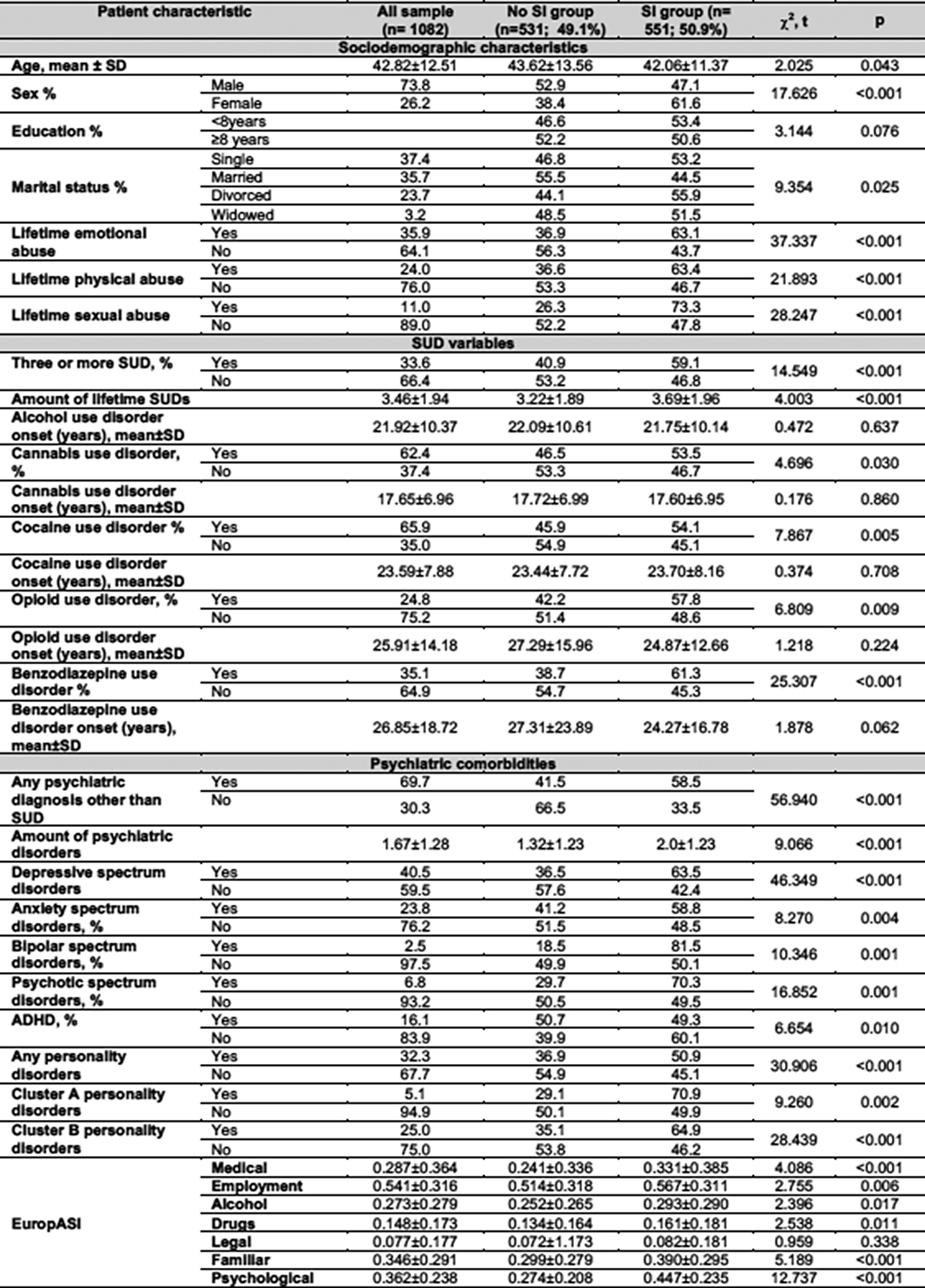
A preliminary analysis of clinical characteristics of patient with alcohol use disorder and suicidal ideation
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S132-S133
-
- Article
-
- You have access
- Open access
- Export citation
Medication choice and psychosis Hospital readmissions: A two-year comparative study
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S288
-
- Article
-
- You have access
- Open access
- Export citation
Non-compliance as ethical dilemma for kidney transplantation
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S577
-
- Article
-
- You have access
- Open access
- Export citation
Neuroinflammation in Recent Onset Mental Health Disorders – Developing Multi-level Signatures of Early-stage Depression and Psychosis in Young Adults
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S45-S47
-
- Article
-
- You have access
- Open access
- Export citation
“Neighbohod Vulnerability and Disability in First Episode of Psychosis”.
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S291-S292
-
- Article
-
- You have access
- Open access
- Export citation
The level of consciousness and mental reactions of children after acute brain injury (interdisciplinary rehabilitation)
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S713
-
- Article
-
- You have access
- Open access
- Export citation
Ethnic differences in pathways to obtain care, maintain care and engage to Early Intervention Service in Spain
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S165
-
- Article
-
- You have access
- Open access
- Export citation
Symptoms of anxiety and depression among osteoporotic women
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S486
-
- Article
-
- You have access
- Open access
- Export citation
Sodium oxybate – new views on an old candidate This presentation will outline the outcome of a clinical development program, including a Phase 3 study, on sodium oxybate in the treatment of alcohol dependence
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S6
-
- Article
-
- You have access
- Open access
- Export citation
When sleep disorders in patients with bipolar disorder indicate a risk of suicidal behavior
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S786
-
- Article
-
- You have access
- Open access
- Export citation
Predictors of Adherence and Response to Exercise Interventions in Schizophrenia
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S11
-
- Article
-
- You have access
- Open access
- Export citation
From guided self-help to comprehensive ED treatment
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S308
-
- Article
-
- You have access
- Open access
- Export citation
Changing Tactics? Optimizing ECT in difficult-to-treat depression (ChaT): study protocol
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S123-S124
-
- Article
-
- You have access
- Open access
- Export citation
Adaptation and analysis of the Hungarian version of the Snaith-Hamilton Pleasure Scale
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S536-S537
-
- Article
-
- You have access
- Open access
- Export citation
Platelet enzymatic activities in patients with late-onset schizophrenia spectrum disorders
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S643
-
- Article
-
- You have access
- Open access
- Export citation
Adverse childhood experiences and 8-year trajectories of depressive symptoms in community-dwelling older adults: Results from the English Longitudinal Study of Ageing
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S333-S334
-
- Article
-
- You have access
- Open access
- Export citation