Refine listing
Actions for selected content:
142351 results in Open Access
Perception of Violence by Psychiatric Nurses: Behind the scenes
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S594
-
- Article
-
- You have access
- Open access
- Export citation
SCHIZOPHRENIC DREAMS: A Brief Description of Sleep Disturbances in Schizophrenia
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S774
-
- Article
-
- You have access
- Open access
- Export citation
Divergent risk of SARS-CoV-2 infection, severe COVID-19 and mortality across psychiatric disorders: analysis from electronic health records in Catalonia
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S264-S265
-
- Article
-
- You have access
- Open access
- Export citation
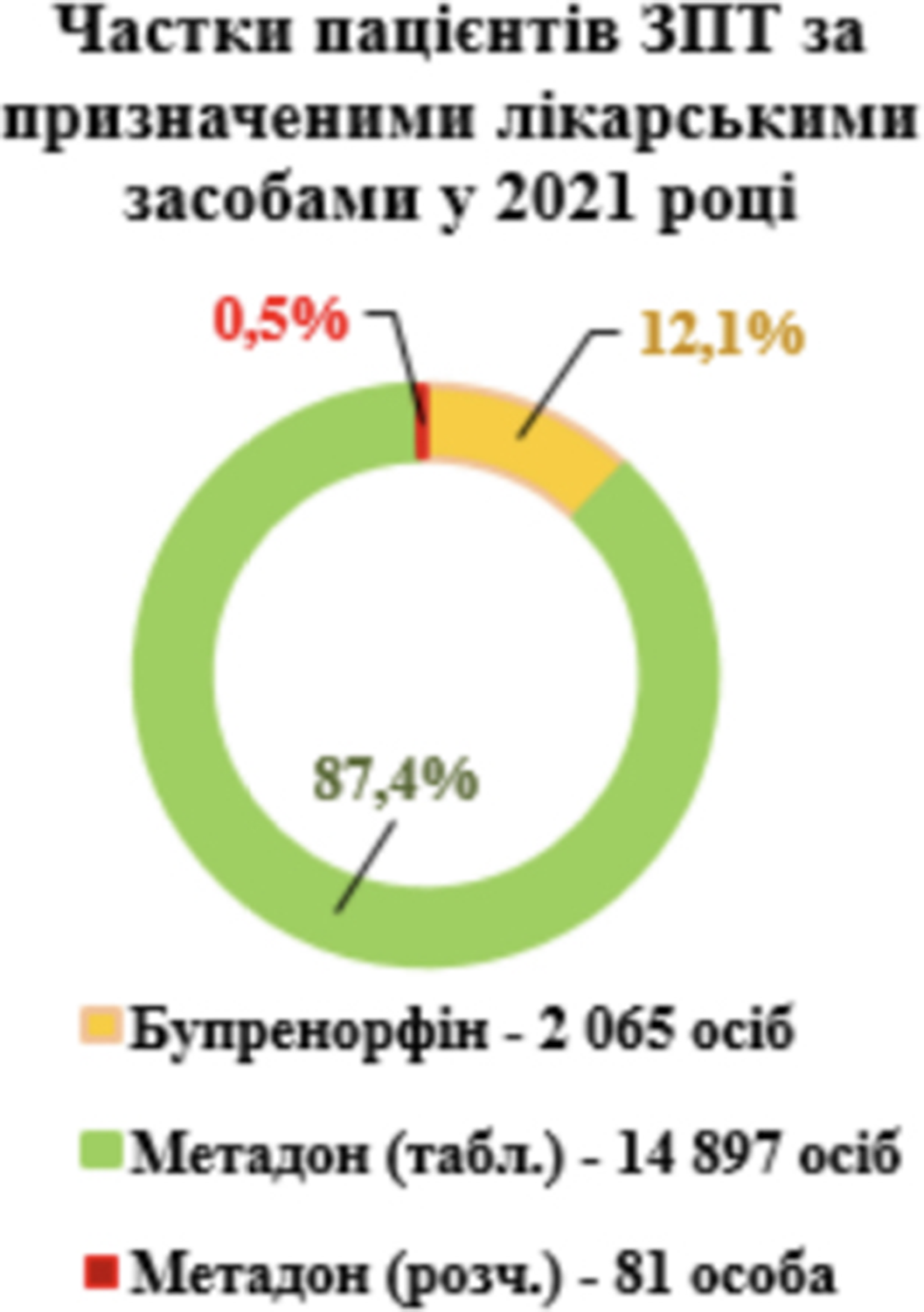
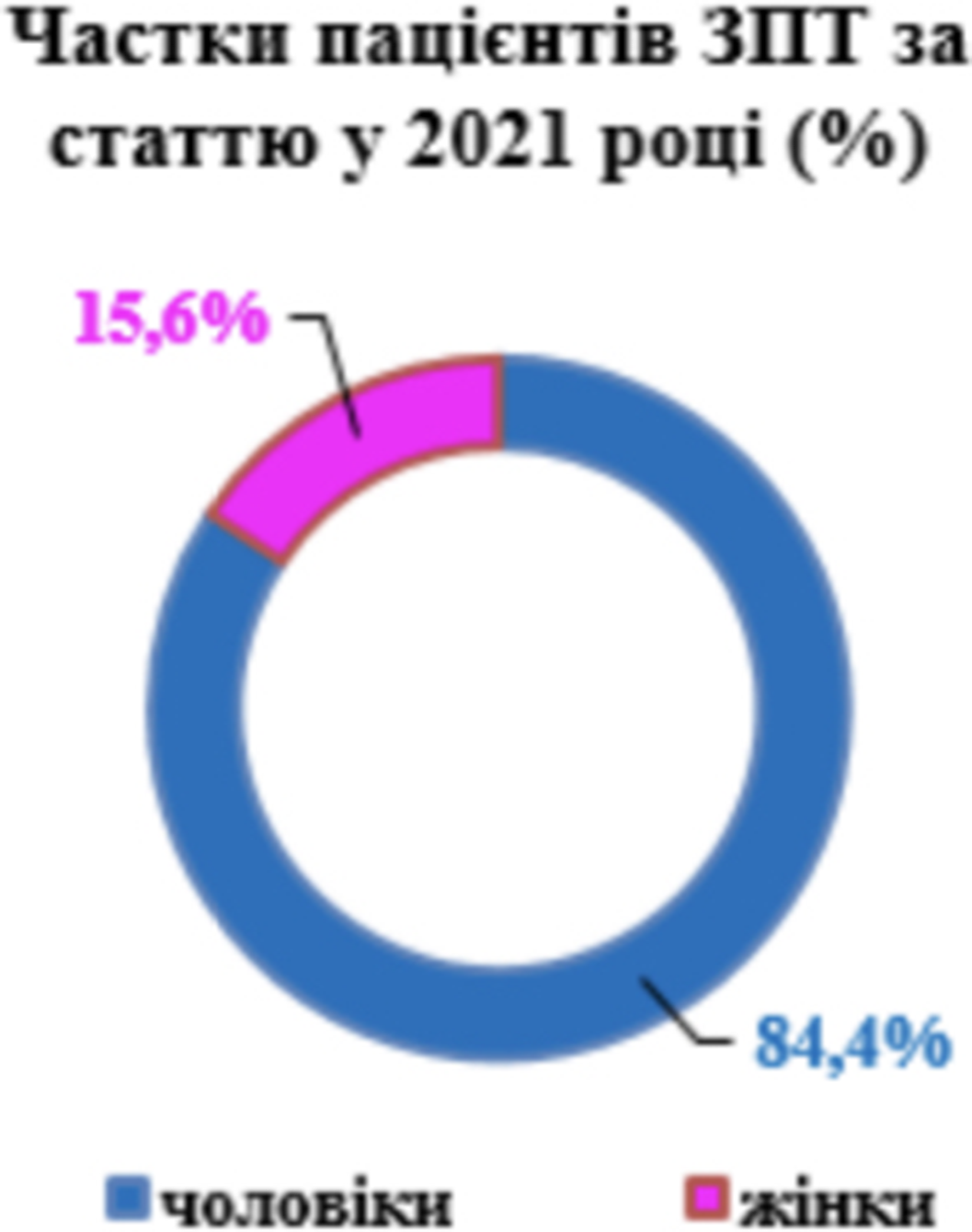
Research of cognitive disorders and quality of life in patients, who are receiving methadone replacement maintenance therapy
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S134-S135
-
- Article
-
- You have access
- Open access
- Export citation
The Influence of Depression in the Evolution of Parkinson’s Disease: A Psychiatric Perspective
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S302
-
- Article
-
- You have access
- Open access
- Export citation
Deliberate self-poisoning in children and adolescents
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S791
-
- Article
-
- You have access
- Open access
- Export citation
Importance of the type of pharmacological treatment in patients with severe mental disorder
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S698-S699
-
- Article
-
- You have access
- Open access
- Export citation
Multifactorial etiology of manic episodes. About a case
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S433
-
- Article
-
- You have access
- Open access
- Export citation
Christian Humanitarianism, Violence and the Debate over Empire
-
- Journal:
- The Journal of Ecclesiastical History / Volume 75 / Issue 4 / October 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. 758-768
- Print publication:
- October 2024
-
- Article
-
- You have access
- Open access
- HTML
- Export citation
The association between glucose 6-phosphate dehydrogenase (G6PD) deficiency and attention deficit/hyperactivity disorder (ADHD)
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S75
-
- Article
-
- You have access
- Open access
- Export citation
A randomized controlled trial comparing trauma-focused treatment with and without concurrent personality disorder treatment in patients with posttraumatic stress disorder and comorbid borderline personality disorder
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S667
-
- Article
-
- You have access
- Open access
- Export citation
Artificial Intelligence in Psychiatry: A Comprehensive Literature Review
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S61
-
- Article
-
- You have access
- Open access
- Export citation
Effectiveness of AI-driven Individualized Learning Approach for Children with Autism Spectrum Disorder (ASD)
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S77
-
- Article
-
- You have access
- Open access
- Export citation
Eating disorder and bipolar mental illness through genome wide association studies
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S555
-
- Article
-
- You have access
- Open access
- Export citation
Improving the Sexual Wellbeing of Patients with Psychotic Illness
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S738-S739
-
- Article
-
- You have access
- Open access
- Export citation
Predictors for Burnout Among Healthcare Workers in a Post -Covid Era
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S499
-
- Article
-
- You have access
- Open access
- Export citation
Haloperidol induced Pisa syndrome in a patient with treatment resistant schizophrenia
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S759
-
- Article
-
- You have access
- Open access
- Export citation
A scoping review of the literature on interventions to reduce stress and burnout among teachers.
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S206-S207
-
- Article
-
- You have access
- Open access
- Export citation
Psychopathological characterization of nomophobia in a sample of patients with severe mental illness
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, p. S375
-
- Article
-
- You have access
- Open access
- Export citation
Anticipatory competence of adolescents with movement disorders in the prevention of deviations
-
- Journal:
- European Psychiatry / Volume 67 / Issue S1 / April 2024
- Published online by Cambridge University Press:
- 27 August 2024, pp. S659-S660
-
- Article
-
- You have access
- Open access
- Export citation